| |
|
The risk of hepatocellular carcinoma in cirrhotic patients with hepatitis C and sustained viral response: role of the treatment regimen
|
| |
| |
Download the PDF here
Jnl of Hepatology, In Press, Nov 15 2017 - - Hamish Innes, Stephen T. Barclay, Peter C. Hayes, ..., Nick Kennedy, Pete Bramley, Sharon J.Hutchinson
---------------------------------
AASLD: Long-term Follow-Up of Patients With Chronic HCV and No or Minimal Fibrosis Shows Low Risk for Liver-Related Morbidity and Mortality After Achieving SVR With DAA-Based Therapy: Results From the Gilead SVR Registry - (11/27/17)
AASLD: Low Rates of De Novo or Recurrent Hepatocellular Carcinoma in HCV Cirrhotic Patients Treated with Direct-Acting Antivirals (DAAs): A Single-Center Experience - (11/16/17)
AASLD: The incidence of hepatocellular carcinoma is not increased after DAA therapy - (11/13/17)
-------------------------
Highlights
⋅Crude risk of HCC higher for IFN-free recipients than IFN-containing recipients.
⋅IFN-free and IFN-containing recipients differ with respect to confounding factors.
⋅Association between IFN-free therapy and HCC disappears after adjusting for baseline confounders.
⋅At HCC diagnosis, no differences in nodule size or nodule number were apparent by regimen.
Background & Aims
Previous studies have reported a high frequency of hepatocellular carcinoma (HCC) occurrence in patients with advanced liver disease, after receipt of interferon (IFN)-free therapy for hepatitis C virus (HCV) infection. Our objective was to verify and account for this phenomenon using data from the Scottish HCV clinical database.
Methods
We identified HCC-naïve individuals with liver cirrhosis receiving a course of antiviral therapy in Scotland from 1997-2016 resulting in a sustained virologic response. Patients were followed-up from their treatment start date to the earliest of: date of death, date of HCC occurrence, or 31 January 2017. We used Cox regression to compare the risk of HCC occurrence according to treatment regimen after adjusting for relevant co-factors (including: demographic factors; baseline liver disease stage; comorbidities/health behaviours, virology, and previous treatment experience). HCC occurrence was ascertained through both the HCV clinical database and medical chart review. For our main analysis, treatment regimen was defined as IFN-free vs. IFN-containing.
Results
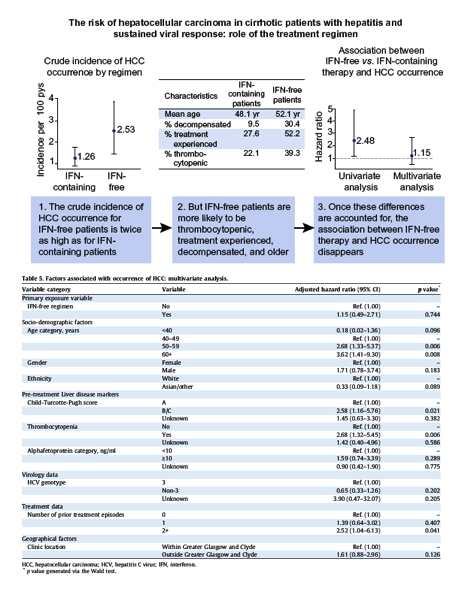
A total of 857 patients met the study criteria, of whom 31.7% received an IFN-free regimen. Individuals receiving IFN-free therapy were more likely to be: older; of white ethnicity, Child-Turcotte-Pugh B/C vs. Child-Turcotte-Pugh A; thrombocytopenic; non-genotype 3; and treatment experienced. HCC occurrence was observed in 46 individuals during follow-up. In univariate analysis, IFN-free therapy was associated with a significantly increased risk of HCC (HR: 2.48; p = 0.021). However, after multivariate adjustment for baseline factors, no significant risk attributable to IFN-free therapy persisted (aHR: 1.15, p = 0.744).
Conclusion
These findings suggest that the higher incidence of HCC following sustained virologic response with IFN-free therapy relates to baseline risk factors/patient selection, and not the use of IFN-free therapy per se.
Lay summary
We examined the risk of liver cancer in 857 patients with cirrhosis in Scotland who received hepatitis C antiviral therapy and achieved a cure. We compared the risk of first-time liver cancer in patients treated with the newest interferon-free regimens, to patients treated with interferon. After accounting for the different characteristics of these two treatment groups, we found no evidence that interferon-free therapy is associated with a higher risk of liver cancer.
