| |
Study Confirms Tesamorelin Significantly Reduces Liver Fat
in HIV Patients With NAFLD - press announcement
|
| |
| |
By
Published: Apr 1, 2019
--------------
Download the PDF here
"There are currently no guidelines that recommend universal screening for NAFLD in the general population or in specific subpopulations. In contrast, the European AIDS Clinical Society (EACS) guideline recommends screening for NAFLD in HIV-infected patients with metabolic syndrome using ultrasound [42]. Since the prevalence of NAFLD among HIV-infected patients with persistent liver enzyme elevations is high, ultrasound screening should also be considered in this population......NAFLD is a clinical-histological diagnosis characterized by the presence of fat accumulation in hepatocytes resulting in necro-inflammation and hepatocyte ballooning in the absence of excessive alcohol use [43]. According to the American Association for the Study of Liver Diseases (AASLD), the threshold of 'significant alcohol consumption' is > 21 standard drinks per week on average for men and > 14 standard drinks on average in woman when evaluating patients with suspected NAFLD [44]. In general, NAFLD is considered to be the hepatic manifestation of the metabolic syndrome. The study of Mellinger et al. showed an association between presence of NAFLD and coronary artery calcium [OR 1.20 (1.10-1.30) P < 0.001][45]. This finding was confirmed in the HIV-positive population in the study of Crum-Cianflone et al., showing that high coronary artery calcification values are associated with the presence of steatosis [46]. Although the natural history of steatosis is usually benign, approximately 10% of patients with 'simple' steatosis progress to NASH. Eventually, 25-35% of the patients with NASH progress to liver fibrosis or even cirrhosis. Eventually, 10% of patients with cirrhosis develop hepatocellular carcinoma (HCC) over a period of several years [36, 37] (Fig. 1)......Insulin resistance (IR) is considered to be the key mechanism in the development of steatosis [47]. IR contributes to hepatic triglyceride accumulation in two ways......high BMI, waist circumference, type 2 diabetes, hypertension and high triglycerides as the significant risk factors for NAFLD
........suggestive of a direct steatotic effect of HIV itself ........obesity-related IR. Insulin resistance is highly prevalent-up to 35%-in HIV-infected patients, as a result of ongoing immune activation...... high levels of pro-inflammatory markers-e.g. TNF alpha and IL-6-were associated with IR [65]. These markers have also been shown to be elevated in chronic HIV-infection, but it is unclear to what extent other immune activation markers like sCD14 and the expansion of CD8+/HLA-DR+ subtype T cells contribute to IR in HIV .......advanced HIV-infection-defined as low CD4 counts and detectable viral load-and IR, measured by fasting lipids, glucoses and insulin levels. This and other observations strongly suggest a link between chronic HIV-induced immune activation and IR with subsequent steatosis development [68-70].......Nucleoside/nucleotide reverse transcriptase inhibitors (NRTIs) are still an essential part of current cART regimens. Especially, early-generation NRTIs are associated with insulin resistance and dyslipidemia [76-78]. The main driver for both metabolic disturbances is mitochondrial toxicity. The first reports of mitochondrial dysfunction in NRTIs were published in the early 1990s, but this adverse event gained increasing attention after the introduction of combination therapy [79-81]. NRTI-related metabolic side effects are caused by the inhibition of the replication of mitochondrial DNA (mtDNA).....unfavorable metabolic profile with an increased risk for insulin resistance and dyslipidemia......maraviroc and enfuviritide) are limited, but no negative effects have so far been reported [109, 110]. None of these agents are implicated in the development of NAFLD......new NNRTI Doravirine was approved by the FDA.....showed lower triglyceride and LDL levels when compared to Efavirenz and Darunavir."
--------------------------
Press Release
Study Confirms Tesamorelin Significantly Reduces Liver Fat in HIV Patients With NAFLD
By
Published: Apr 1, 2019
MONTREAL, April 01, Apr 01, 2019 - Theratechnologies Inc. (Theratechnologies) (TH) today announced that top-line results, from a study funded by the National Institutes of Health led by Dr. Steve Grinspoon and conducted at the Massachusetts General Hospital and Harvard Medical School and the National Institutes of Health, conclude that tesamorelin significantly reduces liver fat in HIV patients with Non Alcoholic Fatty Liver Disease (NAFLD) which was the primary endpoint of the study.
