 |
 |
 |
| |
63% Frail at 65 Years Old-Itlalian Study/NEW HIV Index+Protective Index / HIV-related and social frailty predictors and protectors in 1612-person Italian cohort
|
| |
| |
HIV-related and social frailty predictors and protectors in 1612-person Italian cohort
Download the PDF here
9th International Workshop on HIV and Aging, September 13-14, 2018, New York
from Jules: using new concepts - HIV Index & Protective Index to measure frailty - look at red & green tables below & you will see with bad or high HIV Index (used to measure frailty) a high HIV Index & a low PI, Protective Index results in 48% frailty in 55 year old HIV+; at age 65 this person 63.6% are frail !
Mark Mascolini
Diverse HIV-related factors predicted frailty in 1612 HIV-positive adults in Italy [1]. A half-dozen social factors, mainly related to socioeconomic status, protected against frailty in these people. Combining HIV factors with social factors enhanced predictive power.
Aging of the HIV population has fostered increasing study of clinically defined frailty in people with HIV. But University of Modena researchers who conducted this new study observed that frailty predictors and protectors in HIV-positive people remain poorly understood. To address these issues, they focused on 1612 HIV-positive adults in the Modena HIV Metabolic Clinic prospective cohort. They used multivariate linear and logistic models to assess frailty predictors and protectors from an array of variables and two indices, the HIV Index and the Protective Index.
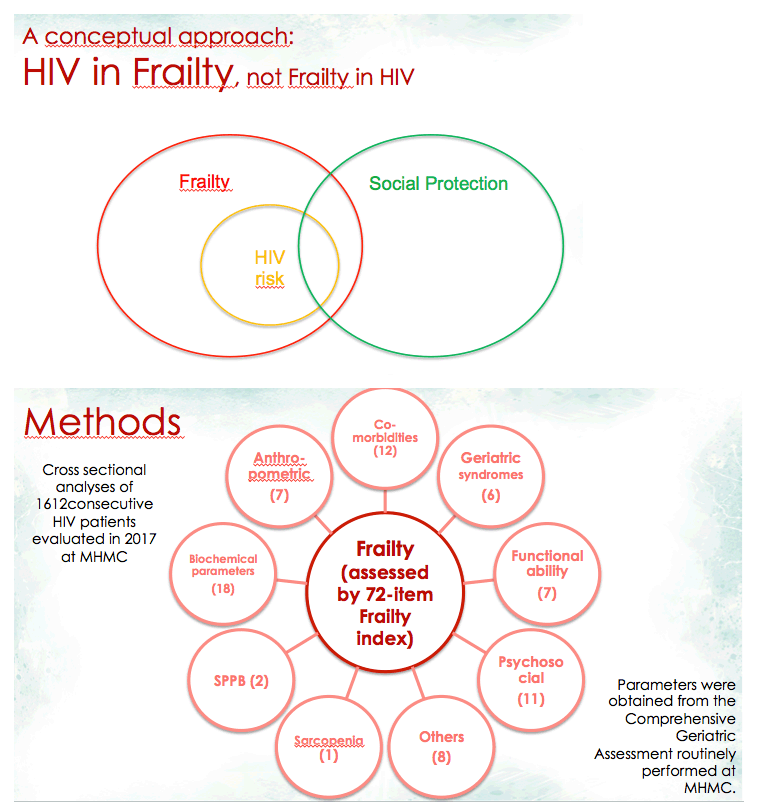
The frailty index used in the Modena study is distinct from the standard 5-item Fried criteria [2]. Instead the Modena team uses an index incorporating 72 non-HIV variables such as body mass index, activities of daily living, sarcopenia, and geriatric syndromes. A study of an earlier version of the Modena frailty index found that it predicts survival and incident multimorbidity independently of HIV-related and behavioral risk factors [3].
