| |
The cost of comorbidities in treatment for HIV/AIDS in California
|
| |
| |
Download the PDF here
-------------------------------------------
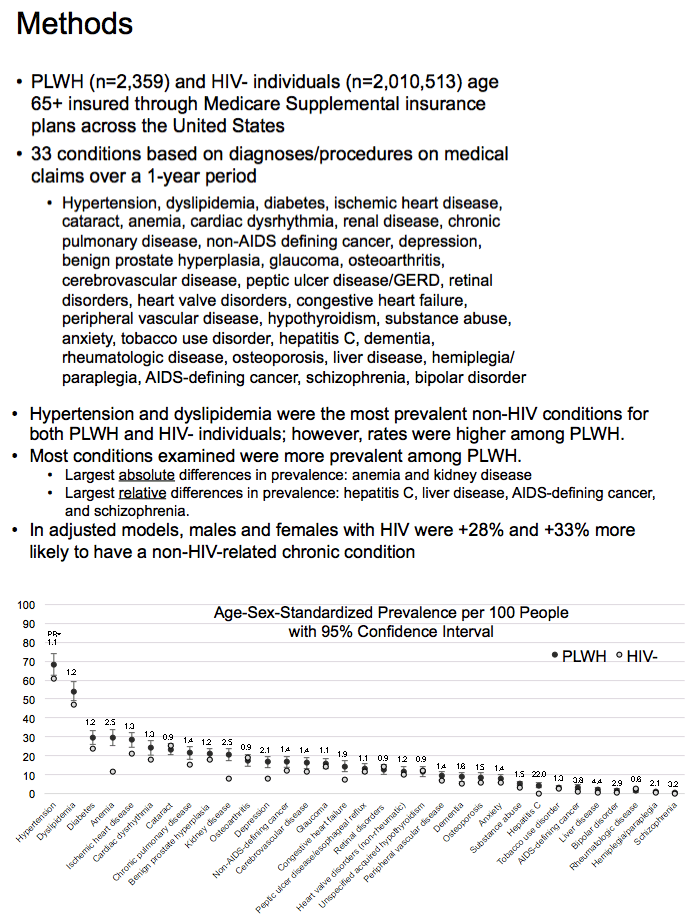
from a separate analysis:
------------------------------------------------------------------
"The aging of the population with HIV will increase the widespread prevalence of comorbidities among PLWH, adding to the already high costs of treatment for this population. Many of the comorbidities that PLWH live with relate to potentially modifiable health habits. However, it may be difficult for providers to effectively provide interventions to modify negative health behaviors because of the small share of HIV care resources devoted to outpatient services........Mean costs of care increased from $30,312 for those without an identified comorbidity to over $46,000 for those with 2 comorbidities, and up to $219,000 for people with 11 or more. Our data confirm that the greater prevalence of comorbidities with increasing age of HIV-infected patients primarily accounts for increased inpatient and outpatient costs with age.[10].....The prevalence of comorbidities likely will increase with the aging of the PLWH population. For example, a modeling study in the Netherlands projects that the percentage of HIV-positive Dutch patients who are over 50 will increase from 28% in 2010 to 73% in 2030. The authors predict that 84% of Dutch HIV-infected patients in 2030 will have 3 or more non-communicable diseases-mostly cardiovascular.....Evidence suggests that patients with HIV have greater numbers of health conditions than age-matched controls. [11,13] Consistent with this, among private insurance beneficiaries with pharmacy benefits, 53.6% of HIV-positive patients over 50 were prescribed more than 5 non-ARV medications over a 12 month period versus 34.3% of HIV negative patients of the same age group.
[13].....comorbidities are associated with increases in median hospital and ambulatory care costs in the PLWH population. Historically, the development of ART dramatically lowered inpatient costs by reducing hospitalization rates for PLWH. Hospitalized PLWH are now more likely to die of conditions other than AIDS (e.g., non-AIDS infections, cardiovascular and liver disease) than of HIV-related conditions, having increased from 43% of hospital deaths among PLWH in 1995 to 70.5% of such deaths in 2011.[27] Our findings suggest that the impact of increasing comorbidities on costs is primarily through greater use of inpatient care, which often requires specialty procedures and intensive care.....health related behavior change may be even more important for PLWH than for the general population. Yet, the ability of physicians to provide comprehensive preventive care and to monitor chronic conditions is constrained by relatively low Medicare and Medicaid reimbursement levels for outpatient primary care, particularly as compared with Ryan White reimbursements. Reimbursements for physician and outpatient clinics remain modest in US public insurance, and have been characterized as "quite meager and ...inadequate to cover the cost of care provision at most HIV clinics in the United States, the majority of which are subsidized by federal and state dollars."[31] Our finding that the share and level of outpatient expenditures are low for Medicare enrollees is particularly relevant because many former Ryan White clients, previously covered by a comprehensive fee, are now covered through the Medicaid expansion, at relatively low reimbursement rates.[32] Similar to Chen, [31] we conclude that outpatient reimbursements are low, given the high rates of preventable comorbidities and the presence of HIV treatment guidelines that call for a minimum of two visits and two viral load assays a year, as well as a number of immunizations and preventive health screens."
