 |
 |
 |
| |
Optimization of the HCV Testing and Care Continuum in an Urban Federally Qualified Health Center in Denver
|
| |
| |
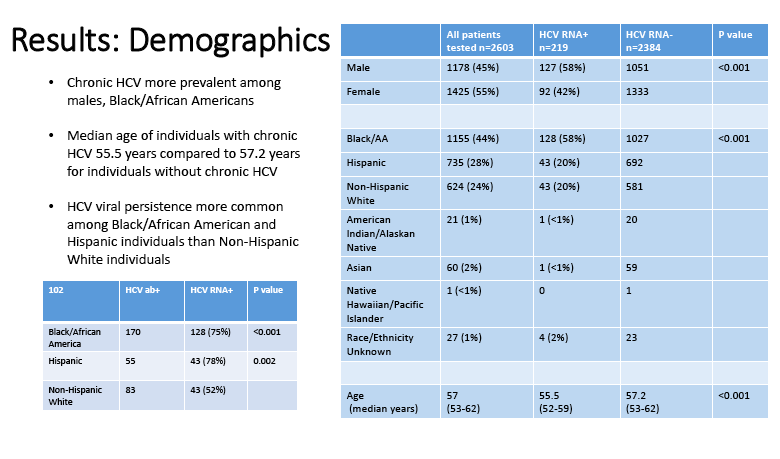
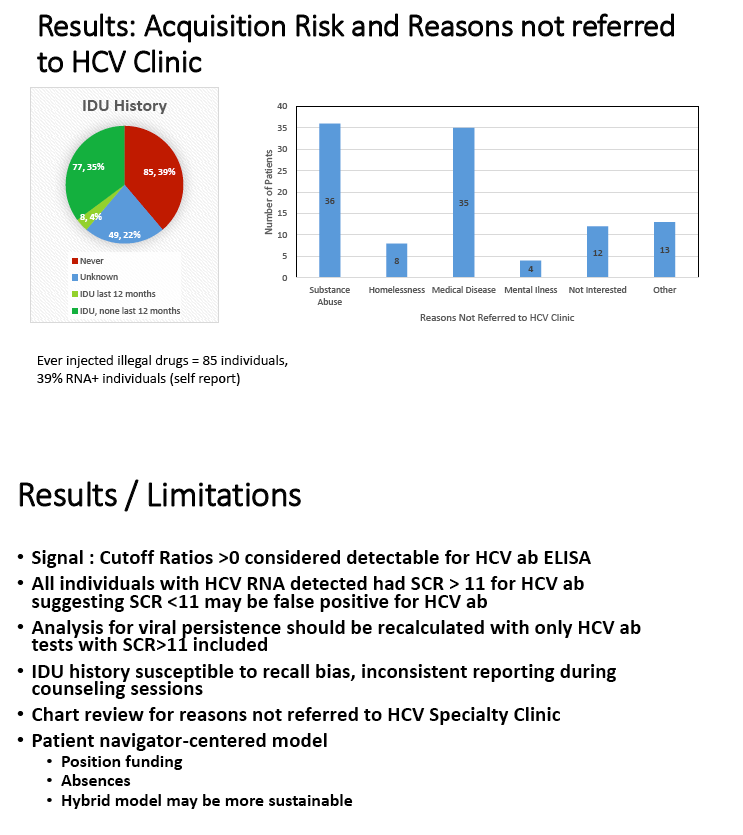
..... from Jules: the prevalence of chronic HCV among Black/AA patients in our cohort was 11%, prevalence among Hispanics was 6%, among whites 7%.......reasons for not referring include: substance abuse 36%, homelessness 8%, medical disease 35%, mental illness 4%.....other similar studies show followup & treatment rates are low in similar patient populations
Reported by Jules Levin
IDSA Oct 8-12 2014 Philadelphia, PA
Sarah E. Rowan, MD, Joshua Blum, MD, Kirsten Spielmann, Katelyn Wanttaja, Jack Lemon, Shawni Vaughn, Edward M. Gardner, William J. Burman
Denver Health and Hospital Authority, Denver, CO

Program abstract:
Background: The reported prevalence of hepatitis C (HCV) among Americans born between 1945 and 1965 is 2.6%. Only half of individuals infected with HCV are aware of their infections, and only 5% are treated and achieve sustained virologic response. As more effective antiviral treatments become available, optimizing the steps in the HCV care continuum are crucial to changing the course of the epidemic.
