 |
 |
 |
| |
Effects of Moderate and Vigorous Exercise on Nonalcoholic Fatty Liver DiseaseA Randomized Clinical Trial - NASH, hypertension, lipids, liver enzymes, weight loss
|
| |
| |
Download the PDF here
Download the PDF here
Download the PDF here
- evaluatesmoderate& vigorous exercise affects on
intrahepatictriglyceridecontact(NASH, fatty liver), and other important measures including hypertension, lipids, weight loss etc....."This study makes an important contribution to our understanding of the therapeutic effect of regular exercise in people with NAFLD. The data demonstrate that long-term (1-year) regular endurance exercise causes a sustained decrease in IHTG content.Moreover, by adjusting for changes in body weight among treatment groups, their results suggest that the effect of exercise on IHTG was mediated by both a decrease in body weight and a weight loss-independent effect of exercise itself.However, the calculated effect of exercise alone on IHTG content was small, accounting for around a 2% decline in IHTG content at 12 months, and neither exercise intervention had an effect on serum alanine transaminase concentration......Changes in serum alanine transaminase and γ-glutamyl transferase levels did not significantly differ among the 3 groups during the 6- or 12-month intervention. However, serum aspartate aminotransferase was significantly increased in the vigorous exercise group compared with the moderate exercise group during the 6-month intervention"
There are 2 commentaries enclosed here on the 1 main study: 1st commentary titled & below: "Moderate Exercise for Nonalcoholic Fatty Liver Disease"
2nd COMMENTARY - "Exercise and NAFLD: Is it worth the effort?"
"This trial represents the largest and longest duration exercise study in people with NAFLD (Table1).....This study makes an important contribution to our understanding of the therapeutic effect of regular exercise in people with NAFLD. The data demonstrate that long-term (1-year) regular endurance exercise causes a sustained decrease in IHTG content. Moreover, by adjusting for changes in body weight among treatment groups, their results suggest that the effect of exercise on IHTG was mediated by both a decrease in body weight and a weight loss-independent effect of exercise itself.However, the calculated effect of exercise alone on IHTG content was small, accounting for around a 2% decline in IHTG content at 12 months, and neither exercise intervention had an effect on serum alanine transaminase concentration. These results are consistent with data from previous randomized, controlled trials, which have shown that exercise training without weight loss has small, albeit statistically significant, effects on IHTG content (Table1) and does not affect serum alanine transaminase concentrations.[6]......Clearly, endurance exercise does decrease IHTG content, but the effect is likely to be small unless there is concomitant weight loss. Therefore, weight loss is the key lifestyle intervention component that is needed to effectively reduce IHTG content and improve liver histology in patients with NAFLD.....physical activity has considerable health benefits for people at high risk for cardiometabolic diseases, because endurance and resistance exercise increase insulin sensitivity and decrease the risk of developing diabetes or dying from coronary heart disease"
-----------------------
Full Study - "Effects of Moderate and Vigorous Exercise on Nonalcoholic Fatty Liver DiseaseA Randomized Clinical Trial"
Discussion
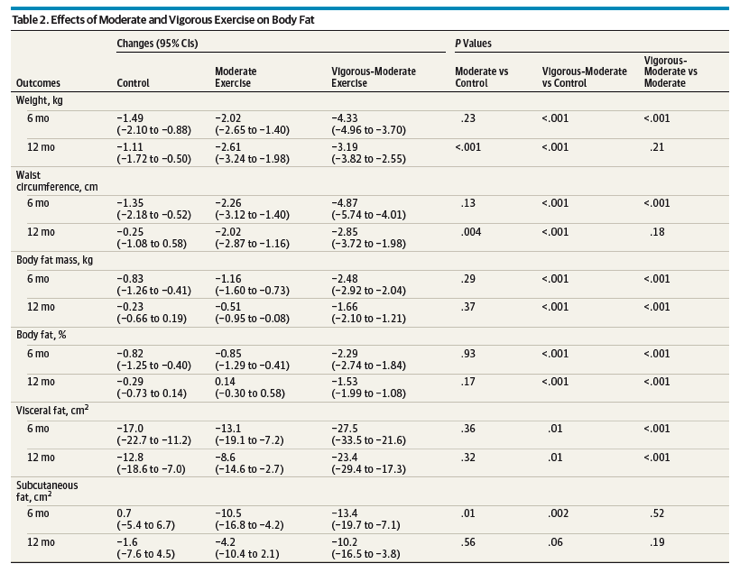
This randomized clinical trial contributes novel findings on the effects of exercise on NAFLD in several aspects. First, this study indicated that vigorous exercise at 65% to 80% of the maximum heart rate and moderate exercise at 45% to 55% of the maximum heart rate for 150 minutes per week are equally effective in reducing the IHTG content among patients with central obesity and NAFLD. Second, most but not all of the effect was mediated by weight loss. Third, only vigorous exercise reduced weight, waist circumference, body fat, and blood pressure at 6 months compared with control. However, moderate exercise reduced weight, waist circumference, and blood pressure but not body fat at 12 months compared with control. Fourth, exercise seems less effective on glucose and lipid reduction in this study population. These findings have important clinical and public health implications.