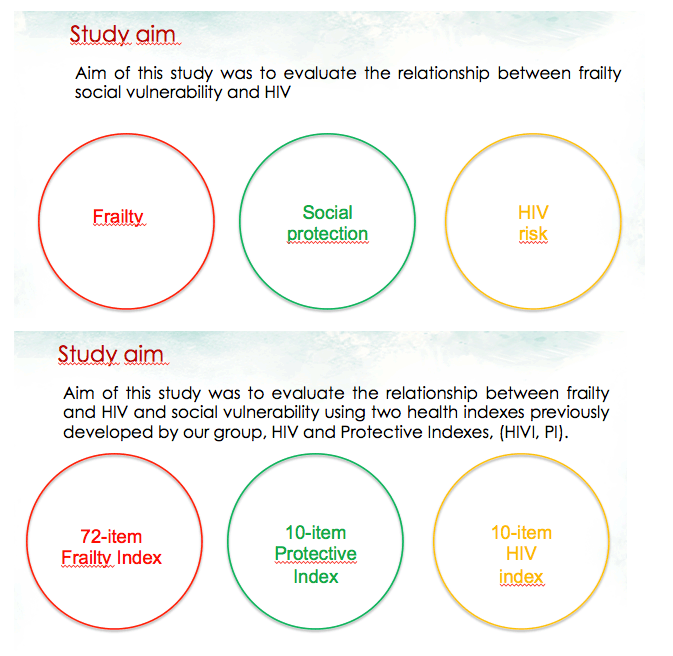
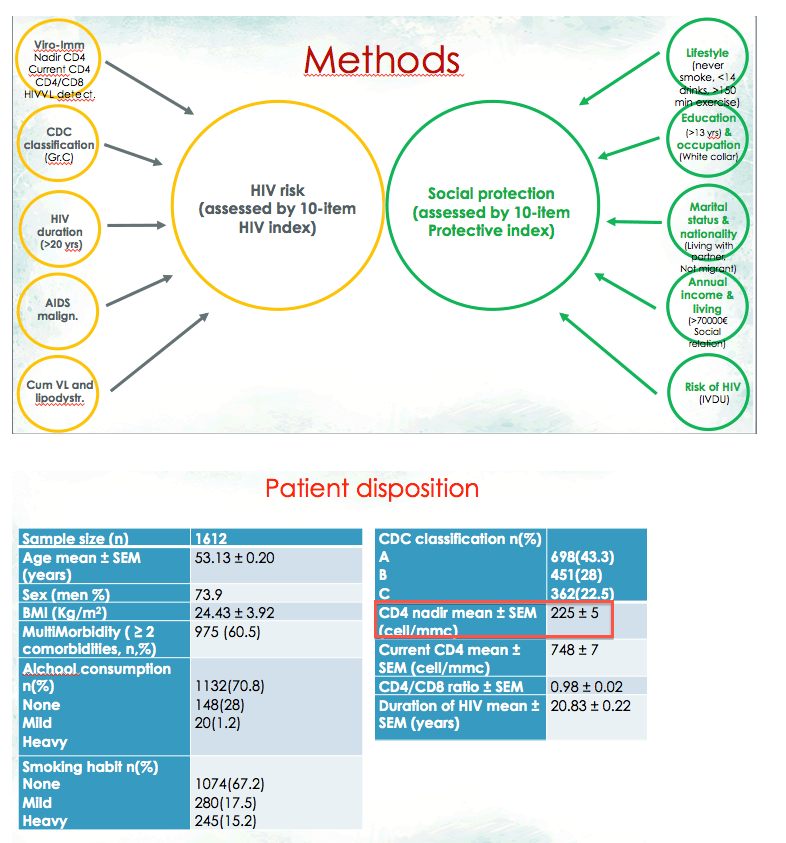
The Modena investigators also developed and tested the 10-item HIV Index (which includes HIV-related variables like CDC disease classification, duration of HIV infection, and current and nadir CD4 count) and the 10-item Protective Index (which includes items found in common social vulnerability indices such as ethnicity, education level, income, and other sociodemographic variables) [4].
