| |
High rates of 30-day mortality in patients with cirrhosis and COVID-19
|
| |
| |
Download the PDF here
JNL of Hepatology June 8 2020 - Massimo Iavarone, MD PhD, Roberta D’Ambrosio, MD, Alessandro Soria, MD, Michela Triolo, MD, Nicola Pugliese, MD, Paolo Del Poggio, MD, Giovanni Perricone, MD, Sara Massironi, MD, Angiola Spinetti, MD, Elisabetta Buscarini, MD, Mauro Viganò, MD PhD, Canio Carriero, MD, Stefano Fagiuoli, MD, Alessio Aghemo, MD, Luca S. Belli, MD, Martina Lucà, MD, Marianna Pedaci, MD, Alessandro Rimondi,
MD, Maria Grazia Rumi, MD, Pietro Invernizzi, MD, Paolo Bonfanti, MD, Pietro Lampertico, MD PhD
Highlights
• Fifty cirrhotic patients with SARS-CoV-2 infection were studied: 64% presented with fever, 42% shortness of breath/polypnea, 22% encephalopathy; respiratory-support was necessary in 71%.
• The 30-day mortality was 34% (95% CI 23-49), higher in those patients with moderate/severe respiratory failure and in those who had a more deteriorated liver function, as indicated by the increased MELD and CLIF-OF scores at COVID-19 diagnosis.
• The 30-days mortality rate was higher in cirrhotics with COVID-19 than in cirrhotics with bacterial infection and in COVID-19 patients without cirrhosis
• No major adverse events related to the thromboprophylaxis with heparin given to 80% of patients and treatments used to tackle the coronavirus infection.
This case series clearly demonstrates the poor outcome of cirrhotic patients (either with compensated or decompensated liver disease) who develop COVID-19. The main causes of death were respiratory complications but also the sudden worsening of liver function leading to end-stage liver disease. To the best of our knowledge, this is the first report on the clinical impact of SARS-CoV-2 infection in patients with cirrhosis.
Abstract
Background and aims
Coronavirus disease (COVID-19) is a major worldwide threat for healthy individuals as well as for patients with comorbidities, but its impact on patients with cirrhosis is currently unknown. This study aimed at evaluating the impact of COVID-19 on the clinical outcome of these patients.
Methods
In this multicenter retrospective study, cirrhotic patients with confirmed Severe Acute Respiratory Syndrome Coronavirus-2 (SARS-CoV-2) infection were enrolled between 1st and 31th March 2020. Clinical and biochemical data at COVID-19 and at the last outpatient visit were obtained through review of medical records.
Study Population
We included cirrhotic patients with laboratory-confirmed SARS-CoV-2 infection who were managed in nine hospitals in Lombardy, Northern Italy, between March 1st and March 31th, 2020. Therefore, all information registered by 3 April 2020 (data-lock) were entered into the database.
A confirmed case of SARS-CoV-2 was defined by a positive result on a reverse-transcriptase–polymerase-chain-reaction (RT-PCR) assay of a specimen collected on a nasopharyngeal swab, as previously described.5
Demographic and clinical data, including clinical symptoms or signs at presentation, laboratory and radiologic results during COVID-19 management as well as administered antiviral therapies and anti-thrombotic prophylaxis, were collected. All laboratory tests and radiologic assessments were performed at treating physician discretion. Data of the last outpatient clinic visit before COVID-19 were also collected for comparison. When SARS-CoV-2 infection occurred during hospitalization, data of COVID-19 diagnosis were compared to those collected at hospital admission.
The Steering Committee for the COVID-19 studies at Foundation IRCCS Ca’ Granda Ospedale Maggiore Policlinico approved the study, which was notified to the Ethical Committee of Milan Area 2. The protocol complies with the ethical guidelines of the 1975 Declaration of Helsinki.
Results
Fifty cirrhotic patients with confirmed SARS-CoV-2 infection were enrolled (age 67 years, 70% men, 38% virus-related, 52% previously compensated cirrhosis). At diagnosis, 64% of patients presented fever, 42% shortness of breath/polypnea, 22% encephalopathy, 96% needed hospitalization or prolonged an ongoing one. Respiratory-support was necessary in 71%, 52% received antivirals, 80% heparin. Serum albumin significantly decreased, while bilirubin, creatinine and prothrombin time significantly increased at COVID-19 diagnosis compared to last available data. The proportion of patients with MELD≥15 increased from 13% to 26% (p=0.037), acute-on-chronic liver failure and and de novo acute liver injury occurred in 14 (28%) and 10 patients, respectively.
