| |
Darunavir + Genvoya [elvitegravir/cobi/FTC/TAF] in Treatment-Experienced Patients with HIV Drug Resistance
|
| |
| |
Download the PDF here
Strategic Simplification: The Efficacy and Safety of Switching to Elvitegravir/Cobicistat/Emtricitabine/Tenofovir Alafenamide (E/C/F/TAF) Plus Darunavir (DRV) in Treatment-Experienced HIV-1-Infected Adults.....http://www.natap.org/2015/IDSA/IDSA_12.htm
Aging Workshop/2016: Efficacy and Safety of Co-formulated Elvitegravir, Cobicistat, Emtricitabine, and Tenofovir Alafenamide in Geriatric Adults with Renal Impairment Similar E/C/F/TAF Safety and Efficacy in Old vs Younger With Renal Impairment - Geriatric patients - (09/29/16)
Week 96 Efficacy and Safety of Tenofovir Alafenamide (TAF) vs Tenofovir Disoproxil Fumarate (TDF) in Older HIV-Infected Virologically-Suppressed Adults - eGFR ≥50 - (09/29/16)
Week 96 Efficacy and Safety of Tenofovir Alafenamide (TAF) vs Tenofovir Disoproxil Fumarate (TDF) in Older, HIV-Infected Treatment-Naïve Adults - (09/29/16)
------------------------------
A Randomized, Open-Label Trial to Evaluate Switching to Elvitegravir/Cobicistat/Emtricitabine/Tenofovir Alafenamide Plus Darunavir in Treatment-Experienced HIV-1-Infected Adults
The goal of our phase 3, open-label, randomized trial (GS-US-292-0119) was to evaluate the efficacy, safety, and PK parameters of switching virologically suppressed participants with a history of treatment failure to a 2-tablet, once-daily antiretroviral regimen combining E/C/F/TAF plus DRV. We report results though week 48.
Of the 199 screened participants, 135 enrolled and received at least one dose of study drug (89 randomized to switch to E/C/F/TAF plus DRV, 46 randomized to remain on their baseline regimen) (Fig. 1). Fewer participants in the E/C/F/TAF plus DRV group prematurely discontinued study drug compared with the baseline regimen group (2% vs. 11%).
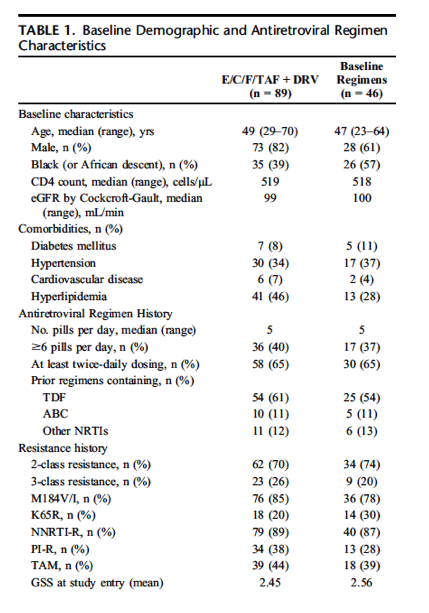
Comorbid conditions included hyperlipidemia (40%), hypertension (35%), diabetes mellitus (9%), and cardiovascular disease (6%). At baseline, participants were taking a median of 5 tablets per day (range, 2-10 tablets per day). Thirty-nine percent of participants were taking 6 or more tablets per day; 65% were taking at least one antiretroviral medication twice daily with 37% taking DRV twice daily. Overall, 59% of participants were on a TDF-based regimen, 11% on an abacavir-based regimen, and 57% on an integrase inhibitor. The distribution of genotypic susceptibility scores at study entry was similar across treatment groups.
All participants had at least 2-class genotypic resistance per eligibility criteria, the most prevalent being M184V/I for 95% of participants with nucleoside reverse transcriptase inhibitor mutations and K103N/S for 88% of participants with nonnucleoside reverse transcriptase inhibitor resistance-associated mutations (Supplemental Digital Content, Table 1, http://links.lww.com/QAI/A932). The tenofovir signature mutation K65R was present at 20% and 30% in the E/C/F/TAF plus DRV and baseline regimen groups. Participants with thymidine analogue mutations (up to 3) represented 44% and 39% of the E/C/F/TAF plus DRV and baseline regimen groups, respectively
E/C/F/TAF plus DRV was noninferior to baseline regimens for the primary outcome (HIV-1 RNA <50 copies per mililiter at week 24; FDA-snapshot algorithm) using the full analysis set (96.6% vs. 91.3%; difference 5.3%; 95.001% CI: -3.4% to 17.4%) (Fig. 3). Virologic success rates at week 24 using the per-protocol analysis set were consistent with the full analysis set (97.6% vs. 100.0%; difference -2.4%; 95.001% CI: -8.6% to 5.9%). At week 48, E/C/F/TAF plus DRV met the prespecified criteria for noninferiority and superiority using the full analysis set (94.4% vs. 76.1%, difference 18.3%; 95.001% CI: 3.5% to 33.0%) (Fig. 2), with consistent results using the per-protocol analysis set (97.6% vs. 85.4%; difference 12.3%; 95.001% CI: 1.8% to 26.4%). Through week 48, no participants discontinued because of lack of efficacy.
