 |
 |
 |
| |
Health Deficits Accumulate Faster With HIV Than Without in Older Adults
|
| |
| |

5th International Workshop on HIV and Aging. October 20-21, 2014. Baltimore.
Mark Mascolini
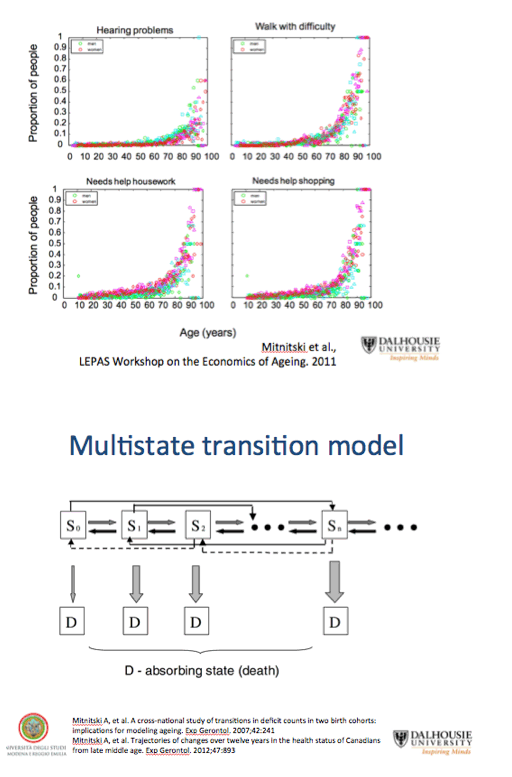
Health deficits from a list of 31 variables accumulated significantly faster over 4 years in older HIV-positive adults in Italy than in a comparison group from the general population [1]. Among people with 3 deficits at a baseline visit, 92% in the HIV cohort had a worse health deficit score 4 years later, compared with 55% in the general population.
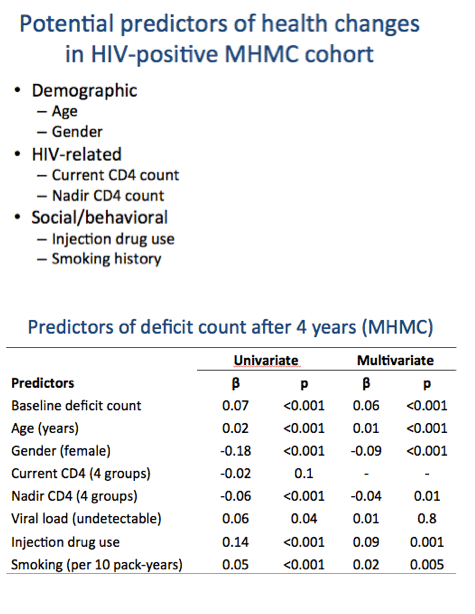
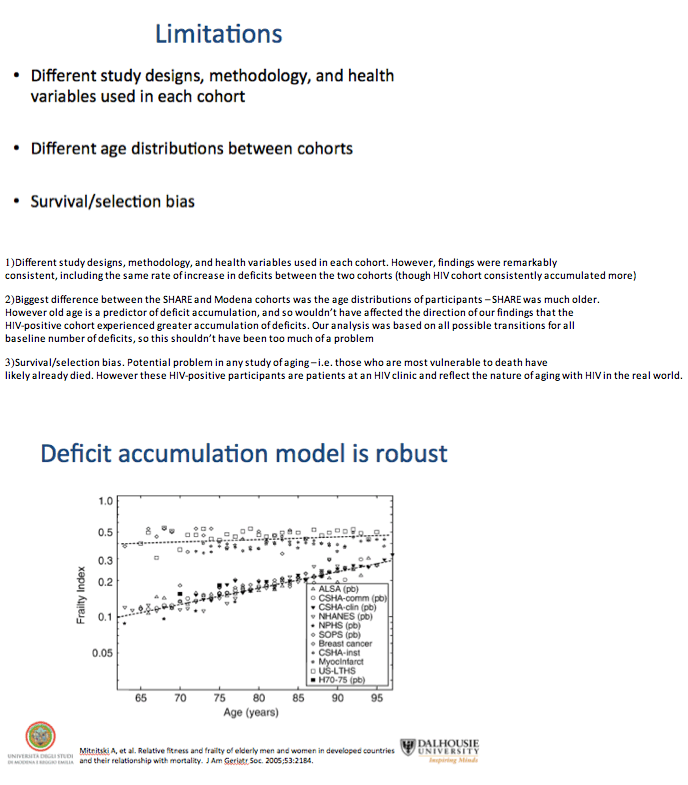
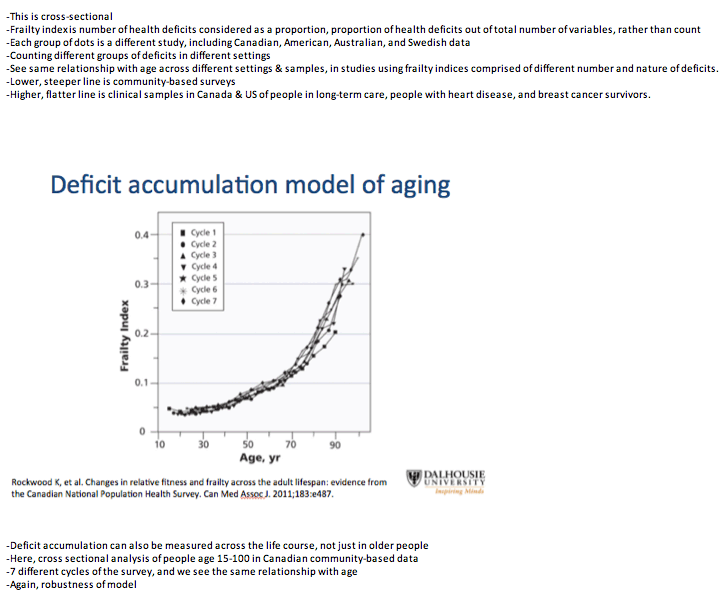
Researchers at Dalhousie University in Halifax and colleagues in Modena and Montreal proposed that aging can be characterized by tabulating health deficits (such as signs, symptoms, and lab abnormalities) on a predetermined list and then assessing