 |
 |
 |
| |
Alcoholic Liver Disease Has Rapidly Emerged As the Leading Indication for Liver Transplant Evaluation
|
| |
| |
Reported by Jules Levin
AASLD 2018 Nov 9-13 SF
Dr. Alisa Likhitsup1, Jessica L. Mellinger1, Lisa M. McElroy2, Naba Saeed3, Ammar Hassan1, Gerald S. Winder4, Dr. Christopher J. Sonnenday2 and Dr. Robert J. Fontana1, (1)Division of Gastroenterology and Hepatology, University of Michigan, (2)Department of Surgery, University of Michigan, (3)Department of Internal Medicine, Beaumont Hospital, (4)Department of Psychiatry, University of Michigan
Program abstract
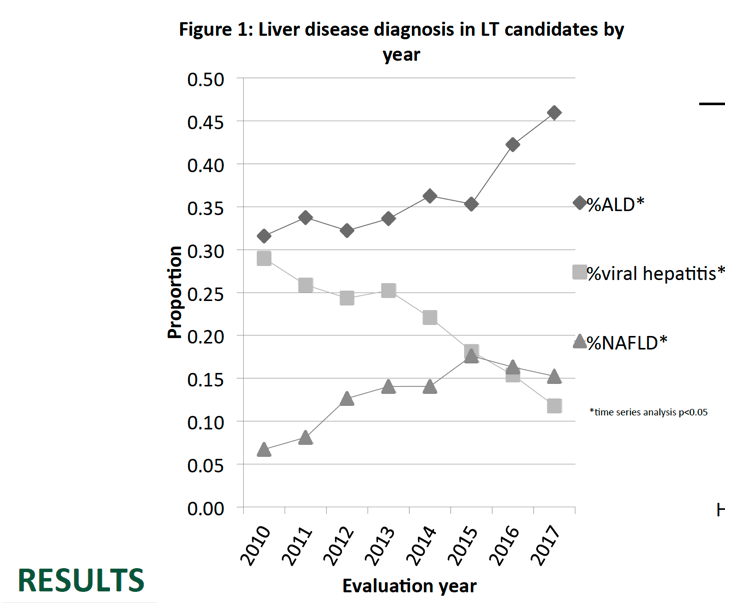
Background: Recent data suggest that the number of liver transplant (LT) candidates with viral hepatitis has decreased while the proportion with NAFLD has increased. However, the number of alcoholic liver disease (ALD) patients referred or listed for LT remains unclear. Our aim was to determine temporal changes in the demographics, diagnosis and evaluation outcomes of LT referrals over the past 8 years at a single center.
Methods: Medical records of all adult patients undergoing initial LT evaluation between Jan, 2010 to Feb, 2017 at a large transplant center were reviewed. Univariate analyses using chi-square tests or independent samples t-test and time-series analysis were performed.
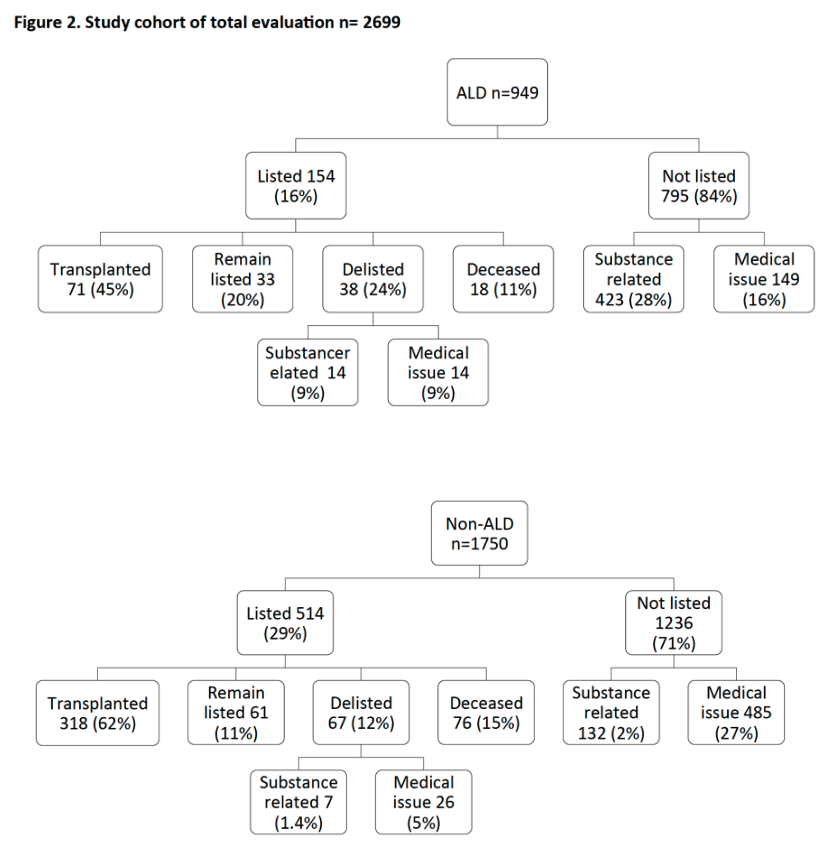
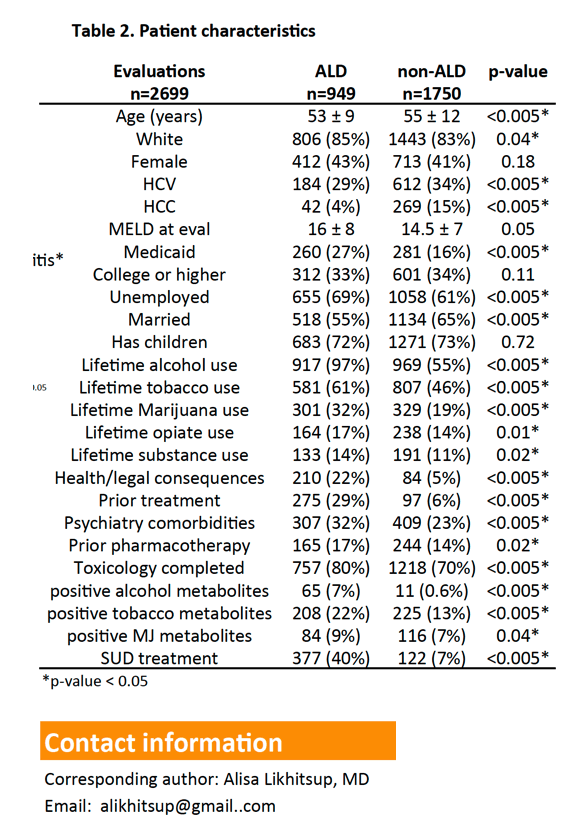