Initial results reported are from the preliminary phase of a 12-month randomized, double-blind, placebo-controlled clinical trial. A total of 61 men and women with HIV infection and hepatic fat fraction greater-than or equal to 5%, assessed by magnetic resonance spectroscopy, were enrolled; 31 patients were randomized in the tesamorelin group while 30 patients were enrolled in the placebo group. At baseline, patients enrolled in the study had hepatic fat levels of 13.8%. In total, 43% of patients had fibrosis as assessed by liver biopsies.
The study achieved its pre-specified primary endpoint. In patients on tesamorelin, liver fat decreased by 32% while it increased by 5% in placebo patients, from baseline, (p=0.02), amounting to a 37% relative reduction in liver fat. Furthermore, 35% of patients in the tesamorelin group returned to liver fat values below 5% in comparison to only 4% of patients on placebo (p=0.007).
Secondary endpoints suggest potential benefits for fibrosis prevention as preliminary results are showing less progression with tesamorelin than placebo. More results will be made available as data analysis is completed.
NAFLD is a strong precursor of NASH which can lead to fibrosis and severe health consequences such as liver cirrhosis. It is estimated that 25% or more of HIV patients have NAFLD. [1]
"Findings from this study have significant clinical implications. Currently, there are no pharmacologic treatments available for NAFLD or NASH specifically proven in HIV patients, among whom NAFLD is common. While tesamorelin is not indicated for the treatment of NAFLD or NASH, the robust results obtained in this NIH-funded study clearly indicate that tesamorelin has now become a prime candidate for a potential indication in the treatment of NAFLD-NASH with further studies," said Dr. Christian Marsolais, Senior Vice President and Chief Medical Officer, Theratechnologies Inc.
"Data analysis is ongoing and Theratechnologies will quickly establish a strategy regarding the potential options now available for the continued development of tesamorelin," said Luc Tanguay President and CEO of Theratechnologies.
Tesamorelin is currently commercialized under the tradename of EGRIFTA [(R)] for the reduction of excess abdominal fat or visceral adipose tissue (VAT) in HIV-infected patients with lipodystrophy.
About EGRIFTA(R)
EGRIFTA(R) is currently approved in the United States, Canada and Mexico for the reduction of excess abdominal fat or visceral adipose tissue (VAT) in HIV-infected patients with lipodystrophy.
You should not take EGRIFTA(R) if you
⋅ have or have ever had any problems with your pituitary gland.
⋅ have cancer or are receiving treatment for cancer.
⋅ are allergic to tesamorelin or any of the ingredients in EGRIFTA(R).
⋅ are pregnant or become pregnant. If you become pregnant, stop using EGRIFTA(R) and talk with your healthcare provider.
⋅ are less than 18 years of age.
The most common side effects of EGRIFTA [(R)] include: joint pain, pain in legs and arms, swelling in your legs, muscle pain, tingling, numbness and pricking, nausea, vomiting. For more information on EGRIFTA(R), please visit www.egrifta.com.
Full prescribing information available at www.egrifta.com
About Theratechnologies
Theratechnologies (TH) is a specialty pharmaceutical company addressing unmet medical needs by bringing to market specialized therapies for people with orphan medical conditions, including those living with HIV. Further information about Theratechnologies is available on the Company's website at www.theratech.com and on SEDAR at www.sedar.com.
Forward-Looking Information
This press release contains forward-looking statements and forward-looking information, or, collectively, forward-looking statements, within the meaning of applicable securities laws, that are based on our management's beliefs and assumptions and on information currently available to our management. You can identify forward-looking statements by terms such as "may", "will", "should", "could", "would", "outlook", "believe", "plan", "envisage", "anticipate", "expect" and "estimate", or the negatives of these terms, or variations of them. The forward-looking statements contained in this press release include, but are not limited to, statements regarding the potential development of tesamorelin and the timing of disclosure of additional study results.
Forward-looking statements are based upon a number of assumptions and include, but are not limited to, the following: sufficient market indicators and data will warrant the further development of tesamorelin for the potential treatment of NAFLD or NASH, and all data analysis will be rapidly completed to assess all Company's options related to such development.
Forward-looking statements are subject to a variety of risks and uncertainties, many of which are beyond our control that could cause our actual results to differ materially from those that are disclosed in or implied by the forward-looking statements contained in this press release. These risks and uncertainties include, among others, that further data analysis and market indicators do not warrant further development of tesamorelin.