Several small clinical trials6-10 assessed the effect of short-term exercise programs on the IHTG content among patients with NAFLD. Johnson and colleagues6 reported that a 4-week supervised, progressive aerobic exercise program reduced the IHTG content by 21% (P < .05) in 12 sedentary obese adults compared with 7 no-exercise controls. Sullivan et al7 found that moderate exercise for 16 weeks resulted in a 10.3% decrease in the IHTG content in 12 obese persons with NAFLD compared with 6 control patients (P < .05). In addition, Keating and colleagues8tested the effects of 3 intervention programs with various levels of intensity and dose of aerobic exercise on the IHTG content in an 8-week clinical trial among 48 sedentary overweight or obese adults and documented that all aerobic exercise regimens reduced liver fat with no difference by dose or intensity. In contrast, Shojaee-Moradie et al9 reported no difference in liver fat during a 6-week exercise program in 10 sedentary overweight men compared with 7 controls. However, these small short-term trials were not able to provide dose-response information to formulate evidence-based clinical guidelines regarding exercise programs in patients with NAFLD.
To our knowledge, this study is the first randomized clinical trial to compare the long-term effect of moderate and vigorous exercise on NAFLD. This trial indicated that moderate and vigorous exercise programs have similar effects on liver fat reduction among obese patients with NAFLD. These results support the current physical activity guidelines (150 minutes of moderate-intensity activity per week) for the management of NAFLD.11-13 Because moderate exercise is more sustainable and provides most of the benefit of vigorous exercise, it should be recommended for the prevention and treatment of NAFLD.
Weight loss via lifestyle intervention has been documented to play a role in reducing liver fat, and a weight loss of 5% or more seems to be desirable for improving NAFLD.21 In this trial, exercise programs resulted in a 3% to 6% weight loss, whereas they reduced relative liver fat by 35% to 40% among patients with NAFLD. After adjustment for weight loss, exercise interventions were no longer significantly associated with IHTG content reduction (except for moderate exercise at 6 months) at a predefined significance level of .008. These findings suggest that the effect of the exercise intervention on the IHTG content reduction was most likely mediated by weight loss.
Although exercise has been recommended as an important weight loss strategy, the exercise intensity required to achieve optimal benefit continues to be the source of considerable uncertainty and debate. Moderate-intensity aerobic exercise has been documented to induce modest reductions in weight and waist circumference in overweight and obese populations.22 However, there is little conclusive evidence for more favorable effects with high-intensity exercise than with moderate-intensity exercise on weight loss.23 Jakicic and colleagues24 compared the effects of different durations and intensities of exercise on 12-month weight loss in a randomized trial of 201 sedentary overweight women.
Significant weight loss was achieved among all exercise groups with no differences based on exercise durations and intensities. Ross and colleagues25 also reported no difference in waist circumference reduction according to exercise amount and intensity in a 24-week randomized trial among 217 abdominally obese adults. Our data indicated that vigorous but not moderate exercise significantly reduced body weight and waist circumference during the 6-month intervention. However, moderate exercise significantly reduced body weight and waist circumference during the 12-month intervention. Our study suggests that short-term vigorous exercise and long-term moderate exercise programs could be recommended for weight reduction in obese individuals.
