 |
 |
 |
| |
More HIV/STI Testing, Fewer Risk Habits With Chemsex Program for London MSM
|
| |
| |
16th European AIDS Conference, October 25-27, 2017. Milan
Mark Mascolini
London men who have sex with men (MSM) engaging in chemsex (using recreational drugs to facilitate sex) significantly increased testing frequency for HIV and sexually transmitted infections (STIs) after participating in a behavioral intervention at Chelsea and Westminster hospital [1]. Men enrolled in the intervention reduced other signals of risky sex, including use of postexposure prophylaxis (PEP) and STI diagnoses.
MSM still account for most HIV transmissions in Western countries, despite making up a small minority of the population. Men who practice chemsex may be the subgroup at highest risk for HIV acquisition and transmission because of their many partners, rare condom use, traumatic sex practices, and increasing drug injection. Because chemsex MSM typically use STI clinics rather than substance use services, researchers tailored a culturally sensitive chemsex support service for use at their sexual health clinic.
Health workers began referring men to the chemsex program in October 2015. This analysis of high-risk behavior markers compared program attenders (more than 3 support sessions) with nonattenders (declined invitation to attend support sessions). From clinic records and questionnaires men completed 6 months before and 6 months after session attendance, researchers collected data on HIV testing and status, recreational drug use, condom-free anal sex, use of PEP and postexposure prophylaxis (PrEP), STI testing and diagnoses, and several behavioral variables.
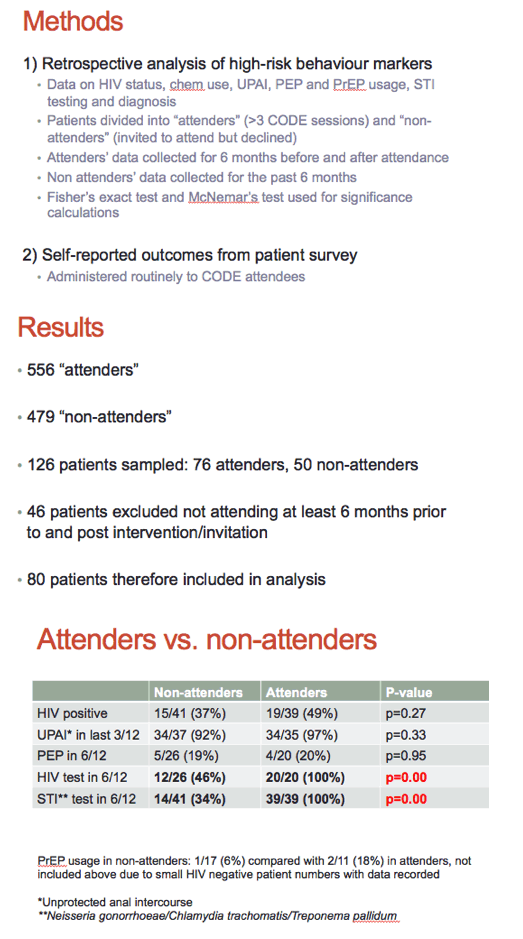
Overall there were 556 attenders and 479 nonattenders. The research team reviewed questionnaires from a sample of 76 attenders and 50 nonattenders. After excluding 46 men who did not complete questionnaires in the required timeframe, the researchers had 80 men for analysis, 39 attenders and 41 nonattenders.
A nonsignificantly higher proportion of attenders than non-attenders had HIV infection (49% versus 37%, P = 0.27) and a nonsignificantly higher proportion had condom-free sex in the last quarter (97% versus 92%, P= 0.33). Attenders were significantly more likely to have an HIV test in the last 6 months (100% versus 46%, P = 0.00) and to have an STI test in the last 6 months (100% versus 34%, P = 0.00).
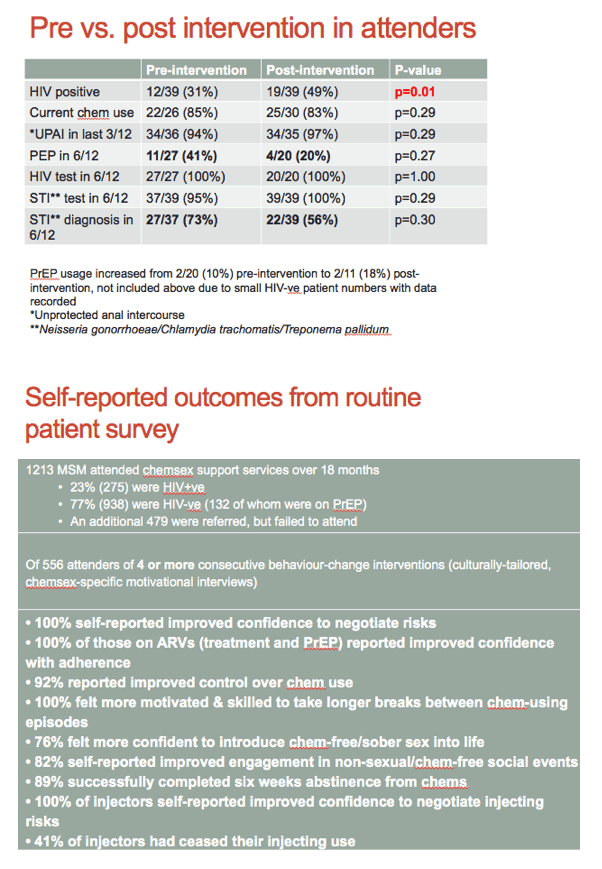
A pre- and postintervention comparison among the 39 attenders showed that HIV prevalence rose significantly from 31% to 49% (P = 0.01), probably because of the 100% HIV testing rate. PEP use in the past 6 months dropped nonsignificantly from 41% to 20% (P = 0.27), while STI diagnoses fell nonsignificantly from 73% to 56% (P = 0.30). The drop in PEP use may reflect a jump in PrEP use from 10% to 18%. Rates of chem use and condomless anal sex did not change from before to after the intervention in these 39 men.
Among all 1213 MSM who took advantage of the chemsex support intervention, 275 (23%) had HIV infection. Among the 938 men without HIV, 132 (14%) used PrEP. Among 556 men (46%) who attended 4 or more intervention sessions, after completing the sessions all reported improved confidence in negotiating risks, all taking antiretrovirals (for treatment or PrEP) reported improved confidence in adherence, all felt more motivated and skilled to take longer breaks between chemsex outings, and all drug injectors reported improved confidence in negotiating injection risks. In this group of 556 attenders, after the sessions 92% reported improved control over chem use, 89% went 6 weeks without chemsex, 82% reported improved engagement in nonsexual social events, 76% claimed greater confidence in practicing sober sex, and 41% of injectors stopped injecting.
The Chelsea and Westminster team concluded that this chemsex support intervention reduced risks behaviors and improved quality of life in MSM. The intervention also gave men a reason to attend the clinic consistently, which enabled regular testing for HIV and STIs.
Reference
1. Stuart D, Atefi D, Zdravkov J, et al. Outcomes of behavioral interventions in men who have sex with men (MSM) engaging in chemsex.16th European AIDS Conference. October 25-27, 2017. Milan. Abstract PS12/3.

|
| |
|
 |
 |
|
|