 |
 |
 |
| |
Trends in incidences and risk factors for hepatocellular carcinoma & other liver events in HIV/HCV co-infected individuals from 2001 to 2014: a multi-cohort study
|
| |
| |
Reported by Jules Levin
EACS 2015 Oct 21-24 Barcelona, Spain
Lars I. Gjærde, Leah Shepherd, Amanda Mocroft,
Andri Rauch, John Gill, Marina B. Klein & Lars Peters
On behalf of EuroSIDA in EuroCoord and the HCC Study Group

Program abstract
Objectives: Liver-related deaths among hepatitis C virus (HCV) and HIV co-infected individuals have declined over the last decade, while hepatocellular carcinoma (HCC) may have increased. We aimed to describe incidence trends and risk factors for HCC and other liver events in people co-infected with HCV and HIV.
Methods: We included HCV antibody-positive HIV-patients under follow-up from 2001 to 2014 in four prospective cohorts (EuroSIDA, South Alberta Clinic Cohort, Canadian Co-infection Cohort, Swiss HIV Cohort Study). Baseline was defined as the latest of 1 January 2001, first visit, or first positive HCV antibody-test. We studied two outcomes: 1) HCC, and 2) other liver events, defined as liver-related deaths or decompensations, excluding HCC. Poisson regression was used to estimate incidence rate ratios.
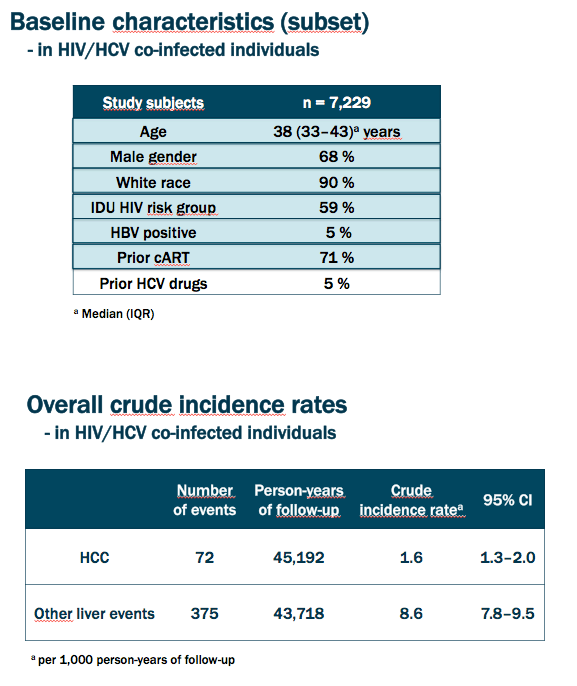
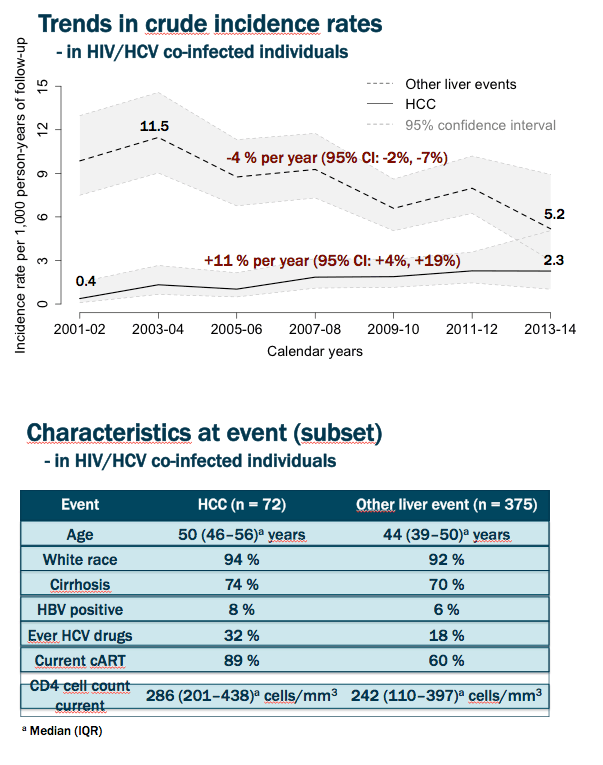
Results: Our study comprised 7,229 individuals (68% male, 90% white) from Eastern Europe and Argentina (27%), Western Europe (58%) and Canada (15%) with a median age of 38.1 years at baseline. During 45,192 person-years of follow-up, 72 cases of HCC and 375 other liver events occurred (crude incidence rate [95% confidence interval] 1.6 [1.3;2.0] and 8.6 [7.8;9.5] cases per 1,000 person-years of follow-up, respectively). At diagnosis of HCC or other liver event, median age was 49.6 and 43.9 years and aspartate aminotransferase-to-platelet ratio index (APRI) was 1.8 and 2.5, respectively. The crude incidence rate of HCC increased over the study period (average change per calendar year [95% confidence interval] 11% [4%;19%]) whilst it decreased for other liver events (-4%, [-7%;-2%]). After adjustment for potential confounders (Figure), the significant decline in other liver events per calendar year of diagnosis remained, whereas the trend for HCC did not.

Conclusion: While other clinical liver events are declining, the incidence rate of HCC remains stable after adjusting for possible confounders. Cirrhosis, hepatitis B virus co-infection, and low CD4 cell count independently predicted both







Romania: (R Radoi), C Oprea, Spitalul de Boli Infectioase si Tropicale: Dr. Victor Babes, Bucarest. Russia: (A Rakhmanova), Medical Academy Botkin Hospital, St Petersburg; A Rakhmanova, St Petersburg AIDS Centre, St Peterburg; T Trofimora, Novgorod Centre for AIDS, Novgorod, I Khromova, Centre for HIV/AIDS & and Infectious Diseases, Kaliningrad; E Kuzovatova, Nizhny Novgorod Scientific and Research Institute, Nizhny Novogrod. Serbia: (D Jevtovic), The Institute for Infectious and Tropical Diseases, Belgrade. Slovakia: A Shunnar, D Staneková, Dérer Hospital, Bratislava.Slovenia: (J Tomazic), University Clinical Centre Ljubljana, Ljubljana. Spain: (J González-Lahoz) S Moreno, J. M. Rodriguez, Hospital Ramon y Cajal, Madrid; B Clotet, A Jou, R Paredes, C Tural, J Puig, I Bravo, Hospital Germans Trias i Pujol, Badalona; JM Gatell, JM Miró, Hospital Clinic Universitari de Barcelona, Barcelona; P Domingo, M Gutierrez, G Mateo, MA Sambeat, Hospital Sant Pau, Barcelona;

|
| |
|
 |
 |
|
|