 |
 |
 |
| |
No Hepatitis Flares When HBsAg+ iPrEx Participants Stop TDF/FTC
|
| |
| |
IAS 2015, July 19-22, 2015, Vancouver
Mark Mascolini
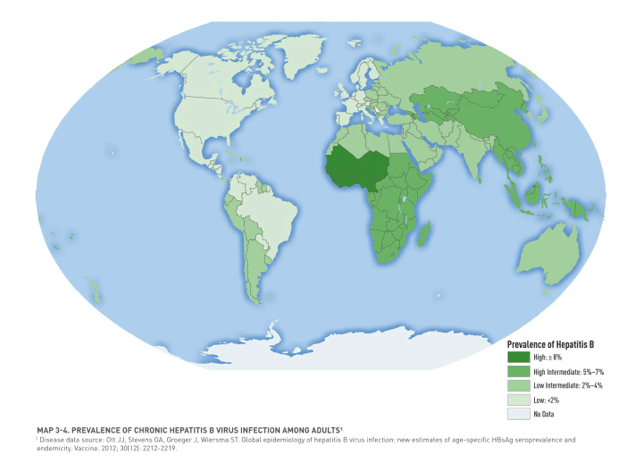
Hepatitis flares did not occur when hepatitis B surface antigen (HBsAg)-positive iPrEx participants with normal or near-normal transaminases stopped the two HBV-active drugs used in their PrEP pill, tenofovir (TDF) and emtricitabine (FTC) [1]. Few of these gay men or transgender women at high risk for HBV infection had been vaccinated against the hepatitis virus.
As preexposure prophylaxis (PrEP), coformulated TDF/FTC has prevented HIV infection in several studies of men who have sex with men (MSM) and heterosexual women and men, including iPrEx [2]. Both TDF and FTC are active against HBV, and stopping anti-HBV medications may allow HBV rebounds that can cause acute or chronic hepatic injury. Risk of such flares is lower with less advanced HBV infection. Stopping anti-HBV drugs may also allow HBV-resistant virus to emerge.
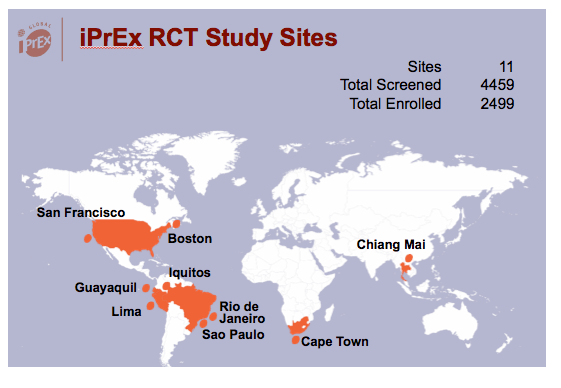
Other PrEP trials excluded HBsAg-positive people, but iPrEx enrolled HBsAg-positive participants if they had aspartate or alanine aminotransferase (AST or ALT) below 2 times the upper limit of normal and no clinical evidence of cirrhosis. HBsAg-positive iPrEx participants had extended follow-up 4, 8, and 12 weeks after stopping PrEP. The iPrEx team offered free HBV vaccination to all HBV-susceptible participants.
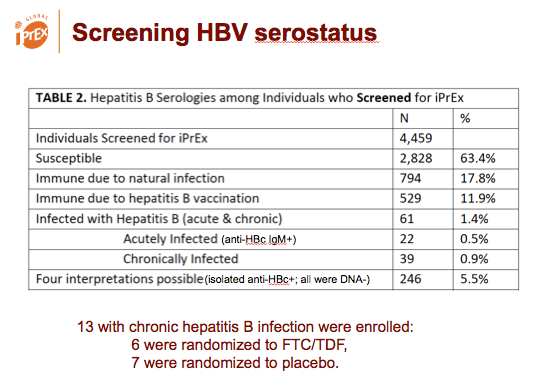
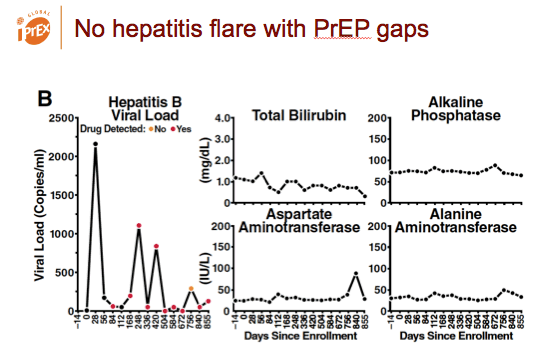
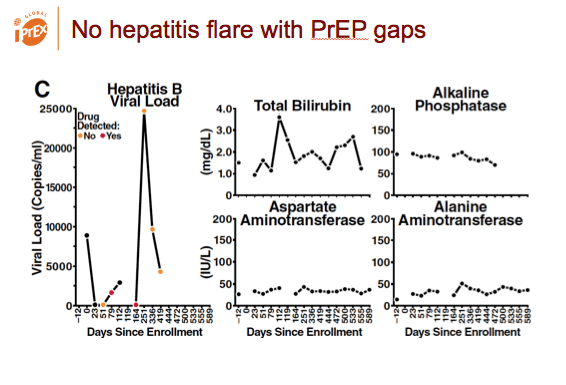
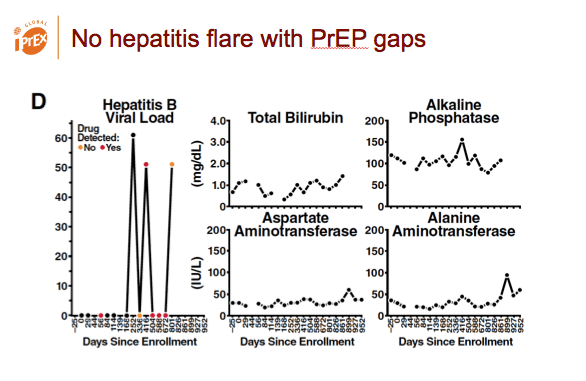
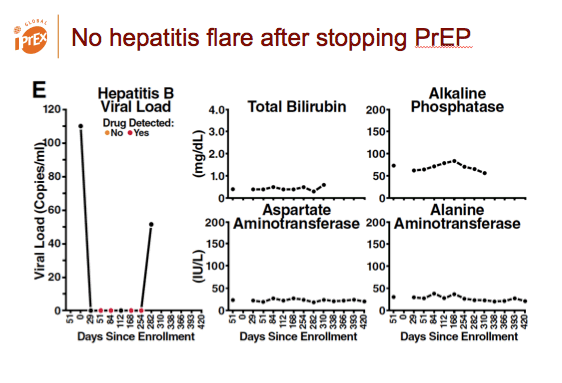
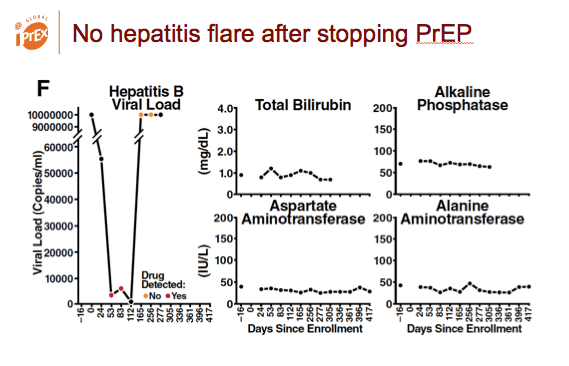