Seventeen patients died after a median of 10 (4-13) days from COVID-19 diagnosis, with a 30-day-mortality rate of 34%. Severity of lung and liver (according to CLIF-C, CLIF-OF and MELD scores) diseases independently predicted mortality. Mortality was significantly higher in hospitalized cirrhotics with COVID-19 than in those hospitalized for bacterial infections.
Conclusion
COVID-19 is associated with liver function deterioration and elevated mortality in cirrhotic patients.
*All HCV patients achieved an SVR and all HBV patients were on effective nucleotide analogue (NA)-therapy; **11 autoimmune hepatitis and 8 NASH in the SARS-CoV-2 negative cohort; ***active or past.
During the study period, 399 patients without cirrhosis required hospitalization at the Foundation IRCCS Cà Granda Ospedale Maggiore Policlinico (Milan), following COVID-19 diagnosis: median age was 62 (51-76) years, 256 (64%) were males. Eithy-one (20%) of these patients died [median age at death 80 (75-86) years]. Thirty-day mortality was lower in non cirrhotics than in cirrhotics with COVID-19 [18% (95%CI 15-22) vs. 34% (95%CI 23-49), p=0.035].
The demographic and clinical characteristics of the patients are reported in Table 1. Age was 67 (61-74) years, 70% were men, 28% with HCV-related and 10% with HBV-related cirrhosis; all patients with virus-related cirrhosis were either HCV-RNA negative after anti-HCV treatment or on long-term anti-HBV treatment. Among our patients, there were only 3 with metabolic (i.e. NAFLD/NASH) aetiology. Diabetes was present in 18 (36%) and arterial hypertension in 29 (58%) patients. Twenty-six (52%) patients had compensated cirrhosis (CPT-A) at the time of their last outpatient visit. Seven (14%) were on waiting list for liver transplantation (LT). Time from last outpatient visit was 1.7 (1.0-4.0) months. SARS-CoV-2 infection was community acquired in 30 (60%) patients and health-care related in the remaining 20 (40%). In fact, 10 (50%) patients reported a history of recent (less than 7 days) hospitalization or admission to hospital services, whilst the other 10 (50%) probably got infected during current hospitalization.
COVID-19 outcome
Thirty-two (64%) patients needed non-invasive respiratory support during hospitalization, while two patients were admitted to ICU and received invasive mechanical ventilation (Table 2). In detail, an acute respiratory distress syndrome was present in 26 (52%) patients: mild (200 mmHg < PaO2/FiO2 ≤ 300 mmHg) in 12, moderate (100 mmHg < PaO2/FiO2 ≤ 200 mmHg) in 11 and severe (PaO2/FiO2 < 100 mmHg) in 3 patients. Moreover, 4 (8%) patients experienced hypotension and needed vasopressors.
Overall, 26 (52%) patients received specific anti-SARS-CoV-2 treatment: 9 (18%) received hydroxychloroquine alone, 3 (6%) received antiviral therapy with lopinavir–ritonavir, and 14 (28%) received both anti-viral treatment and hydroxychloroquine; none of the patients have been treated with tocilizumab or remdesivir. Only mild gastrointestinal adverse events were reported in patients treated with hydroxychloroquine, whilst one patient showed a mild increase in ALT values. In one case, treated with hydroxychloroquine plus lopinavir–ritonavir, a prolongation of electrocardiographic QT interval occurred, leading to treatment discontinuation, however without sequelae.
Thromboprophylaxis with heparin (mainly with low molecular weight heparin, LMWH) was started at COVID-19 diagnosis in 80% of patients, with two minor haemorrhagic events (epistaxis and haematuria). Progression of pre-existing portal thrombosis was ascertained in one patient, despite LMWH use. Patients in thromboprophylaxis vs. those untreated were comparable in terms of INR [1.23 (1.09-1.55) vs 1.45 (1.21-1.54), p=0.97] and platelet count [132,000 (85,000-183,000) vs 89,000 (34,500-136,000) per microliter, p=0.064], more frequently had well-compensated cirrhosis (CPT A in 51% vs 18%, p=0.05), and less frequently oesophageal varices (42% vs 81%, p=0.023).
At data lock (April, 30), among the 48 hospitalized patients, 17 (35%) died during hospital stay, 24 (50%) were discharged home after recovery [median stay length 15 (10-23) days], and 7 (15%) were still hospitalized [median stay length at data-lock 15 (9-33) days].
