 |
 |
 |
| |
Increasing Number of Metabolic Co-Morbidities are Associated
with Higher Risk of Advanced Fibrosis in Patients with Nonalcoholic
Steatohepatitis
|
| |
| |
Reported by Jules Levin
EASL 2019 April 10-14 Vienna
Robert Wong1, Tram Tran2, Harvey Kaufman3, Justin Niles3,
Robert G. Gish4.
1Alameda Health System, Oakland, United States;
2Gilead Sciences, Inc., Foster City, United States; 3Quest Diagnostics
Corporate Headquarters, Secaucus, United States; 4Stanford Health Care,
Palo Alto, United States

program abstract
Background and aims: Accurate estimates of non-alcoholic steatohepatitis (NASH) prevalence are lacking, particularly the subset of patients with advanced fibrosis. We aim to evaluate prevalence and predictors of advanced fibrosis among patients with probable NASH using national clinical laboratory data.
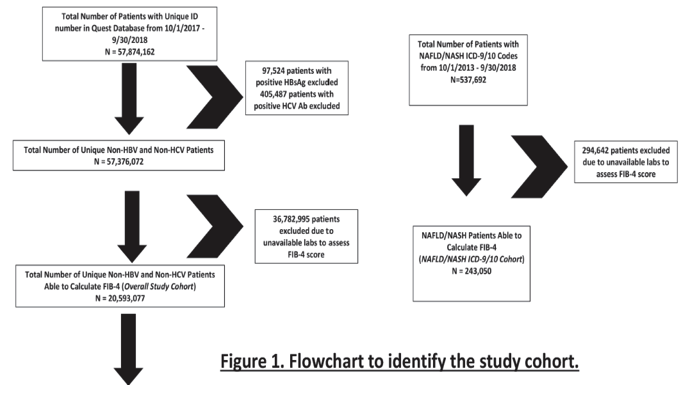
Method: Clinical laboratory data from October 1, 2017-September 30, 2018 were collected using Quest Diagnostics database, which tests ∼30% of U.S. adults annually. Adults with negative hepatitis B surface antigen, negative hepatitis C antibody, and elevated alanine aminotransferase (ALT) (>25 U/L women, >35 U/L men) were evaluated for prevalence of ≥F 3 fibrosis using fibrosis-4 score (FIB-4)>2.67.
Patients were grouped by presence of one, two, or three concurrent metabolic co-morbidities (decreased high density lipoprotein (<40 mg/dL in men, <50 mg/dL in women), elevated triglycerides (≥1 50 mg/dL), or elevated hemoglobin A1C (≥6 .5%)). We further evaluated patients specifically with NAFLD/NASH ICD-9/10 codes from October 1, 2013-Septebmer 30, 2018 (n = 243, 050). Multivariate logistic regression models evaluated for predictors of ≥F 3 fibrosis.
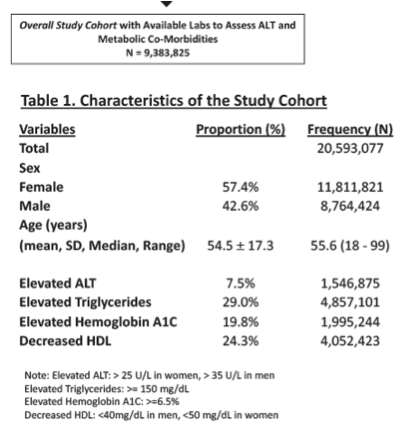
Results: Among 20, 593, 077 patients (42.6% male, mean age 54.5), 9.4 million had available results to assess ALT and metabolic comorbidities.