The trial enrolled 13 people with chronic HBV infection, 6 of whom got randomized to the TDF/FTC arm. During the trial no hepatitis flares occurred during gaps in PrEP dosing. After TDF/FTC PrEP stopped, all liver function tests remained within normal limits except for one grade 1 AST/ALT elevation.
Hepatitis did not flare after PrEP stopped.
Four iPrEx participants, 2 of them in the TDF/FTC arm, had evidence of acute HBV infection upon enrollment in the trial. Both participants had grade 4 transaminase jumps by study week 4, and both elevations resolved.
The iPrEx team used population sequencing to look for HBV-resistant virus in participants with measurable HBV DNA during the trial. They detected no evidence of HBV resistance to TDF or FTC.
Among 1633 iPrEx participants eligible for HBV vaccination, 1587 (97%) got at least one dose and 1382 (85%) got all three doses. Proportions immune (anti-HBs-positive) after 1, 2, and 3 doses were 44.4%, 74.5%, and 86.9%. The researchers concluded that PrEP provides an opportunity for HBV vaccination in this vulnerable population. HBV vaccination rates were low at screening, they noted, "yet uptake and efficacy were high when offered" free of charge.
The iPrEx team proposed that "HBsAg-positive persons with normal or near normal AST and ALT have a very low risk of hepatitis B flare when stopping HBV-active medications." They suggested that HBsAg screening only delays PrEP "and provides unclear safety benefits."
References
1. Solomon MM, Schechter M, Liu AY, et al. The safety of HIV pre-exposure prophylaxis in the presence of hepatitis B infection. IAS 2015. 8th Conference on HIV Pathogenesis, Treatment and Prevention. July 19-22, 2015. Vancouver. Abstract TUAC0201.
2. Grant RM, Lama JR, Anderson PL, et al. Preexposure chemoprophylaxis for HIV prevention in men who have sex with men. N Engl J Med. 2010;363:2587-2599.
-------------------
Reported by Jules Levin







|
| |
|
 |
 |
|
|