COVID-19 impact on cirrhosis
When compared to the last outpatient visit [median time-lapse 1.7 (1.0-4.0) months], or to blood tests performed at admission, but before SARS-CoV-2 infection, most parameters had changed at the time of COVID-19 diagnosis. Bilirubin, INR, ALT and creatinine (p=0.007) significantly increased (p=0.026, p=0.042, and p=0.024, respectively), whilst albumin levels significantly decreased (p=0.0003), thus influencing both CPT and MELD scores (Table 3). The distribution of CPT scores significantly changed (p=0.05, Table 3), the number of patients with MELD ≥15 increased from 5 to 13 (13% vs 26%, p=0.037) and 12 out of 26 (46%) patients decompensated. No upper-gastrointestinal bleeding episodes occurred, despite the wide use of anti-thrombosis prophylaxis. ACLF at COVID-19 was diagnosed in 14 (28%) patients: Ia in 3, Ib in 5, II in 5 and III in 1.
Overall and disease specific mortality
Seventeen (34%) patients died after a median of 10 (4-13) days from diagnosis of SARS-CoV-2 infection, and their median age was 70 (61-80) years. COVID-19 with respiratory failure was considered the cause of death in 12 (71%) patients, while end-stage-liver disease (ESLD) accounted for death in 5 (29%). Nevertheless, all patients dying for ESLD required respiratory support for concomitant hypoxemic respiratory failure. Three (18%) of the 17 patients who died were on the LT waiting-list.
The 30-day cumulative probability of overall mortality was 34% [95% Confidence Interval (CI) 23-49] (Figure 1A). The corresponding features for COVID-19- and liver-related mortality were 25% (95% CI 15-40) and 12% (95% CI 5-26), respectively (Figure 1B). Predictors of mortality are reported in Table 4. In the multivariate analysis, only CLIF-OF (HR 1.426, 95%CI 1.122-1.668, p≤0.0001) and moderate/severe lung failure (HR 1.608, 95%CI 1.079-2.395, p=0.019) independently predicted mortality. When CLIF-C was introduced, MELD, CLIF-C and moderate/severe respiratory failure remained as independent predictors. MELD and CLIF independently predicted mortality also when analysed as dichotomous variables. Figure 2a and 2b show the cumulative probability of mortality according to MELD≥15 and CLIF-OF>9 at diagnosis. MELD≥15 at development of SARS-CoV-2 infection occurred in 2/33 (6%), 5/10 (50%) and 6/7 (86%) of patients with MELD scores of 6, 7-11 and >11 at last record before SARS-CoV-2 infection, respectively (p<0.0001).
Comparative analysis
Table 5 shows the comparison between the main cohort (i.e. 48 cirrhotics hospitalized with COVID-19) and 47 cirrhotics hospitalized for acute liver decompensation due to bacterial infection, which served as controls. In the control group, bacterial pneumonia was diagnosed in 18 (38%) patients, spontaneous bacteraemia in 14 (30%), cholangitis in 5 (11%), urinary tract infection in 4 (9%), spontaneous bacterial peritonitis in 4 (9%) patients, arthritis in one (2%) and gastroenteritis due to Clostridioides difficile in one (2%). Patients with COVID-19 were significantly older, with lower white blood cells counts despite concomitant infection, and lower MELD and CPT B/C scores. However, ACLF prevalence was similar (Table 5). The 30-day cumulative probability of overall mortality was 17% (95%CI 8-32) vs 34% (95%CI 23-49; p=0.03). At multivariate analysis, COVID-19 (HR 3.594, 95%CI 1.465-8.819, p=0.005) and CLIF-OF (HR 1.369, 95%CI 1.219-1.539, p≤0.0001) independently predicted mortality.
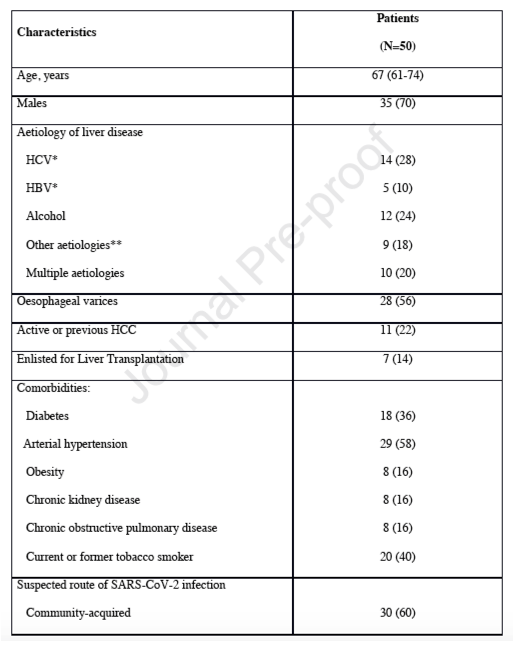
*All HCV patients achieved a sustained virological response (SVR) and all HBV patients were on effective nucleotide analogue (NA)-therapy. **Other aetiologies: autoimmune hepatitis/cholangitis (n=3); non-alcoholic steatohepatitis (n=3); erythropoietic protoporphyria (n=1); unknown (n=2). HCV: hepatitis C virus; HBV: hepatitis B virus; HCC: Hepatocellular Carcinoma; SARS-CoV-2: Severe Acute Respiratory Syndrome Coronavirus-2.