We refer potential investors to the "Risk Factors" section of our annual information form dated February 20, 2019 for additional risks regarding the conduct of our business and Theratechnologies. The reader is cautioned to consider these and other risks and uncertainties carefully and not to put undue reliance on forward-looking statements.
Forward-looking statements reflect current expectations regarding future events and speak only as of the date of this press release and represent our expectations as of that date.
We undertake no obligation to update or revise the information contained in this press release, whether as a result of new information, future events or circumstances or otherwise, except as may be required by applicable law.
For media inquiries:
Denis Boucher
Vice President, Communications and Corporate Affairs
514-336-7800
[1] Infect Dis Ther. 2019 Mar;8(1):33-50.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6374241/
---------------------
HIV as Risk Factor for NAFLD
The term NAFLD encompasses a wide spectrum of entities ranging from 'simple' steatosis to non-alcoholic steatohepatitis (NASH) [7]. Since the major risk factors for NAFLD-insulin resistance [8, 9], mitochondrial dysfunction [10] and concurrent viral infections [11]-are highly prevalent in HIV-infected patients, this population is at risk for liver-related morbidity.
In this review, we describe the epidemiology and pathogenesis of NAFLD in HIV-infected patients. We also discuss the future with respect to novel (antiretroviral) medication and anti-NAFLD interventions. This article is based on previously conducted studies and does not contain any studies with human participants or animals performed by any of the authors.
Although NAFLD is common in HIV-infected patients as a result of traditional risk factors, it is suggested that its exact aetiology may differ from the general population [59]. Interestingly, histopathological studies from the pre-cART era report high numbers of steatosis in treatment-naïve HIV-infected patients-suggestive of a direct steatotic effect of HIV itself [60, 61]. Furthermore, HIV-infected patients with NAFLD tend to have a lower BMI than HIV-negative controls with NAFLD [62]. These data suggest that HIV-related factors are associated with NAFLD, even in the absence of traditional risk factors such as obesity-related IR. Insulin resistance is highly prevalent-up to 35%-in HIV-infected patients, as a result of ongoing immune activation [63, 64]. This phenomena has also been described in the setting of rheumatoid arthritis in which high levels of pro-inflammatory markers-e.g. TNF alpha and IL-6-were associated with IR [65]. These markers have also been shown to be elevated in chronic HIV-infection, but it is unclear to what extent other immune activation markers like sCD14 and the expansion of CD8+/HLA-DR+ subtype T cells contribute to IR in HIV [66]. Most studies on IR in this population describe cART-treated patients, but only one study evaluated the occurrence of IR in treatment-naïve HIV-positive patients [67]. In this heterogeneous prospective cohort, there was a clear association between advanced HIV-infection-defined as low CD4 counts and detectable viral load-and IR, measured by fasting lipids, glucoses and insulin levels. This and other observations strongly suggest a link between chronic HIV-induced immune activation and IR with subsequent steatosis development [68-70].
In contrast to the limited number of studies on glucose haemostasis in HIV-positive patients, several studies have been performed on the occurrence of dyslipidemia-also associated with NAFLD [50]. A study in the early 1990s established that untreated HIV-infected patients with advanced immunodeficiency have higher triglycerides and FFA levels compared to healthy controls [71]. In addition to hypertriglyceridemia, untreated HIV-infected patients have decreased high-density lipoprotein cholesterol and total cholesterol levels. These observations were confirmed in several other studies, although the mechanism of HIV-related dyslipidemia is poorly understood. [72, 73] The study by El-Sadr et al. even established an association between high HIV RNA levels and hypertriglyceridemia [67]. Based on these observations, it seems reasonable to assume that HIV-infection itself plays a role in the development of NAFLD.
Antiretroviral Therapy as a Risk Factor for NAFLD
As the vast majority of HIV-infected patients treated with cART will reach virological suppression and (near) inhibition of immune activation, the impact of hypertriglyceridemia and IR caused by the virus itself will diminish. In contrast, certain antiretroviral therapy can contribute to the development of NAFLD [74]. cART seems to influence the development of NAFLD in two different ways. First, several antiretroviral drugs cause unfavorable metabolic changes such as dyslipidemia and insulin resistance [75]. Second, the use of certain antiretroviral drugs is associated with mitochondrial dysfunction.
