 |
 |
 |
| |
EFFECTS OF HIV INFECTION AND IMMUNE REGULATION ON LONGITUDINAL LUNG FUNCTION DECLINE
|
| |
| |
CROI 2020 March 10
Reported by Jules Levin
Jing Sun, Jacquie Astemborski, SarathRaju, M. Brad Drummond, Robert H. Brown, Shruti H. Mehta, Richard D. Moore, Meredith C. McCormack,
Gregory D. Kirk, for the SHIELD study

Program Abstract
People living with HIV (PWH) have higher prevalence of lung function abnormalities compared to demographically and behaviorally similar people without HIV (HIV-). However, high quality longitudinal data describing the impact of HIV and of immune dysregulation on lung function decline over prolonged observation by age remains limited.
Data from the Study of HIV Infection in the Etiology of Lung Disease (SHIELD) cohort was used to evaluate the role of HIV and aging on lung function decline. Pre-bronchodilator FEV1 was repeatedly measured by spirometry at semiannual visits from 2009 to 2017 using ATS standards. HIV serostatus, HIV RNA, CD4 and CD8 counts were measured either in study or routine clinical visits. Time-varying CD4 nadir was defined as lowest CD4 observed up until each visit. Linear regression with generalized estimating equations, adjusted for age at entry, race, gender, current smoking status, and life-time pack-years, was used to evaluate longitudinal change in annualized FEV1 by HIV serostatus, CD4:CD8, and CD4 nadir.
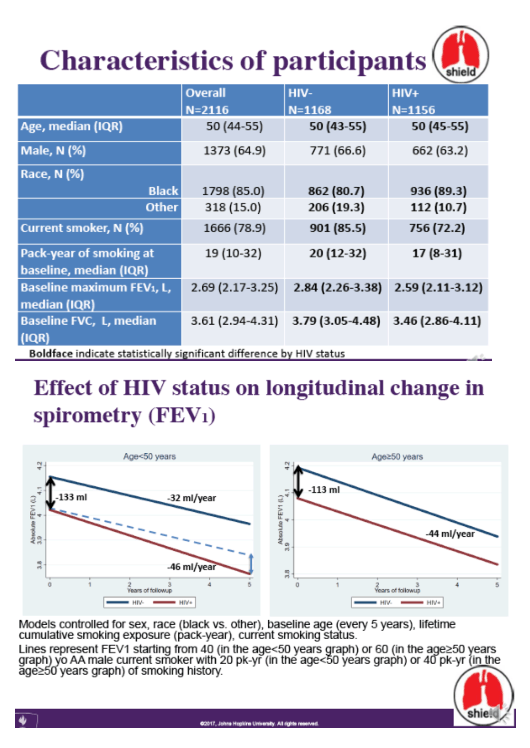
Of 1156 HIV+ and 1168 HIV- participants with 8341 person-years of follow-up, median age at entry was 50 years, 85% were black, 65% male, 79% current smokers, median cigarette exposure was 19 pack-years, and median % predicted FEV1 was 90%.
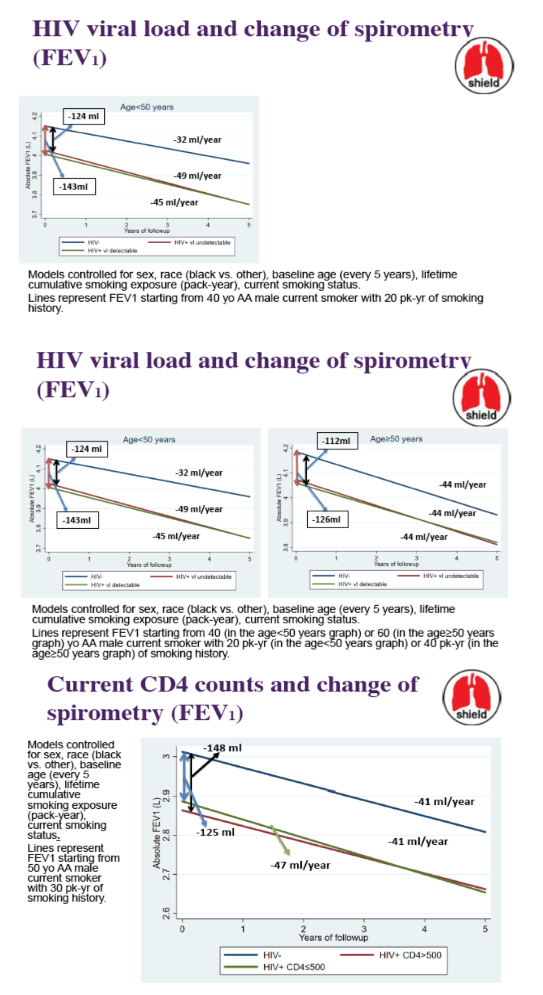
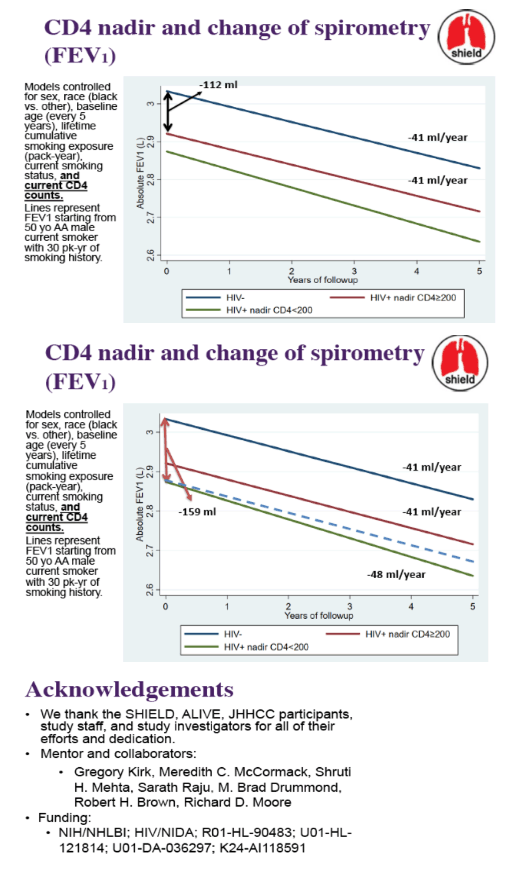
Among PWH, 38% had CD4 <200, 59% had detectable HIV RNA, 78% had CD4:CD80.8. At entry, PWH had 133 ml lower FEV1 compared to HIV- (p<0.01). FEV1 declined significantly faster among PWH before age of 50, but declined at similar rate after age of 50 (Table). Within the subset with available data (N=1518), PWH with immune dysregulation (CD4:CD8<0.8) had lower (-120ml, p<0.01) and faster decline (-6ml per year faster, pinteraction=0.02) of FEV1 compared to HIV-. PWH with CD4 nadir<200 also had lower (-159ml, p<0.01) and faster decline (-6ml/year faster, pinteraction=0.02) of FEV1 compared to HIV- adjusted for current CD4 and covariates.
Among these participants with heavy tobacco exposure, lung function was significantly lower among PWH compared to HIV- and declined more rapidly in PWH than HIV- in those age <50. Low CD4 nadir (independent of current CD4) and immune dysregulation had a significant impact on lung function decline, irrespective of age. This finding suggests that HIV may manifest with impaired lung function in earlier ages. It also addresses the importance of achieving immune regulation in order to preserve lung function among PWH.


|
| |
|
 |
 |
|
|