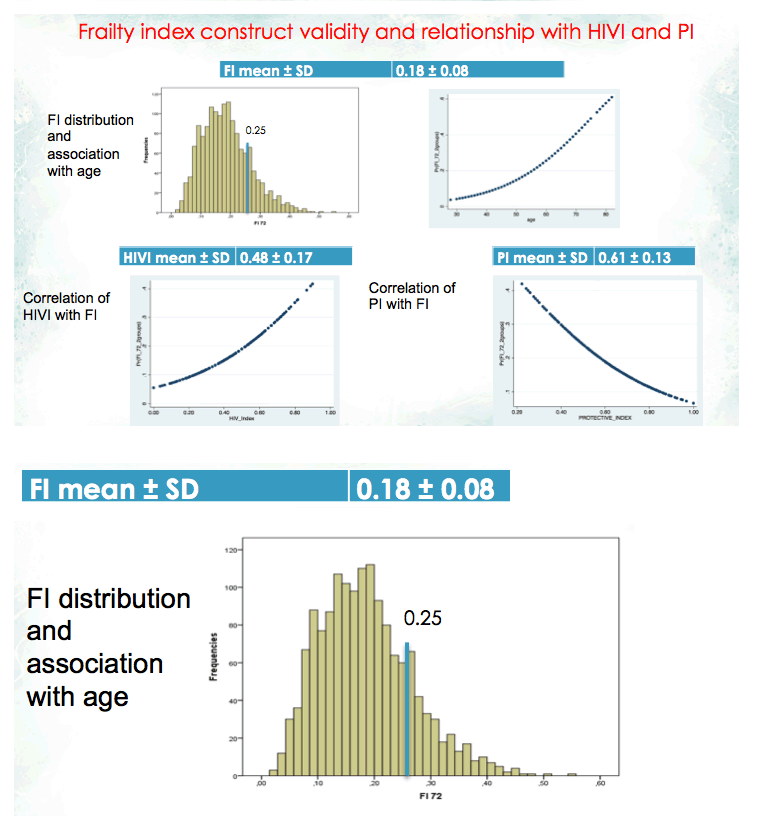
This cross-sectional analysis focused on 1612 adults with HIV, 74% of them men, averaging 53.1 years in age (+/- 0.20). Almost two thirds of cohort members (60.5%) had 2 or more comorbidities. Frailty index averaged 0.18 +/- 0.08, HIV Index 0.48 +/- 0.17, and Protective Index 0.61 +/- 0.13. Multivariate analysis identified 6 independent predictors of frailty:
-- CDC HIV disease class: odds ratio (OR) 2.20, P < 0.001
-- Longer HIV duration: OR 3.86, P < 0.001
-- Longer time from HIV diagnosis to antiretroviral initiation: OR 1.65, P = 0.002
-- Lipodystrophy: OR 1.86, P = 0.001
-- Current CD4 count: OR 1.66, P < 0.001
-- Higher (worse) HIV Index: OR 1.025, P < 0.001
Seven variables independently protected against emergence of frailty:
