 |
 |
 |
| |
A Study of Neurocognitive Performance
in Women Living With and Without HIV in South Africa
|
| |
| |
Aging & HIV Workshop 2020 Sept 29-Oct 2 virtual
Reported by Jules Levin

Cassim H1, Buckley J1, Otwombe K1, Joyce C1, Nyati M1, Galvin L1, Hlongwane K1, Yende-Zuma N2, Aizire J3, Brummel S5, Taha T3, Fowler M4, Violari A1
1Perinatal HIV Research Unit, University of the Witwatersrand, Johannebsurg, South Africa, 2Centre for the AIDS Programme of Research in South Africa (CAPRISA), University of KwaZulu Natal, Durban, South Africa, 3Johns Hopkins Bloomberg School of Public Health, Johns Hopkins University, Baltimore, USA, 4Johns Hopkins School of Medicine, Johns Hopkins University, Baltimore, USA, 5Harvard T. H. Chan School of Public Health, Harvard University, Boston, USA

ABSTRACT
Background: HIV is thought to cause accelerated as well as accentuated aging in several organs. Neurocognitive data from people living with HIV and receiving antiretroviral therapy (ART) and their relationship to their HIV negative counterparts are lacking. We investigated the relationship between HIV status and neurocognitive (NC) functioning in women living with HIV (WLHIV) and those without.
Materials and Methods: In this cross-sectional study conducted between 08 July 2018 and 02 December 2019, WLHIV were sourced from the PROMOTE cohort study at the Soweto site; the majority had been on ART for at least 5 years. For comparison, HIV-uninfected (HIV-) women of similar age were recruited. In-depth neuropsychological testing in domains affected by HAND were administered. Tests included Verbal Learning and Memory, Visual Learning and Memory, Motor Speed, Executive Function, Language and Information Processing. Depression, alcohol use and functional impairment were also assessed. Mild Neurocognitive Disorder (NCD) was defined as 2 standard deviations (SD) below the mean in one or more domains. Major NCD was defined to include both functional and NC impairment (Diagnostic and Statistical Manual 5 criteria). Categorical data were compared between the two groups with the chi-square test and continuous variables were summarized using medians and interquartile ranges (IQR). Relative risks (RR) of NCD comparing levels were estimated using the log-binomial regression adjusting for demographic and clinical factors.
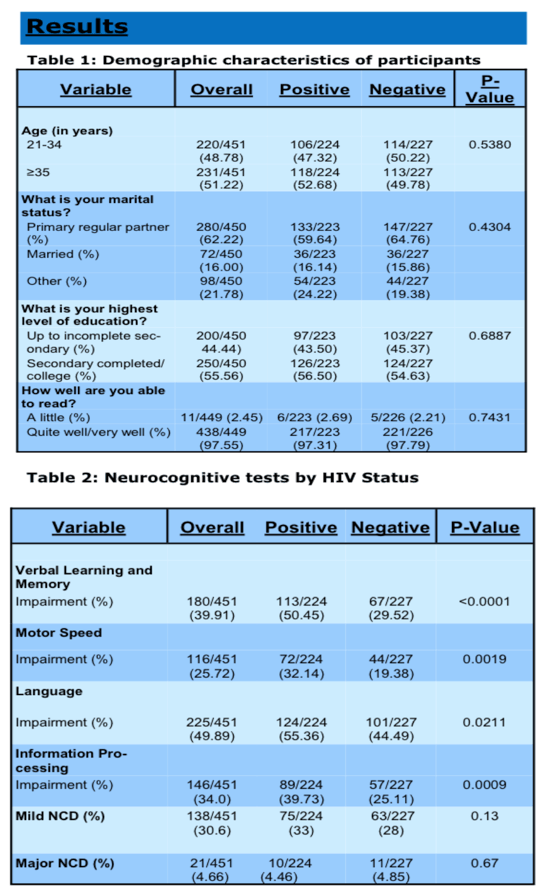
Results: Median age of 227 WLHIV and 245 HIV- women was 35 (IQR:31-39) and 34 (IQR:31-39) years respectively; 97% (219/226) of WLHIV were virally suppressed (VL < 400 copies/ml) and 95% (215/226) were on fixed dose combination of EFV/FTC/TDF. There was no difference in rates of depression and alcohol use by HIV status. WLHIV compared to HIV- had higher impairment in some domains: verbal learning and memory (40% [113/224] vs. 23% [67/227]; p<0.001), motor speed (32% [72/224] vs. 19% [44/227]; p=0.002), language (55% [124/224] vs. 44% [101/227]; p=0.002) and information processing (40% [89/224] vs. 25% [57/227]; p=0.0009). Mild NCD was identified in 33% (75/224) of WLHIV vs. 28% (63/227) in HIV- (p=0.13) while Major NCD was seen in 4% (10/224) and 5% (11/227) respectively (p=0.67). In multivariable analysis, HIV status and level of education were not associated with NCD; Being 35 years or older relative to 21-34 years (RR: 1.69, 95%CI: 1.27-2.26) and ability to read a little compared to reading quite well or very well (RR: 1.64, 95%CI: 1.13-2.38) was associated with NCD.
Conclusions: This is one of few studies in Africa to focus on NC functioning using full Neuropsychological testing in women who initiated ART before severe immunosuppression. WLHIV had significantly higher impairment in specific domains compared to HIV-; despite that the number of those diagnosed with mild or major NCD was similar between the groups. Additionally, older women ≥ 35 years and those with lower ability to read had a higher frequency for NCD irrespective of HIV status. This remains an important clinical concern as it could worsen with age and could have important implications for functioning, parenting and ART adherence.