Nucleoside/Nucleotide Reverse Transcriptase Inhibitors (NRTIs)
Nucleoside/nucleotide reverse transcriptase inhibitors (NRTIs) are still an essential part of current cART regimens. Especially, early-generation NRTIs are associated with insulin resistance and dyslipidemia [76-78]. The main driver for both metabolic disturbances is mitochondrial toxicity. The first reports of mitochondrial dysfunction in NRTIs were published in the early 1990s, but this adverse event gained increasing attention after the introduction of combination therapy [79-81]. NRTI-related metabolic side effects are caused by the inhibition of the replication of mitochondrial DNA (mtDNA) by binding to intra-mitochondrial polymerase gamma. This leads to impairment of the oxidative phosphorylation and promotes the formation of reactive oxygen species which eventually damage the mtDNA even further, resulting in mitochondrial dysfunction [82].
NRTI-related mitochondrial dysfunction contributes to the development of NAFLD in several ways. First, both IR and dyslipidemia can be the result of mitochondrial dysfunction in the peripheral fat tissue [83]. Even though the mechanism is not exactly clear, mitochondrial dysfunction seems to induce adipocyte apoptosis, leading to peripheral lipodystrophy. The clinical syndrome is characterized by the degeneration of peripheral fat tissue combined with metabolic changes such as IR and dyslipidemia [81, 84]. In addition to peripheral effects, mitochondrial dysfunction also occurs in the liver. Hepatic mitochondria play an essential role in the oxidation of FFAs. In the setting of mitochondrial dysfunction, mitochondria are unable to process this oxidation, leading to a local accumulation of triglycerides which is the hallmark of NAFLD [85]. Early-generation NRTIs are most commonly associated with mitochondrial dysfunction; especially stavudine, didanosine, zalcitabine and-to a lesser extent-zidovudine [86]. Modern NRTIs-e.g. tenofovir, abacavir, lamivudine and emtricitabine-are rarely implicated in clinically significant mitochondrial dysfunction and are less likely to contribute to NAFLD development in this way [87].
Protease Inhibitors (PIs)
Introduction of protease inhibitors (PIs) in 1995 broadened the possibilities in the treatment of HIV infection. However, PIs display an unfavorable metabolic profile with an increased risk for insulin resistance and dyslipidemia.
Especially, the early-generation PIs-e.g. indinavir and therapeutic-dosed ritonavir-were known for their ability to induce IR [88]. Two animal studies showed that these PIs act as potent isoform-specific inhibitors of the transport function of the GLUT4-receptor, resulting in hyperglycemia and hyperinsulinemia [89, 90]. Additional data suggested the ability to directly inhibit insulin secretion from the beta cells [91, 92]. In contrast to early-generation PIs, current PIs like atazanavir and darunavir display a far more favorable profile with regard to IR [93]. Although the newer generation PIs seem to have little impact on the lipid levels in monotherapy, when combined with ritonavir or cobicistat as a pharmacological booster, these drugs still have an unfavorable lipid profile compared to most other classes of antiretroviral drugs [94-97]. The exact mechanism of PI-induced dyslipidaemia remains the subject of debate. Data suggest that PIs attribute to an increase of ApolipoproteinB which transports LDL- and VLDL-cholesterol and triglycerides in the circulation [98]. Secondly, experimental research in mice showed that ritonavir inhibits the clearance of triglycerides from the circulation [99].
Non-Nucleoside Reverse Transcriptase Inhibitors (NNRTIs)
The amount of data describing the metabolic profile of the non-nucleoside reverse transcriptase inhibitors (NNRTIs) is limited compared to the number of studies for PI-based treatment. Rilpivirine and nevirapine have a more favorable profile compared to efavirenz [100, 101]. Etravirine does not seem to influence lipid levels when compared with placebo [102]. Recently, the new NNRTI Doravirine was approved by the FDA; in the DRIVE-AHEAD and DRIVE-FORWARD trials, this novel drug showed lower triglyceride and LDL levels when compared to Efavirenz and Darunavir [103, 104].
Integrase Strand Transfer Inhibitors (INSTI)
In 2008, the first integrase strand transfer inhibitor (INSTI), raltegravir, was introduced. This new drug class is generally considered advantageous in respect with the metabolic profile. [105, 106] The lipid profile of the recently approved bictegravir is comparable to dolutegravir. [107, 108].
Other Antiretroviral Classes
Data on entry-inhibitors (e.g. maraviroc and enfuviritide) are limited, but no negative effects have so far been reported [109, 110]. None of these agents are implicated in the development of NAFLD.
