 |
 |
 |
| |
Raltegravir Switch and Biomarkers of Liver Steatosis and Metabolic Syndrome in Women
|
| |
| |
Reported by jules Levin
CROI 201 Feb 14-16 Seattle WA
Netanya S Utay1, David Reynoso1, AnomaSomasunderam1, MaitreyeeNigalye1, Judith S Currier2, Jordan E Lake2, 3
1University of Texas Medical Branch at Galveston, Galveston, TX, USA; 2University of California, Los Angeles, Los Angeles, CA, USA; 3University of Texas Health Science Center at Houston, Houston, TX, USA

Abstract Body:
Persons with well-controlled HIV infection on antiretroviral therapy (ART) are at risk for metabolic syndrome (MetS) and fatty liver disease. Hepatic steatosis and fibrosis and MetS have been associated with changes in circulating levels of adiponectin, soluble ST2 (sST2, or IL-33R), chitinase 3-like 1 (Chi3L1, or YKL40), hyaluronic acid (HA), TIMP-1, lysyl oxidase-like-2 and TGF-β in non-HIV-infected populations and animal models. Protease (PI) and non-nucleotide reverse transcriptase inhibitors (NNRTI) may contribute to MetS and other comorbidities. The effect of switching from PI- or NNRTI-based regimens to raltegravir-based regimens on these biomarkers is unknown.
Plasma was obtained from a completed, prospective trial of 37 women with lipohypertrophy and well-controlled HIV infection on NNRTI- or PI-based regimens who were randomized to immediate vs delayed (24 weeks) switch to raltegravir. We quantified the above biomarkers by ELISA and Multiplex assays at baseline and 24 weeks after randomization. Wilcoxon signed-rank test evaluated within group changes. We investigated correlations among biomarkers and clinical covariates with nonparametric (Spearman) and parametric (linear regression) analyses. Associations were also evaluated by regression modeling.
