 |
 |
 |
| |
A Prospective Study of The Association of Body Morphometry With Hepatic Steatosis and Fibrosis in HIV-HCV Coinfected Patients
|
| |
| |
Reported by jules Levin
AASLD 2016 Nov 11-15 Boston, MA
C.M. Awad, T.A. Nguyen, P. Puri, A.J. Sanyal, V.A. Luketic, R. Stravitz , M.S. Siddique, I. Bouneva, R.K. Sterling, Virginia Commonwealth University , Richmond, Virginia, UNITED STATES

Program Abstract
Background: Hepatic steatosis is prevalent in those with HIV-HCV and may affect the the natural history and reduce the response to anti-HCV therapy. Abnormal body morphometry (BM) is common in those with HIV. However, its association with steatosis and fibrosis in HIV-HCV has not been defined.
Aim: To determine the prevalence and association between BM measures and steatosis and fibrosis in HIV-HCV patients (pts).
Methods: In this prospective study, data from HIV-HCV pts seen were analyzed. At the time of biopsy, demographic, laboratory and clinical data on the presence or absence of diabetes (DM) and hypertension (HTN) were recorded. BMI, waist circumference (WC), % body fat by anthropomorphic skin fold (SF) and bioimpedience (BI) measurements were obtained by a registered dietician. Histology was assessed for steatosis (Brunt) and fibrosis (Ishak) scores blinded to clinical data. Univariate analyses were used to determine associations with the presence of steatosis (>5%) and advanced fibrosis (bridging fibrosis or cirrhosis). Multivariate logistic regression analyses were used to control for confounders including age, sex, race, and HCV genotype (GT).
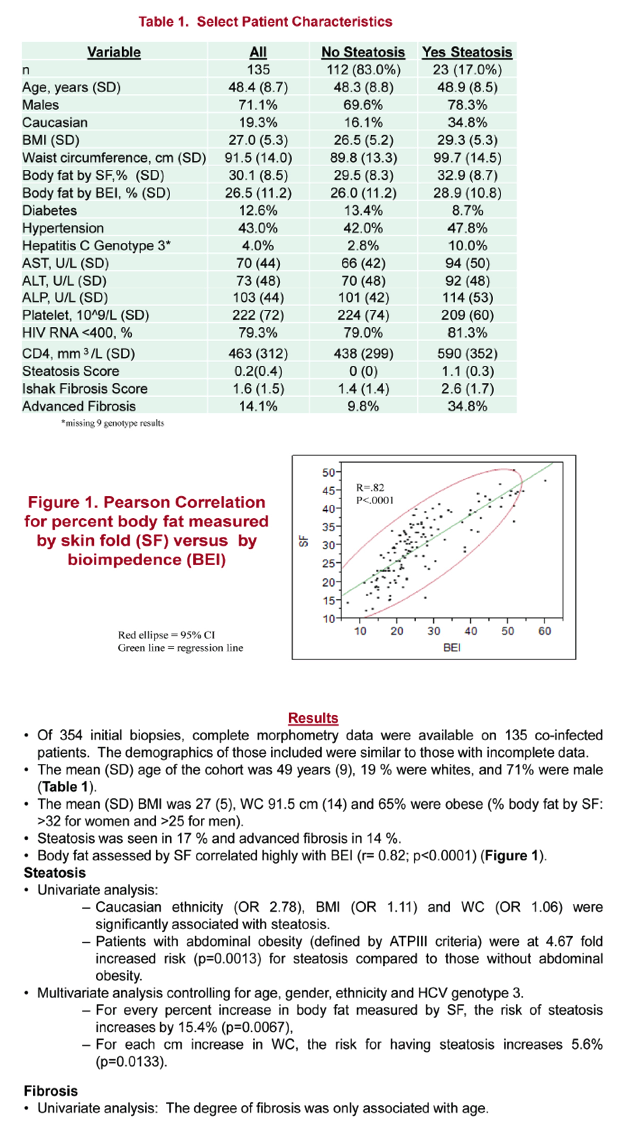
Results: Of 354 initial biopsies, complete BM data were available on 135 pts. Those included were similar to those with incomplete data. The mean (SD) age of the cohort was 49 (9) years, 19% were whites, and 71% were male. BM showed the mean (SD) BMI of 27 (5), WC 91.5 (14) cm and 65% were obese (% body fat by SF: >32 for women and >25 for men). Steatosis (>5%) was seen in 17% and advanced fibrosis in 14%. Body fat assessed by SF correlated highly with BI (r= 0.82; p<0.0001). On univariate analysis, steatosis was associated with white race (OR 2.78), increasing BMI (OR 1.1) and WC (OR 1.05). On multivariate analysis, for every % increase in body fat by SF, the risk of steatosis increases by 16% (p=0.005), and for each cm increase in waist, the risk for having steatosis increases 5.6% (p=0.0039). Pts with abdominal obesity were at 6.62 fold increased risk for steatosis compared to those without abdominal obesity defined by ATPIII criteria. On a univariate analysis, degree of fibrosis was only associated with age.
Conclusions: Abnormal BM and obesity were common in our HIV-HCV cohort. Body fat assessed by SF correlated highly with BI supporting its use in clinical practice. Abnormal BM, assessed by SF, WC, and BMI were independently associated with steatosis but not associated with advanced fibrosis. Future studies on the impact of improved body morphometry and weight reduction on steatosis and its impact on the natural history of HCV in HIV coinfection are needed.

|
| |
|
 |
 |
|
|