Non-HIV or -cART-Related Risk Factors for NAFLD
In addition to the risk factors that are directly linked to HIV-infection and cART, HIV-infected patients are exposed to other risk factors for the development of NAFLD. First of all, a significant proportion of the population is suffering from a hepatitis C virus (HCV)/HIV co-infection [111]. HCV genotype 3 has been identified as an independent risk factor for the development of NAFLD [112]. The current literature suggests that these specific genotype 3 antigens induce upregulation of hepatic fatty acid synthesis [113, 114]. When HCV genotype 3-infected patients achieve sustained viral response (i.e. cure) after treatment, the degree of steatosis diminishes [115]. In contrast to HCV genotype 3 infection, the current literature suggests that hepatitis B virus is associated with a lower risk for NAFLD [116]. However, the most important non-HIV/non-cART risk factors are probably the previously mentioned 'traditional' risk factors such as obesity-related IR and diabetes mellitus. Nowadays, HIV-patients grow old enough to be exposed to these traditional risk factors. Recent publications describe increases in median body-mass index (BMI) and the incidence of diabetes mellitus in the HIV-infected population, adding more risks for this population [14, 117, 118]. The impact of traditional risk factors was emphasized by the results of the meta-analysis of Maurice et al., identifying high BMI, waist circumference, type 2 diabetes, hypertension and high triglycerides as the significant risk factors for NAFLD [19].
Abstract
The burden of liver-related morbidity remains high among HIV-infected patients, despite advances in the treatment of HIV and viral hepatitis. Especially, the impact of non-alcoholic fatty liver disease (NAFLD) is significant with a prevalence of up to 50%. The pathogenesis of NAFLD and the reasons for progression to non-alcoholic steatohepatitis (NASH) are still not fully elucidated, but insulin resistance, mitochondrial dysfunction and dyslipidemia seem to be the main drivers. Both HIV-infection itself and combination antiretroviral therapy (cART) can contribute to the development of NAFLD/NASH in various ways. As ongoing HIV-related immune activation is associated with insulin resistance, early initiation of cART is needed to limit its duration. In addition, the use of early-generation nucleoside reverse transcriptase inhibitors and protease inhibitors is also associated with the development of NAFLD/NASH. Patients at risk should therefore receive antiretroviral drugs with a more favorable metabolic profile. Only weight reduction is considered to be an effective therapy for all patients with NAFLD/NASH, although certain drugs are available for specific subgroups. Since patients with NASH are at risk of developing liver cirrhosis and hepatocellular carcinoma, several non-antifibrotic and antifibrotic drugs are under investigation in clinical trials to broaden the therapeutic options. The epidemiology and etiology of NAFLD/NASH in HIV-positive patients is likely to change in the near future. Current guidelines recommend early initiation of cART that is less likely to induce insulin resistance, mitochondrial dysfunction and dyslipidemia. In contrast, as a result of increasing life expectancy in good health, this population will adopt the more traditional risk factors for NAFLD/NASH. HIV-treating physicians should be aware of the etiology, pathogenesis and treatment of NAFLD/NASH in order to identify and treat the patients at risk.
Epidemiology
The worldwide prevalence of NAFLD varies greatly among different geographical areas, with the highest numbers in northern America and the lowest in Africa; overall prevalence is estimated to be around 25% [12]. In addition to many epidemiological studies in the general population, several studies describe the prevalence in a general HIV-infected population, with a prevalence varying from 28 to 48% [13-18]. In the meta-analysis by Maurice et al., the prevalence of imaging-based diagnosis of NAFLD was 35%, which is higher than the general population [19]. In patient populations with persistent liver enzyme elevations, the prevalence is even higher with approximately three-quarters of the patients having NAFLD [20-24] (Table 1). However, Price et al. performed a matched-control study which surprisingly showed a higher prevalence of NAFLD in the HIV-negative control group compared to their HIV-positive counterparts (19% vs. 13%, P = 0.02) [25]. This prevalence will be an underestimation of the 'real-life' prevalence due to exclusion of patients with a history of cardiovascular surgery and those with severe excess body weight. In another report, the imaging-based prevalence of NAFLD in a small cohort of HIV-positive patients was compared with HIV-negative controls [26]. The prevalence of steatosis tended to be higher among HIV-infected men compared to HIV-negative men (41% vs. 33%; not statistically significant), but was lower in HIV-positive versus HIV-negative women (17% vs. 33%). Both studies showed that classic risk factors-such as obesity-related insulin resistance-were the most important determinants for the development of NAFLD; HIV-related factors certainly contributed to this risk but its impact appeared to be limited. Therefore, it remains difficult to draw conclusions from these small studies because of methodological issues and small sample sizes; larger cross-sectional studies are thus needed.
