 |
 |
 |
| |
The Increasing Importance of Non-alcoholic Fatty Liver Disease (NAFLD) in Patients with Human Immunodeficiency Virus (HIV)
|
| |
| |
Reported by Jules Levin
EASL 2019 April 10-14 Vienna
James Paik1, Linda Henry2, Pegah Golabi1, Saleh A. Alqahtani3, Greg Trimble4, Zobair M. Younossi1,4
1. Betty and Guy Beatty Center for Integrated Research, Inova Health System, Falls Church, VA
2. Center for Outcomes Research in Liver Diseases, Washington, DC
3. Division of Gastroenterology and Hepatology, Johns Hopkins University, Baltimore, MD
4. Center for Liver Disease, Department of Medicine, Inova Fairfax Medical Campus, Falls Church, VA
program abstract
The increasing importance of non-alcoholic fatty liver disease in human deficiency virus (HIV)
positive patients
James Paik1, Pegah Golabi1 2, Greg Trimble2, Leyla Deavila1 2, Linda Henry3, Zobair Younossi1 2
1Betty and Guy Beatty Center for Integrated Research, Inova Health System, Falls Church, United
States; 2Center for Liver Diseases- Department of Medicine, Inova Fairfax Medical Campus, Falls
Church, United States; 3Center for Outcomes Research in Liver Disease, Washington DC, United
States
Background and aims: The development of highly effective antiretroviral regimens for HIV led to a
decrease in the associated mortality. On the other hand, mortality from hepatitis C virus (HCV)-related