Introduction
The arrival of interferon (IFN)-free direct acting antiviral (DAA) regimens from 2014-2015 has transformed the treatment of hepatitis C virus (HCV) infection. In addition to causing few adverse effects and being convenient to administer (i.e. with one tablet per day dosing for only 8-12 weeks), IFN-free therapy results in cure rates exceeding 90%, even in patients with advanced liver disease.[1], [2] With IFN-based regimens, a cure is associated with an 81% (95% CI 56-92), and 94% (95% CI 81-98) reduction in the risk of hepatocellular carcinoma (HCC) and liver mortality, respectively for patients with advanced fibrosis.3 However, the relatively recent introduction of IFN-free therapy means that we do not yet know what the analogous value of an IFN-free cure is - i.e. whether it is better, worse or equivalent to an IFN-based cure (although the assumption thus far, for instance in cost effectiveness modelling work,4 has been one of equivalence).
Recently, a number of European studies have described high rates of HCC occurrence and recurrence following receipt of IFN-free regimens.[5], [6], [7], [8] Reig et al. reported that of 58 patients from Spain with a complete radiological response to HCC, 16 (27.6%) developed HCC recurrence 5.7 months after receiving an IFN-free regimen.5 Similarly, Conti et al. reported that of 59 patients from Italy with a complete response to resection/ablation of HCC, 28.8% developed HCC recurrence 24 weeks after starting IFN-free treatment.6 In terms of HCC occurrence, Conti et al. report that 3.2% of 285 patients with cirrhosis developed HCC for the first time by 24 weeks after starting IFN-free therapy in Italy.6 Another study from Portugal noted a similar rate of HCC occurrence (7.4% with HCC at twelve months after starting an IFN-free regimen).7 Prima facie, this level of HCC recurrence and occurrence is higher than expected. For instance, data from the STORM trial following individuals after successful response to surgical resection/local ablation of HCC, reported ∼15-20% HCC recurrence at six months.9 Meanwhile, HCC occurrence in cirrhotic patients attaining a hepatitis C cure through pegylated interferon and ribavirin has ranged from 1.0-1.4% per annum.[10], [11]
Two theories have dominated the discussion of these findings thus far. Firstly, Reig et al. and others have speculated that the rapid decline in hepatitis C viral load upon starting antiviral therapy, and the abrupt cessation of liver inflammation that results from this, may have the unintended consequence of adversely dampening cancer immune-surveillance activities that serve to identify and remove cancer-prone hepatocytes. Individuals receiving IFN-free therapy may be particularly prone to this theoretical mechanism for HCC because the transition to undetectable viral load is far more rapid with IFN-free therapies relative to IFN-containing regimens, and/or because IFN has anti-proliferative and immune-modulating properties that may offset any such downregulation of immune surveillance.5 Alternatively, others have suggested that the higher risk of HCC reflects a shift in the case mix of individuals attaining a HCV cure post-IFN-free availability.12 That is to say, patients treated and achieving sustained virologic response (SVR) with IFN-free therapy may on average, have a greater pre-existing risk of HCC relative to those treated with IFN-containing regimens, making uncontrolled comparisons misleading.
Data reporting the risk of HCC by treatment regimen from large and representative cohorts of cured HCV patients are needed to answer this important question. Thus, we herein used the well-characterised Scottish Hepatitis C clinical database - a nationwide registry of HCV treatment patients - to identify cirrhotic patients attaining SVR in Scotland between 1997 and 2016. Our objective was to examine the incidence of de novo HCC occurrence according to the type of regimen received. In particular, we wanted to assess the credibility of the shifting case mix theory - that is whether differences in patient characteristics could account for the "higher" risk of HCC occurrence following receipt of IFN-free regimens vs. IFN-containing regimens.
Patients and methods
Data source: clinical database and medical chart review
We used data from the Scottish HCV clinical database, which consists of standalone Microsoft Access databases installed at 17/18 HCV treatment clinics across Scotland. Each database captures detailed clinical and epidemiological information on individuals who have attended an appointment for care/management of HCV infection.[13], [14] An anonymised extract of each database is downloaded annually by Health Protection Scotland and assembled into several nationwide datasets (at the time of this analysis, the latest extracts were complete up to May 2016). Patients on the clinical database have provided informed "opt-out" consent for use of their data in administrative and research purposes.