----------------------------------------
What Is Cognitive Impairment?
Cognitive (or memory and thinking) skills are needed for just about everything a person does, including:
• Focusing
• Remembering things
• Solving problems
Cognitive disorders in people living with HIV
Lancet HIV July 2020, Alan Winston, Serena Spudich
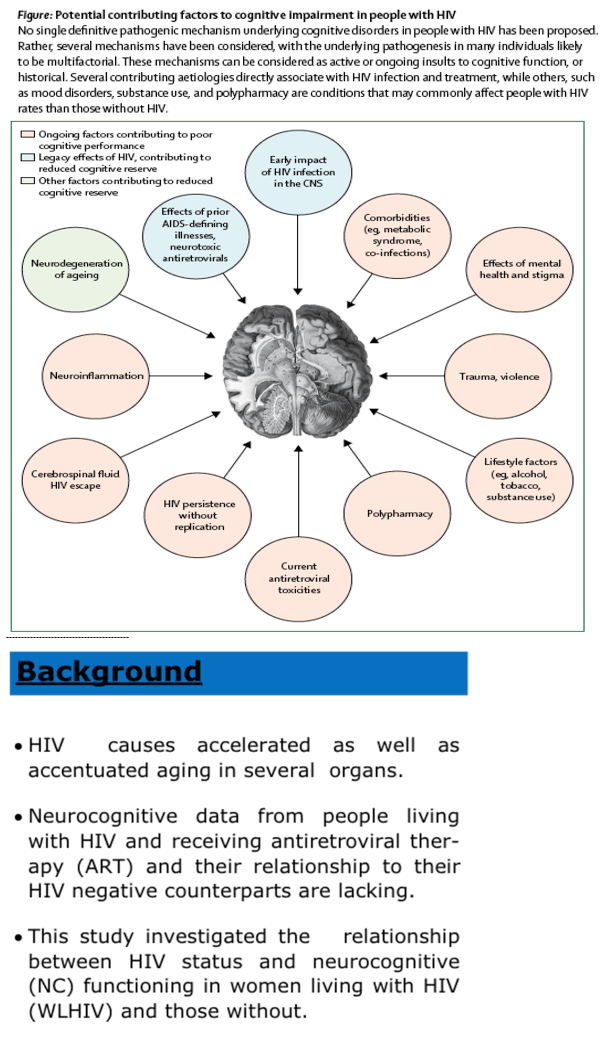
Pathogenesis and contributing factors:
Legacy effects from HIV and its complications, Neuroinflammation, Antiretroviral toxicities, Ageing and comorbidities, Lifestyle factors, Cerebrospinal fluid HIV RNA escape and HIV persistence
Potential causes of cognitive impairment in effectively-treated people with HIV are described, highlighting the contribution of HIV-related factors as well as lifestyle factors.
Legacy effects from HIV and its complications
Advances in HIV management over the past 20 years have been unprecedented. Prior to these advances, people with HIV experienced many conditions which may have had long-term effects on brain health, such as clinically evident AIDS-defining CNS infections and cancers, and toxicities from the initial generations of antiretroviral drugs. Additionally, processes associated with cognitive disorders in HIV, including neuroinflammation, brain atrophy, and injury to neurons, as detected via the cerebrospinal fluid and neuroimaging, can be initiated and progressively worsen during early untreated HIV infection. While these processes appear to be attenuated once ART is started and viral suppression is achieved, the lengthy duration of HIV infection in many people with HIV prior to initiation of therapy might lead to a subtle but lasting neural dysfunction. Although these legacies are not ongoing or necessarily progressive during modern stable treatment regimens, the resultant detrimental effects on cognitive reserve, which does not recover, may be apparent several decades later. For individuals who have experienced these so-called legacy effects and therefore have a reduced cognitive reserve, current insults to the CNS, including natural changes with ageing, might have a greater impact (figure).
As outlined previously, people with HIV frequently have concurrent medical conditions and lifestyle factors that can affect overall cognitive function. Medical conditions that can affect cognitive function include depression, anxiety and other mental health illnesses, liver disease, and cardiovascular disease.
The treatments for these medical conditions, which might include psychoactive medications that impact cognition, are also potential factors in cognitive impairment in this population. Lifestyle factors that can affect cognition include excessive alcohol intake, the use of recreational drugs, and tobacco smoking.
Questions also remain regarding the high rates of cognitive impairment observed in cohort studies that have used the HAND criteria. Rates of cognitive impairment of up to 50% are widely reported when the HAND criteria are applied. The relevance of this finding can therefore be questioned, given that such high rates of cognitive impairment are generally not apparent in clinical practice.
Furthermore, in HIV-negative control populations, the HAND criteria classify a high percentage of individuals as having a cognitive disorder, which clearly cannot be related to HIV, given that the controls are HIV-negative. In addition, heterogeneity is likely to exist in cognitive profiles across different populations and cultures. As with many criteria for defining cognitive disorders, the HAND criteria do not differentiate individuals on the basis of specific cognitive domain types that are deemed to be impaired, but rather the total number of cognitive domains deemed impaired.
-----------------------------------------


|
| |
|
 |
 |
|
|