-----------------------------
A Randomized, Open-Label Trial to Evaluate Switching to Elvitegravir/Cobicistat/Emtricitabine/Tenofovir Alafenamide Plus Darunavir in Treatment-Experienced HIV-1-Infected Adults
AIDS Feb 1 2017 Huhn, Gregory D. MD, MPHTM; Tebas, Pablo MD, FIDSA; Gallant, Joel MD, MPH, FIDSA; Wilkin, Timothy MD, MPH; Cheng, Andrew MD, PhD; Yan, Mingjin PhD; Zhong, Lijie PhD; Callebaut, Christian PhD; Custodio, Joseph M. PhD; Fordyce, Marshall W. MD; Das, Moupali MD, MPH; McCallister, Scott MD
Abstract
Background: HIV-infected, treatment-experienced adults with a history of prior resistance and regimen failure can be virologically suppressed but may require multitablet regimens associated with lower adherence and potential resistance development.
Methods: We enrolled HIV-infected, virologically suppressed adults with 2-class to 3-class drug resistance and at least 2 prior regimen failures into this phase 3, open-label, randomized study. The primary endpoint was the percentage of participants with HIV-1 RNA <50 copies per milliliter at week 24 [Food and Drug Administration (FDA) snapshot algorithm].
Results: For 135 participants [elvitegravir/cobicistat/emtricitabine/tenofovir alafenamide (E/C/F/TAF) plus darunavir (DRV), n = 89; baseline regimen, n = 46], most of whom were taking a median of 5 tablets/d, simplification to E/C/F/TAF plus DRV was noninferior to continuation of baseline regimens at week 24 (plasma HIV-1 RNA <50 copies per milliliter: 96.6% vs. 91.3%, difference 5.3%, 95.001% CI: -3.4% to 17.4%). E/C/F/TAF plus DRV met prespecified criteria for noninferiority and superiority at week 48 for the same outcome. E/C/F/TAF plus DRV was well tolerated and had an improved renal safety profile compared with baseline regimens, with statistically significant differences between groups in quantitative total proteinuria and markers of proximal tubular proteinuria. Compared with baseline regimens, participants who switched to E/C/F/TAF plus DRV reported higher mean treatment satisfaction scale total scores and fewer days with missed doses.
Conclusions: This study demonstrated that regimen simplification from a 5-tablet regimen to the 2-tablet, once-daily combination of E/C/F/TAF plus DRV has durable maintenance of virologic suppression and improvements in specific markers of renal safety. Such a strategy may lead to greater adherence and improved quality of life.
INTRODUCTION
Morbidity and mortality in HIV infection have dramatically improved after the introduction of antiretroviral therapy (ART),1-3 even among patients with extensive treatment experience and multiclass drug resistance.4 With the approval of new drugs, particularly the integrase strand transfer inhibitors (INSTIs) and more potent protease inhibitors (PIs) [ie, darunavir (DRV)], construction of fully suppressive "salvage" regimens, containing at least 2 effective drugs from different classes, was possible.5 Despite these advances, "salvage" regimens are often complicated regimens with high pill burden, high dosing frequency, and/or dietary restrictions, factors resulting in higher cost, more side effects, poorer quality of life, and greater risk for nonadherence that may lead to virologic failure and accumulation of additional drug resistance.4,6 Current treatment guidelines recommend regimen simplification to maintain viral suppression if future treatment options are not compromised,7,8 but simplification is challenging in treatment-experienced patients with a history of drug resistance. Newer combination tablets enable simplification of these regimens; however, concerns of potential drug interactions in the absence of pharmacokinetic (PK) and pharmacodynamic data have limited their use.9
The single-tablet coformulation of elvitegravir/cobicistat/emtricitabine/tenofovir alafenamide (E/C/F/TAF) has demonstrated high efficacy and improved renal and bone safety compared with tenofovir disoproxil fumarate (TDF)-containing regimens in phase 3 clinical trials of HIV-infected participants.10-12 E/C/F/TAF has been approved by the United States (US) Food and Drug Administration (FDA), European Medicines Agency, and other health authorities for treatment of naïve and stably suppressed patients age 12 and older and is one of the recommended initial regimens in guidelines in the USA and in Europe.13-17 DRV is a recommended protease inhibitor with a high genetic barrier to resistance, well-established safety profile at a once-daily dose in treatment-experienced patients without DRV-associated resistance mutations, and can be boosted by either ritonavir or cobicistat.18,19 The 2-tablet, once-daily combination of E/C/F/TAF plus DRV may be an effective treatment option in select treatment-experienced patients with multiclass resistance. The goal of our phase 3, open-label, randomized trial (GS-US-292-0119) was to evaluate the efficacy, safety, and PK parameters of switching virologically suppressed participants with a history of treatment failure to a 2-tablet, once-daily antiretroviral regimen combining E/C/F/TAF plus DRV. We report results though week 48.
|
|
| |
| |
|
|
|