In this study, key data from the clinical database were supplemented with a medical chart review carried out in February and March of 2017 by data entry staff and lead clinicians at participating clinics. This chart review entailed the retrieval and study of an individual's medical records to obtain information on HCC occurrence, mortality events and relevant exposure variables, where that information was missing, or otherwise not available from the database at the time of the last download. The study protocol was approved by the Scottish HCV clinical database monitoring committee.
Inclusion/exclusion criteria
This study included patients from the 12 Scottish HCV clinics, whose clinical database was complete at the time of the last download, and that were able to carry out the requisite medical chart review. Collectively, these 12 clinics account for circa 85% of all HCV treatment episodes occurring nationally in Scotland. We identified all individuals at these clinics who: (i) attained SVR between 1 Jan 1997 and 1 April 2016; and (ii) had received a diagnosis of liver cirrhosis prior to commencing therapy. We excluded patients with hepatitis B or HIV co-infection prior to treatment, or with HCC prior to starting treatment. An SVR was defined as testing viral RNA negative for a minimum of 12 or 24 weeks following completion of treatment, as per clinical guidelines. Up to 2014, the minimum time period required to establish SVR was exclusively 24 weeks (i.e. a SVR 24). From 2014, in keeping with changed clinical guidelines15 reflecting strong concordance between SVR12 and SVR24,16 SVR was defined as a negative test beyond 12 weeks post-treatment.
Primary outcome event
The primary outcome event was first time occurrence of HCC through to 31 Jan 2017 following commencement of antiviral therapy. We used the date of HCC diagnosis (i.e. date of the first cross-sectional image meeting HCC diagnostic criteria,17 or, if performed, the date of biopsy diagnostic of HCC) as a surrogate for time of HCC occurrence. HCC diagnoses in this cohort will have been triggered either through (i) symptomatic onset of HCC, or (ii) six-monthly abdominal ultrasound screening (which, as per best practice guidelines,17 is offered to all patients diagnosed with cirrhosis in Scotland). We identified all new post-treatment diagnoses of HCC through the clinical database and medical chart review. All cases identified were cross-checked against instances of HCC registered in the Scottish Cancer database -which, at the time of analysis, provided complete individual-level data on cancer incidence up until 31 Dec 2014 - to ensure no HCC events were missed. For each identified case of HCC, we sought via medical chart review, information on the number of HCC nodules; and the maximum HCC nodule diameter at the time of HCC diagnosis; this aspect of the chart review was completed by the lead clinician at the clinic where the individual(s) in question attained SVR. We also collected data on the last abdominal ultrasound screening test for HCC through to 1 August 2016 for all individuals in the cohort.
Primary exposure variable
The primary exposure variable was the type of treatment regimen received- specifically whether the regimen included interferon, or whether the regimen was interferon-free. We also explored an alternative definition, whether or not the course of therapy included a DAA.
Data on and definitions of relevant covariates
Data on a wide range of baseline covariates were included in this analysis. These were as follows: age; gender; ethnicity; Child-Turcotte-Pugh (CTP) score; platelet count; alphafetoprotein; diabetes, alcohol use history; smoking; HCV transmission route; genotype; previous treatment history and deprivation status and clinic location. CTP score assigns each individual into one of three levels of cirrhosis severity (the least severe being level A, and the most severe being level C), based on pre-treatment bilirubin, albumin, prothrombin time and the presence/absence of ascites and encephalopathy. For the bilirubin, albumin and prothrombin time components of this score, we used the most recent test carried out 0-90 days prior to treatment. Individuals who did not receive a prothrombin time test in this period were assumed to be CTP stage A if they did not have ascites or encephalopathy and had albumin level of >3.5 g/dl, and bilirubin <2 mg/dl (applying to 21.1% of the cohort). Information on platelet count, and alphafetoprotein were similarly based on the most recent test carried out 0-90 days prior to starting treatment.
