 |
 |
 |
| |
Aging HIV+ Brain - The relationship between synaptodendritic
neuropathology and HIV-associated neurocognitive disorders is moderated by age
|
| |
| |
Reported by Jules Levin
& Aging International Workshop 2018
New York, NY Sept 13-14 2018
Erin E. Sundermann, PhD
HIV Neurobehavioral Research Center, UC San Diego
HIV
Program Abstract
The relationship between synaptodendritic neuropathology and HIV-associated neurocognitive disorders is moderated by age
Sundermann E1, Levine A2, Paolillo E1, Masliah E3, Adame A1, Soontornniyomkij V1, Letendre S1, Moore D1
1University Of California, San Diego, La Jolla, United States, 2University of California, Los Angeles, Los Angeles, United States, 3National Institute on Aging, Bethesda, United States
Background: Approximately 45% of people living with HIV (PLWH) develop HIV-associated neurocognitive disorders (HAND) in the era of effective antiretroviral therapy. Given the rising rates of older PLWH, it is important to determine whether older PLWH are more vulnerable to the effects of HIV disease processes on HAND. In this study, we examined whether age moderates the relationship between synaptodendritic neuropathology and cognitive performance and rates of HAND. We hypothesized that minimal to moderate levels of neuropathology would be more strongly associated with cognitive function in older versus younger PLWH, whereas severe neuropathology would be strongly associated with cognitive function regardless of age.
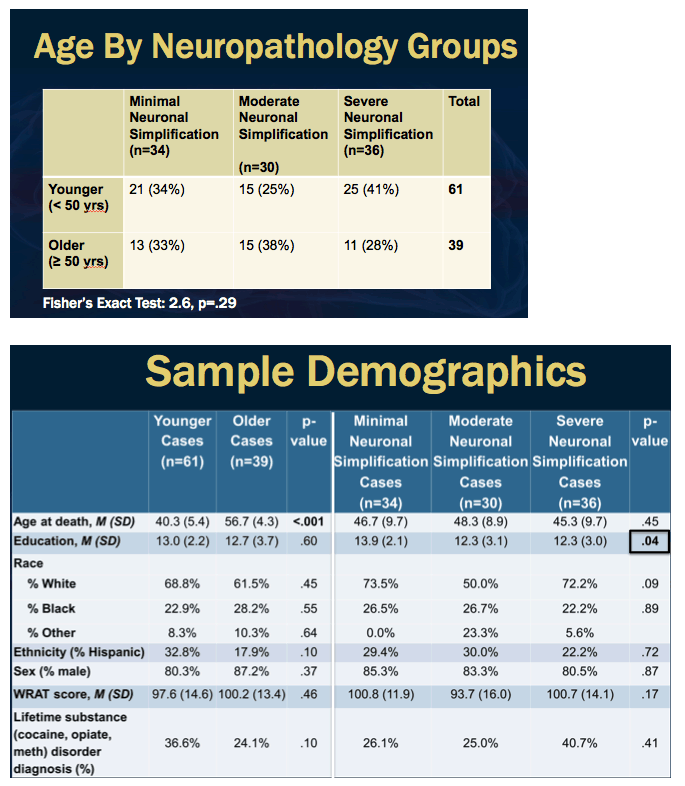
Methods: Analysis included 100 HIV-seropositive post-mortem cases (mean age=46.7, [SD=9.5], mean education=12.9 yrs [SD=2.8], 83% male, 66% White) who were enrolled in the National NeuroAIDS Tissue Consortium and were diagnosed as HAND or no HAND within one year of death. Synaptodendritic neuropathology was determined based on the density of (1) synaptophysin (SYP, a marker of presynaptic terminals) and (2) microtubule-associated protein-2 (MAP2, a marker of neuronal cell bodies and dendrites) immunoreactivity in sections of the frontal cortex. A composite score of SYP and MAP2 was divided into tertiles representing minimal, moderate and severe neuropathology. HAND was diagnosed according to Frascati criteria. We used Fisher's exact test to examine differences in HAND rates among neuropathology groups within older (≥50 years old; n=39) and younger (<50 years old; n=61) cases. In a subset of cases with demographically-corrected, standardized T-scores from 15 neuropsychological tests (N=77), T-scores were averaged to create a global T-score, and linear regressions were used to examine the interactive effect of age and neuropathology group on global T-scores. Analyses were adjusted for relevant demographic and clinical factors (e.g., education, sex, estimated duration of HIV infection, CD4+ T-cell count).