-- More years of education: OR 0.24, P < 0.001
-- White-collar profession: OR 0.41, P < 0.001
-- Higher income: OR 0.26, P < 0.05
-- No injection drug use: OR 0.49, P < 0.001
-- No smoking history: OR 0.44, P < 0.001
-- Physical activity: OR 2.94 P < 0.001
-- Higher (better) Protective Index: OR 0.972, P < 0.001
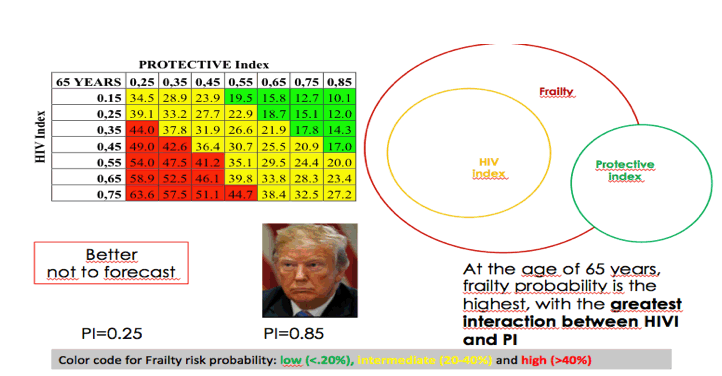
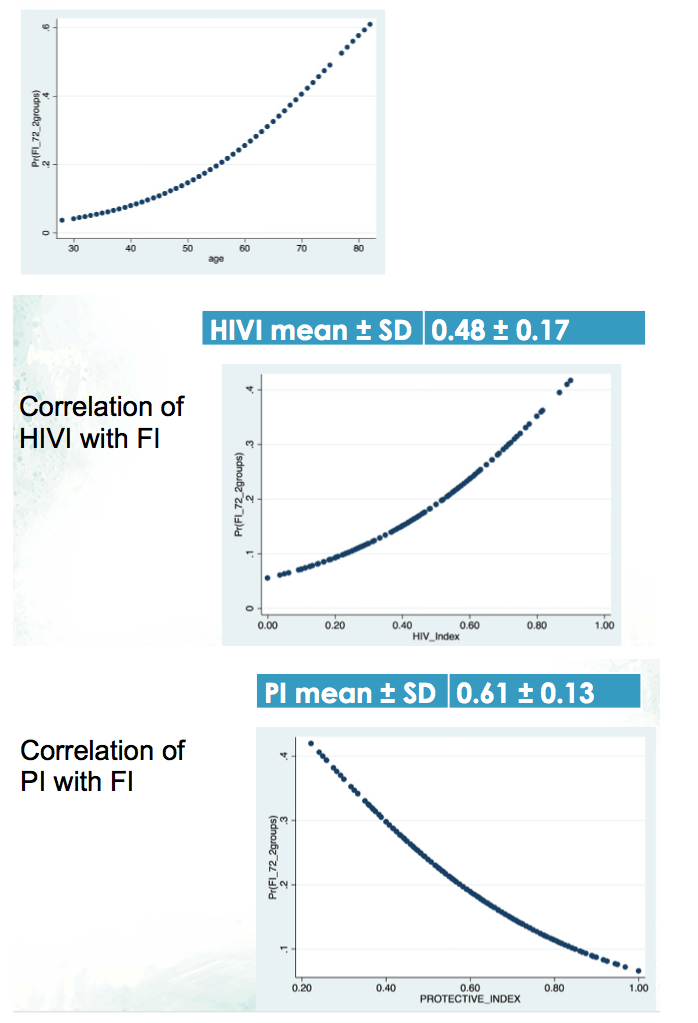
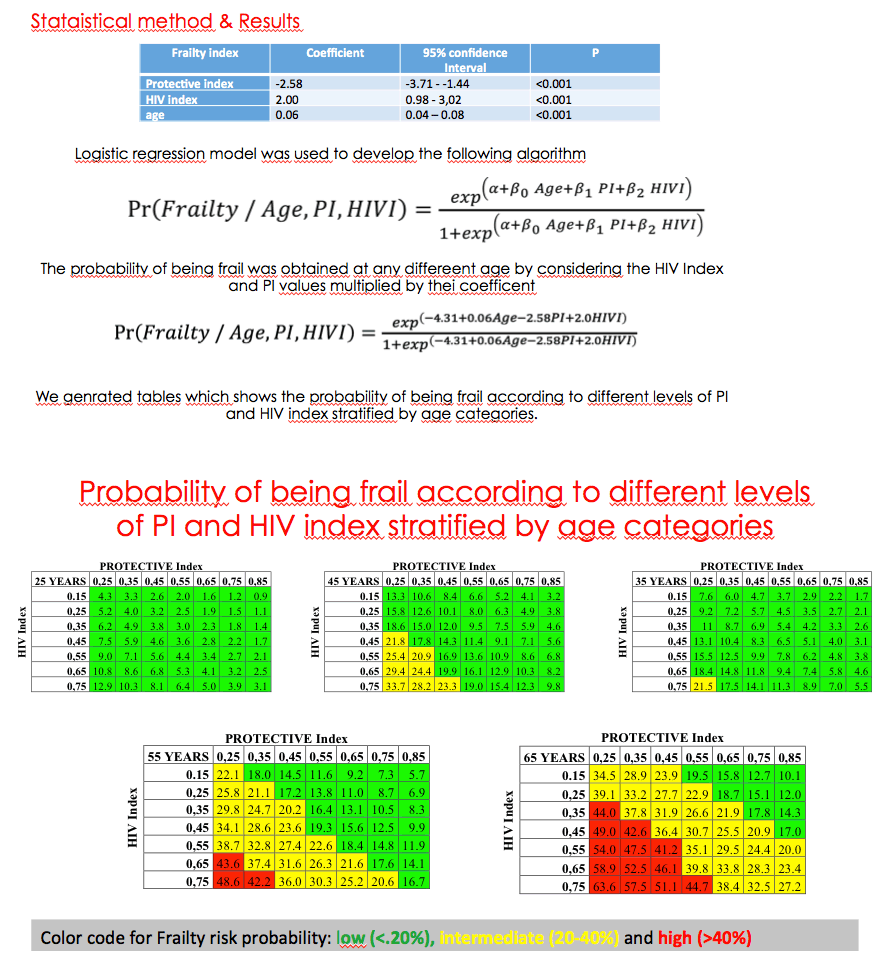
The Modena team used logistic regression analysis to develop an algorithm that estimated the probability of frailty as a function of age, Protective Index, and HIV Index. With this algorithm, they generated tables showing the probability of frailty according to Protective Index and HIV Index stratified by 5 ages (25, 35, 45, 55, and 65 years).