Diagnosis
The gold standard in diagnosing NAFLD is liver biopsy by which discrimination between steatosis and NASH is possible [27]. Given its invasive nature with risks such as haemorrhagic complications and pain, liver biopsy is not useful as an epidemiological screening tool [28]. As a result, current cross-sectional epidemiological data are mainly based on surrogate markers such as imaging rather than on histopathological data. Considering the higher sensitivity, lower costs and wide availability, ultrasound is preferred over CT-scanning for diagnosing NAFLD [29]. However, its sensitivity is limited in the setting of mild NAFLD and in morbidly obese patients [30, 31]. Magnetic resonance spectroscopy proton density fat fraction (MRS-PDFF) is a very sensitive imaging modality, with a sensitivity up to 100% [31]. Due to its wider availability and low risk for sampling error, magnetic resonance imaging proton density fat fraction (MRI-PDFF) is increasingly used in research. In a recent review by Caussy et al., the differences and impact of MRS-PDFF and MRI-PDFF were extensively discussed. Considering the high costs and limited availability, MRI-based imaging is currently still not a useful screening tool and its use remains limited to research [32]. In 2010, a new non-invasive tool for the detection of steatosis, called controlled attenuation parameter (CAP), was introduced [33]. It is an addition to the Fibroscan (Echosens, Paris, France) and measures steatosis simultaneously with fibrosis. CAP determines the total ultrasonic attenuation at a frequency of 3.5 MHz and is reported in decibel/meter (dB/m). In a meta-analysis by Wang et al., CAP provided good sensitivity and specificity [34]. For example, the sensitivity for the detection of ≥ S1 steatosis (≥ 5% of the hepatocytes affected with lipid accumulation) was 0.78 with an area under the curve (AUC) of 0.86 (95% CI 0.82-0.88). For stage S3 (> 66% of the hepatocytes affected), the sensitivity was 0.86 with an AUC of 0.94 (95% CI 0.91-0.96). It should be emphasized that none of the above-mentioned imaging modalities can assess the degree of NAFLD/NASH as assessed by the histological Brunt classification [35]. Differentiating between NAFLD and NASH is important since 25-35% of patients with NASH eventually progress to liver fibrosis or even cirrhosis [36, 37]. Using serum alanine aminotransferase (ALT) levels in addition to imaging to discriminate between steatosis and NASH turns out to be disappointing. Several studies showed that a significant proportion of the patients with biopsy-proven NASH had normal ALT values, although some studies suggested that the common laboratory cut-off value for ALT was too high [38-40]. There are several risk scores-such as the NAFLD Fibrosis score-available to evaluate which patients with NAFLD are at risk for (advanced) fibrosis, but its utility still needs to be evaluated in the HIV-positive population [41]. There are currently no guidelines that recommend universal screening for NAFLD in the general population or in specific subpopulations. In contrast, the European AIDS Clinical Society (EACS) guideline recommends screening for NAFLD in HIV-infected patients with metabolic syndrome using ultrasound [42]. Since the prevalence of NAFLD among HIV-infected patients with persistent liver enzyme elevations is high, ultrasound screening should also be considered in this population.
Pathogenesis
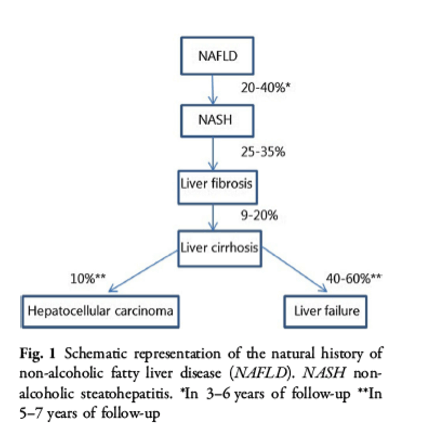
NAFLD is a clinical-histological diagnosis characterized by the presence of fat accumulation in hepatocytes resulting in necro-inflammation and hepatocyte ballooning in the absence of excessive alcohol use [43]. According to the American Association for the Study of Liver Diseases (AASLD), the threshold of 'significant alcohol consumption' is > 21 standard drinks per week on average for men and > 14 standard drinks on average in woman when evaluating patients with suspected NAFLD [44]. In general, NAFLD is considered to be the hepatic manifestation of the metabolic syndrome. The study of Mellinger et al. showed an association between presence of NAFLD and coronary artery calcium [OR 1.20 (1.10-1.30) P < 0.001][45]. This finding was confirmed in the HIV-positive population in the study of Crum-Cianflone et al., showing that high coronary artery calcification values are associated with the presence of steatosis [46]. Although the natural history of steatosis is usually benign, approximately 10% of patients with 'simple' steatosis progress to NASH. Eventually, 25-35% of the patients with NASH progress to liver fibrosis or even cirrhosis. Eventually, 10% of patients with cirrhosis develop hepatocellular carcinoma (HCC) over a period of several years [36, 37] (Fig. 1).