liver disease (LD) became a leading cause of death in HIV (+) patients. The recent approval of new
anti-HCV drugs have resulted in high cure rates in HIV-HCV co-infected patients. As viral hepatitis is
effectively treated in HIV (+) patients, NAFLD could become a prominent LD. We aimed to assess the
prevalence and mortality trends of NAFLD, viral hepatitis and other LDs in HIV infected Medicare
recipients in the US.
Method: We used inpatient and outpatient data (random 5%) for the Medicare beneficiaries (1/1/2006
to 12/31/2016) with ICD-9 and ICD-10 diagnostic codes, resource utilization, and mortality rates.
Prevalence rates for HCV, HBV, NAFLD, and other LDs (such as alcohol-LD, cholestatic LD etc.) were
determined. Logistic regression models were used to assess 1-year mortality risk in NAFLD, HBV,
HCV, and controls without LD.
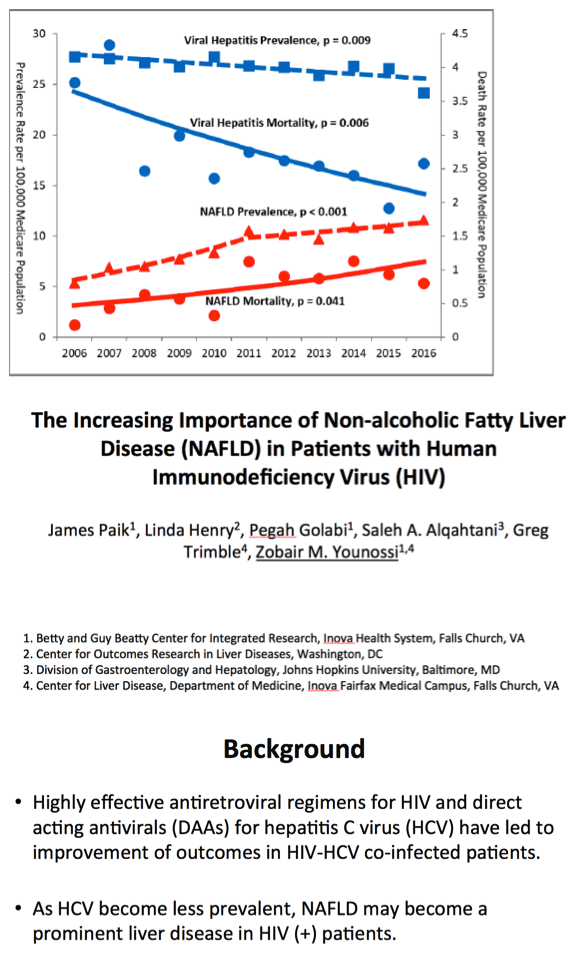
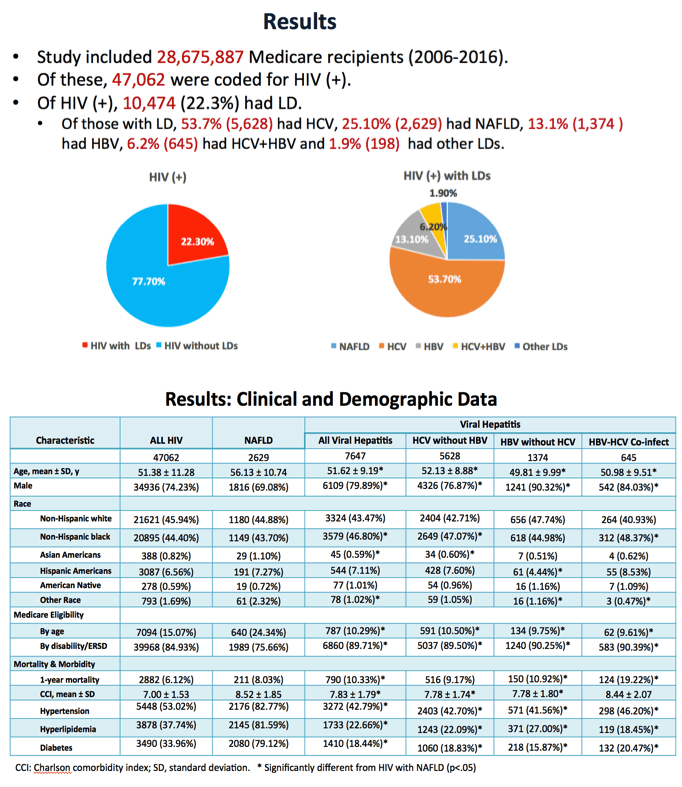
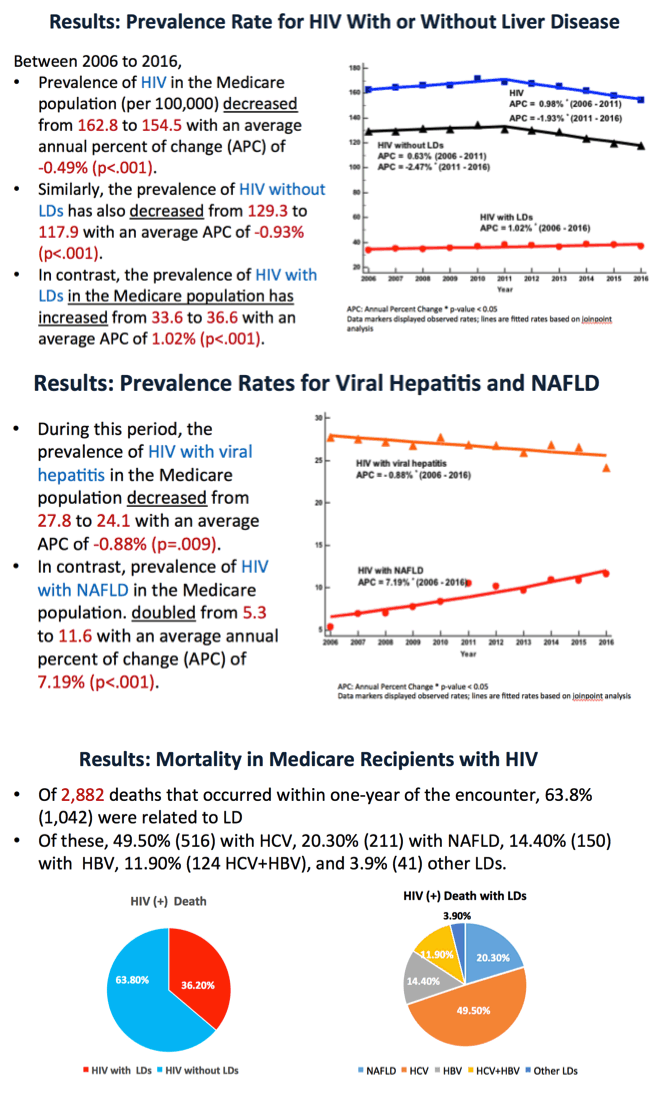
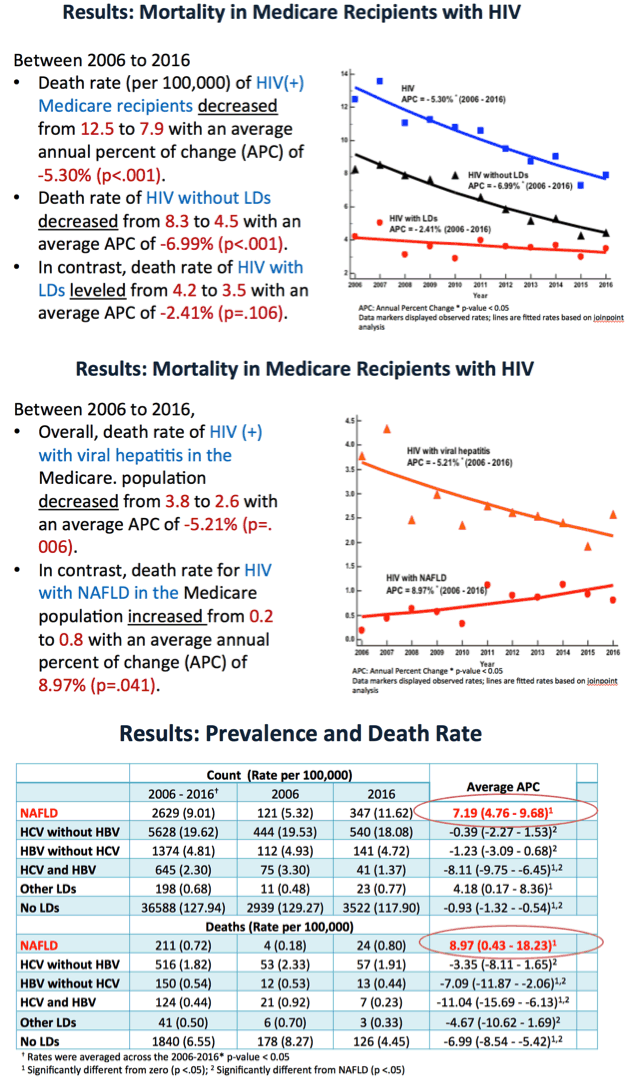
Results: Among the 28, 675, 887 unique Medicare beneficiaries, there were 47, 062 HIV (+) subjects with 10, 474 having LD (5, 628 HCV, 1, 374 HBV, 645 HCV+HBV, 2, 629 NAFLD, 198 other LDs.). Between 2006 and 2016, rates for viral hepatitis decreased from 27.75 to 24.17 (p = .009) while, the rate for NAFLD in HIV (+) Medicare recipients doubled from 5.32 to 11.62 per 100, 000 (p < .001).