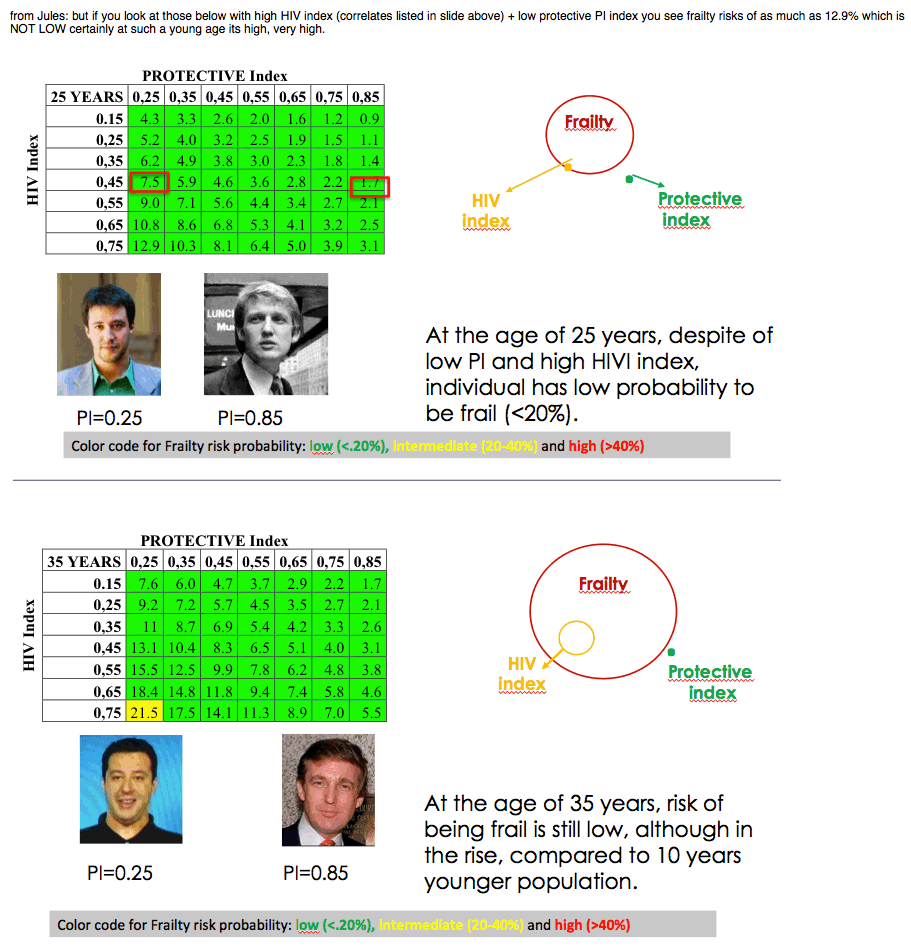
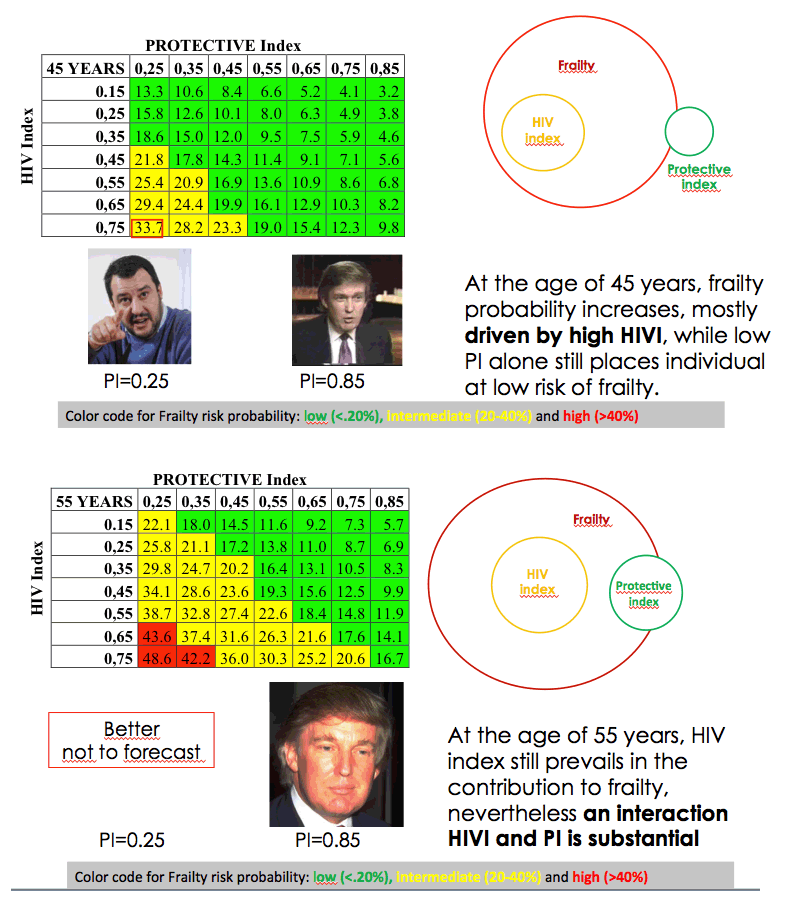
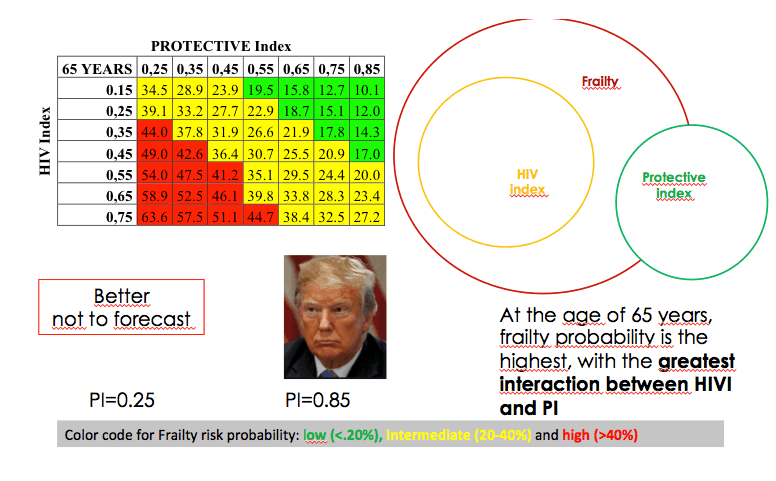
The tables predicted a low probability of failure (under 20%) for 25-year-olds regardless of Protective Index or HIV Index. For 45-year-olds probability of frailty was intermediate (20% to 40%) at lower Protective Index values coupled with higher HIV Index values. For 65-year-olds frailty probability was high (above 40%) when low Protective Index values combined with high HIV Index values. Interaction between the 2 indices was greatest at age 65.