changes in accumulated deficits over time. To compare aging trajectories in older adults with and without HIV, these investigators compared health deficit changes in a large HIV group at the Modena HIV Metabolic Clinic and a general-population Italian comparison group from Survey of Health, Aging, and Retirement in Europe (SHARE).
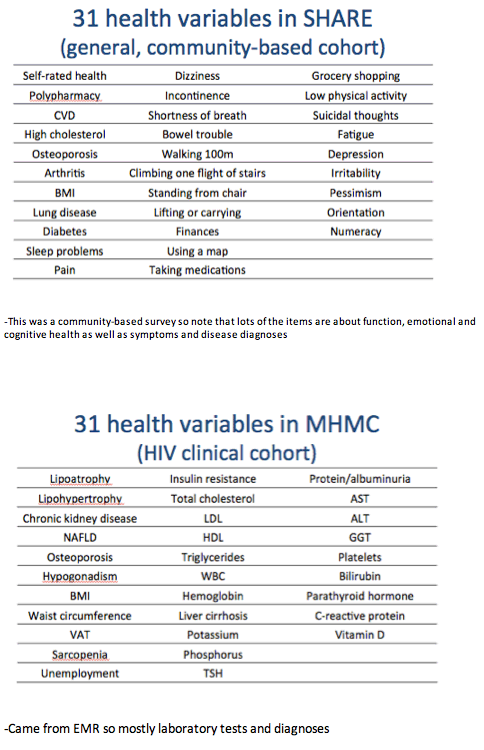
The HIV group made annual visits, while the community-dwelling comparison group made study visits every 2 years. For each participant, researchers recorded health deficits from a list of 31 items. The 31 deficits differed for people with and without HIV, with minimal overlap. The SHARE list included variables addressing function, emotional and cognitive health, and disease symptoms and diagnoses. The HIV list included mostly lab tests but also clinical symptoms and conditions. Shared items were body mass index, cholesterol, and diabetes (SHARE) or insulin resistance (HIV).
