 |
 |
 |
| |
AFFORDABLE CARE ACT MEDICAID EXPANSION IMPROVED LIVER TRANSPLANT WAITLIST PLACEMENT AND SLOWED RACIAL DISPARITIES
|
| |
| |
Download the PDF here
AASLD 2020 Nov 11-16
Nabeel Wahid1, Russell Rosenblatt2, Alyson Kaplan3, Catherine Lucero2, Arun B Jesudian2, Brett E. Fortune2 and Robert S. Brown Jr.2, (1)New York Presbyterian Hospital - Weill Cornell, (2)Center for Liver Disease and Transplantation, New York Presbyterian Hospital - Weill Cornell, (3)Gastroenterology and Hepatology, New York Presbyterian Hospital - Weill Cornell
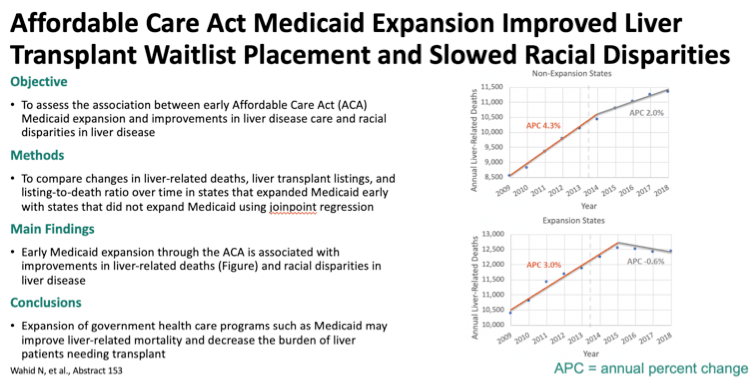
Background: The Affordable Care Act (ACA) was enacted to improve health equity in part by expanding Medicaid in participating states. We aimed to assess the impact of ACA Medicaid expansion on listings for liver transplantation (LT), end-stage liver disease (ESLD) mortality, and racial disparities.
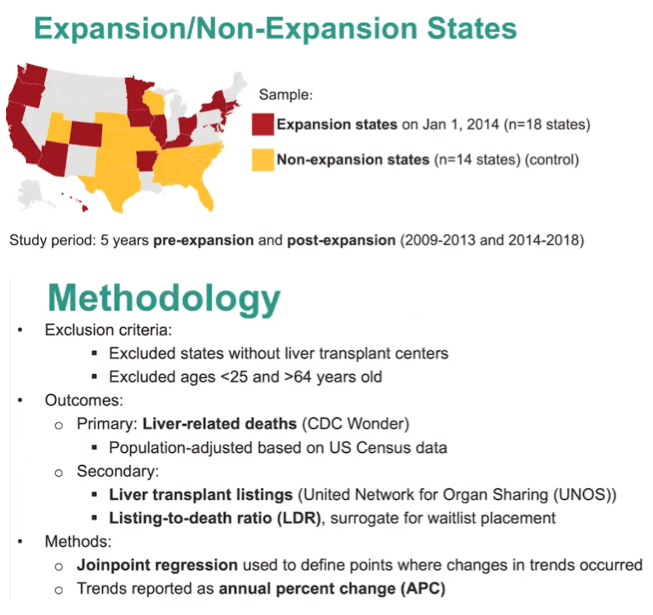
Methods: States with transplant centers that expanded Medicaid on January 1, 2014 (n=18) were compared to a control group of states that did not expand Medicaid (n=14). The pre-expansion time period (2009-2013) was compared to the post-expansion time period (2014-2018) to assess the impact of Medicaid expansion. The primary outcome was listing-to-death ratio (LDR), used as a novel quality metric for how effectively states listed patients for liver transplant compared to mortality from ESLD. Data for listing and ESLD mortality was obtained from the UNOS and CDC WONDER databases, respectively. Trends were analyzed using difference-in-differences analysis . We also analyzed year-to-year trends with joinpoint regression and annual percent change (APC) to assess if Medicaid expansion had a delayed impact. Racial impact was evaluated in subgroup analysis.