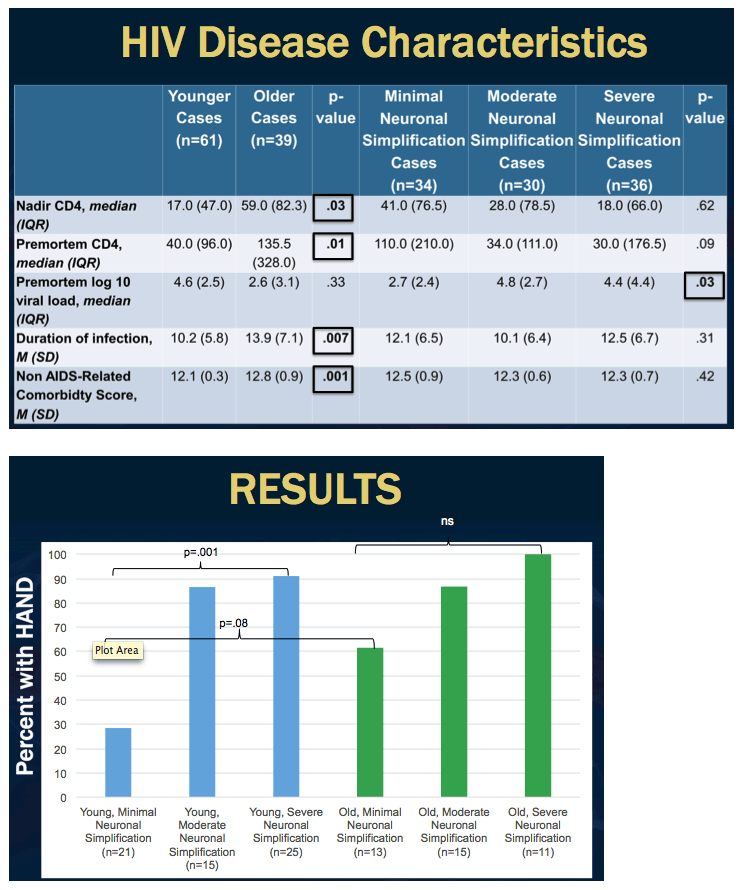
Results: Among those with moderate and severe neuropathology, rates of HAND diagnoses were similar between younger (moderate: 87%, severe: 100%) and older cases (moderate: 87%, severe: 91%); however, among those with minimal neuropathology, older cases had rates of HAND that were higher than younger cases (61.5% vs. 28.5%, p=.08), although not significant, and similar to older cases with moderate neuropathology (61.5% vs. 86.7%, p=.20). Conversely, among younger cases, rates of HAND were lower in those with minimal versus moderate neuropathology (28.5% vs. 86.7%, p=.001). There was a significant age by neuropathology group interaction on global T-scores (p=.04), whereby the relationship between severe (versus minimal) neuropathology and poorer global T-scores was stronger among older (B=-14.67, p=.001) versus younger (B=-5.59, p=.03) cases. The comparisons of moderate versus minimal and moderate versus severe neuropathology with global T-scores did not differ by age group (p's>.05).
Conclusions: Findings indicate that age moderates the relationship between synaptodendritic neuropathology and neurocognitive performance. In the presence of minimal neuropathology, older PLWH are more likely to have HAND than younger PLWH. When severe neuropathology is present, almost all PLWH have HAND regardless of age; however, HAND may be more severe in older PLWH compared to younger PLWH.




|
| |
|
 |
 |
|
|