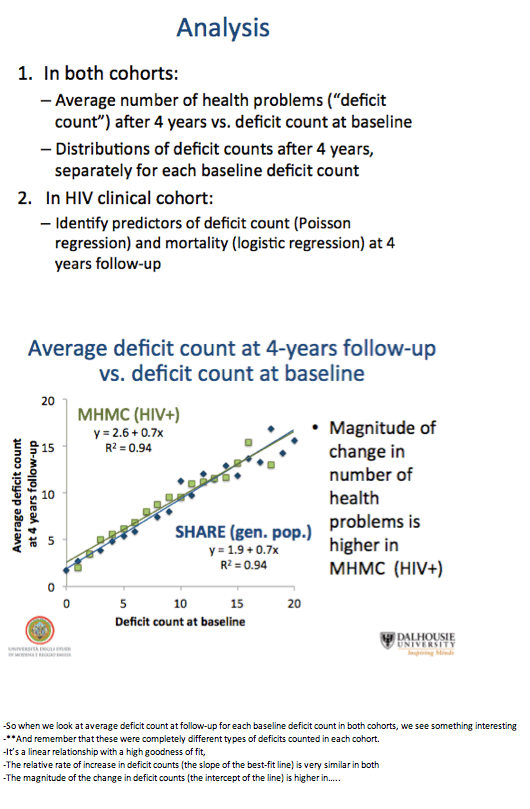
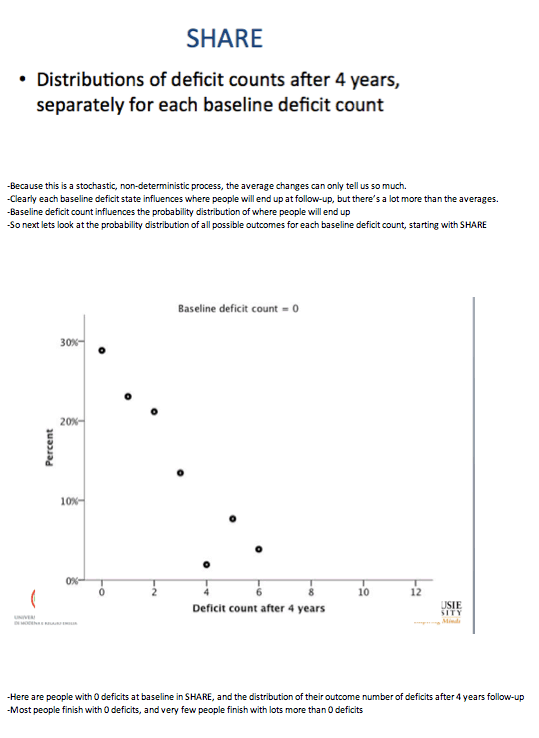
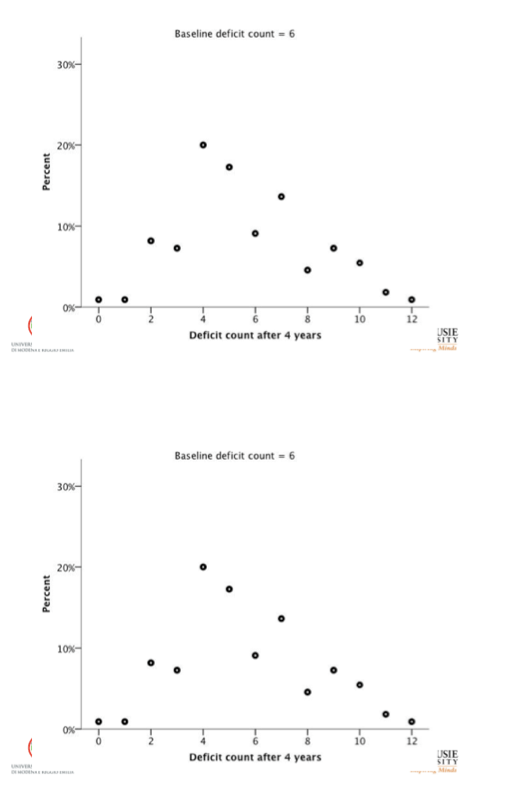
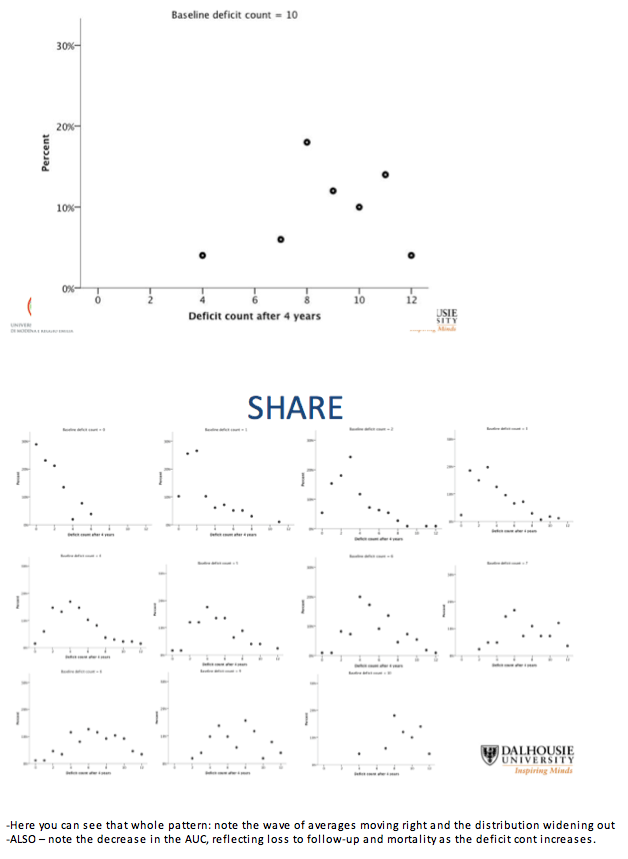
The investigators calculated probabilities of health state changes, including death, every 4 years with a multistate transition model. They first assessed the relationship between baseline deficit count and average deficit count at follow-up. Then they assessed probabilities of deficit counts at follow-up and risk of death in relation to baseline deficit count, age, and gender.
