 |
 |
 |
| |
ASSESSMENT OF IMMEDIATE INITIATION OF ANTIRETROVIAL THERAPY IN NYC
|
| |
| |
Download the PDF here
CROI 2020 March 8-11
Reported by Jules Levin
Daniel F. Bertolino1, Erica D’Aquila1, Nadia Nguyen2, Denis Nash3, Abigail Baim-Lance3, Bisrat Abraham1,4
1New York City Department of Health and Mental Hygiene, New York City, USA, 2HIV Center for Clinical & Behavioral Studies, New York State Psychiatric Institute and Columbia University, New York City, USA,
3City University of New York Institute for Implementation Science in Population Health, New York City, USA, 4Weill Cornell Medicine, Division of Infectious Diseases, New York City, USA

program abstract
Background: Rapid or immediate initiation of antiretroviral therapy (iART) after a positive HIV test has been shown to decrease time to viral suppression (VS), in turn reducing transmission of HIV. New York City (NYC) and New York State (NYS) have expanded access to iART for people living with HIV (PLWH) through targeted programs at clinics in NYC. We evaluated iART knowledge, attitudes, and practices among clinical and non-clinical staff in NYC clinics, as well as barriers and facilitators to iART implementation.
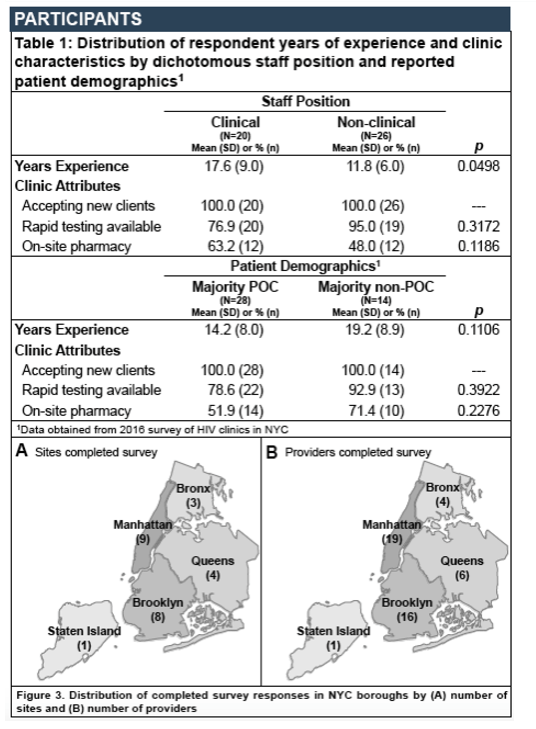
Methods: We recruited at least one clinical (i.e., medical provider) and one non-clinical (i.e., administrator or social service provider) staff member to complete an online survey from a purposive sample of 30 NYC clinics providing primary care to one or more PLWH. Clinics were selected to ensure a diverse representation of health outcomes (e.g., clinic VS), clinic resources (e.g., iART funding) and clinic location and type (e.g., borough, hospital-based clinic). Descriptive and bivariate analyses were performed on collected data.