In this trial, vigorous but not moderate exercise significantly reduced body fat and visceral fat. A meta-analysis26 of clinical trials suggests that there seems to be a threshold for exercise intensity to have an effect on the reduction of visceral fat. Several clinical trials27-29 indicated that vigorous or moderate to vigorous exercise reduced visceral fat, whereas another trial26 found that low to moderate exercise did not reduce visceral fat. Irving and colleagues30 compared the effect of low-intensity and high-intensity aerobic exercise with a no-exercise control on abdominal adiposity among 27 obese women and reported that only high-intensity exercise reduced abdominal fat and visceral fat during a 16-week intervention. Our study is the first large trial, to our knowledge, to compare the effect of moderate and vigorous exercise on visceral fat reduction. Our study suggests that vigorous exercise may be required for reducing visceral fat among obese individuals.
Our study finding that aerobic exercise reduced blood pressure was consistent with previous clinical trials.31 However, exercise did not significantly reduce lipid or glucose levels in our study. Previous clinical trials32,33 also reported inconsistent effects of aerobic exercise on low-density lipoprotein cholesterol, high-density lipoprotein cholesterol, and glucose levels in participants without dietary intervention.
This study has some limitations. First, to test the effect of transitioning from vigorous to moderate exercise on NAFLD, the vigorous exercise intervention lasted for only 6 months. Future trials should compare the long-term effects of vigorous and moderate exercise on the IHTG content and metabolic risk factors among patients with NAFLD. Second, the primary outcome was the IHTG content instead of biopsy-proven fibrosis or steatosis.
However, the IHTG content measured by magnetic resonance spectroscopy is highly reproducible and correlated with the histologic features of fibrosis and steatosis.34,35 Magnetic resonance spectroscopy is regarded as the most accurate noninvasive method of measuring liver fat among patients with NAFLD in clinical practice.36 In addition, the IHTG content is more sensitive than the steatosis grade determined by histologic analysis in quantifying changes in liver fat content and has been recommended for this specific use in clinical trials.37 In our study, magnetic resonance spectroscopy was performed using a standard protocol based on 1.3-ppm lipid methylene protons to avoid measurement variations.38 Third, dietary calorie and fat intake were not controlled in this study because we aimed to examine isolated effects of exercise on NAFLD. Future clinical trials should examine the effects of combined intervention strategies on long-term outcomes of NAFLD.
Conclusions
This study indicates that vigorous and moderate exercise were equally effective in reducing IHTG content, whereas vigorous exercise might have additional benefits in reducing weight, body fat, and blood pressure among patients with NAFLD. For individuals who might have difficulty engaging in vigorous exercise, moderate exercise would have the same effects on the prevention and treatment of NAFLD. Most of the effect of the interventions on the IHTG content appeared to be mediated by weight loss.
Meaning Vigorous and moderate exercise was equally effective in reducing intrahepatic triglyceride content among patients with nonalcoholic fatty liver disease.
Body weight, waist circumference, and blood pressure were significantly reduced in the vigorous-moderate exercise group compared with the moderate exercise and control groups at the 6-month assessment and in the vigorous-moderate and moderate exercise groups compared with the control group at the 12-month assessment. In addition, body fat was significantly reduced in the vigorous-moderate exercise group compared with the moderate exercise and control groups at the 12-month assessment. After adjusting for weight loss, the net changes in intrahepatic triglyceride content were diminished and became nonsignificant between the exercise and control groups (except for the moderate exercise group at the 6-month assessment).....Conclusions and Relevance Vigorous and moderate exercise were equally effective in reducing intrahepatic triglyceride content; the effect appeared to be largely mediated by weight loss.
