 |
 |
 |
| |
ECONOMIC BURDEN OF NASH-ASSOCIATED CIRRHOSIS: US PAYOR'S PERSPECTIVE
|
| |
| |
AASLD 2020 Nov 11-16
Reported by Jules Levin
Essy Mozaffari1, Amy Law1, Melissa Lingohr-Smith2, Amarita Randhawa1, Bryan Velez De Villa1 and Jay Lin2, (1)Intercept Pharmaceuticals, Inc., (2)Novosys Health
Background: Nonalcoholic steatohepatitis (NASH) is a chronic, progressive liver disease. Progressive advanced liver fibrosis due to NASH is associated with increasing risk of adverse clinical outcomes, such as cirrhosis. The goal of managing NASH is to prevent progression to cirrhosis and ultimately reduce liver-related complications, which incur significant clinical and economic burden. Healthcare utilization and costs among NASH patients with cirrhosis are poorly described in the literature. The objective of this study was to quantify the total economic burden among patients diagnosed with NASH, with and without cirrhosis.
Methods: The study population included adults diagnosed with NASH (ICD-10-CM code K75 .81) from a US national administrative healthcare claims database between January 2017 and March 2019. Patients were required to be enrolled in the health plan 12 months before and at least 6 months after the NASH diagnosis claim. Any individual with a claim for another chronic liver disease was excluded. Individuals with cirrhosis were identified via relevant ICD-10 codes. Descriptive statistics were used to summarize patient characteristics, healthcare resource utilization, and reimbursed amounts (reported as per-patient-per-month [PPPM] for each cohort).
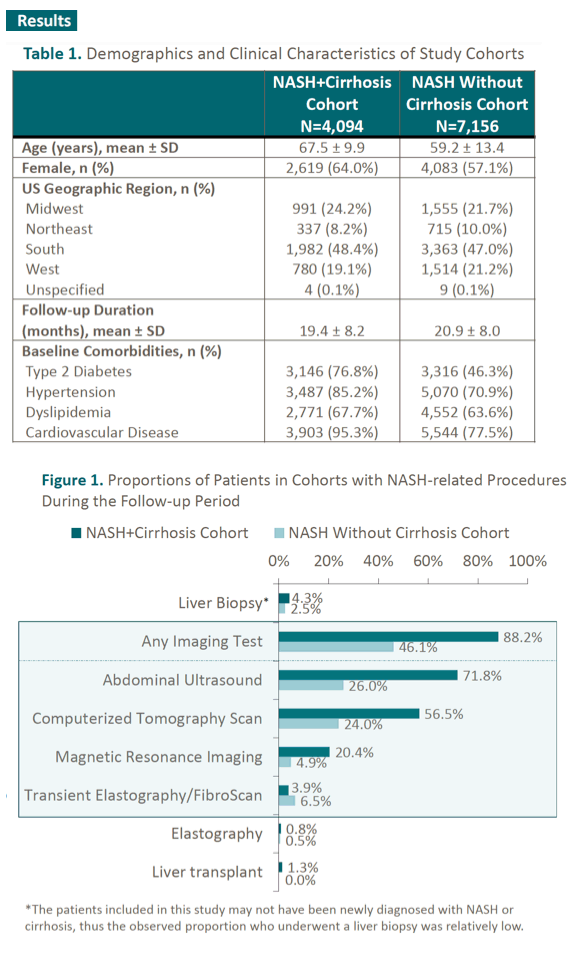
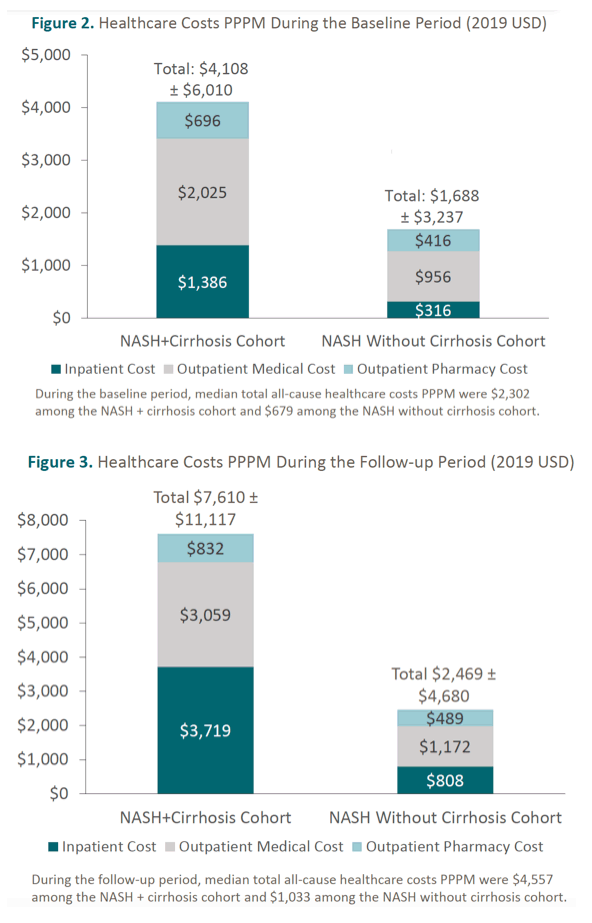
Results: We identified 4094 patients with NASH+Cirrhosis and 7156 with NASH without cirrhosis diagnoses during the study period . Patients with NASH+Cirrhosis were older (mean age: 68 vs 59 years) and included more females (64% vs 57%) (Table). Both groups were similar in geographic representation and follow-up duration post NASH diagnosis. NASH+Cirrhosis patients were more likely to have other comorbidities, such as diabetes. In the follow-up period, a greater proportion of NASH+Cirrhosis patients had imaging tests (88% vs 46%); similar proportions had liver biopsies (4.3% vs 2 .5%). Total average reimbursed amount prior to NASH diagnosis was $4108 and $1688 PPPM for NASH+Cirrhosis and NASH without cirrhosis, respectively, and the corresponding figures during the follow-up time were $7610 and $2469.
Conclusion: Patients with NASH+Cirrhosis incur substantial healthcare costs for US payors. Individuals with NASH+Cirrhosis incurred more than 3 times the healthcare costs (PPPM) to insurers than those without cirrhosis. Treatments aimed at preventing progression to cirrhosis and related sequelae are urgently needed to reduce the economic burden associated with NASH-associated cirrhosis.



|
| |
|
 |
 |
|
|