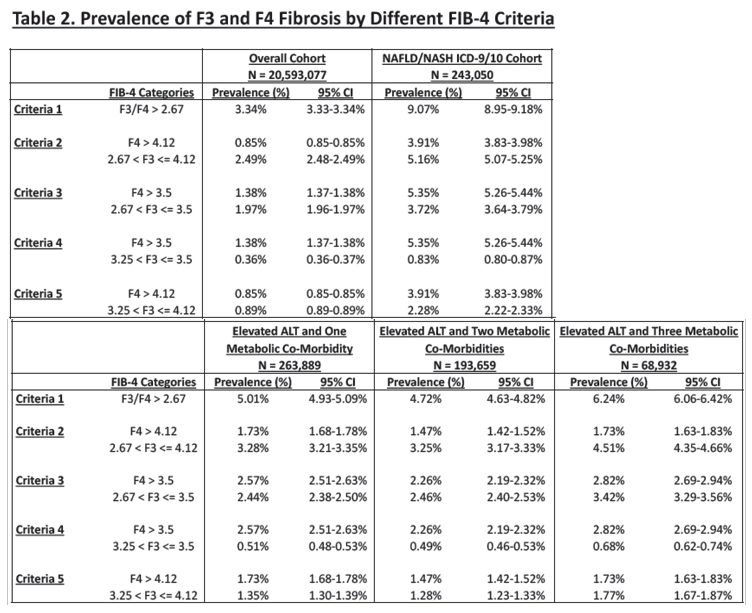
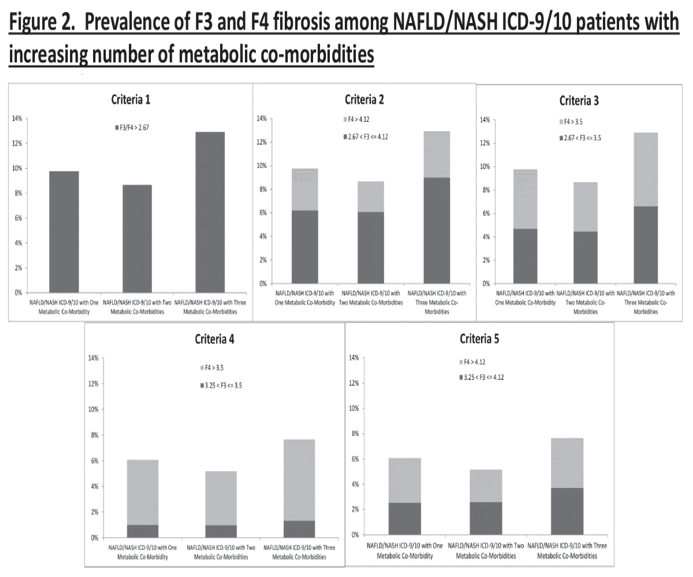
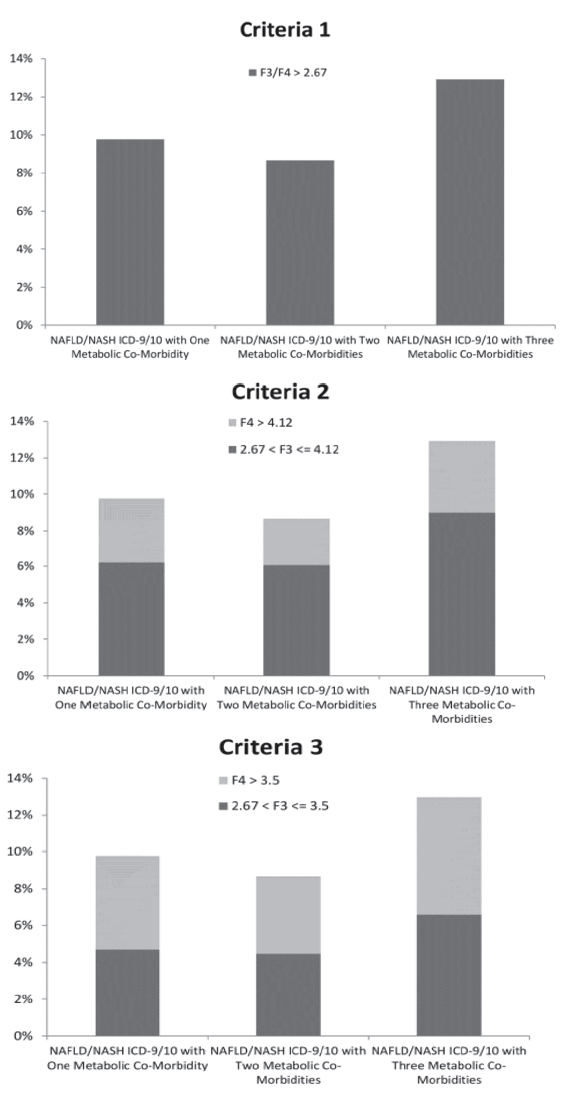
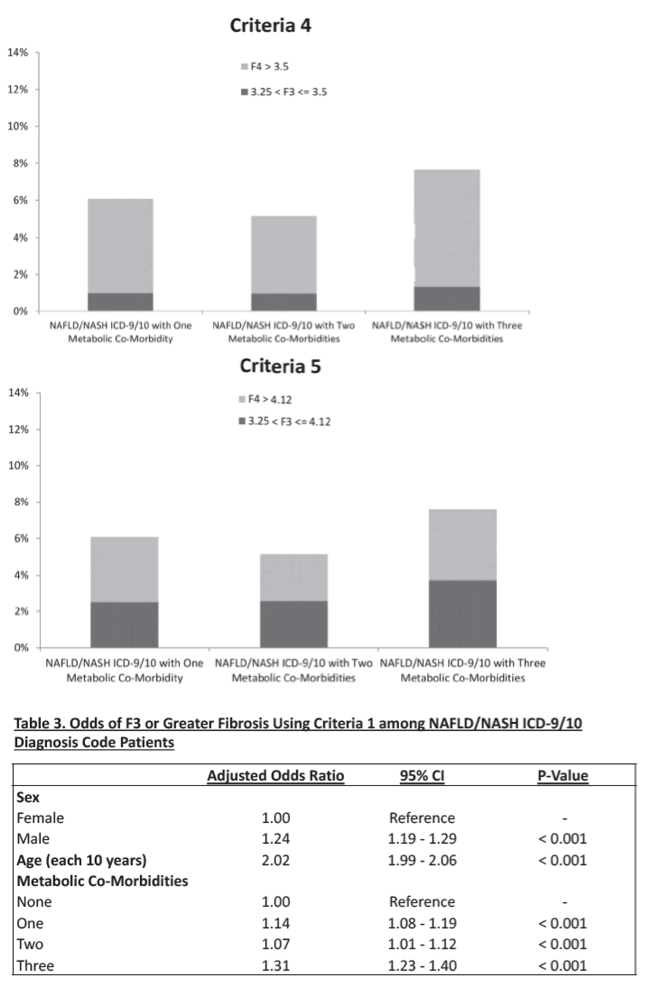
Overall prevalence of ≥F 3 fibrosis was 3.34% (95% CI 3.33-3.34), which increased from 4.72% (95% CI 4.63-4.82) in patients with one metabolic co-morbidity to 6.24% (95% CI 6.06-6.42) in patients with three metabolic co-morbidities. Among patients with NAFLD/NASH ICD-9/10 codes, prevalence of ≥F 3 fibrosis was 9.07% (95% CI 8.95-9.18), which increased from 9.77% (95% CI 9.18-10.36) in patients with one metabolic co-morbidity to 12.91% (95% CI 11.79-14.03) in patients with three metabolic co-morbidities. On multivariate regression, significantly higher odds of ≥F 3 fibrosis was observed in men vs. women (OR 1.24, 95% CI 1.19-1.29), every 10-year increase in age (OR 2.02, 95% CI 1.99-2.06), and concurrent metabolic abnormalities (OR for three metabolic abnormalities vs. none: 1.31, 95% CI 1.23-1.40).
Conclusion: Among a large national sample of U.S. adults, estimated prevalence of ≥F 3 fibrosis among NASH patients ranged from 3.34- 9.07%, representing 2.5-6.8 million individuals.
Concurrent metabolic co-morbidities are associated with significantly higher odds of advanced fibrosis with estimated prevalence as high as 12.91% in patients with NASH and three metabolic co-morbidities.


|
| |
|
 |
 |
|
|