At SARS-CoV-2 diagnosis, 44 (88%) patients presented at least one symptom: 18 (36%) presented with cough, 21 (42%) with polypnea or shortness of breath, 32 (64%) with fever and 11 (22%) with acute hepatic encephalopathy (Table 2). Six (12%) patients were asymptomatic at presentation: in these cases, nasopharyngeal swab was performed according to surveillance protocols (i.e. contact with positive subjects).
Discussion
This case series clearly demonstrates the poor outcome of cirrhotic patients (either with compensated or decompensated liver disease) who develop COVID-19. The main causes of death were respiratory complications but also the sudden worsening of liver function leading to end-stage liver disease. To the best of our knowledge, this is the first report on the clinical impact of SARS-CoV-2 infection in patients with cirrhosis.
We retrospectively collected data on 50 patients with known cirrhosis and COVID-19 managed in nine hospitals in Lombardy. Interestingly, a health-care related SARS-CoV-2 infection was registered in 40% of our patients. This fact could be the consequence of their general increased need of hospitalization and assistance due to cirrhosis complications, as well as their increased susceptibility to infections. According to the Italian ISS report, the nosocomial SARS-CoV-2 infection rate was 9.9% in Italy, which is lower than what we observed in our cohort. Moreover, the clinical presentation of SARS-CoV-2 infection in our cohort of cirrhotics slightly differed from what reported in the general population. Indeed, fever was less frequent,
16
whilst an expected increase in cirrhosis complications rate was observed, particularly hepatic encephalopathy. In our study, the 30-days mortality rate was higher in those patients with moderate/severe respiratory failure and in those who had a more deteriorated liver function, as indicated by the increased MELD and CLIF-OF scores at COVID-19 diagnosis. While the association between severity of lung failure and early mortality was expected, this study is the first to define the predictive role of CLIF and MELD scores in the setting of acute failure of chronic liver disease due to COVID-19.
The corresponding 30-day mortality rate in non-cirrhotic patients hospitalized following COVID-19 diagnosis was significantly lower, with higher median age of deceased patients. Unfortunately, no data are available on the role of factors (i.e. co-morbidities, lung failure severity, etc) potentially influencing mortality rates in this control group, as the ICD-9 system has been used for data collection. In the same period, 7,600 (16%) of 46,071 patients with SARS-CoV-2 infection died in Lombardy, with a median age of 79 years (73-87). These data significantly differ from what reported in our cirrhotic cohort, characterized by a higher mortality rate and lower age at death.
Moreover, our study highlighted that infection with SARS-CoV-2 led to rapid clinical deterioration in otherwise stable cirrhotic patients: 25 CPT A patients with low MELD score experienced a rapid deterioration in their liver function, so that CPT score increased to B/C after COVID-19 diagnosis in more than a third of them. This was even worst for those patients with a decompensated disease before SARS-CoV-2 infection, since we reported that high MELD scores at last visit independently predicted the risk of MELD≥15 at COVID-19 diagnosis. The short interval between the last outpatient visit (or hospital admission) before SARS-CoV-2 diagnosis, supports the role of this acute infection in worsening liver function, which is common in cirrhotic patients of any aetiology. The comparative analysis with cirrhotic patients hospitalized for decompensation due to bacterial infections, confirmed that mortality rate due to infections is high, independently of the etiological agent. However, the 30-day mortality for COVID-19 cirrhotics was higher than that reported among cirrhotics hospitalized following bacterial infections, although MELD score was lower in the former group. Multivariate analysis confirmed that COVID-19, together with high CLIF-OF, was independently associated with 30-day mortality. This is probably due to several factors, which include the unavailability of effective treatments against SARS-CoV-2 as well as the impact of lung failure on early mortality even in patients who died because of ESLD. In fact, also in cirrhotic patients who died for ESLD, respiratory function had been severely compromised by SARS-CoV-2, since all of them needed respiratory support.
