 |
 |
 |
| |
GLOBAL PREVALENCE OF HEPATITIS C VIRUS IN WOMEN
OF CHILDBEARING AGE IN 2019: A MODELING STUDY
|
| |
| |
AASLD 2020 Nov 11-16
Ellen Dugan1, Sarah Blach1, Mia Biondi2, Zongzhen Cai1, Mindi DePaola1, Chris Estes1, Jordan J. Feld3, Ivane Gamkrelidze4, Kathryn Jerabek1, Shyam Kottilil5, Siya Ma1, Poonam Mathur6, Shauna Montoya1, Devin Razavi-Shearer1, Kathryn Razavi- Shearer7, Sarah Robbins1, Jonathan Schmeltzer1 and Homie Razavi1, (1)Cda Foundation, (2)Toronto Centre for Liver Disease, Toronto General Hospital, University Health Network, (3)Toronto Centre for Liver Disease/Viral Hepatitis Care Network (VIRCAN), University Health Network, (4) Center for Disease Analysis Foundation, (5)Division of Clinical Care and Research, Institute of Human Virology, University of Maryland School of Medicine, Baltimore, MD, United States, (6)Medicine, Institute of Human Virology, (7)Analysis, Cda Foundation
Interventions that specifically target women, especially those of childbearing age are lacking; yet such efforts could prevent community spread and vertical transmission

abstract
Background: Global elimination of hepatitis C virus (HCV) is now feasible due to advancements in the understanding of disease epidemiology and highly effective treatment, however, HCV treatment during pregnancy has not proven to be safe. Interventions that specifically target women, especially those of childbearing age are lacking; yet such efforts could prevent community spread and vertical transmission. To determine the impact of such interventions, improved prevalence estimates in this cohort are needed.
Methods: A literature review was conducted to identify studies published between January 1, 2000 and June 30, 2018 reporting prevalence in women aged 15-49 years . HCV disease burden models for 110 countries inputted with country-specific data on population, mortality and HCV epidemiology were also used to calculate prevalence in women of childbearing age in 2019 . Data and forecasts from these models were then extrapolated by Global Burden of Disease (GBD) Region for the remaining 139 countries of the world that lacked data, to calculate a global estimate.
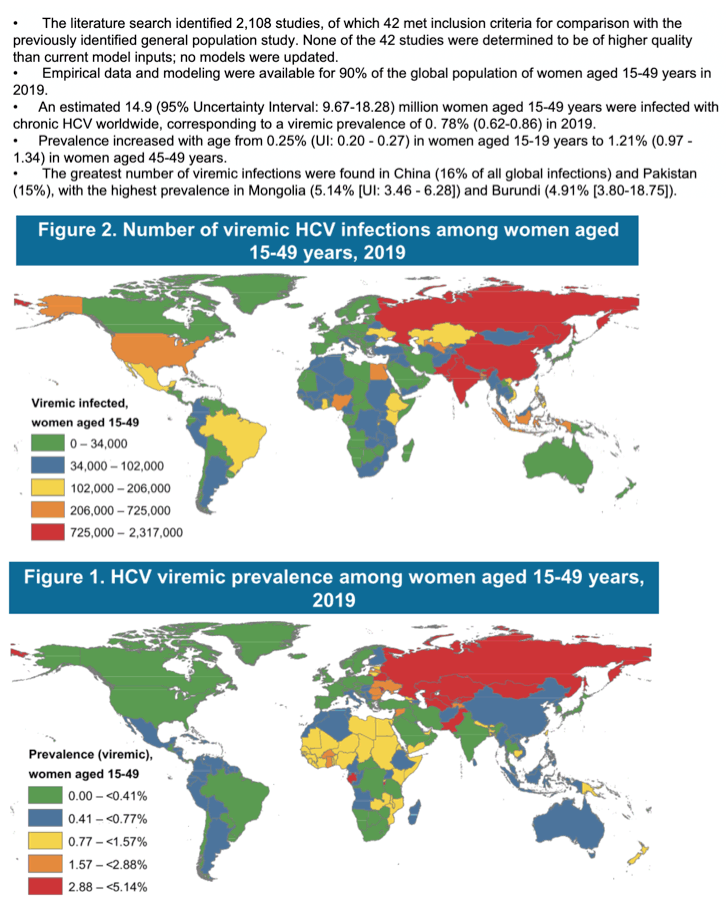
Results: Empirical data and modeling was available for 90% of the global population of women aged 15-49 years in 2019 These models informed regional estimates for the remaining 139 countries lacking available data. An estimated 14.9 (95% uncertainty interval [UI]: 9 .67-18 .28) million women aged 15- 49 years of age were infected with chronic HCV worldwide, corresponding to a viremic prevalence of 0.78% (0 .62-0 .86) in 2019.
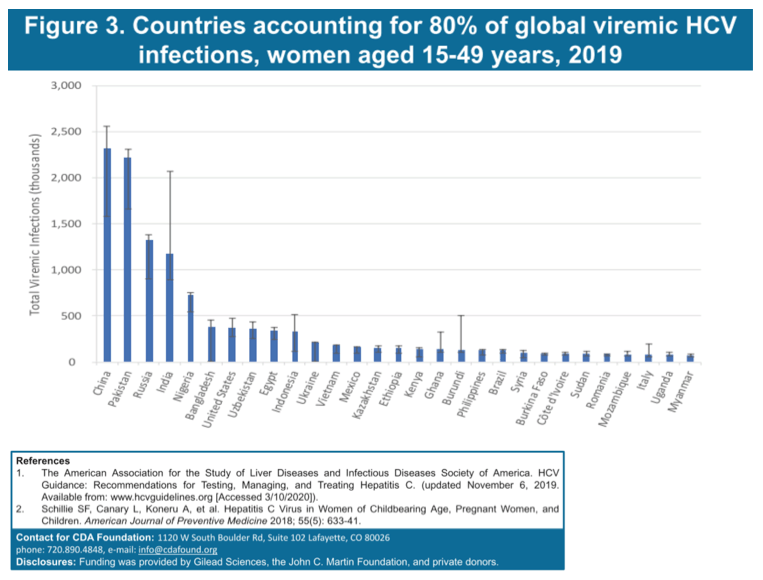
Prevalence increased with age from 0.25% (UI:0 .20 - 0 .27) in women aged 15-19 years to 1.21% (0 .97 - 1 .34) in women aged 45-49 years. The greatest number of prevalent infections were found in China (16%) and Pakistan (15%), with the highest prevalence in Mongolia (5 .14% [UI: 3 .46 - 6 .28]) and Burundi (4 .91% [3 .80-18 .78]). The lowest HCV prevalence was found in high income countries, estimated to be 0.37% (UI:0 .24-0 .53) among women of childbearing age. Among the GBD regions, eastern Europe and central Asia had the highest prevalence estimates at 3.39% (UI:1 .88 - 3 .54) and 3.25% (2.31 - 3.72).
Conclusion: This is the first global HCV prevalence estimate in women of childbearing age . These data shed light on the need for governments, global health agencies and advocacy groups to formulate improved preconception test-and-treat strategies which could reduce vertical transmission and total disease burden among women of childbearing age and their children.

|
| |
|
 |
 |
|
|