 |
 |
 |
| |
Prenatal Exposure to Zidovudine and Risk for Ventricular Septal Defects and Congenital Heart Defects:
Data From the Antiretroviral Pregnancy Registry (APR)
|
| |
| |
Reported by Jules Levin
20th International AIDS Conference, July 20-25, 2014, Melbourne
V Vannappagari,1,2 J Albano,3 N Koram,1 H Tilson,2 AE Scheuerle,4 M Napier2
1Worldwide Epidemiology, GlaxoSmithKline, RTP, NC, USA; 2Gillings School of Global Public Health, University of North Carolina-Chapel Hill, NC, USA; 3INC Research, Post Approval and Strategic Services, Raleigh, USA; 4Tesserae Genetics, Dallas, TX, USA

program abstract
Background: We assessed the risk for ventricular septal defect (VSD) and congenital heart defects (CHD) following zidovudine (ZDV) exposure during pregnancy in the Antiretroviral Pregnancy Registry (APR), which monitors for early signals of teratogenicity following prenatal exposure to antiretrovirals.
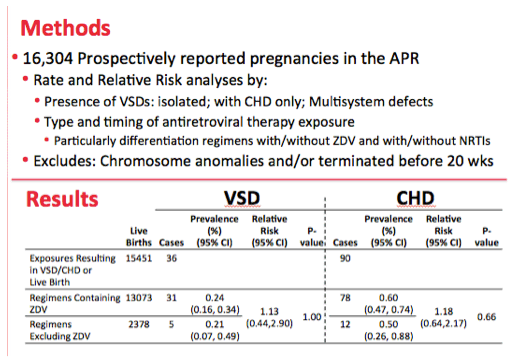
Methods: Using data on 16,304 prospectively reported pregnancies closed with outcome through July 31, 2013, we estimated the frequency of and risk for VSD and CHD, comparing exposure to ZDV-containing regimens to exposure to non-ZDV antiretroviral (ARV) regimens. Numerator includes defect cases in outcomes at ≥ 20 weeks gestational age. Denominator includes live birth outcomes. Infants with chromosomal anomalies were excluded from these analyses.
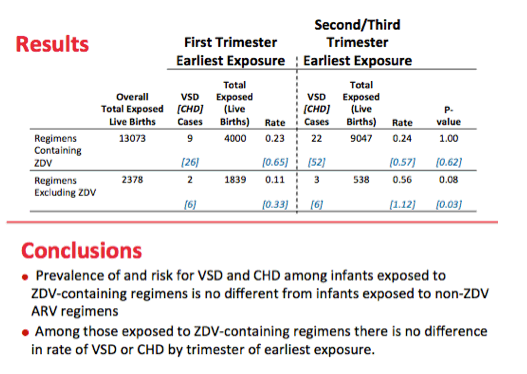
Results: There were 15,451 live birth outcomes; 13,073 were prenatally exposed to ZDV-containing and 2,378 to non-ZDV containing regimens. There were 36 VSD cases; 31 exposed to prenatal ZDV; 5 unexposed. Nine of the ZDV-exposed cases had earliest exposure in the 1st trimester; 22 had 2nd/3rd trimester exposure.
There were 5 VSD cases not exposed to ZDV; 2 had earliest exposure to non-ZDV ARV regimen in the 1st trimester; 3 had 2nd/3rd trimester exposures. The prevalence of VSD for infants exposed to ZDV-containing regimens was 0.24% (95% CI: 0.16-0.34); for non-ZDV regimens, 0.21% (95% CI: 0.07-0.49). The relative risk (RR) comparing the two was 1.13 (95% CI: 0.44-2.90).
There were a total of 90 CHD cases; 78 were exposed prenatally to ZDV-containing regimens; 12 were unexposed. Twenty-six of the ZDV-exposed cases had earliest exposure in the 1st trimester; 52 had 2nd/3rd trimester exposure. Six CHD cases with non-ZDV ARV regimens had earliest exposure in the 1st trimester; 6 had 2nd/3rdtrimester exposure. The prevalence of CHD for infants exposed to ZDV-containing regimens was 0.60% (95% CI: 0.47-0.74); for non-ZDV regimens, 0.50% (95% CI: 0.26-0.88). The RR comparing the two was 1.18 (95% CI: 0.64-2.17).
Conclusions: The prevalence of and risk for VSD and CHD among infants exposed to ZDV-containing regimens is no different from infants exposed to non-ZDV containing regimens.
|
| |
|
 |
 |
|
|