Several papers reported the impact of SARS-CoV-2 infection on transaminases levels in the general population, although they were not specifically focused on the clinical significance of these alterations in terms of both morbidity and mortality, especially in cirrhotic patients. 18
In the setting of chronic liver diseases, persistent and/or severe alteration of transaminases may negatively impact cirrhosis course, also in those patients who had remained stable and free from liver-complications for long time. Recently, Dong et al reported a 50% ALT increase in 202 consecutive patients with confirmed COVID-19, which included 38% with non-alcoholic fatty liver disease (NAFLD). Interestingly, the authors reported that NAFLD patients had higher likelihood of abnormal liver function tests from admission to discharge [70% (53/76) vs 11.1% (14/126) p<0.0001]. 18
Our study is the first reporting the impact of SARS-CoV-2 infection on ALT levels in patients with cirrhosis, showing that acute liver injury was observed in nearly a half of patients with previously normal transaminases values. Moreover, a hepatitis flare was not uncommon at SARS-CoV-2 diagnosis. However, more data are needed to clarify the impact of ALT increase in the natural history of cirrhotic patients with SARS-CoV-2, and to better explain the pathogenic mechanism of coronavirus in causing liver damage at the level of liver cells. A potential direct cytopathic effect has been suggested, since the abundant ACE2 receptors in the liver might favour SARS-CoV-2 entry into the hepatocytes. 19
Otherwise, the liver might be indirectly involved in the severe inflammatory response following SARS-CoV-2 infection, as it contains a large number of macrophages (Kupffer cells) and is a potent cytokine producer. 20
Specific treatment against SARS-CoV-2 was not standardized in our cohort, but rather based upon regional guidelines issued by scientific societies and expert opinions. Single physician’s decision on every patient was the balance between rapidly available repurposed drugs and acceptable tolerability and safety. Most of the patients received hydroxychloroquine, while only one third received lopinavir/ritonavir. With all the caveats of a small sample size, only one major adverse event was reported (QT prolongation leading to drug discontinuation). Generally, lopinavir/ritonavir has been used cautiously in patients with more advanced cirrhosis, due to its known hepatic metabolism and its possible detrimental effect on residual hepatic function. At the time of data collection, a phase II trial with tocilizumab was available only in few referral centers, thus excluding the chance to enrol patients with cirrhosis. In the period before data-lock, access to remdesivir was reserved to mechanically ventilated patients on the basis of a treating physician-initiated request in a compassionate use program. The two intubated patients of our cohort did not receive remdesivir. The reason for not applying for compassionate use in these two cases are unknown but could be due to the difficult access in programs of experimental drugs in the dramatic hospital emergency we faced in March 2020 in Lombardy.
Interestingly, most patients (80%) in our cohort received thromboprophylaxis, mainly with LMWH, without any evidence of major haemorrhagic complications. The high prevalence of thromboprophylaxis in our cohort might be explained by the established awareness of the increased thrombotic risk in this population, as well as by the ascertained skill in anti-thrombotic management in most centers dealing with cirrhotic patients.
We are aware that our study suffers from some limitations, mainly due to the retrospective design of the study. They include the limited number of patients, the short follow-up following the diagnosis of SARS-CoV-2 infection and the low number of patients admitted in ICUs. However, we believe that this last point might be not only a consequence of the retrospective collection of data but also of the effective limited access to ICUs of patients with severe comorbidities, such as cirrhotics. In fact, during the study period, we faced with a dramatic scarcity of bed in ICUs trying to cope with the awesome outbreak of SARS-CoV-2 infection and COVID-19 in Italy. Another limitation is the imbalance of baseline characteristics (age and MELD) between patients with viral and bacterial infection, although multivariate analysis confirmed SARS-CoV-2 infection as an independent predictor of 30-day mortality. On the other hand, strengths of our study are the involvement of most tertiary referral Centers for both infectious and liver diseases in Lombardy, thus limiting the risk of underestimating the number of hospitalized cirrhotics within our Region.as well as the availability of “historical” information for almost all patients, The inclusion of control groups of well characterized hospitalized patients with cirrhosis and acute decompensation following bacterial infection and without cirrhosis but with COVID-19, further strengthens the present study.
In conclusion, as the current pandemic of SARS-CoV-2 is spreading, physicians and hepatologists should be aware of the potential detrimental effects of this infection on the short-term outcome of such a fragile patient population as cirrhotics.
|
|
| |
| |
|
|
|