Metabolic Risk Factors
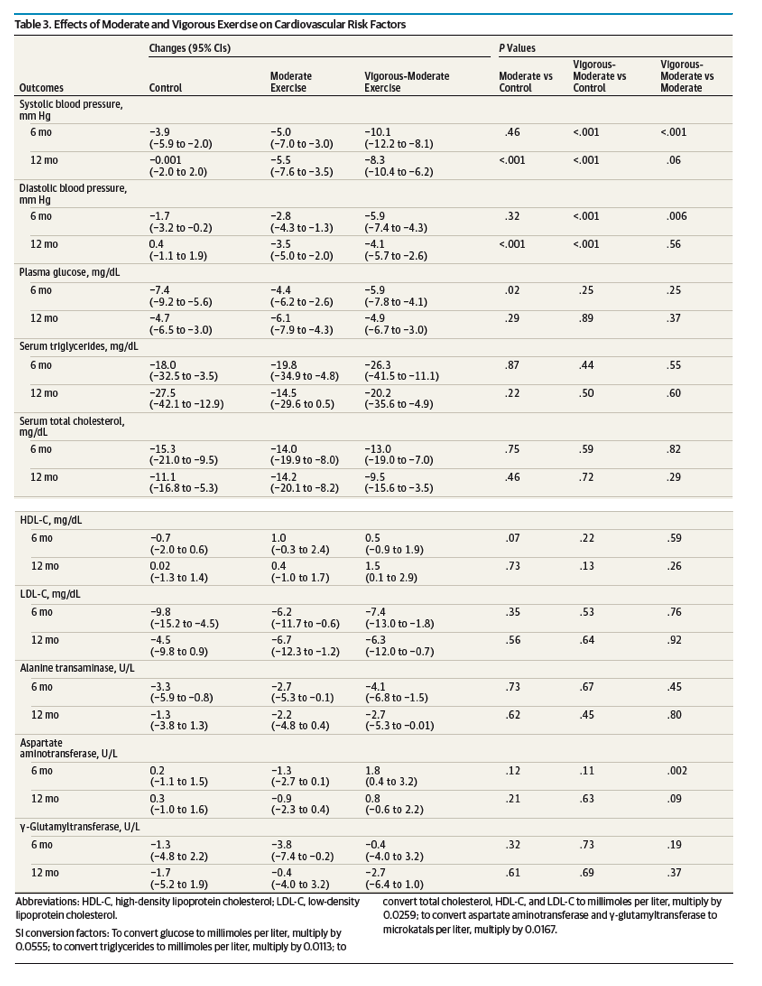
During the 6-month intervention, vigorous exercise significantly reduced systolic and diastolic blood pressure compared with control and moderate exercise (Table 3). During the 12-month intervention, moderate exercise and vigorous-moderate exercise significantly reduced blood pressure compared with control. Both vigorous and moderate exercise did not significantly reduce fasting glucose or lipid levels during the 6-month or 12-month intervention.
Liver Enzymes
Changes in serum alanine transaminase and γ-glutamyl transferase levels did not significantly differ among the 3 groups during the 6- or 12-month intervention. However, serum aspartate aminotransferase was significantly increased in the vigorous exercise group compared with the moderate exercise group during the 6-month intervention (Table 3).
Introduction
Nonalcoholic fatty liver disease (NAFLD) has reached epidemic proportions worldwide and is the most common cause of chronic liver disease.1The condition affects 20% to 30% of adults in the general population and 70% to 90% of patients with obesity or diabetes in Western countries.1,2 In China, approximately 20% of adults in the general population have NAFLD.3 Nonalcoholic fatty liver disease is closely related to insulin resistance and metabolic risk factors (ie, abdominal obesity, hypertension, dyslipidemia, hyperglycemia).4 Furthermore, NAFLD has been associated with an increased risk of cardiovascular disease independent of metabolic risk factors.1
A retrospective clinical study5 indicated that vigorous but not moderate exercise was associated with a lower risk of steatohepatitis and advanced fibrosis in patients with biopsy-proven NAFLD. Several small clinical trials6-9 reported inconsistent findings of short-term exercise programs on intrahepatic lipids among patients with NAFLD. In addition, these studies did not provide dose-response information needed to formulate evidence-based clinical guidelines for NAFLD management. Furthermore, the long-term effect of current physical activity guidelines on NAFLD is uncertain.10-13
The current study aimed to compare the effects of moderate and vigorous exercise on intrahepatic triglyceride (IHTG) content and metabolic risk factors among patients with NAFLD. In addition, we also compared the effects of transitioning from vigorous to moderate exercise on IHTG and metabolic risk factors.
----------------------------
2nd COMMENTARY
Exercise and NAFLD: Is it worth the effort?
Hepatology11 October 2017
Nonalcoholic fatty liver disease (NAFLD) represents a spectrum of liver abnormalities, characterized by an increase in intrahepatic triglyceride (IHTG) content that can progress to inflammation and fibrosis. In addition, NAFLD is associated with an increased risk of serious cardiometabolic abnormalities, including atherogenic dyslipidemia, hypertension, metabolic syndrome, diabetes, and coronary heart disease.[1] Lifestyle therapy that is targeted toward decreasing energy intake and increasing physical activity is considered the cornerstone of therapy for patients with NAFLD. The liver is very responsive to calorie restriction and weight loss. Even 48 hours of consuming a low-calorie diet decreases IHTG content,[2] and progressive 5%, 11%, and 16% diet-induced weight loss decreases IHTG content by 15%, 50%, and 65%, respectively, in people with NAFLD and moderate steatosis (∼10% liver volume as triglyceride).[3] Moreover, 5%-10% weight loss improves most histological features of NAFLD, including NAFLD activity score, steatosis, inflammation, and ballooning, and �10% weight loss decreases hepatic fibrosis.[4] However, the type, intensity, and volume of exercise needed for optimal therapeutic effects in patients with NAFLD are not clear.