The study involved 3179 HIV-positive people averaging 45 years in age (range 16 to 76); 33% were women. The general-population SHARE group included 2500 people averaging 64 years in age (range 39 to 100). More than half (56%) were women. So the study populations differed substantially in age and gender.
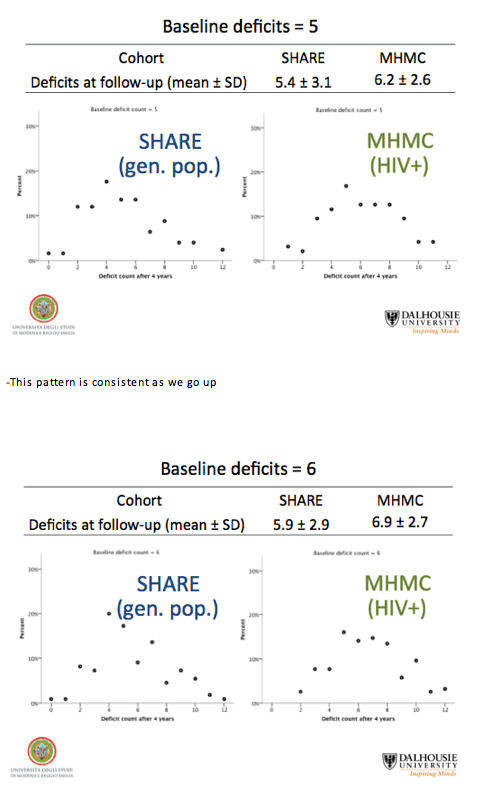
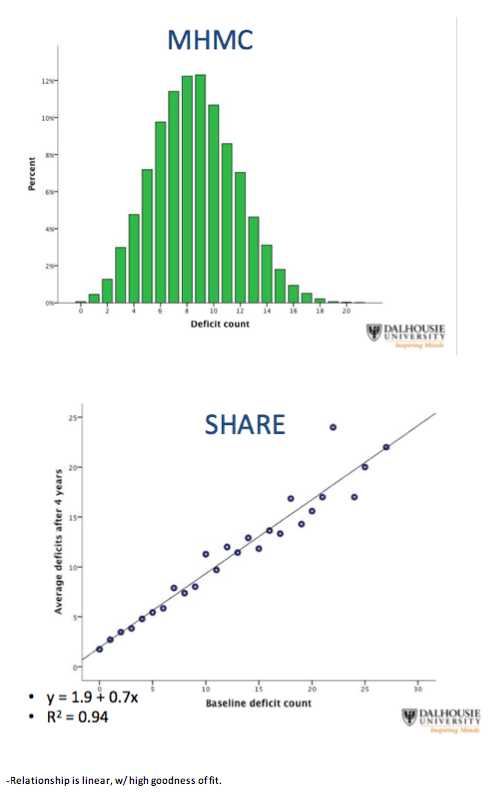
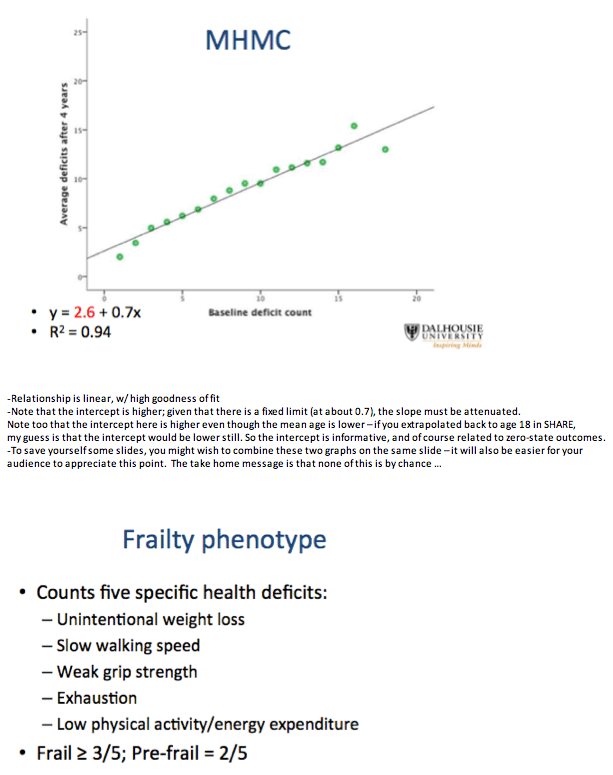