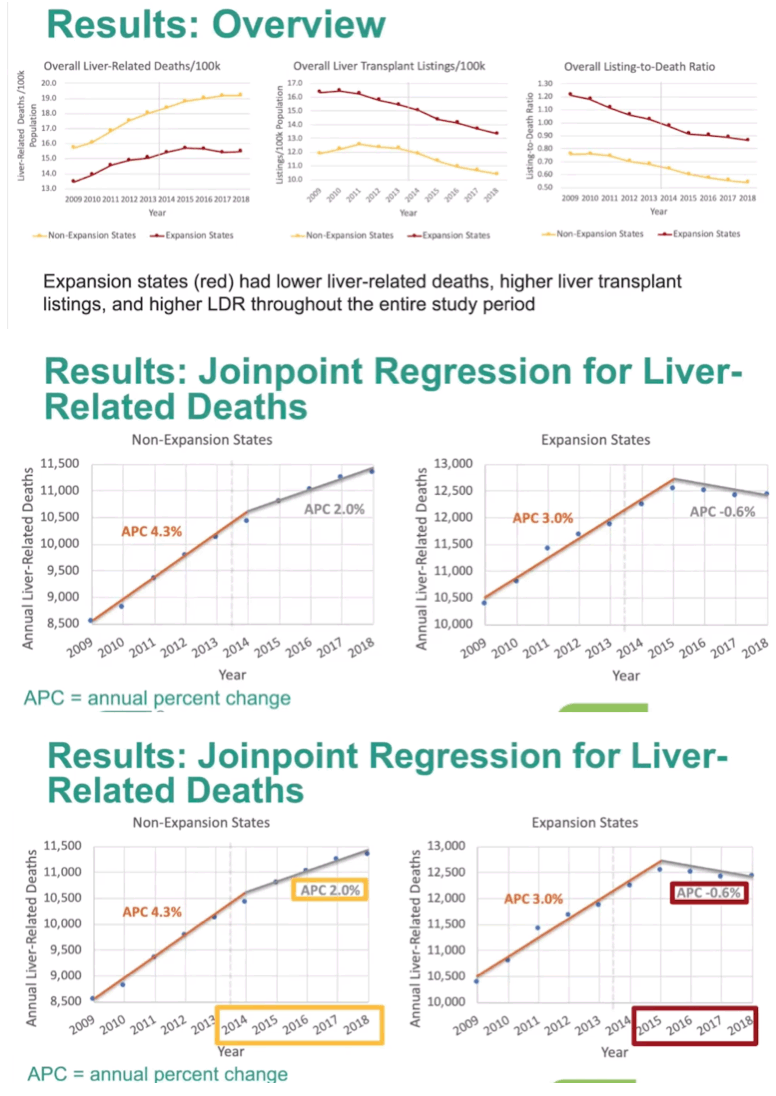
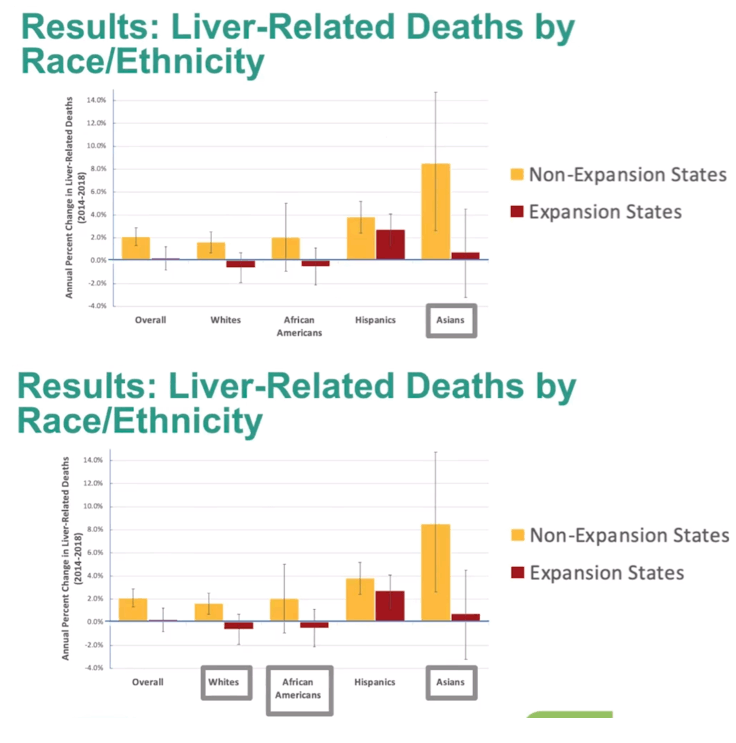
Results: LDR was significantly greater in expansion states than non-expansion states before (0.54 and 0.35, respectively) and after (0 .64 and 0 .42, respectively) Medicaid expansion (both p<0.001). However, there was no significant difference-in-difference in LDR overall (p=0 .24) or in any of the racial subgroups (p=0 .60-0 .86) . We then analyzed trends in LDR year-to-year to assess for a potential delayed impact from Medicaid expansion. While LDR for non-expansion states continued to decrease from 2011-2018 (Figure 1A), there was a breakpoint (less steep decline in LDR) for expansion states in 2015 (Figure 1B). When analyzing year-to-year by race, we found that Blacks had no significant change in LDR over the study period in expansion states (APC -0 .1, 95% CI [-1.3, 0.3]) but had a significant decrease in non-expansion states (APC -2 .1, 95% CI [-3 .1, -1 .1]). Additionally, the same breakpoint was noted for Blacks in 2015 for expansion states only.
Conclusion: As assessed by LDR, expansion states had more effective listing for LT than non-expansion states both before and after Medicaid expansion. While there was no difference-in-difference, expansion states had a breakpoint in 2015 for LDR, suggesting that Medicaid expansion did positively impact waitlist placement. However, the impact took a year to be appreciated. This is unsurprising as it often takes months to a year to identify, evaluate, and list patients for LT. Medicaid expansion also prevented worsening disparities for Blacks. Therefore, Medicaid expansion appears to have had a positive effect on listing for LT, particularly in Blacks.




|
| |
|
 |
 |
|
|