 |
 |
 |
| |
GREATER INCIDENCE OF DIABETES OVER 10 YEARS
AMONG DEPRESSED US VETERANS WITH HIV
|
| |
| |
CROI 2020
Reported by Jules Levin
Kassem Bourgi1, Suman Kundu2, Jesse C. Stewart1, Matthew Freiberg2, Samir K. Gupta1
1Indiana University, Indianapolis, IN, USA,2Vanderbilt University, Nashville, TN, USA
Abstract
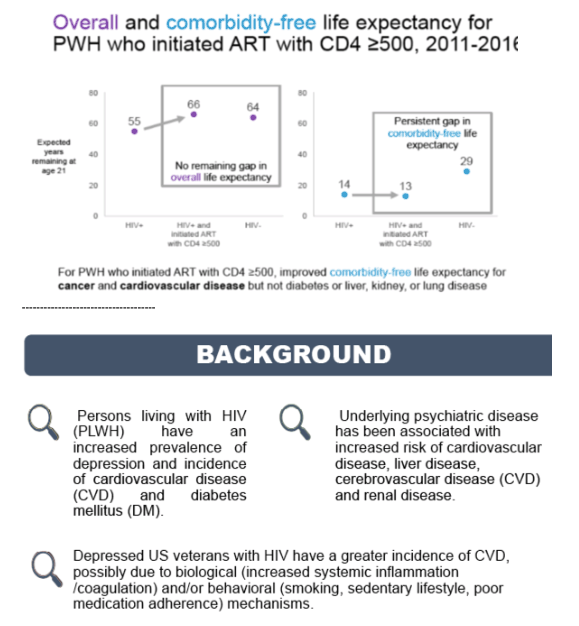
Persons living with HIV (PLWH) have an increased prevalence of depression and incidence of cardiovascular disease (CVD) and diabetes mellitus (DM). We previously found that depressed US veterans with HIV have a greater incidence of CVD, possibly due to biological (increased systemic inflammation/coagulation) and/or behavioral (smoking, sedentary lifestyle, insomnia, poor medication adherence) mechanisms. As these mechanisms may also predispose to DM, we evaluated whether baseline depressive symptom severity predicts incident DM in US veterans living with HIV.
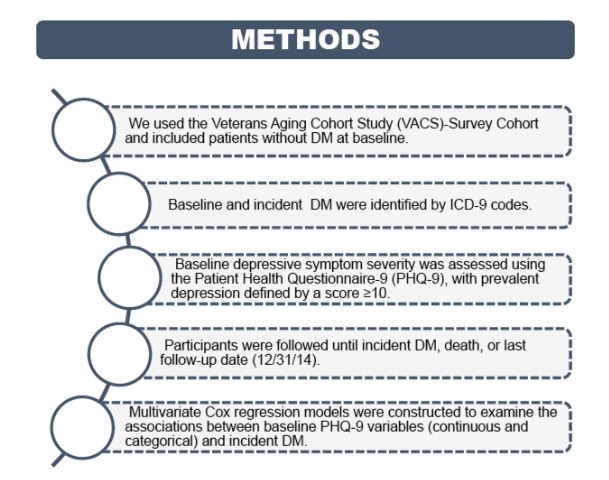
We used the Veterans Aging Cohort Study (VACS)-Survey Cohort and included patients without DM at baseline. Baseline DM was identified by a validated measure consisting of ICD-9 codes, laboratory tests, and DM medications. Baseline depressive symptom severity was assessed using the Patient Health Questionnaire-9 (PHQ-9), with prevalent depression defined by a score ≥10. Participants were followed until incident DM, death, or last follow-up date (12/31/14). Incident DM cases were identified by ICD-9 codes. Multivariate Cox regression models were run to examine the associations between baseline PHQ-9 variables (continuous and categorical) and incident DM.