Thrombocytopenia was defined as a platelet count of <100 per 109/L. Clinic location was assessed in terms of whether the clinic attended was within or outside of the Greater Glasgow and Clyde (GGC) health board (the largest regional NHS board in Scotland with the greatest burden of diagnosed chronic HCV). Diabetes status referred to whether the patient had ever received a diagnosis of diabetes from a health professional. We defined a history of heavy alcohol use as consumption of more than 50 units of alcohol per week for six months or more, at any point in time. Previous treatment history refers to the number of treatment episodes the patient had commenced prior to their eventual SVR. Data on mortality through to June 2016 were obtained via linkage to the Scottish mortality register, whilst mortality in the more recent period of June 2016 to 31 January 2017 was ascertained through the aforementioned medical chart review carried out by data entry staff in February-March 2017. Deprivation was measured through the Scottish Index of multiple deprivation (SIMD), which assigns a deprivation score to each address in Scotland. This SIMD score was obtained via an anonymised linkage to the Community Health Index database, which holds the address of each individual registered with a general practitioner in Scotland and maps that address to an SIMD score. For this analysis, we grouped the SIMD score into quintiles and compared outcomes in the two lower (i.e. two most deprived) quintiles to the three upper (i.e. most affluent) quintiles. All of these aforementioned data linkages were approved by the National Services Scotland Public Benefit Privacy Panel.
Statistical analysis
We adopted a survival analysis approach for this analysis. Follow-up time began at the treatment start date resulting in SVR, and ended at either: the date of HCC occurrence; the date of mortality, or 31 January 2017 (which ever came first). We calculated the unadjusted and adjusted association between treatment regimen and HCC occurrence using Cox regression. For the adjusted association between treatment regimen and HCC, we controlled for all co-factors associated either with the outcome (i.e. HCC occurrence) or with the primary exposure (i.e. treatment regimen). For this we defined "association" conservatively as that demonstrating a p value <0.1. We also fitted an interaction term between time period (defined as before and after 24 weeks post-treatment completion) and HCC occurrence to assess the timing of HCC occurrence according to treatment regimen. Conformity to the proportional hazards assumption was assessed graphically and via the Schoenfeld residual test.
Sensitivity analysis
We carried out two one-way sensitivity analyses (SA). In SA-1 we additionally censored follow-up time at the date of last HCC screening attrition (if at all). The HCC screening attrition date was defined as date of the last ultrasound screening test plus six months, with six months referring to the recommended regularity of HCC screening for patients with cirrhosis.17 In SA-2 we explored an alternative definition of treatment regimen; that being DAA-containing vs. DAA-free.
For further details regarding the materials used, please refer to the CTAT table.
Results
Derivation of final cohort
We identified 902 patients commencing treatment and attaining SVR between January 1997 and April 2016, who were not co-infected with either HIV or hepatitis B virus. From this initial cohort, we excluded 43 patients with a date of HCC diagnosis prior to their treatment start date. We also excluded all patients diagnosed with HCC after the onset of therapy if suspicion of their HCC predated the antiviral therapy start date (n = 2, both with suspicious focal lesions on pre-treatment ultrasound, confirmed on MRI as HCC post-treatment initiation). Our final sample therefore included 857 patients.
Description of cohort at baseline
Approximately a third (31.7%) of the cohort were treated with an IFN-free regimen, whilst the remainder received an IFN-containing regimen. The most common IFN-free regimen received was sofosbuvir + ledipasvir±ribavirin (58.8%) followed by sofosbuvir + daclatasvir (16.2% Table 1). Most patients treated with IFN-containing therapy received either pegylated interferon ± ribavirin (47.4%), or pegylated interferon ± ribavirin + sofosbuvir (38.1%). Patients treated with IFN-free therapy were different in many respects to patients treated with IFN-containing therapy. Specifically, those treated with an IFN-free regimen were more likely to have/be: older; of white ethnicity, CTP- B/C; thrombocytopenic; non-genotype 3; failed HCV treatment at least twice in the past; been treated outside of GGC (Table 1).
HCC occurrence during follow-up
The median duration of follow-up was 2.4 years overall, but varied markedly by treatment regimen (1.7 and 3.5 year for IFN-free and IFN-containing recipients, respectively). Over this follow-up period, 46 cases of HCC occurrence were identified. Of these, 34 and 12 were treated with an IFN-containing and IFN-free regimen, respectively. The crude rate of HCC occurrence was 1.45 events per 100 person-years (95% CI 1.09-1.94). However, there was variation in this crude rate by treatment regimen; the event rate was 1.26 per 100 person-years for individuals treated with IFN-containing therapy, vs. 2.53 for individuals treated with IFN-free therapy (Table 2 and Fig. S1). Most cases of HCC occurrence (61%) comprised a single nodule. The median diameter of the largest HCC nodule was 2.6 cm. No significant differences in the number of nodules or the maximum nodule size, were observed with respect to IFN-free vs. IFN-containing regimens (Table 3 and Table S2).