Even though deficit items differed between the HIV group and the general-population group, baseline deficit score correlated strongly with average deficit count after 4 years in both the HIV group and the SHARE comparison group (r2 = 0.94 for both). Health status as reflected by deficit count generally worsened with age, but deficit counts could remain stable or even improve over time.
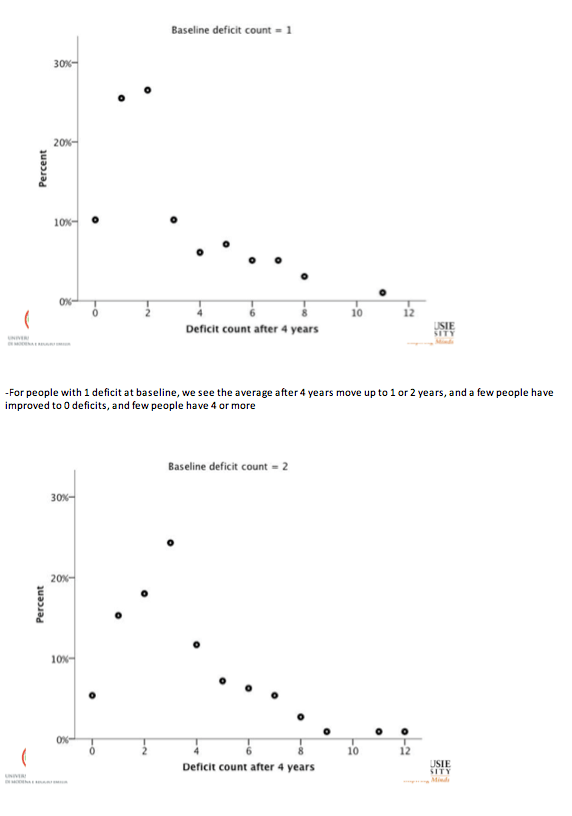
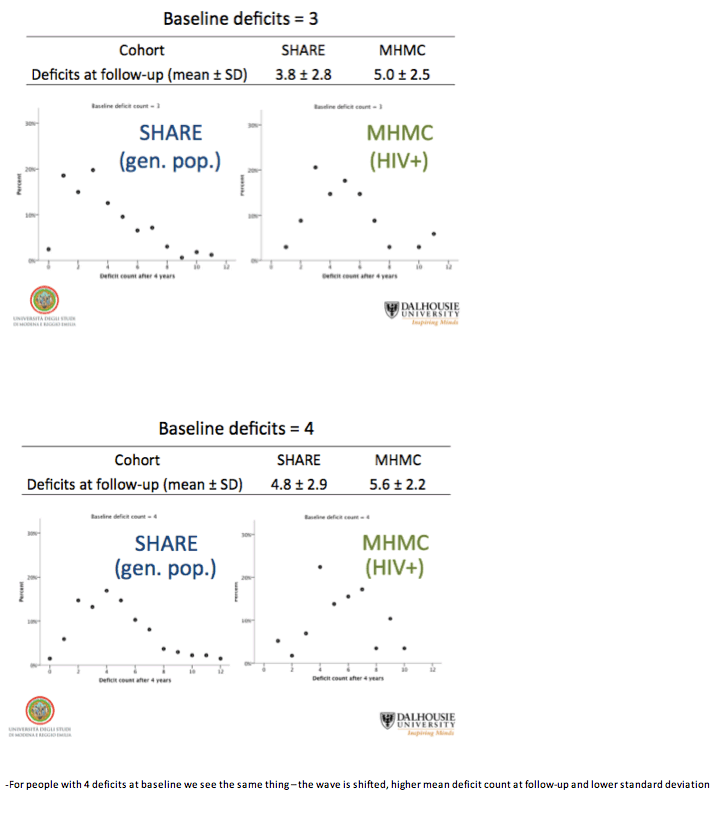
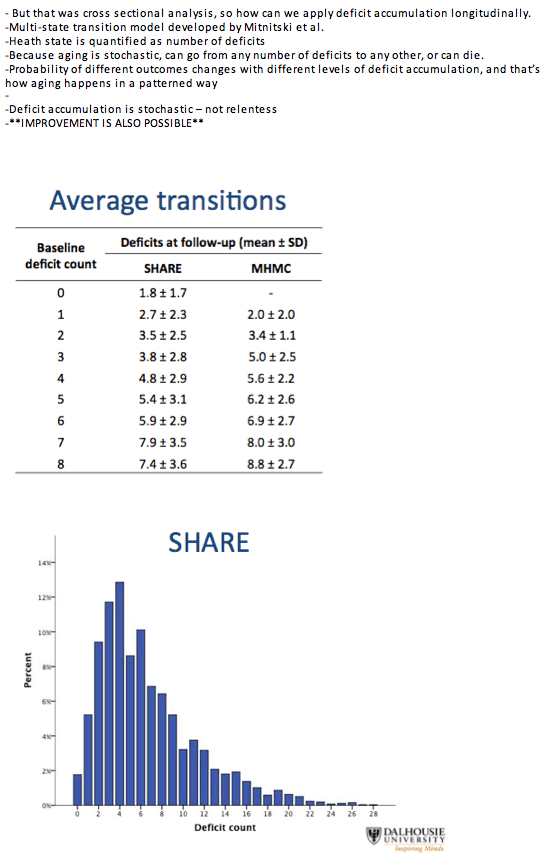
People with HIV proved more likely than SHARE members to acquire health deficits over the years. For example, people with 3 baseline deficits had an average 4.07 (+/- 1.94) in 4 years in the HIV group and an average 3.84 (+/- 2.80) in SHARE. Among people with 3 baseline deficits in SHARE, 55% had a higher deficit tally 4 years later, while the rest had the same number of deficits or fewer. Among people with 3 baseline deficits in the HIV group, 92% had more deficits 4 years later and 8% remained stable or improved.