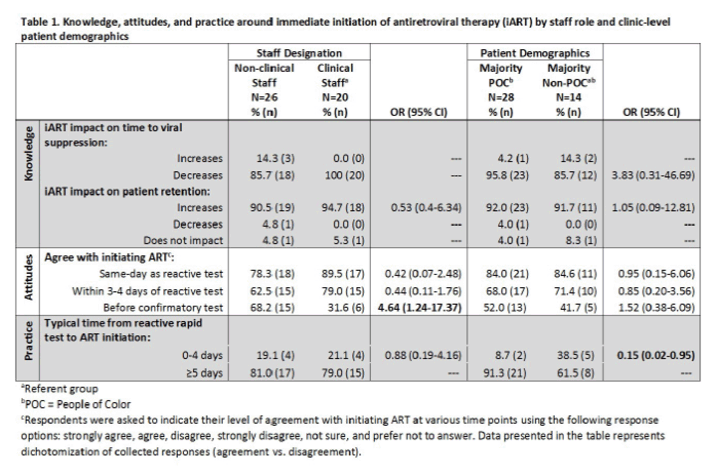
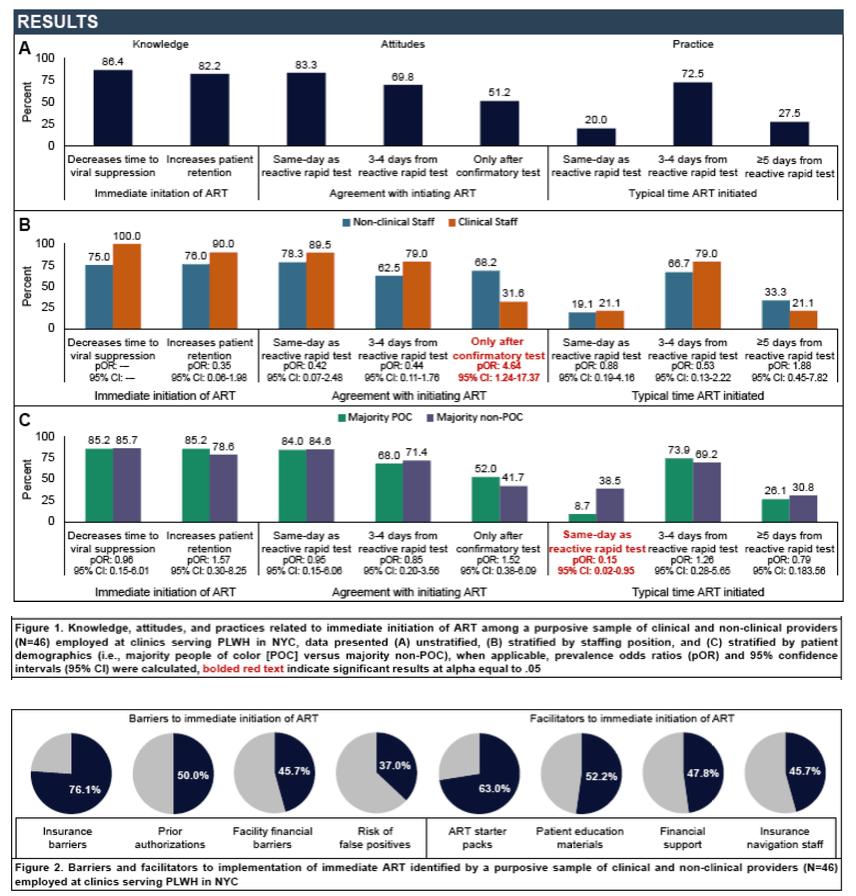
Results: We received 46 survey responses, representing 25 NYC clinics, 98% of which reported prior knowledge of iART. Over 80% of respondents identified iART as decreasing time to VS and increasing patient retention. Overall, 80% and 67% of respondents agreed that ART should be initiated on the same-day or within three to four days of a positive HIV test, respectively. Conversely, 51% of respondents believed ART should not be initiated prior to confirmatory test results, with non-clinical staff being more likely to hold this belief (odds ratio [OR]: 4.64, 95% confidence interval [CI]: 1.24-17.37). Among all respondents,66% reported zero to four days as the typical length of time from a positive HIV test to ART initiation. Clinics serving a majority people of color were less likely to meet the same-day benchmark (OR: 0.15, 95% CI: 0.02-0.95). Commonly reported facility-level and patient-level barriers to iART included: insurance barriers (76%), medication prior authorizations (50%), financial barriers (46%), and concern about false positives (37%). ART medication starter packs (63%) and patient education materials (52%) were the most commonly reported facilitators to iART.
Conclusion: Despite high levels of knowledge around the benefits associated with iART, it is not yet the standard of care across NYC clinics. The proven benefits of iART warrant further efforts to overcome barriers to implementation, with a focus on achieving health equity.

|
| |
|
 |
 |
|
|