 |
 |
 |
| |
Hepatitis C Care in the Department of Veterans Affairs: HIT Process Improvement Program
|
| |
| |
Reported by Jules Levin
AASLD Annual Meeting 2017, Washington, DC, USA, October 20-24
Tim R. Morgan, MD
Rachel Gonzalez, MPH

The Hepatitis C Innovation Team Collaborative is a multi-disciplinary team-based approach grounded in Lean principles.
This was the brainchild of Dr. David Ross, Director of the HIV, Hepatitis and Related Conditions Program, part of VA's central administration. The execution of this program depends on the collaborative efforts and resources of many operational partners.
The NHCRC and VERC are charged with implementation of the program and supporting multi-disciplinary teams across all regions of the VA healthcare system.
A key component of the program is our ability to provide 'real-time' data to our clinicians and HITs in the field, thanks to VA;s Office of Population Health.
Evaluation team is small but mighty, analyzing the implementation strategies in place and providing feedback about what makes our program successful and where we have opportunities for improvement.
The #1 characteristic to take away from this is that the collaborative opened a consistent line of communication between executive leadership, operational partners, and clinicians.
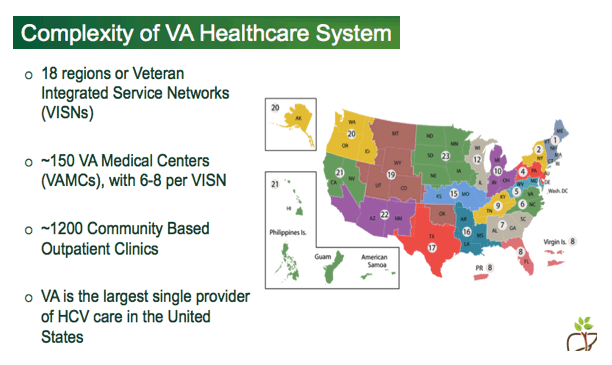
This is critical information when you recognize the breadth and complexity of VHA.
Veterans Health administration is organized into 18 regions or VISNs; it was re-organized within the last 18 months. I mention that as an example of the types of structural and policy changes that occur within VA and that the teams are equipped to adapt to, and adapt quickly, due to the open line of communication between partners.
A VAMC generally consists of an acute care hospital, outpatient clinics, diagnostic facilities, and support services.
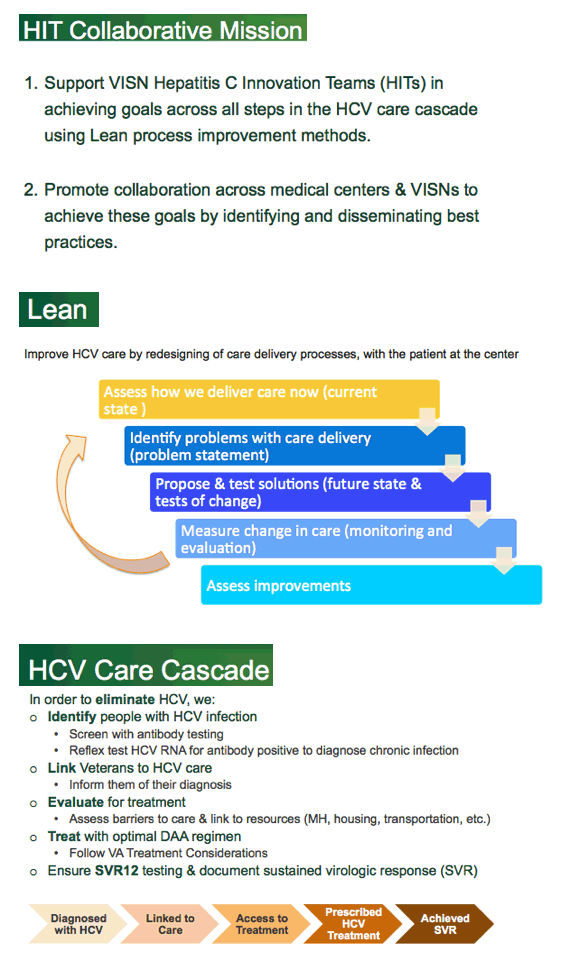
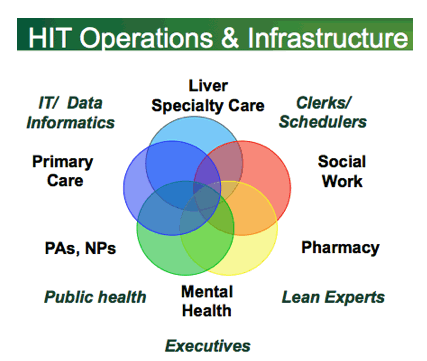

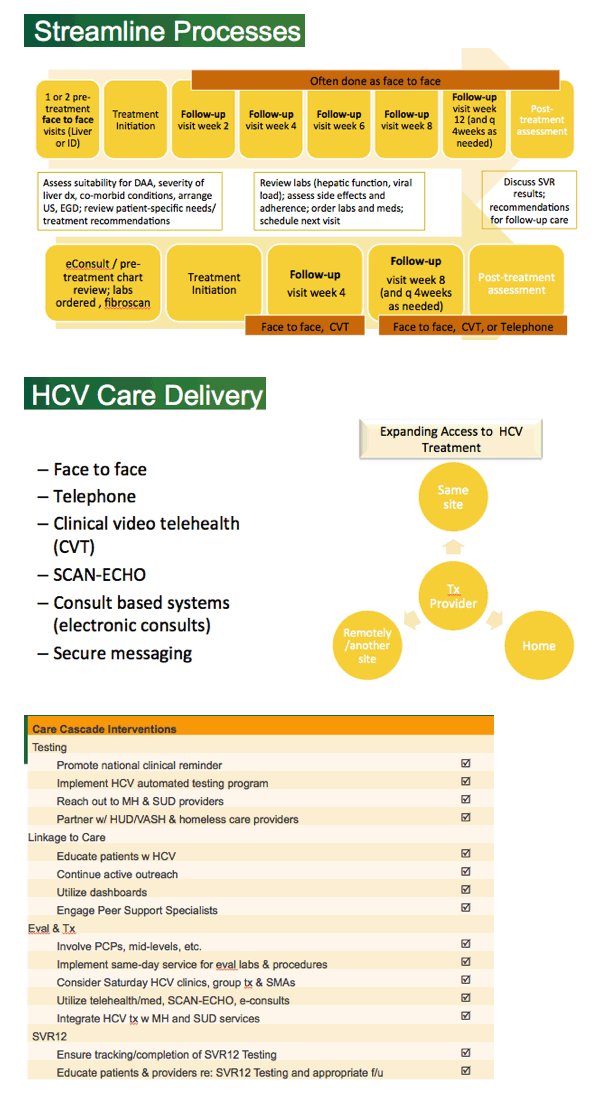


As results have been shared and disseminated, the most common question we're asked if "How can we replicate this?" For the most part our colleagues working with HCV patients are the ones asking, but this approach can be applied to innumerable clinical populations. To implement a process-improvement program, you need to know a few things.
Can you apply a population health approach by clearing defining the clinical problem? Can you identify these patients through a database or EHR? Do you have a mechanism to track progress? Does your organization truly respect people - does your organization trust the experience and insight of its clinicians? Do you value the knowledge of non-clinical stakeholders? Most importantly, does your team recognize that any change or improvement we make is ultimately made to improve the experience of the patients. I want to paraphrase Dr. James Rawson who said something that has stuck with me - It's going to be hard to put the patient in the center of health care if we're standing there ourselves.

|
| |
|
 |
 |
|
|