 |
 |
 |
| |
Rising BMI Tied to Risk of Diabetes But Not CVD in D:A:D Analysis
|
| |
| |
CROI 2020, March 8-11, 2020, Boston
Mark Mascolini
Body mass index (BMI) gains during antiretroviral therapy (ART) inflated the risk of diabetes in a 43,000-person D:A:D Cohort analysis [1]. But BMI gains did not drive up risk of cardiovascular disease (CVD).
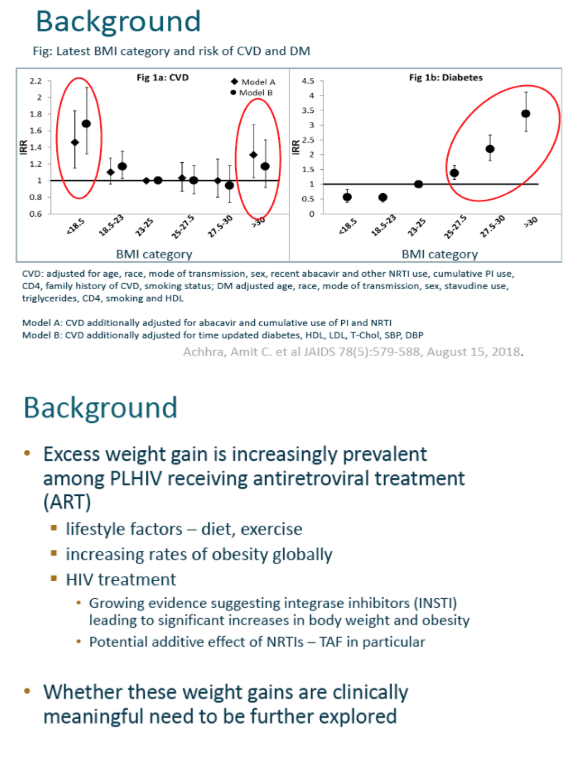
In the general population, research links rising BMI to diabetes, CVD, and other serious conditions. In people with HIV, low BMI boosts chances of cancer, CVD, and death [2]. Because overweight and obesity affect growing proportions of people with HIV, D:A:D investigators set out to determine the clinical impact of weight change in their cohort.
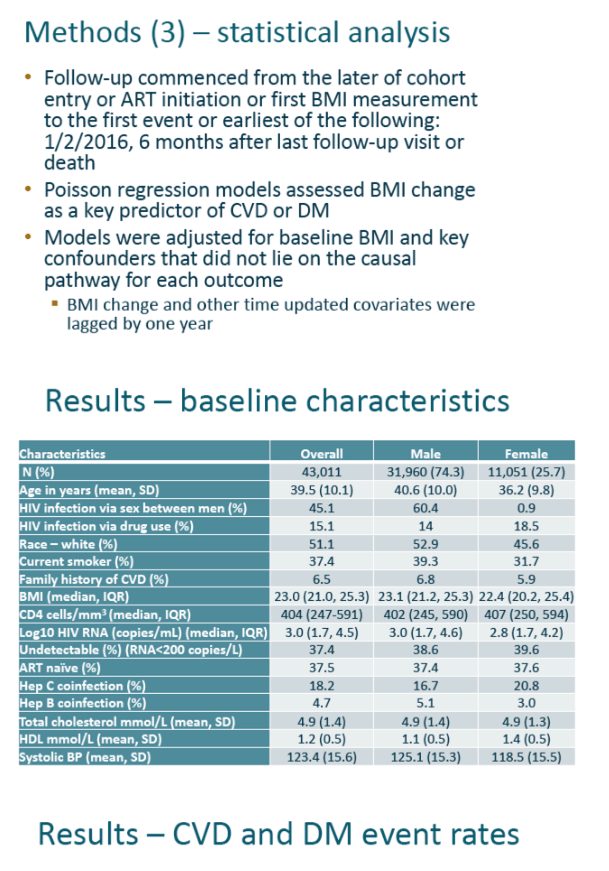
The analysis included all D:A:D participants taking ART who had at least two BMI measures and at least 1 year of further follow-up after entering the cohort in 1999-2009. The researchers excluded people who had previous CVD or diabetes. CVD meant myocardial infarction, stroke, or an invasive cardiovascular procedure. Diabetes was defined by standard measures including use of antidiabetic drugs. Follow-up began when people entered D:A:D, began ART, or had their first BMI measure, whichever came last. Follow-up continued until diabetes or CVD diagnosis, January 2016, 6 months after the last follow-up visit, or death, whichever came first.
D:A:D researchers grouped participants by baseline (initial) BMI: below 20, 20 to 25, 25 to 30, or 30+ kg/m2. BMI measured over time put participants into 5 change groups: decrease more than 2 kg/m2, decrease 1-2 kg/m2, stable (+/- 1 kg/m2), increase 1-2 kg/m2, or increase more than 2 kg/m2. The investigators used Poison regression to assess BMI change as a predictor of diabetes or CVD. They adjusted the model for initial BMI and for confounders that did not lie on the causal pathway for diabetes or CVD.
The 43,011 study participants included 31,960 men (74%) and 11,051 women (26%). Men were older than women (average 40.6 versus 36.2) and included a higher proportion of whites (52.9% versus 45.6%), a higher proportion of current smokers (39.3% versus 31.7%), and a higher proportion with a family history of CVD (6.8% versus 5.9%). Median baseline BMI was higher in men than women (23.1 versus 22.4 kg/m2).