During the study period, there were 2, 882 deaths within one-year of the encounter. Of these, 36.2% were related to LD (49.5% dying from HCV, 14.4% from HBV, 11.9% from HCV+HBV, 20.3% from NAFLD, and 3.9% from other LDs).
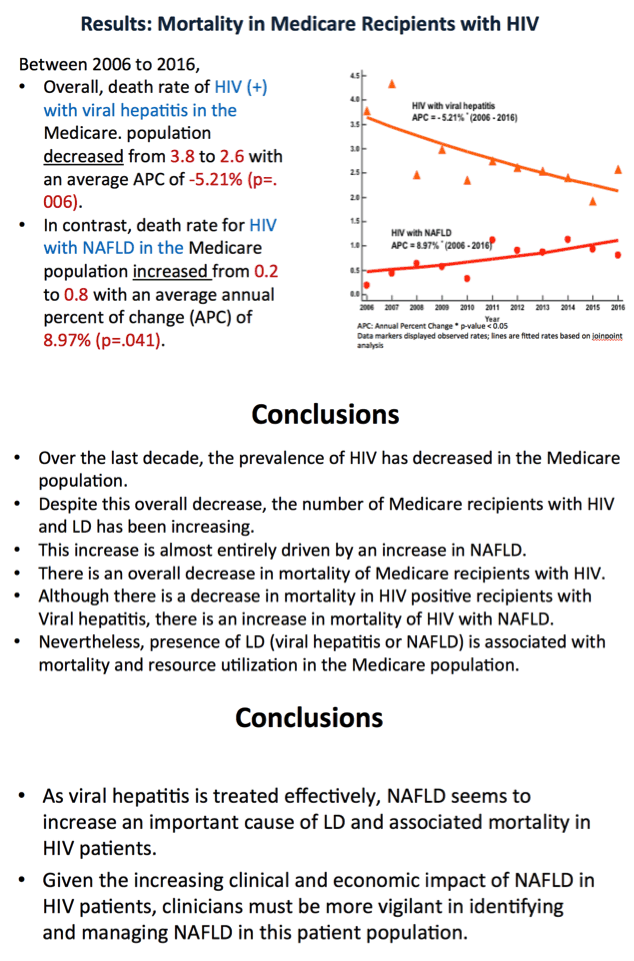
During the study period, the death rates related to viral hepatitis in HIV (+) Medicare recipients decreased from 3.78 to 2.58 (p = .006), while the mortality for NAFLD in this group increased from 0.18 to 0.80 for NAFLD (p = .041).
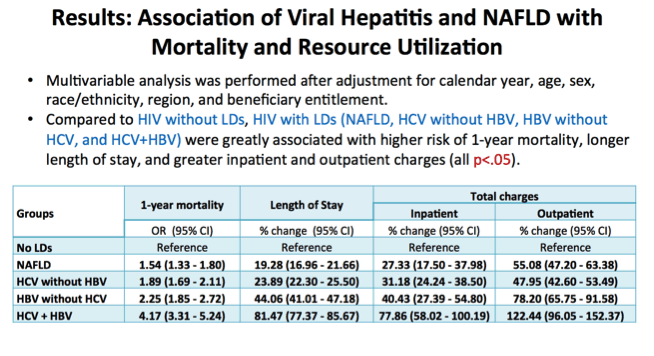
After adjustments for calendar year, age, sex, race/ethnicity, region, and beneficiary entitlement, presence of HCV (Odds ratio [OR] = 1.89, 95% CI: 1.69-2.11), HBV (OR = 2.25, 95% CI: 1.85-2.72), HCV+HBV (OR = 4.17, 95% CI: 3.31-5.24), and NAFLD (OR = 1.54, 95% CI: 1.33-1.80) were associated with increased risk of 1-year mortality in the HIV (+) Medicare recipients [vs. HIV (+) without LD].
Conclusion: As highly effective regimens for HIV, HBV and HCV lead to a reduction in associated mortality in HIV (+) patients, NAFLD is increasing as an important cause of LD and reason for liver mortality in this group of patients.
Figure:

|
| |
|
 |
 |
|
|