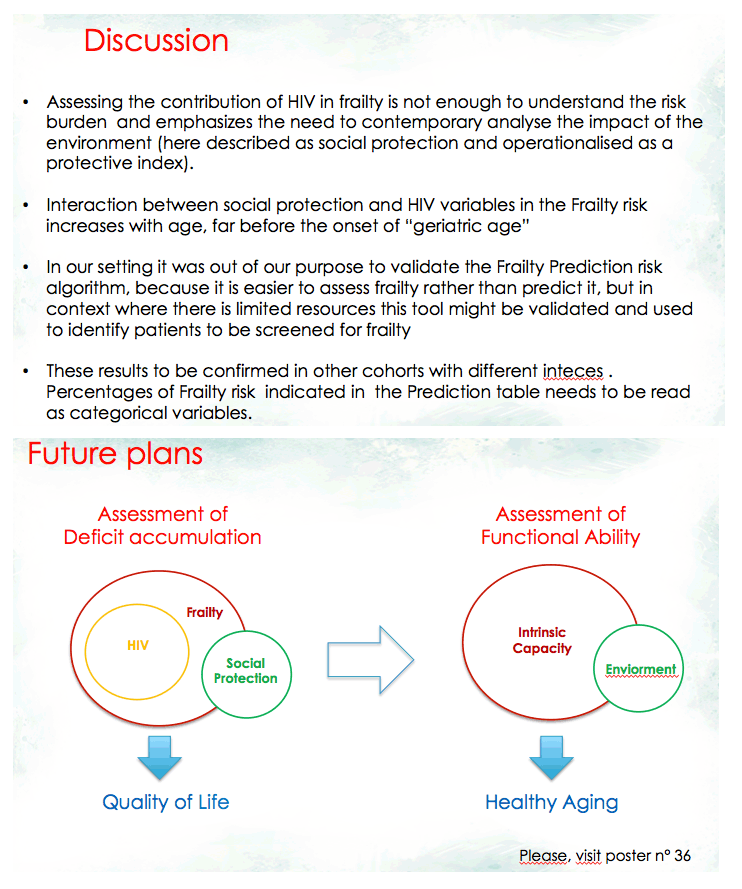
The researchers believe their work suggests that--besides HIV-related variables-"social vulnerability factors contribute to frailty in an HIV aging cohort." They stressed that both their HIV Index and their Protective Index predicted frailty in this large population. The Modena team urged HIV colleagues to consider "geriatric assessment tools even for patients who would not normally be classified as geriatric on the basis of their chronological age."