Introduction
Care for people infected with HIV has traditionally focused on optimal management of HIV infection and ensuring access to providers with specialty knowledge of HIV care. The success in managing HIV infection has led to increased survival for people living with HIV (PLWH), with the result that in 2014 45% of Americans diagnosed with HIV were aged 50 and older.[1] As a result, PLWH are increasingly experiencing the common diseases of aging.
Non-HIV comorbidities are common among those infected with HIV, particularly among Medicare and Medicaid enrollees. [2-12] The prevalence of comorbidities rises with age. An analysis of health insurance claims data found that 83% of PLWH aged 50 and older and 63% of PLWH aged 18-49 had at least one comorbidity. In contrast, 69% of age/gender matched controls without HIV who were 50 and older had at least one medical condition.[13] A study of Medicare enrollees with HIV found that 20.1% had kidney disease, 19.4% had diabetes, and 27.3% had hyperlipidemia, and 16.0% experienced a cardiovascular event in 2013.[2] Cancer is more prevalent among PLWH than in the general population.[14] Among Medicare enrollees over 65, those with HIV were diagnosed with new cancers over a 5 year period at a rate 50% greater than the cancer incidence rate for Medicare enrollees without HIV.[15]
Multimorbidity is also common among PLWH. Insurance claims data show that among PLWH aged 50 and older, 22% had one medical condition in addition to HIV, 36% had 2-3 comorbidities, 15% had 4-5, and 10% had >5.[13] There is also evidence that PLWH may develop some diseases at earlier ages than people who are not infected with HIV due to immune exhaustion from chronic inflammation engendered by even well-controlled/treated HIV infection.[16]. A study in Italy estimated that PLWH experience rates of non-infectious comorbidities that were comparable to those of patients without HIV who were 10-15 years older. [11]
As care for HIV infections has matured and PLWH are living longer without AIDS, the resources needed to manage and treat their non-HIV comorbidities have increased in importance. One measure of these resources is the cost of treating these comorbidities, which adds to the substantial costs of HIV/AIDS treatment. Historically, overall costs of HIV treatment have been driven largely by the high costs of antiretrovirals and of hospitalizations.[17,18] In recent guidelines for use of ART, HHS calls on providers to inform themselves about antiretroviral regimen costs, patient insurance regulations, and availability of antiretroviral therapy (ART).[19] While the costs of comorbidities have been examined for PLWH in Italy and in Canada, little is known about how treatment for non-HIV comorbidities relate to outpatient, inpatient and pharmaceutical costs for PLWH in the United States, particularly those who are publicly insured.[10-12]
This paper seeks, first, to characterize the number and types of comorbidities diagnosed among publicly-insured PLWH covered by Medicare. Secondly, we examine how comorbidities predict outpatient, inpatient and pharmaceutical expenditure.
Discussion
The findings of this paper describe how medical complexity dramatically increases the already high baseline costs of care for PLWH. In our sample of Medicare enrollees with HIV, nearly 2/3 (64%) had at least one non-HIV related condition, and 39% had two or more. Mean costs of care increased from $30,312 for those without an identified comorbidity to over $46,000 for those with 2 comorbidities, and up to $219,000 for people with 11 or more. Our data confirm that the greater prevalence of comorbidities with increasing age of HIV-infected patients primarily accounts for increased inpatient and outpatient costs with age.[10]
The prevalence of comorbidities likely will increase with the aging of the PLWH population. For example, a modeling study in the Netherlands projects that the percentage of HIV-positive Dutch patients who are over 50 will increase from 28% in 2010 to 73% in 2030. The authors predict that 84% of Dutch HIV-infected patients in 2030 will have 3 or more non-communicable diseases-mostly cardiovascular.[25] Thus there is a need to better understand the impact of increasing comorbidities and in turn, increasing medical expenditures for treatment of PLWH. The current results, which show that including information on comorbidities improves the accuracy of predictions of median costs of treating PLWH, will allow for more accurate forecasts of future medical costs for an aging HIV population subject to greater numbers of comorbidities.
