 |
 |
 |
| |
COPD Markers Linked to Tripled Mortality Risk in People With HIV
|
| |
| |
Conference on Retroviruses and Opportunistic Infections (CROI), February 13-16, 2017, Seattle

Mark Mascolini
Markers of chronic obstructive pulmonary disease (COPD) raised chances of mortality up to 3-fold in an analysis of 196 veterans with HIV [1]. None of the markers assessed had a similar impact in 165 HIV-negative veterans.
Partly because smoking prevalence remains so high in HIV populations, COPD (which includes emphysema and chronic bronchitis [2]) has emerged as a growing concern. Because the impact of COPD on mortality in people with HIV remains uncertain, researchers working with the Veterans Aging Cohort Study (VACS) assessed mortality and pulmonary predictors in this group.
The analysis involved 196 HIV-positive and 165 smoking-matched HIV-negative people in the EXHALE substudy of the VACS. Participants were recruited between 2009 and 2012, and follow-up continued through September 2015. Researchers measured self-reported smoking status and pack-years, forced expiratory volume in 1 second (FEV1), forced vital capacity (FVC), diffusion capacity (DLCO), and emphysema (by chest CT). They defined airflow obstruction as FEV1/FVC below 0.7. For each participant, they also calculated the VACS index [3], which predicts mortality in people with HIV and incorporates age, CD4 count, HIV RNA level, HCV infection, and measures of organ dysfunction (hemoglobin, FIB-4, eGFR). To assess the independent impact of COPD markers on all-cause mortality, the investigators used Cox proportional hazards models adjusted for smoking pack-years, demographics, and the VACS index.
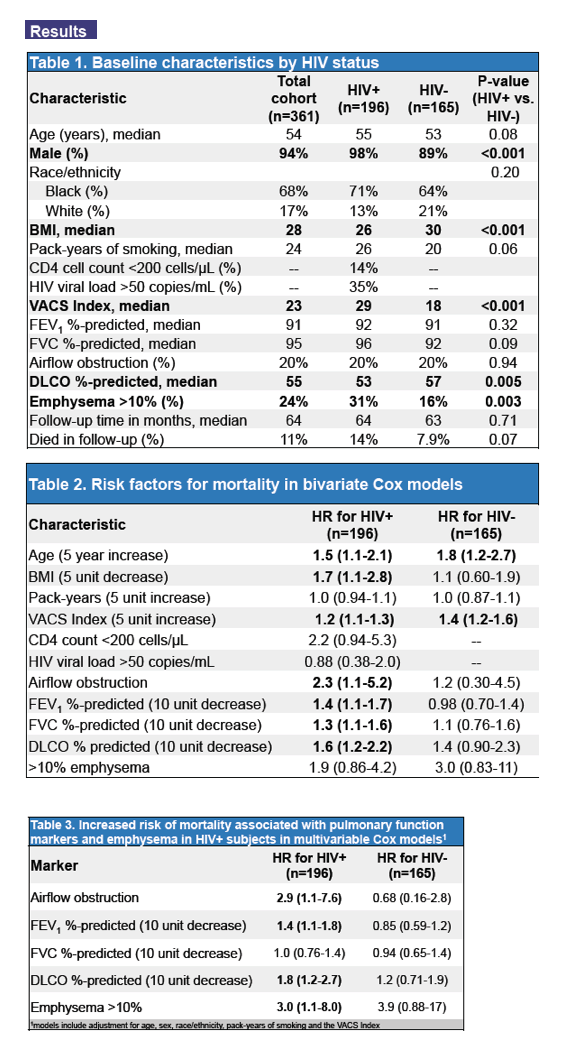
The HIV group was marginally older than the HIV-negative group (median 55 vs 53 years, P = 0.08), included a higher proportion of men (98% vs 89%, P < 0.001), and had a lower median body mass index (26 vs 30, P < 0.001), more pack-years of smoking (26 vs 20, P = 0.06), and a higher (worse) VACS index (29 vs 18, P < 0.001). FEV1, FVC, and airflow obstruction were statistically similar in veterans with and without HIV, but the HIV group had a lower (worse) DLCO (53% vs 57%, P = 0.005), and a higher proportion with emphysema (31% vs 16%, P = 0.003).
Through a median follow-up of 64 months, 14% with HIV and 7.9% without HIV died (P = 0.07). In bivariate Cox models, older age and higher VACS index were associated with mortality in both groups, while lower body mass index and four pulmonary function variables (FEV1, FVC, airflow obstruction, DLCO) were associated with mortality only in HIV-positive veterans.
The multivariable model identified associations between four pulmonary markers and greater risk of death in the HIV group but not in HIV-negative veterans, at the following adjusted hazard ratios (aHR) (and 95% confidence intervals):
-- Airflow obstruction: aHR 2.9 (1.1 to 7.6)
-- FEV1: aHR 1.4 (1.1 to 1.8)
-- DLCO: aHR 1.8 (1.2 to 2.7)
-- Emphysema >10%: aHR 3.0 (1.1 to 8.0)
The researchers conclude that markers of COPD are associated with mortality in HIV-positive people independent of the VACS index. They plan further work to examine these findings in a larger cohort and to determine whether adding pulmonary measures to the VACS index improves its ability to predict mortality.
References
1. Triplette M, Brown ST, Goet MB, et al. Chronic obstructive pulmonary disease and mortality in HIV. Conference on Retroviruses and Opportunistic Infections (CROI), February 13-16, 2017, Seattle. Abstract 658. http://www.croiconference.org/sites/default/files/posters-2017/658_Triplette.pdf
2. National Heart, Lung, and Blood Institute. What is COPD? https://www.nhlbi.nih.gov/health/health-topics/topics/copd
3. Veterans Aging Cohort study. VACS index information and VACS calculator. https://medicine.yale.edu/intmed/vacs/welcome/vacsindexinfo.aspx

Matthew Triplette,1 Sheldon T. Brown,2 Matthew Bidwell Goetz,3 Joon W. Kim,2 Maria C. Rodriguez-Barradas,4 Guy W. Soo Hoo,3
Cherry Wongtrakool,5 Kathleen Akgün,6 Amy Justice,6 Kristina Crothers1
1University of Washington, Seattle, WA, 2 James J. Peters VA Medical Center and Icahn School of Medicine at Mt. Sinai, New York, NY, 3 VA Greater Los Angeles Healthcare System and David Geffen School of Medicine at UCLA, Los Angeles, CA, 4 Michael E. DeBakey VAMC and Baylor College of Medicine, Houston, TX, 5 Atlanta VAMC, Decatur, GA and Emory University, Atlanta, GA, 6 VA Connecticut Healthcare System and Yale University, West Haven, CT

|
| |
|
 |
 |
|
|