Recently, the results of a 12-month, randomized, controlled trial, conducted by Zhang et al. in Xiamen, China, that evaluated the effects of moderate and vigorous endurance exercise training on IHTG content and cardiometabolic risk factors in people with NAFLD was reported in JAMA Internal Medicine.[5] This trial represents the largest and longest duration exercise study in people with NAFLD (Table 1). A total of 220 men and women with NAFLD participated in this study (54% women; mean age, ∼54 years; mean body weight, ∼72 kg; mean BMI, ∼28 kg/m2; and mean IHTG content, ∼18%). Participants were randomized in a 1:1:1 allocation to one of the following three groups: (1) no-exercise control group (NE); (2) vigorous-moderate exercise group (V-ME), in which subjects performed supervised vigorous intensity exercise (jogging at 65%-80% of maximal heart rate) for 30 minutes, 5 days/week for 6 months followed by moderate-intensity exercise (brisk walking at 45%-55% of maximal heart rate) for 30 minutes, 5 days/week for 6 months; or (3) moderate intensity exercise group (ME), in which subjects performed supervised moderate intensity exercise for 30 minutes, 5 days/week for 12 months.
At 6 months, IHTG content decreased more in the V-ME (by 5.0%) and ME (by 4.2%) groups than in the NE control group, without a difference between the two exercise groups. At 12 months, the decline in IHTG content was also greater in the both the V-ME (by 3.8%) and ME (by 3.5%) groups than the NE control group, without a difference between the two exercise groups. Body weight in the V-ME, ME, and NE groups decreased by 4.3, 2.0, and 1.5 kg, respectively, at 6 months and by 3.2, 2.6, and 1.1 kg, respectively, at 12 months. The significance of the beneficial effect of exercise training on IHTG content at 6 and 12 months remained after adjusting for changes in body weight. Serum alanine transaminase concentrations did not change in any group after 6 or 12 months of intervention.
This study makes an important contribution to our understanding of the therapeutic effect of regular exercise in people with NAFLD. The data demonstrate that long-term (1-year) regular endurance exercise causes a sustained decrease in IHTG content. Moreover, by adjusting for changes in body weight among treatment groups, their results suggest that the effect of exercise on IHTG was mediated by both a decrease in body weight and a weight loss-independent effect of exercise itself. However, the calculated effect of exercise alone on IHTG content was small, accounting for around a 2% decline in IHTG content at 12 months, and neither exercise intervention had an effect on serum alanine transaminase concentration. These results are consistent with data from previous randomized, controlled trials, which have shown that exercise training without weight loss has small, albeit statistically significant, effects on IHTG content (Table 1) and does not affect serum alanine transaminase concentrations.[6]
There are several issues that need to be considered in translating the results from the study by Zhang et al. into clinical practice. First, the moderate and vigorous exercise training intervention in this study are identical to the lowest and highest range of exercise intensity and volume recommended by the Department of Health and Human Services, the American College of Sports Medicine, and the American Heart Association to achieve health benefits in adults. Therefore, the exercise interventions tested in this study are already recommended for all adults, with or without NAFLD. Second, physical activity has considerable health benefits for people at high risk for cardiometabolic diseases, because endurance and resistance exercise increase insulin sensitivity and decrease the risk of developing diabetes or dying from coronary heart disease.[7] Third, the study by Zhang et al. was conducted in an Asian population, which is known to be at increased risk of developing NAFLD at much lower body mass index (BMI) values than white, Hispanic, and black populations.[8] Therefore, it is not known whether the results from this study apply to other ethnic/racial groups. Nonetheless, the consistency of their results with those of previous studies, as summarized in Table 1, suggest that their findings are likely relevant to other populations. Fourth, compliance with the exercise intervention in the study by Zhang et al. was extraordinary because of comprehensive supervision and monitoring, which is not practical in a typical clinical setting; more than 90% of participants in the ME and V-ME groups participated in 80% or more of the exercise sessions. Finally, the importance of the exercise interventions studied by Zhang et al. in the management of NAFLD cannot be fully appreciated without an evaluation of the histological features of NAFLD that determine disease severity.