Factors associated with HCC occurrence
In univariate analysis, individuals treated with an IFN-free regimen had a significantly higher risk of HCC occurrence relative to individuals treated with an IFN-containing regimen (HR 2.48; 95% CI 1.14-5.37 Table 4). Other factors associated (at p value <0.1) with an increased risk of HCC occurrence in univariate analysis were: increasing age; CTP-B/C; thrombocytopenia; alphafetoprotein ≥10 ng/ml; failing HCV treatment at least twice in the past; and treatment outside of GGC. The higher risk associated with IFN-free regimens in univariate analyses was considerably attenuated after multivariate adjustment (aHR 1.15; 95% CI 0.49-2.71 Table 5). The two biggest contributors to this attenuation were adjustment for pre-treatment platelet count and CTP score (Fig. 1). The association between treatment regimen and HCC occurrence was consistent across time period with no suggestion of clustering by time (Fig. 2). Factors that were significantly associated in multivariate analysis with HCC occurrence at p <0.05 were: (i) age 50-59 years vs. 40-49 years (aHR 2.68; p = 0.006); (ii) age 60+ years vs. 40-49 years (aHR 3.62; p = 0.008); (iii) CTP-B/C vs. CTP-A (aHR 2.58; p = 0.021); (iv) thrombocytopenia (aHR 2.68; p = 0.006); and (v) prior failure of 2+ courses of therapy (aHR 2.52, p = 0.041). No violations of the proportional hazards assumption were observed in either univariate or multivariate models.
Sensitivity analysis
In SA-1, more than half (55%) of the cohort were censored for HCC screening attrition (Table S3). The unadjusted association between regimen (IFN-free vs. IFN-containing) and HCC was HR 2.82 (95% CI 1.04-7.63). This association attenuated to HR 1.28 (95% CI 0.41-4.00) following full multivariate adjustment. Thus, the pattern of association between treatment regimen and HCC occurrence was similar between SA-1 and our base case analysis (Fig. S2). When defined in terms of DAA-containing vs. DAA-free (SA-2) treatment regimen was not associated with HCC occurrence, either at the univariate level (HR 1.36; 95% CI 0.66-2.79), or in multivariate analysis (aHR 0.57; 95% CI 0.24-1.40).
Discussion
Principle findings
Recent studies from Europe have warned that the risk of HCC occurrence in cirrhotic individuals may be higher after attaining an IFN-free hepatitis C cure vs. an IFN-containing cure.[6], [7], [8] Although this finding could have major implications for the treatment of HCV, the studies on which it was predicated did not carry out multivariate adjustment for confounding factors, and involved small sample sizes only. In the present study, our aim was to investigate the issue of HCC occurrence by treatment regimen more robustly using data from the Scottish clinical database - a large unselected nationwide cohort of individuals treated for chronic hepatitis C infection. Of 857 patients with cirrhosis who achieved SVR between 1997-2016, we did find, prima facie, a 2.5-fold higher risk of HCC occurrence among patients receiving an IFN-free regimen compared to an IFN-containing regimen (HR 2.48; 95% CI 1.14-5.37). Yet, as noted previously elsewhere,[12], [18] the baseline characteristics of individuals with an IFN-free cure were demonstrably different from those with an IFN-containing cure. Specifically, patients with an IFN-free cure were more likely to: be older; have a CTP score of B/C vs. A; be thrombocytopenic; and be treatment experienced. A major finding from this study therefore, is that upon adjusting for these differences (in particular differences in CTP score and platelet count (Fig. 1)), the elevated risk of HCC associated with IFN-free regimens was almost entirely attenuated (aHR 1.15; 95% CI 0.49-2.71). This would tend to indicate that the higher risk of HCC occurrence among individuals receiving IFN-free therapy is a reflection of the shifting patient case mix, as opposed to the pharmacodynamics of IFN-free therapy or any other direct or indirect consequence of IFN-free therapy itself.
