 |
 |
 |
| |
Association Between Emergent Antiretroviral Drug Resistance and Baseline CD4 Cell Count in
Treatment-Naive Patients Initiating Protease-Inhibitor-Based Therapy in Clinical Trials
|
| |
| |
Reported by Jules Levin
IDSA Oct 17-21 San Diego 2012
Daniel Seekins, MD and Jonathan Uy, MD
Bristol-Myers Squibb Research and Development,
Plainsboro, NJ
Program Abstract:
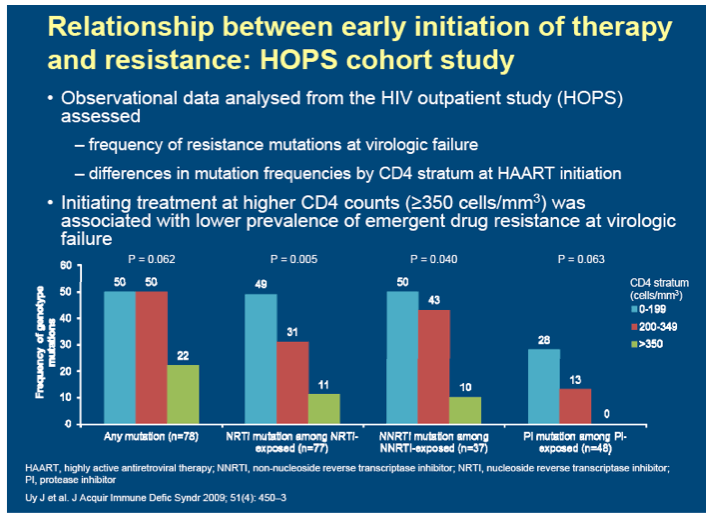
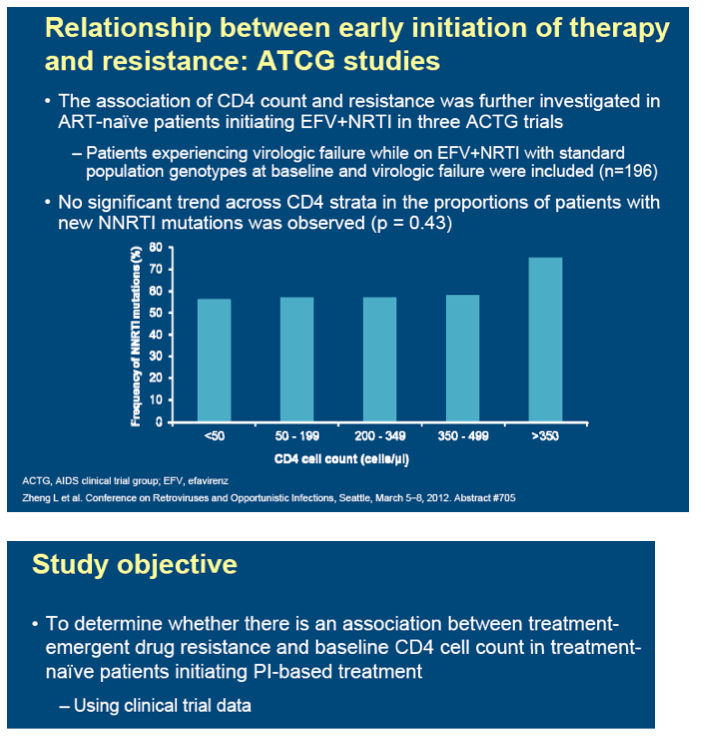
Background: The risk of developing drug resistance is cited by the US treatment guidelines (DHHS 2012) as a potential limitation of earlier treatment initiation. However, one study utilizing observational cohort data suggests that a lower prevalence of emergent drug resistance at the time of virologic failure occurs in patients who initiated treatment at higher CD4 counts (Uy 2009). A more recent analysis utilizing clinical trials data that studied EFV-based treatment did not confirm this finding (Zheng, CROI 2012). The purpose of this analysis is to study the association between treatment-emergent drug resistance and baseline CD4 cell count utilizing clinical trials data in treatment-naive patients initiating protease-inhibitor-based treatment.