What can be learned from this study that affects the clinical management recommendations for patients with NAFLD? Despite the considerations noted in the previous paragraph, the results from the study by Zhang et al., in conjunction with the data from previous randomized, controlled trials, help put the role of endurance exercise in proper perspective with some good and bad news. Moderate endurance exercise (brisk walking, 30 minutes/day, 5 days/week) is probably just as good as vigorous endurance exercise (jogging, 30 minutes/day, 5 days/week) in reducing IHTG content. However, even though most people are more likely to adhere to a moderate-intensity than a vigorous-intensity exercise program,[9] adherence with any exercise intervention is often poor and the compliance achieved by Zhang et al. is unlikely to occur in real life. Clearly, endurance exercise does decrease IHTG content, but the effect is likely to be small unless there is concomitant weight loss. Therefore, weight loss is the key lifestyle intervention component that is needed to effectively reduce IHTG content and improve liver histology in patients with NAFLD.
George G. Schweitzer,
Ph.D.Samuel Klein, M.D.
Center for Human Nutrition
Washington University School of Medicine
St. Louis, MO
-----------------------
1st Commentary
Invited Commentary
Less Is More
August2016
Moderate Exercise for Nonalcoholic Fatty Liver Disease
JAMA Intern Med. 2016;176(8):1083-1084. doi:10.1001/jamainternmed.2016.3221
Long-term nutritional excess coupled with reduced physical activity has fueled the rise of obesity-related metabolic conditions. In many countries with high population density, overnutrition is now responsible for more morbidity than undernutrition. Nonalcoholic fatty liver disease (NAFLD) is 1 of the consequences of the imbalance between caloric intake and expenditure and is a leading cause of chronic liver disease, affecting up to 30% of the world's population. Nonalcoholic fatty liver disease is associated with significant morbidity, particularly for those with the progressive version nonalcoholic steatohepatitis. Nonalcoholic steatohepatitis may progress to cirrhosis, with mortality primarily driven by cardiovascular disease and malignant tumors. Nonalcoholic fatty liver disease is strongly associated with visceral obesity and may contribute independently to the development of other metabolic conditions, such as diabetes, cardiovascular disease, and hyperlipidemia.
Given that NAFLD stems from overnutrition, it is not surprising that weight loss is the first-line treatment for all stages of the condition. Data on the beneficial effects of weight loss are consistent, and the extent of histologic improvement correlates with the percentage of body weight lost. For example, as little as 5% can reduce intrahepatic triglyceride content, but higher degrees of weight loss (>7%-10%) are needed to reverse histologic features associated with disease progression (nonalcoholic steatohepatitis and fibrosis).1 In contrast, there is a paucity of high-quality evidence to support exercise specifically as a primary treatment for NAFLD.2 One study3 suggests that aerobic and resistance exercise can decrease hepatic steatosis, improve cardiovascular health, and decrease insulin resistance even if weight loss is not achieved. However, current guidelines provide little direction on the type or level of exercise intensity needed to benefit patients with NAFLD.
In this issue of JAMA Internal Medicine, Zhang et al4 present the results of a clinical trial examining the effects of exercise on intrahepatic triglyceride content in 220 individuals with NAFLD randomized to 3 different exercise programs (vigorous-moderate, moderate, and control groups). Patients in the vigorous-moderate group exercised 30 minutes 5 days per week for 6 months at high intensity (goal, 65%-80% of the maximum predicted heart rate [8-10 metabolic equivalents]) followed by 6 months of a moderate-intensity regimen (goal, 45%-55% of the maximum predicted heart rate [3-6 metabolic equivalents]).
The moderate exercise group maintained this moderate-intensity regimen for 12 months, and the control group did not change their level of physical activity from baseline. Study participants were asked to continue their typical diet. Both vigorous-moderate and moderate exercise reduced intrahepatic triglyceride content at 6 and 12 months when compared with the control arm (-5.01% and -3.85% and -4.16% and -3.48%, respectively, P < .001). When the vigorous-moderate and moderate groups were directly compared, reductions of intrahepatic triglyceride content at 12 months were similar, suggesting that high-intensity exercise did not offer additional benefit with respect to improving hepatic steatosis.