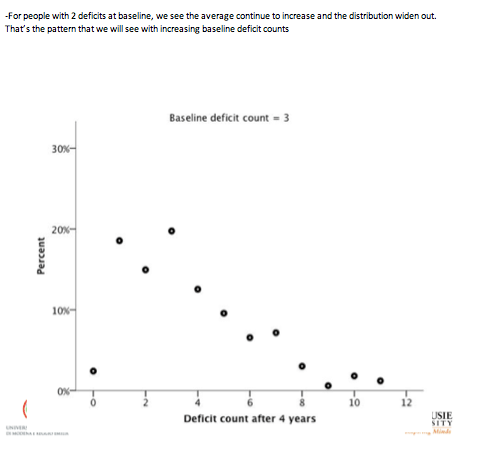
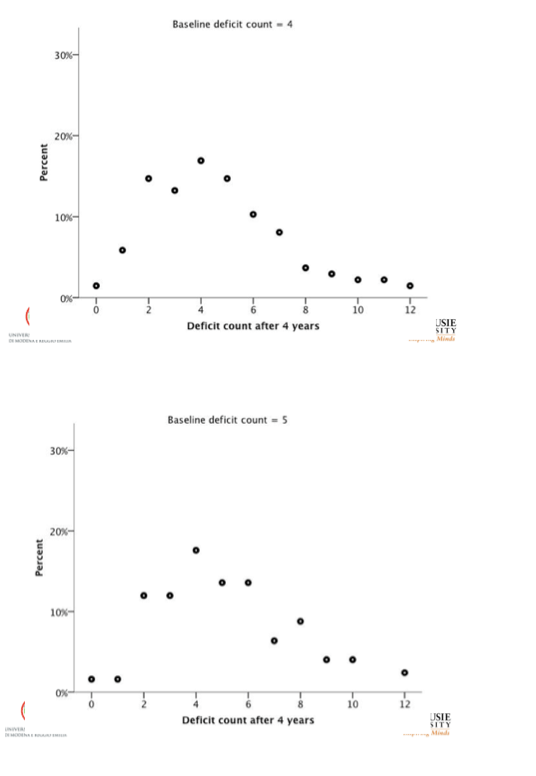
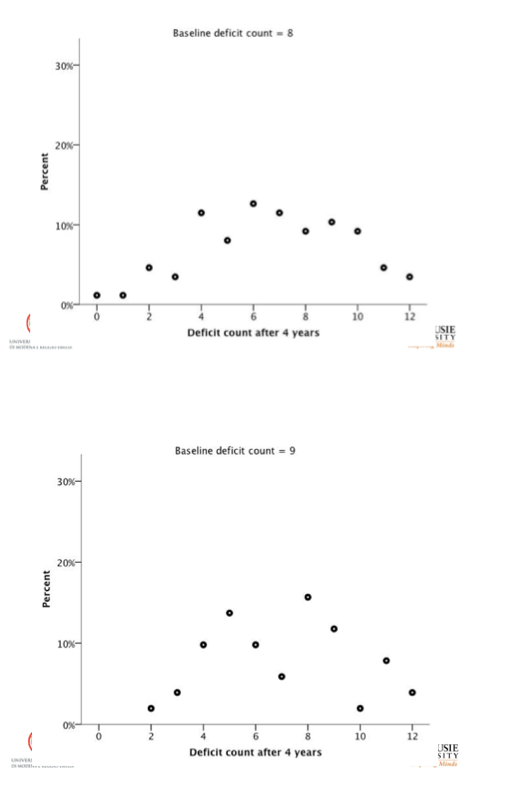
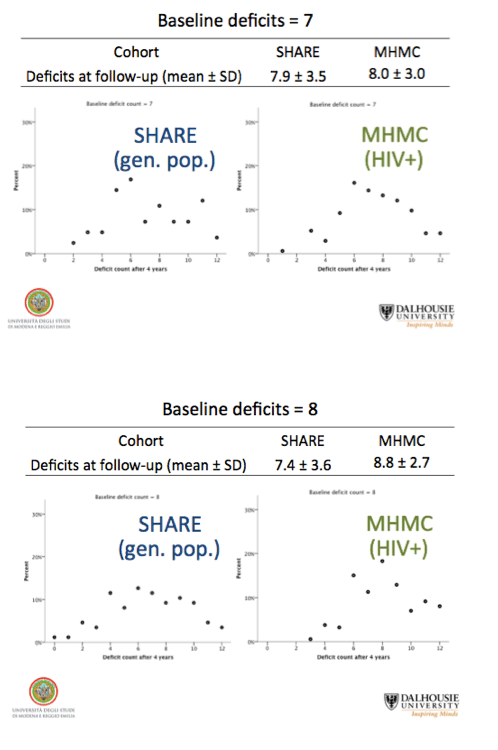
For people with 4, 6, and 8 deficits at baseline, average deficit scores 4 years later were always higher in the HIV group than the SHARE group, while variability (standard deviation) was always lower in the HIV cohort:
-- 4 baseline deficits: 5.6 +/- 2.2 versus 4.8 +/- 2.9
-- 6 baseline deficits: 6.9 +/- 2.7 versus 5.9 +/- 2.9
-- 8 baseline deficits: 8.8 +/- 2.7 versus 7.4 +/- 3.6
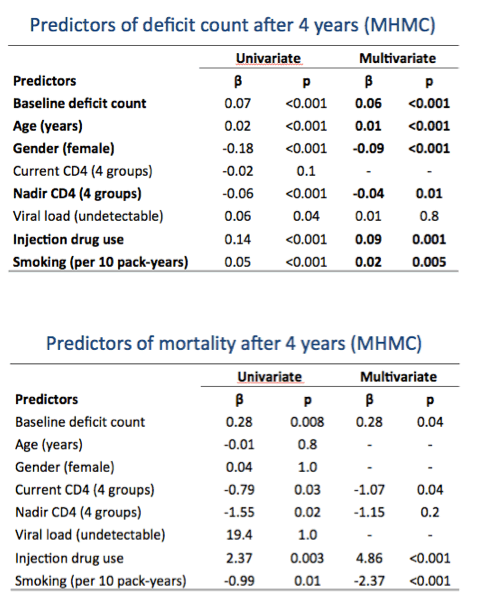
Multivariate analysis identified six predictors of deficit count after 4 years in people with HIV: baseline deficit count (beta 0.06, P < 0.001), older age (beta 0.01, P < 0.001), female gender (beta -0.09, P < 0.001), nadir CD4 count (beta -0.04, P = 0.01), injection drug use (beta 0.09, P = 0.001), and smoking (beta 0.02 per 10 pack-years, P = 0.005).
Four-year mortality in the HIV cohort stood at 4%. Four factors predicted mortality after 4 years in people with HIV: baseline deficit count (beta 0.28, P = 0.04), current CD4 count (beta -1.07, P = 0.04), injection drug use (beta 4.86, P < 0.001), and smoking (beta -2.37 per 10 pack-years, P < 0.001).
The researchers concluded that similar patterns of deficit accumulation occurred in the general population and in people with HIV over 4 years. But, compared with the general population, HIV-positive people acquired more health problems over the same period and had less variability in outcomes (a smaller standard deviation).
Another study using the same deficit scoring in the Modena HIV population found that frailty and age are independently associated with patterns of antiretroviral prescribing (reviewed separately by NATAP) [2].
References
1. Brothers TD, Kirkland S, Theou O, et al. Exploring aging trajectories among people with HIV and a general community-based cohort: transitions in health status and risk of death. 5th International Workshop on HIV and Aging. October 20-21, 2014. Baltimore. Abstract 11.
2. Guaraldi G, Brothers TD, Zona S, et al. Frailty and age are independently associated with patterns of HIV antiretroviral use in a clinical setting. 5th International Workshop on HIV and Aging. October 20-21, 2014. Baltimore. Abstract 10.








'


|
| |
|
 |
 |
|
|