In the current analyses, pharmaceutical costs account for the greatest share of costs for PLWH, but are largely insensitive to comorbidities because the high cost of ART overshadows the cost of drug treatment of other comorbidities. Our data show that drugs account for a 64% of total average costs versus 18% for inpatient costs, continuing the pattern initiated when HAART first came into wide use.[18] In 1996, drugs accounted for 34% of total costs and inpatient 49% of total costs. By 1997, after wider adoption of HAART treatment, drugs' share rose to over half of expenditures and the share of inpatient costs fell to 33% of a total cost of $1,521 per patient per month. [18,26] HAART improved overall survival of PLWH, resulting in extended lifetime, and greater prevalence of comorbidities in this population.
Evidence suggests that patients with HIV have greater numbers of health conditions than age-matched controls. [11,13] Consistent with this, among private insurance beneficiaries with pharmacy benefits, 53.6% of HIV-positive patients over 50 were prescribed more than 5 non-ARV medications over a 12 month period versus 34.3% of HIV negative patients of the same age group. [13]
In contrast to their moderate effect on pharmaceutical costs, comorbidities are associated with increases in median hospital and ambulatory care costs in the PLWH population. Historically, the development of ART dramatically lowered inpatient costs by reducing hospitalization rates for PLWH. Hospitalized PLWH are now more likely to die of conditions other than AIDS (e.g., non-AIDS infections, cardiovascular and liver disease) than of HIV-related conditions, having increased from 43% of hospital deaths among PLWH in 1995 to 70.5% of such deaths in 2011.[27] Our findings suggest that the impact of increasing comorbidities on costs is primarily through greater use of inpatient care, which often requires specialty procedures and intensive care.
This analysis is unique in looking at a range of non-HIV diagnoses to isolate the effect of each diagnosis on the resources used to treat PLWH. Our analysis examines a broad range of comorbidities, not just one, as in Yanik. [15] The most costly comorbidities occur less frequently and different comorbidities are diversely associated with each component of cost. Some, such as hemophilia and metastatic cancer, are associated with extremely high outpatient costs. Others, such as uncomplicated diabetes and pulmonary circulation disorders are associated with high costs for pharmaceuticals. Given the large share of spending on drugs, there is little opportunity to trim spending on either outpatient or inpatient services. [12, 28] An alternative strategy would be to reduce drug expenditures by negotiating with manufacturers to lower their prices-especially given the new recommendations to begin therapy immediately upon diagnosis.
Evidence of the relative contribution of lifestyle factors to morbidity among PLWH is beginning to accumulate.[29] Some have opined that lifestyle changes may have an even more important impact on health in HIV-infected individuals than in the general population, in part because they decrease the inflammatory state. [30] Indeed, we found that comorbidities relating to health habits-diabetes, hypertension, liver disease (hepatitis C), renal insufficiency, are prevalent among those infected with HIV.[2-9, 11] Thus, health related behavior change may be even more important for PLWH than for the general population. Yet, the ability of physicians to provide comprehensive preventive care and to monitor chronic conditions is constrained by relatively low Medicare and Medicaid reimbursement levels for outpatient primary care, particularly as compared with Ryan White reimbursements. Reimbursements for physician and outpatient clinics remain modest in US public insurance, and have been characterized as "quite meager and ...inadequate to cover the cost of care provision at most HIV clinics in the United States, the majority of which are subsidized by federal and state dollars."[31] Our finding that the share and level of outpatient expenditures are low for Medicare enrollees is particularly relevant because many former Ryan White clients, previously covered by a comprehensive fee, are now covered through the Medicaid expansion, at relatively low reimbursement rates.[32] Similar to Chen, [31] we conclude that outpatient reimbursements are low, given the high rates of preventable comorbidities and the presence of HIV treatment guidelines that call for a minimum of two visits and two viral load assays a year, as well as a number of immunizations and preventive health screens.