References
1. Guaraldi G, Franconi I, Theou O, et al. Correlation between HIV-index (HIVI), protective index (PI) and frailty in an HIV ageing population. 9th International Workshop on HIV and Aging, September 13-14, 2018, New York. Abstract 15.
2. Fried LP Tangen CM, Walston J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol, Series A. 2001;56:M146-M157.
3. Guaraldi G, Brothers TD, Zona S, et al. A frailty index predicts survival and incident multimorbidity independent of markers of HIV disease severity. AIDS. 2015;29:1633-1641. https://www.ncbi.nlm.nih.gov/pubmed/26372273
4. Franconi I, Theou O, Wallace L, et al. Correlation between HIV-Index (HIVI), Protective Index (PI) and frailty in an HIV ageing population. 10th Italian Conference on AIDS and Antivirals. May 22-24, 2018. Rome.
www.icar2018.it/public/repository/slide/3_2_2_0_6_slide.pdf
Program Abstract
Correlation between HIV-Index (HIVI), Protective Index (PI) and frailty in an HIV ageing population.
Guaraldi G1, Franconi I1, Theou O2, Wallace L2, Malagoli A1, Eendebak R2, Milic J1, Rockwood K2, Mussini C1
1Metabolic Clinic, University Of Modena And Reggio Emilia, Modena, Italy, 2Dalhousie University, Halifax, Canada
Background: Currently, the impact of HIV and protective social-environmental conditions on frailty in HIV ageing population is not known. Frailty can be operationalized as a deficit accumulation, building a scale which can be used to standardise accumulated deficits in order to estimate survival probability without reference to chronological age.
Aim of this study was to evaluate the relationship between frailty and HIV and social vulnerability using two health indexes previously developed by our group, HIV and Protective Indexes, (HIVI, PI).
Material and methods: This study was performed within the Modena HIV Metabolic Clinic (MHMC) prospective cohort Frailty was evaluated with a 72-items frailty index (FI). All patients with a FI score ≥ 0.25 were considered frail. HIVI and PI were built using commonly recollected HIV and social vulnerability data. Multivariate linear and logistic models were used to evaluate predictors of frailty among all variables and Indexes.
Results: 1565 subjects were included. Mean age 53.15±8.03, 73.9% males. Mean FI was 0.19±0.08. Mean HIVI and PI were 0.48±0.17 and 0.63±0.14 respectively.
Independent predictors of frailty were:
- CDC class (OR=2.20, p< 0.001),
- duration of HIV (OR=3.86, p < 0.001),
- time from diagnosis to initiation of ART (OR=1.65, p = 0.002),
- lipodystrophy (OR=1.86, p = 0.001), current CD4+ (OR=1.66, p<0.001)
- and a higher HIVI score (OR=1.025, p<0.001).
Social protective factors were:
- higher years of education (OR=0.24, p<0.001),
- white collar profession (OR=0.41, p<0.001),
- higher income (OR=0.26, p<0.05),
- no history of injective drug use (OR=0.49, p<0.001),
- no smoking habit (OR=0.44 p < 0.001),
- physical activity (OR=2.94 p < 0.001) and a
- higher PI score (OR=0.972, p<0.001).
Conclusion: Our work suggests that HIV and social vulnerability factors contribute to frailty in an HIV ageing cohort. Interestingly, higher HIVI and lower PI scores correlate with frailty. Taking into consideration the medical and socioeconomic burdens affecting older people living with HIV, a more holistic approach to the assessment of global health and care must be favored, resorting to geriatric assessment tools even for patients who would not normally be classified as geriatric on the basis of their chronological age.


|
| |
|
 |
 |
|
|