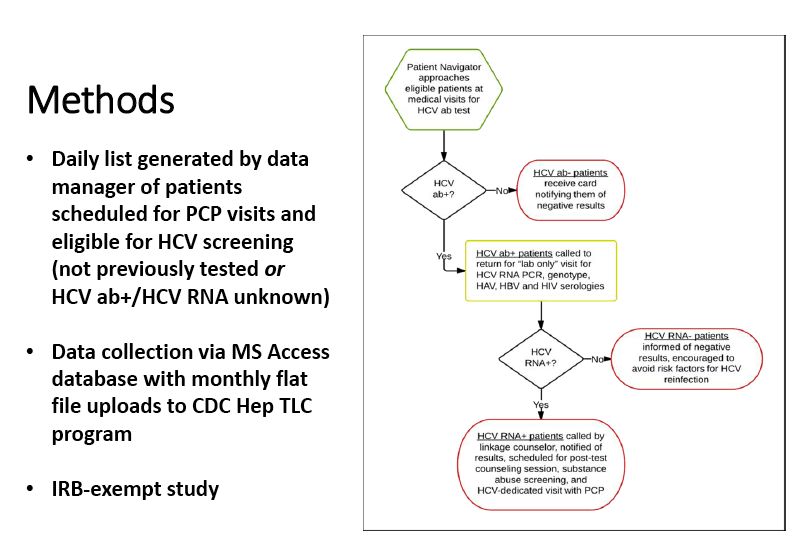
Methods: Birth cohort testing and linkage to care was prospectively evaluated at two federally qualified community health centers among patients who had no prior HCV testing, or who had a prior positive HCV antibody (ab) test without a follow-up RNA test. Of the patients scheduled for routine medical care, an automated list of those eligible for birth cohort testing was generated daily. While waiting to see their providers, patients were offered HCV screening by a patient navigator. Results were then reviewed by the navigator who arranged for subsequent testing and linkage to care. See Figure 1.
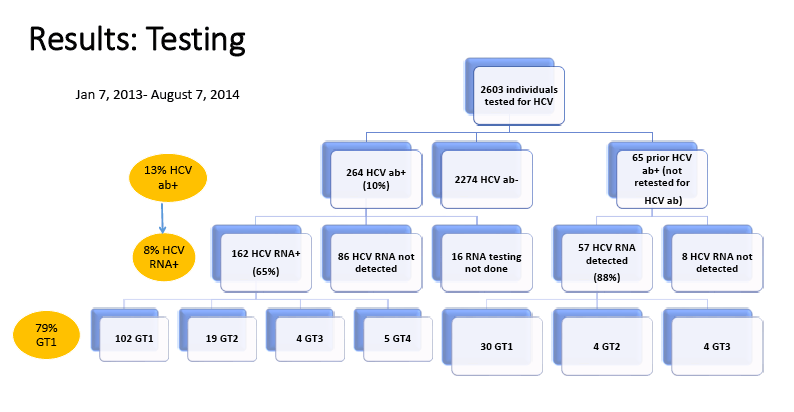
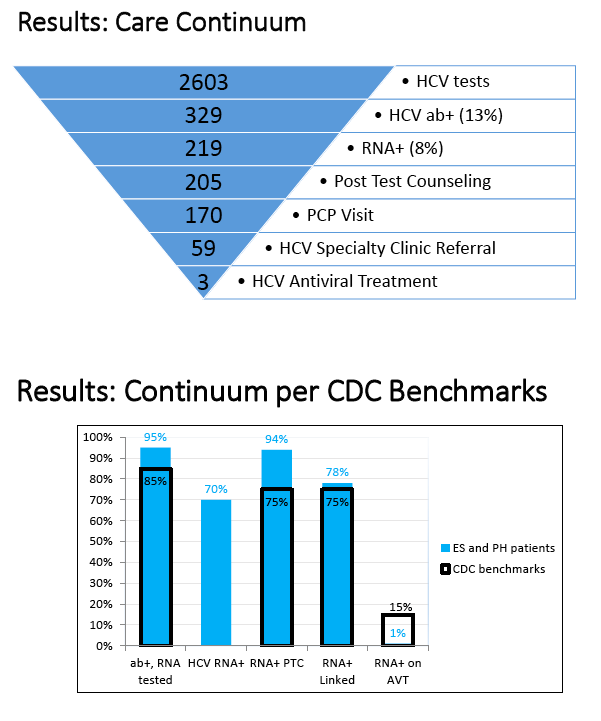
Results: Between January 7, 2013 and April 16, 2014, 2034 individuals were screened for HCV, 263 (13%) were HCV ab+, and 171 (8%) were diagnosed with chronic HCV (detectable RNA). All of the individuals diagnosed with chronic HCV had signal to cutoff ratios>11 for HCV abs. Of the individuals diagnosed with chronic HCV, 34 (20%) had a positive HCV ab test prior to the study period. 93% of individuals with chronic HCV completed a post-test counseling session and 75% had an HCV-dedicated visit with a primary care provider. See Figure 2. Compared to those without HCV, those diagnosed with chronic HCV were more often African American (61% vs 44%, p<0.001) and male (55% vs 43%, p=0.007). Viral persistence after infection was higher among African Americans than non-African Americans (79% vs 59%, p<0.001).
Conclusion: The prevalence of HCV ab and RNA positivity in our birth cohort population was substantially higher than reported nationally. Through optimization of the HCV care continuum, we achieved high rates of follow-up testing, counseling, and linkage to primary care providers, though the percentage of individuals started on HCV antiviral therapy remained low. These analyses should be repeated when direct acting antiviral medications are more readily available.


|
| |
|
 |
 |
|
|