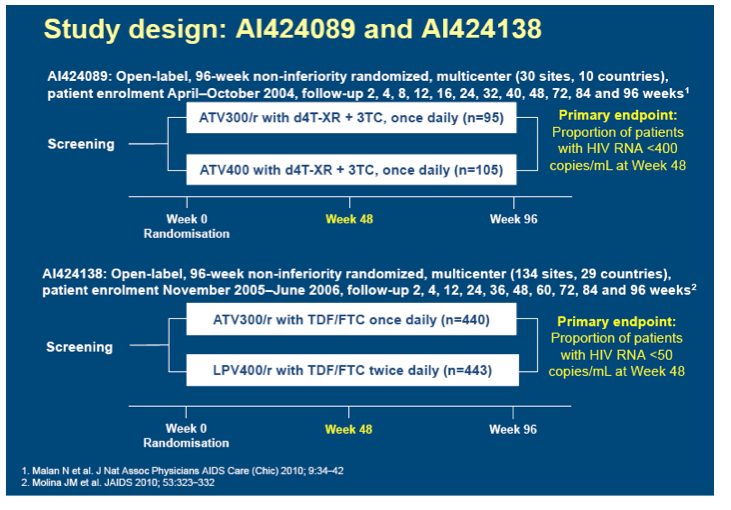
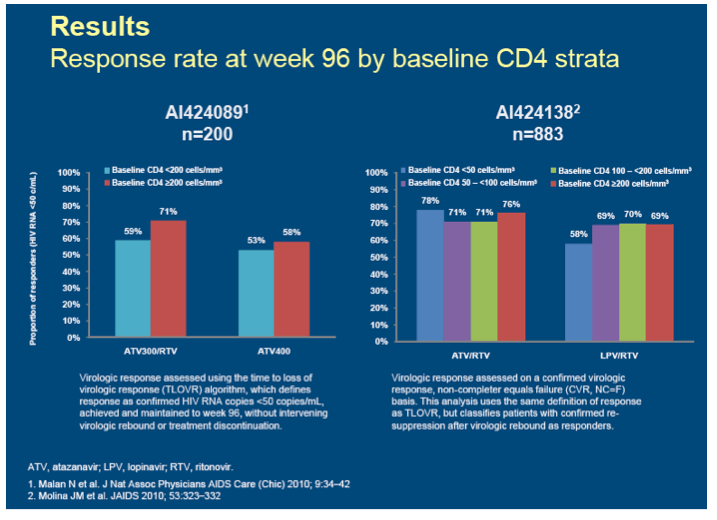
Methods: Data utilized this analysis are from two international clinical trials that studied treatment-naive patients: AI424089 (ATV/r vs. ATV, each with d4T-XR + 3TC; Malan 2010) and AI424138 (ATV/r vs. LPV/r, each with TDF/FTC; Molina, 2009). 96 week data were used. Patients who had a resistance test done after virologic failure were included in the analysis. Emergent resistance was defined as having ≥1 major resistance-associated mutation in a class used in treatment (NRTI, PI) defined by IAS-USA and Stanford HIVDB. Two-sided P values for association between baseline CD4 cell count strata (<200, 200-<350, ≥350) and emergent resistance were calculated with the Cochran-Armitage exact test.