Another study5 found that more intense exercise is needed to more significantly reduce hepatic steatosis, inflammatory markers, and metabolic parameters. The study by Zhang and colleagues4 is the first prospective randomized trial, to our knowledge, to find that a lower-intensity exercise program may be beneficial to patients with NAFLD during 12 months. It is possible that a 12-month vigorous exercise group would have had even further benefit compared with the other groups. If 6-month data are examined, patients completing the intense exercise phase of the vigorous-moderate exercise group had significantly more weight loss and reductions in body fat mass, blood pressure, and visceral adipose tissue compared with the moderate exercise and control groups. Interestingly, improvements in visceral adipose tissue persisted in the vigorous-moderate exercise group at 12 months after intensity had been reduced and despite mild weight gain during the latter 6 months.
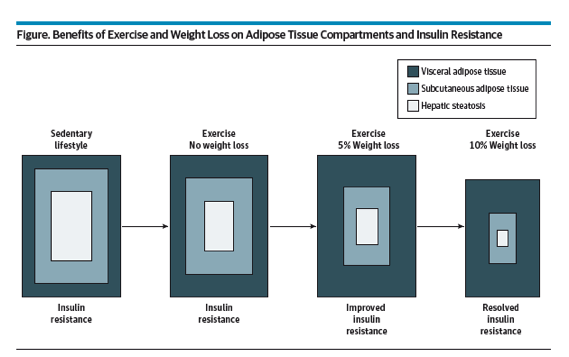
Visceral adipose tissue plays a central role in the pathogenesis of NAFLD and insulin resistance, and an exercise routine with the greatest effect on visceral adipose tissue should be the goal. The results in the moderate exercise group are similar to studies evaluating the role of lower-intensity resistance training. Many of these studies suggest that resistance training reduces intrahepatic fat, but its effects on visceral adipose tissue and other metabolic parameters have not been convincing. Loss of visceral adipose tissue typically occurs when patients lose 5% to 10% of their initial body weight.6 High-intensity exercise burns more calories and can facilitate faster weight and visceral adipose tissue loss.7 The benefits of exercise and weight loss on adiposity and insulin resistance are shown in the Figure. Although not yet studied rigorously in patients with NAFLD, an exercise plan that incorporates strength and aerobic training or one that incorporates short bursts of high-intensity exercise may be the most beneficial.
Exercise alone can reduce hepatic steatosis and have a modest effect on visceral adipose tissue, but additional
weight loss can provide a greater effect on visceral adipose tissue and subcutaneous adipose tissue. Weight loss first improves visceral adipose tissue followed by subcutaneous adipose tissue. Improvement in insulin resistance occurs with improvement in visceral adipose tissue.
----------------------------------
Even if high-intensity exercise is ideal, participation in it is limited. A previous study8 found that patients with NAFLD engage in less physical activity than healthy controls. The study by Zhang et al4 provides encouragement that maintaining a moderate-intensity exercise program is feasible (96% completed the 12-month program). Because the trial did not include a diet arm, it is impossible to compare the benefits of exercise that are independent of weight loss from those attributable to weight loss alone. However, when the authors adjusted for weight loss, they found that much but not all of the effect on intrahepatic triglyceride content was explained, suggesting that exercise and weight loss are likely to benefit NAFLD.
There are important genetic and environmental determinants of NAFLD, and the disease phenotype can differ greatly among ethnic groups. Compared with whites and Hispanics, Asians develop NAFLD at a lower body mass index and have lower rates of obesity. Although Asians tend to have lower body mass indexes, they have relatively higher levels of visceral adipose tissue and are more susceptible to metabolic disease. Thus, the findings by Zhang et al,4 although important, may not be generalizable to other populations or ethnicities. Another factor that limits generalizability is that patients with diabetes were excluded, and NAFLD is present in 40% to 70% of patients with diabetes.
Lifestyle intervention is the cornerstone of treatment for NAFLD because it treats the root cause of the disease and its comorbidities. For clinicians, the study by Zhang et al4 validates that encouraging patients to engage in moderate-intensity activity not only is better than nothing at all but also has reasonable efficacy compared with more intense regimens if it is sustained. This study also suggests that if patients are motivated, it is likely that higher-intensity exercise may have an incremental positive effect on drivers of disease progression, such as visceral adipose tissue, and provide superior cardiovascular benefit, which is more likely to favorably affect long-term outcomes in patients with NAFLD.
|
| |
|
 |
 |
|
|