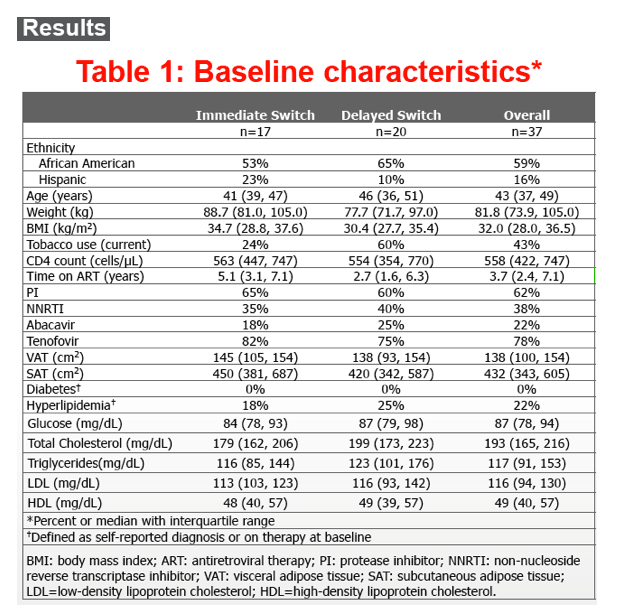
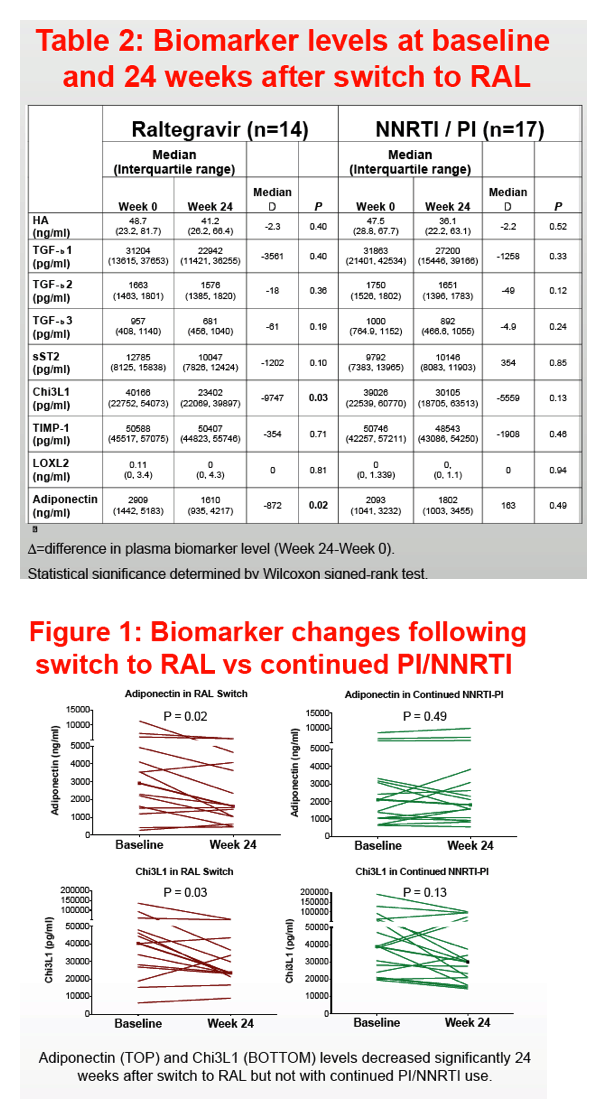
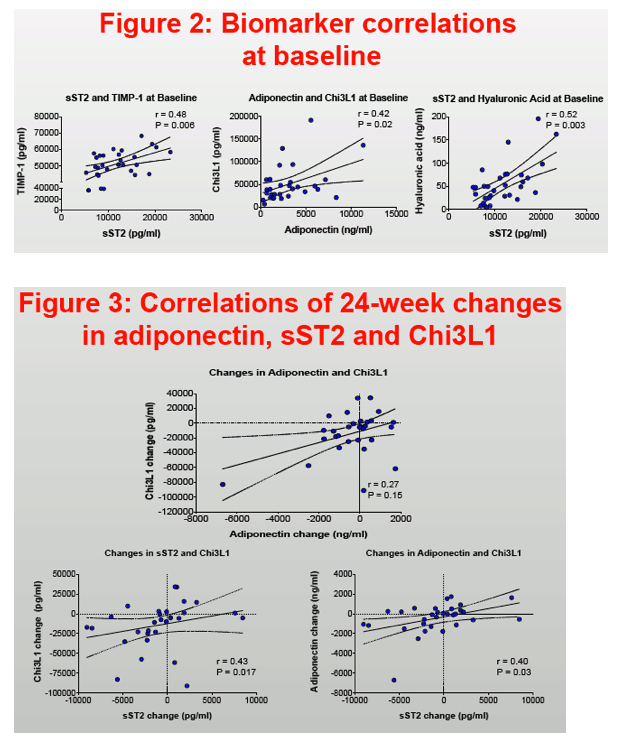
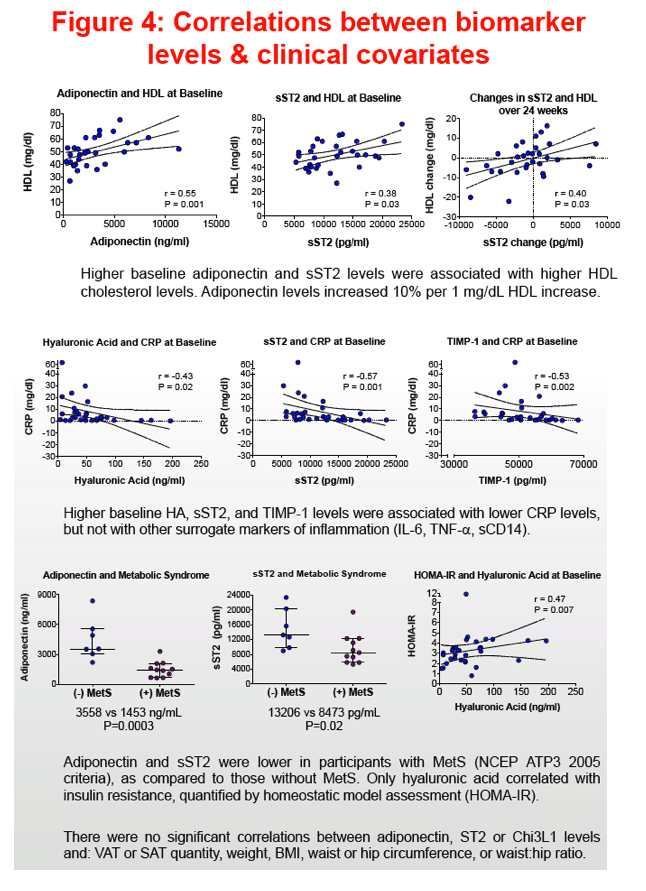
Participants had median age of 43 years, CD4 558 cells/mm3 and BMI 32 kg/m2; 35% met criteria for MetS. At baseline, higher adiponectin levels correlated with higher Chi3L1 levels (r=0.42, P=0.02), as did changes after 24 weeks (r=0.40, P=0.03). Baseline sST2 levels correlated with HA (r=0.52, P=0.003) and TIMP-1 levels (r=0.48, P=0.006); changes in sST2 correlated with changes in Chi3L1 (r=0.43, P=0.02) and adiponectin (r=0.40, P=0.03). Adiponectin and Chi3L1 levels decreased more in women switched to raltegravir immediately compared to those continuing NNRTI- or PI-based ART (Table). Other biomarkers did not change significantly. Adiponectin levels increased 10% per 1 mg/dL HDL increase. Adiponectin (1453 vs 3346 ng/ml, P=0.01) and sST2 (8473 vs 13206, P=0.02) were lower in participants with MetS vs without MetS. Adiponectin levels were also lower among women with higher subcutaneous adipose tissue volumes.
In women with HIV and lipohypertrophy, the hepatic steatosis/fibrosis marker Chi3L1 and the adipokine adiponectin decreased with switching to raltegravir. Whether switching from NNRTI/PI-based regimens to raltegravir would improve hepatic steatosis and dysmetabolism requires further study.

|
| |
|
 |
 |
|
|