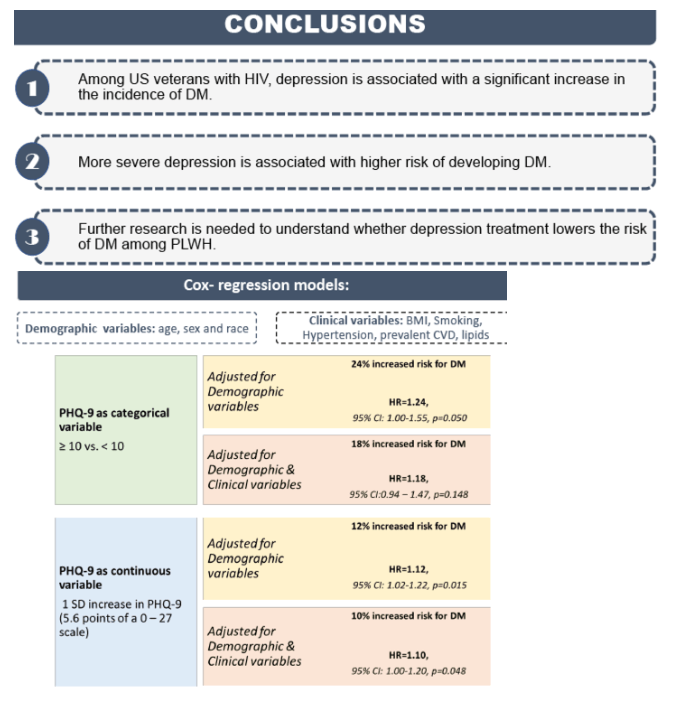
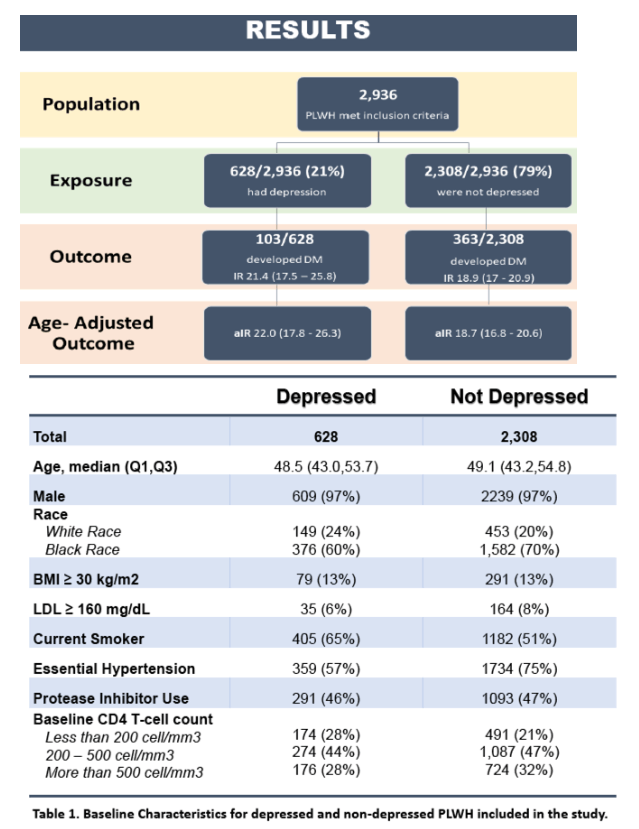
2,936 PLWH were included, 628 (21%) of whom had prevalent depression. The median follow-up time was 9.6 years, and a total of 466 (15.8%) incident diabetes cases were identified. The unadjusted incidence rate of DM per 100 person-year was 21.4 (95% CI: 17.5-25.8) in depressed veterans vs 18.9 (95% CI: 17.0-20.9) in nondepressed veterans. Cox models revealed that each 1-SD increase in PHQ-9 score (5.6 points of a 0-27 scale) was associated with a 12% (HR=1.12, 95% CI: 1.02-1.22, p=0.015) and 10% (HR=1.10, 95% CI: 1.00-1.20, p=0.048) increase in the risk of incident diabetes after adjustment for demographics alone and demographics plus traditional DM risk factors, respectively. Similarly, compared to nondepressed veterans, depressed veterans (PHQ-9 score10) had a 24% (HR=1.24, 95% CI: 1.00-1.55, p=0.050) and 18% (HR=1.18, 95% CI: 0.94-1.47, p=0.148) greater risk of incident diabetes after adjustment for demographics alone and demographics plus traditional DM risk factors, respectively.
Among US veterans with HIV, depression is associated with a significant increase in the incidence of DM. Future research should examine whether depression treatment lowers diabetes risk in PLWH.
EndFragment
----------------------------------------
CROI: CAUSES OF DEATH IN PERSONS WITH AND WITHOUT HCV INFECTION (03/18/20)
Among persons with HCV, the five most common causes of death were: Liver related (19.6%); malignancy (18.0%); ASCVD (16.8%); self-harm (6.2%); pulmonary disease (5.6%). Among those without HCV, the five most common causes were: Malignancy (25.2%); ASCVD (23.0%); pulmonary disease (7.8%); infections (5.4%); endocrine including diabetes (5.1%).
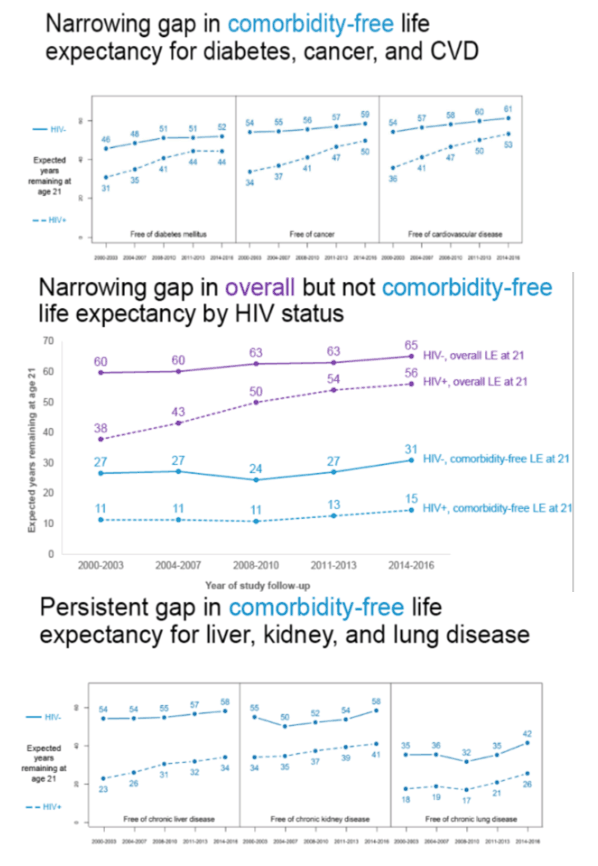
CROI: Increased overall life expectancy but not comorbidity-free years for people with HIV - (03/27/20)


|
| |
|
 |
 |
|
|