Limitations
This paper has a number of limitations. First, the data relate only to California and may not generalize to other states. Secondly, only 20% of all PLWH have Medicare coverage. [33] Finally, the analyses rely on insurance claims data, so we do not observe services that were not submitted for reimbursement. However, providers had strong incentives to bill for services they provided. Thus we have confidence in the comprehensiveness of the reports.
Conclusions
The aging of the population with HIV will increase the widespread prevalence of comorbidities among PLWH, adding to the already high costs of treatment for this population. We have shown that including comorbidity measures in predictions of future medical expenditures for PLWH will improve the accuracy of the spending forecasts. Many of the comorbidities that PLWH live with relate to potentially modifiable health habits. However, it may be difficult for providers to effectively provide interventions to modify negative health behaviors because of the small share of HIV care resources devoted to outpatient services.
Sociodemographics
The majority of this sample of PLWH who are enrolled in Medicare are male (90%) and between the ages of 41 and 60 (72%). (Table 1). Whites comprise 57% of the sample while African Americans account for 19% and Hispanics 20%. Over 94% of the sample live in urban areas and approximately two-thirds (63%) had access to a provider treating 50 or more publicly insured patients. Seventy four percent of the Medicare sample also have Medicaid coverage and most (91%) qualified for Medicare due to long-term disability.
The mean Medicare expenditure for California enrollees with HIV was $47,036 in 2010 (Table 1). Drug costs were the largest expense category, accounting for almost 2/3 of the total ($30,052). Mean outpatient costs of $8,714 amounted to 19% of total annual expenditures. The 26% of the sample who experienced an inpatient episode had mean hospital costs of $32,668. Across the entire sample, inpatient costs accounted for 18% of total costs for the average patient.
Comorbidities
Comorbidities were common (Table 1). About 64% of this HIV-positive sample had at least one additional condition. Both mean and median per capita treatment costs rose monotonically with the number of comorbidities.
Table 2 shows the prevalence of individual comorbidities among sample members. The most frequently identified comorbidity was uncomplicated hypertension (32%). A diagnosis of complicated hypertension was received by 5% of enrollees. Uncomplicated diabetes, liver disease, and chronic pulmonary disease were each diagnosed in more than 10% of the sample. The prevalence of cancer was relatively rare: 2% of the sample had lymphoma, fewer than 1% had metastatic cancer and 6% had solid tumors without metastasis.
Regression results
An individual can have more than one comorbidity, thus we examine net costs of each comorbidity in a multi-variable framework that controls for the presence of other comorbidities as well as demographic factors.
Quantile regression was used to relate logged expenditures for each of the cost components (outpatient, drugs, and inpatient costs, if hospitalized) to demographic factors and presence of comorbidities. (Table 3). Logistic regressions modeled the probability of inpatient use. (Table 4). Models that combined Medicare-Only and Dual samples, and included all demographic and comorbidity variables as predictors minimized MAE for outpatient and drug costs, although the improvement over the estimate without covariates was small. (Table 5). The improvement in prediction was greatest for the inpatient model, where adding comorbidities reduced the MAE by 20%, from $8,489 TO $6,792. (Table 6).
Each comorbidity coefficient can be interpreted as the percentage increase in median spending associated with this comorbidity compared to a non-disabled, white, urban, male Medicare-only enrollee of mean age with no other chronic conditions, who did not visit a high volume provider (50+ HIV patients).
Every comorbidity examined increased the cost of outpatient treatment. While obesity and uncomplicated diabetes had modest effects on outpatient costs, (12% and 14% increase in median costs, respectively), all three cancers added substantially to outpatient costs. In contrast, pharmaceutical expenses were relatively insensitive to individual conditions, except in the case of hemophilia.
The median inpatient cost differential associated with each comorbidity varied over a wide range. Logistic regressions (Table 4) show that, as expected, comorbidities and the likelihood of hospitalization are positively related. However, after controlling for comorbidities, age and Dual status had the greatest effects on the odds of hospitalization.
Median outpatient costs also varied by patients' demographic characteristics. Hispanic PLWH incurred lower median cost for outpatient services, while African-Americans had lower costs for both outpatient services and drugs. Female PLWH had about 19% higher outpatient costs, but their medication costs were only 89% of males'. Age did not have a large effect, net of other demographics and comorbidities. Dual enrollees, with both Medicare and Medicaid coverage, had median outpatient costs that were 21% greater than Medicare-Only patients. Patients with high volume providers had slightly higher outpatient and drug costs (8% and 11%, respectively) than patients with lower volume providers.
|
|
| |
| |
|
|
|