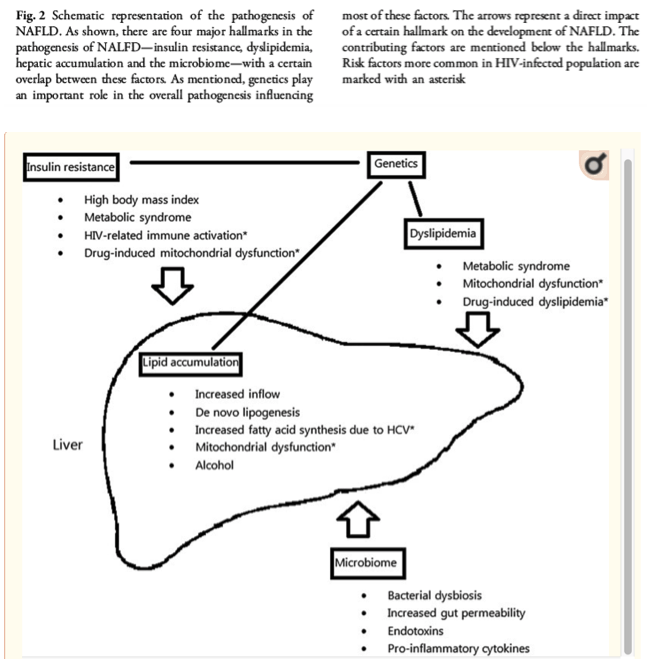
Insulin resistance (IR) is considered to be the key mechanism in the development of steatosis [47]. IR contributes to hepatic triglyceride accumulation in two ways. First, insulin normally suppresses the activity of hormone-sensitive lipase (HSL). HSL is present in all adipocytes and is able to hydrolyse stored triglycerides into free fatty acids (FFAs) [48]. In the case of IR, the suppression of HSL is diminished, resulting in an increased hydrolysis in peripheral adipose tissue and therefore an increase in delivery of FFAs to the liver [49]. In the liver, the FFAs undergo esterification into triglycerides contributing to the process of steatosis. Second, the synthesis of lipids in the liver is increased in the setting of NAFLD. Donnelly et al. showed that hepatic de novo lipogenesis (DNL) accounts for 26.1% of the hepatic triglyceride formation in NAFLD patients [50]. In contrast, the contribution of DNL in healthy individuals is less than 5% [51] (Fig. 2). Several studies in animals and humans have shown that both hyperinsulinemia and hyperglycaemia-as markers of IR-stimulate DNL by various pathways, leading to the development of steatosis [52]. The reason why steatosis progresses to NASH is still not fully elucidated. Traditionally, the two-hit theory was widely adopted [53]. In this theory, the 'first hit' is the hepatic accumulation of triglycerides-as a result of an increase in circulating free fatty acids (FFAs). The accumulation increases the susceptibility of the liver for additional hepatotoxic hits. Such an additional factor-'second hit'-eventually leads to local inflammation and NASH. Suggested contributing factors (second hit) include mitochondrial dysfunction, adipose tissue dysfunction and genetic factors. However, some authors state that the 'two-hit' hypothesis is obsolete, as it is inadequate to explain the several molecular and metabolic changes that take place in NAFLD. [47] Therefore, the current literature tends to speak of a 'multiple hit theory' that states that the pathogenesis of NASH is very complex and is the result of multiple hits and not limited to one additional hit in addition to the presence of steatosis. A third theory suggests that the accumulation of triglycerides itself provokes oxidative stress and eventually leads to inflammation and NASH [54].
|
|
| |
| |
|
|
|