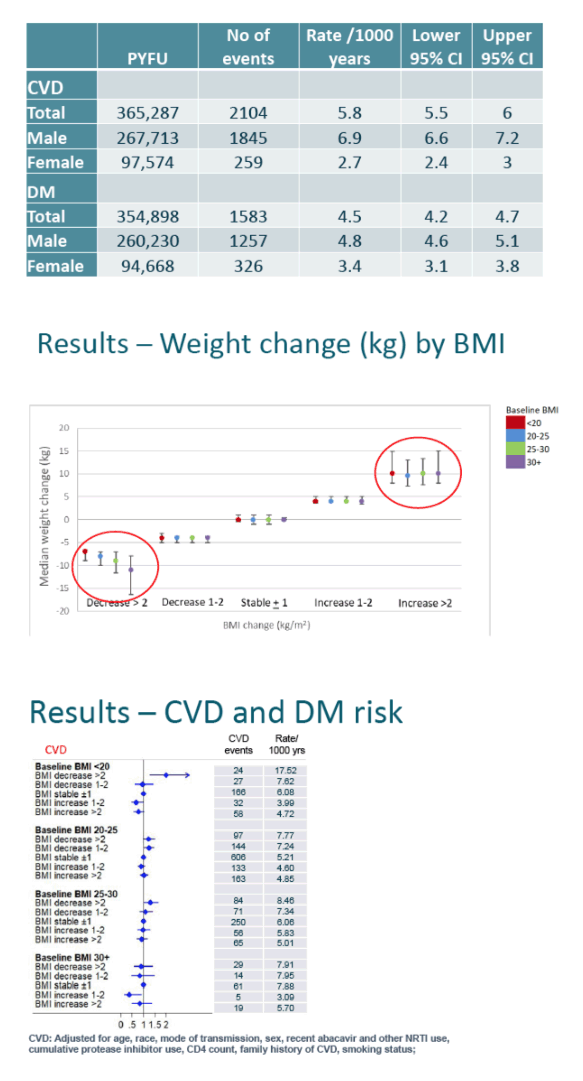
Overall new diagnoses of CVD measured 5.8 per 1000 person-years (6.9 in men and 2.7 in women), while new diabetes diagnoses stood at 4.5 per 1000 person-years (4.8 in men and 3.4 in women).
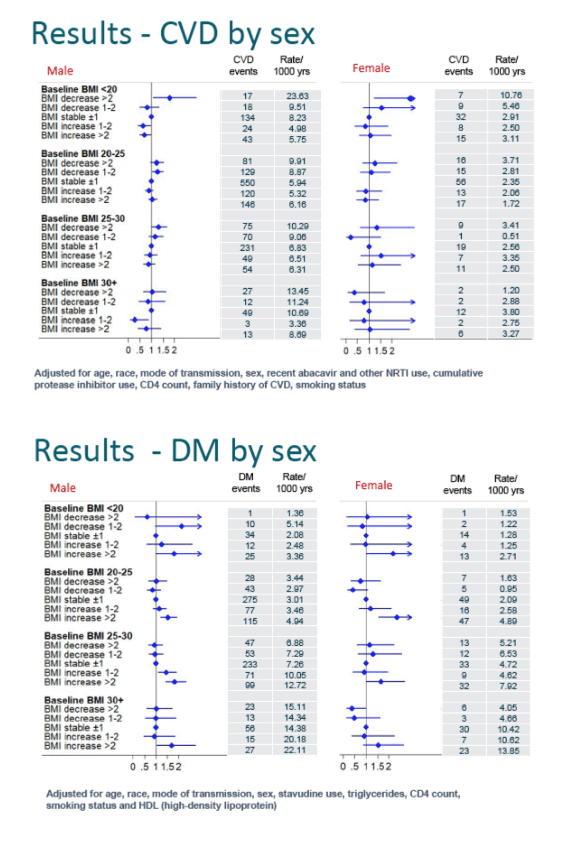
Across all baseline BMI levels, more than a 2-kg/m2 BMI increase was consistently independently associated with a higher risk of diabetes. Among people in the overweight range at baseline (25 to 30 kg/m2), a BMI gain of 1-2 kg/m2 independently boosted diabetes risk. These associations held true for both men and women in every baseline BMI bracket: gaining more than 2 kg/m2 during follow-up magnified diabetes risk.
In contrast, the analysis did not link rising BMI to higher CVD risk in men or women. Among both men and women who entered the cohort with a BMI below 20 kg/m2, a subsequent loss of more than 2 kg/m2 made CVD more likely.
The D:A:D team cautioned that their analysis did not consider the impact of specific antiretrovirals, particularly integrase inhibitors (study cutoff was January 2016). Therefore, they said, "the extent to which these results apply to people living with HIV with increased weight while receiving contemporary ART [is] uncertain." The researchers also cautioned that they did not have behavioral data that would affect weight, such as diet and exercise.
References
1. Petoumenos K, Kuwanda L, Ryom L, et al. Changes in body mass index and risk of cardiovascular disease: the D:A:D study. Conference on Retroviruses and Opportunistic Infections (CROI). March 8-11, 2020. Boston. Abstract 83.
2. Achhra AC, Sabin C, Ryom L, et al. Body mass index and the risk of serious non-AIDS events and all-cause mortality in treated HIV-positive individuals: D: A: D cohort analysis. J Acquir Immune Defic Syndr. 2018;78:579-588.



|
| |
|
 |
 |
|
|