Results: A total 2699 patients (949 ALD and 1750 non-ALD) were evaluated for LT; 58% were male and 83% were Caucasian. Overall evaluations for ALD and NAFLD candidates have increased significantly over time (p<0.05) while the proportion of patients with viral hepatitis alone has decreased. Compared to non-ALD, mean age was lower in ALD (53 vs. 55 yrs; p<0.005) while the mean MELD score was higher (16 vs 14.5; p=0.05). The proportion of unemployed (69% vs 61%) and Medicaid insured (27% vs 16%) patients was higher in ALD vs non-ALD (p<0.005). ALD patients were also more likely to have a recent tobacco, marijuana, opioid, and other illicit substance use, psychiatric comorbidity, and detectable alcohol and tobacco metabolites at evaluation vs non-ALD (P<0.05). During evaluation, substance use treatment intervention or referral was more common in ALD vs non-ALD (40% vs 7%; p<0.005). The proportion of patients listed for LT was significantly lower in ALD vs non-ALD (16% vs 29%; p<0.005) and this proportion did not change over time. During a median follow-up of 419 (0 - 2784) days, 45% of ALD vs 62% of non-ALD patients were transplanted (p<0.005). Delisting was more frequent in ALD vs non-ALD (24% vs 12%, p<0.005) with active substance use cited as a more common reason for delisting (9% vs 1.4%) (p<0.005).
Conclusion: Our data demonstrate that ALD has rapidly emerged as the leading indication for LT referral exceeding referrals for viral hepatitis and NAFLD combined in 2017. However, ALD patients present with psychosocial complexity and substance use is a common reason for listing ineligibility as well as delisting. Therefore, careful psychosocial screening and attention to early substance use disorder detection and treatment may help more ALD patients qualify for LT.


|
| |
|
 |
 |
|
|