Coherence with previous work
The initial studies suggesting a higher risk of HCC occurrence following a IFN-free cure vs. an IFN-containing cure[6], [7], [8] entailed small sample sizes and did not perform multivariate regression against a suitable control group. The present study is consistent with these initial data however, insofar as we too, before multivariate adjustment, found an increased risk of HCC occurrence among patients receiving IFN-free therapy. Yet, this study advances that initial work by reporting considerable attenuation in that "higher" risk after adjustment for relevant confounding factors. Our findings are also consistent with recent work by Cheung et al. from England.19 This study reported that, of 406 patients with decompensated cirrhosis treated with IFN-free therapies, HCC occurred in 4.2% of patients during the first six months from commencing treatment. Although this incidence, at first glance, is high (at least in respect to individuals receiving a IFN-containing cure[9], [10]), it was nevertheless equivalent to occurrence seen in a matched control group comprising untreated patients at a comparable disease stage. Thus, similar to this present study, Cheung et al. found no evidence for an elevated risk of HCC occurrence following IFN-free treatment after benchmarking against an appropriate control group (albeit this study is likely to suffer from the same limitations around HCC surveillance as outlined for this study; see strength and limitations paragraph).
Strengths and limitations
A significant strength of this study is that it robustly addresses a very topical issue, of major importance to patients with HCV and the field of HCV treatment in general. A second strength is that our cohort comprises a majority (∼85%) of cured patients in Scotland. In contrast, previous studies examining this question[5], [6], [7], [8] were confined to patients attending a smaller number of potentially select clinics and may not have been representative of the wider treated/cured population. However, this study has several limitations. Firstly, although our study is one of the largest to-date to examine the risk of HCC occurrence according to IFN-free vs. IFN-containing regimens, our sample size may nevertheless still be inadequate to detect a difference in the risk of HCC by regimen, if that difference was small. Secondly, whilst six-monthly abdominal ultrasound examinations were offered to all patients in this cohort, the uptake of this offer was suboptimal. SA-1 indicates that at least 55% of our cohort had missed a six-monthly ultrasound exam at least once during follow-up. This poor compliance has been found in other settings too,20 however the issue did not affect our headline results - i.e. the pattern of association between regimen and HCC after including additional censoring for screening attrition was no different to our base case result (Fig. S2). Indeed, even though adherence to HCC surveillance is suboptimal, most patients with HCC will present anyway with symptomatic disease within a relatively short timeframe if not identified through screening; as such, one would not necessarily expect this limitation to cause appreciable bias. Another issue is that patients were not necessarily screened for HCC at time zero (i.e. at the point of starting antiviral therapy). Thus, we cannot be absolutely certain that the incident HCC cases identified in our cohort were not already present at the time of starting antiviral therapy. However, we did exclude all cases of HCC that were diagnosed prior to antiviral therapy, and further excluded all cases diagnosed after antiviral therapy if suspicion of that HCC predated treatment onset. Fourthly, a diagnosis of liver cirrhosis was a key eligibility condition for this study. Over the time frame of this study, a cirrhosis diagnosis would typically have been made through a combination of: (i) liver biopsy; (ii) transient elastography; (iii) abdominal ultrasound; (iv) clinical examination and (v) routine liver function tests. However, a further limitation of this study is that we lacked data to describe the exact modality/combination of modalities used to make this diagnosis. Fifthly, our study only examined the risk of HCC occurrence, and not of HCC recurrence. The null association noted here between an IFN-free cure and HCC occurrence, does not in itself rule out an association between an IFN-free cure and HCC recurrence. Although one recent study entailing controlled comparisons from three prospective French cohorts, has recently cast doubt on this association too.21Finally, inclusion in this study required a diagnosis of SVR, meaning that study participants must have survived the time interval between starting treatment and eligibility for SVR 12/SVR 24 assessment. Treatment responders who developed HCC during treatment and died soon after would have been excluded from this study if they did not live long enough to demonstrate SVR; our methods therefore may have missed a small number of patients with rapidly progressive disease. Patients with HCC may be less likely to achieve an SVR,22 and examination of risk of HCC per regimen, independent of SVR would be an alternative approach. The manpower required to conduct a case note review of the large numbers of historic treatment failures, together with the small number of treatment failures with DAAs, made this approach impractical. In addition, assumed equivalence with IFN achieved SVR underpins the rationale and cost effectiveness for treatment with DAAs, making testing this assumption vitally important.
Conclusion
This study, based on data from a large and representative sample of cured hepatitis C patients in Scotland, suggests that the higher risk of HCC occurrence following receipt of IFN-free therapies reflects a change in patient case mix, as opposed to the direct or indirect consequences of IFN-free therapy per se. However, further data from other large cohorts should be sought to confirm these findings.
| |
| |
| |
|
|
|