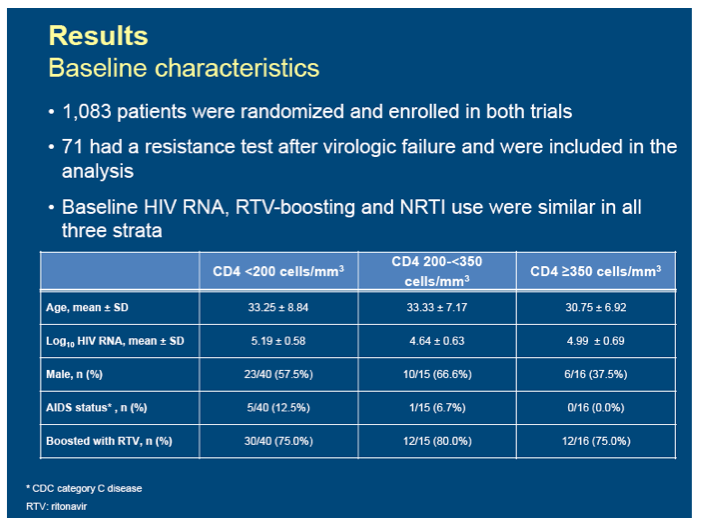
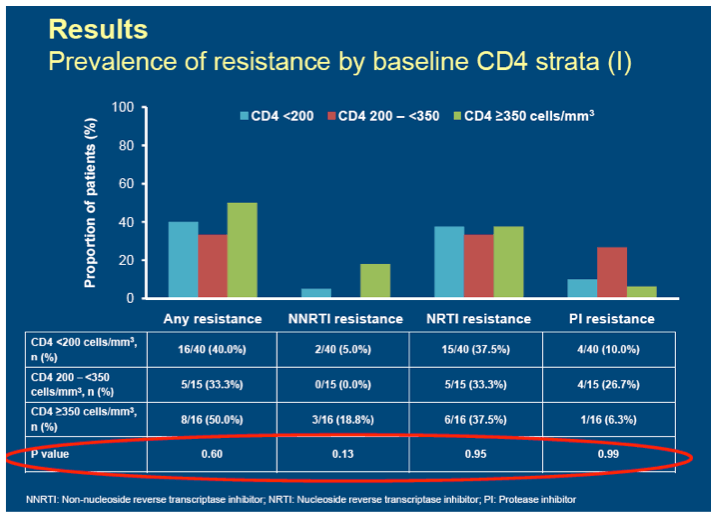
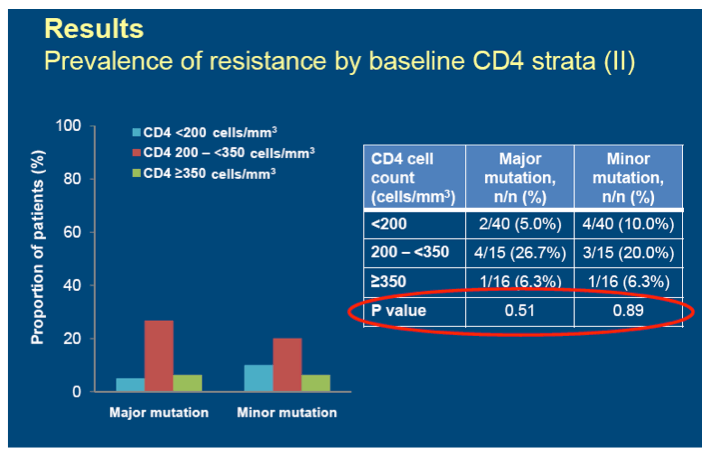
Results: A total of 1,083 patients were randomized and enrolled in both trials. 74 patients with a resistance test after virologic failure were included in the analysis. RTV-boosting, NRTI use and baseline HIV RNA were similar in all three strata. Prevalence of resistance by baseline CD4 strata are presented in the table:
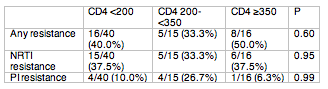
Conclusion: In this analysis of two treatment-naive clinical trials using protease inhibitor-based treatment, there was no association between emergent antiretroviral drug resistance and baseline CD4 cell count strata.




|
| |
|
 |
 |
|
|