 |
 |
 |
| |
Anal Cancer Screening: Is it Time for Cytology and High-risk HPV Co-testing?
|
| |
| |
CROI 2020
Reported by Jules Levin
Michael Gaisa MD PhD1, Yuxin Liu MD PhD1, John Winters MD1, Ashish A. Deshmukh PhD2, Keith M. Sigel MD PhD1 1Icahn School of Medicine at Mount Sinai, New York, NY, USA, 2University of Texas at Houston, Houston, TX, USA
Program Abstract
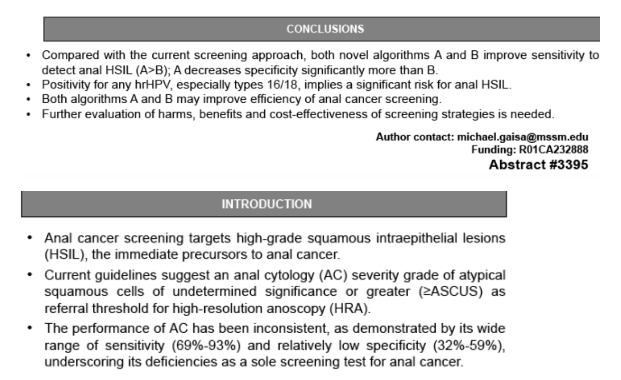
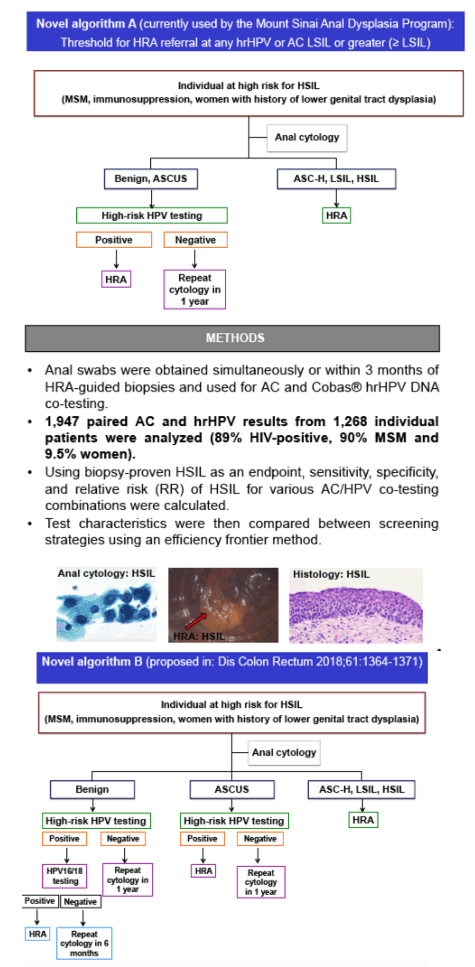
Anal cancer screening targets cancer precursors, defined as high-grade squamous intraepithelial lesions (HSIL). Current guidelines suggest an anal cytology (AC) severity grade of atypical squamous cells of undetermined significance or greater (ASCUS) as referral threshold for high-resolution anoscopy (HRA). This study sought to determine whether co-testing AC for high-risk human papillomavirus (hrHPV) improves screening performance and to compare the efficiency of two novel HRA referral thresholds to current clinical practice. Novel algorithm A sets the threshold for HRA referral at any hrHPV or AC with low-grade squamous intraepithelial lesion or greater (LSIL); algorithm B was recently proposed by Sambursky et al.
Anal swabs were obtained simultaneously or within 3 months of HRA-guided biopsies and used for AC and Cobas® hrHPV DNA co-testing. Using biopsy-proven HSIL as an endpoint we calculated sensitivity, specificity, positive predictive value (PPV) and negative predictive value (NPV) as well as relative risk (RR) of HSIL for various AC/HPV co-testing combinations. Test characteristics were then compared between screening strategies using an efficiency frontier method.
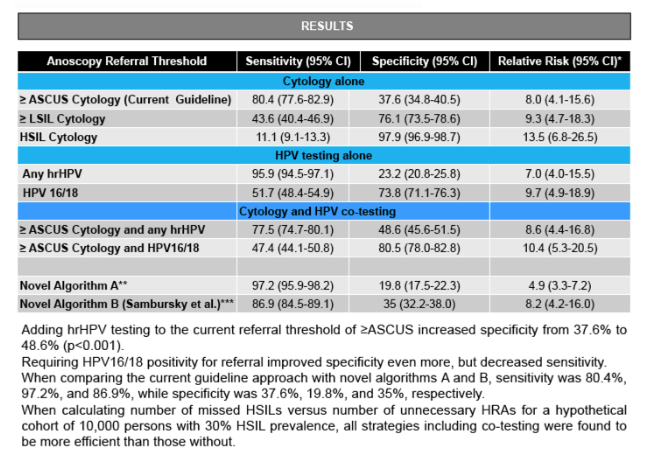
1,947 paired AC and hrHPV results from 1,268 individual patients were analyzed (89% HIV-positive, 90% MSM and 9.5% women). Adding hrHPV testing to the current AC referral threshold of ASCUS increased sensitivity from 80.4% to 95.9% (p<0.001). Requiring HPV16/18 positivity for referral markedly improved specificity but decreased sensitivity. For each AC category, the RR of HSIL was substantially greater when any hrHPV was detected. When comparing screening strategies, sensitivity for the current guideline approach, algorithm A and B was 80.4%, 96.4%, and 86.9%, while specificity was 37.6%, 22.4%, and 35%, respectively (see table). When calculating number of missed HSILs versus number of unnecessary HRAs for a hypothetical cohort of 10,000 persons with 30% HSIL prevalence, all strategies including co-testing were found to be more efficient than those without.
Co-testing AC for hrHPV improves the sensitivity to detect anal HSIL for all AC categories. Positivity for any hrHPV, especially types 16/18, implies a significant risk for anal HSIL. Algorithm A, combining LSIL AC and reflex hrHPV testing for benign and ASCUS cytology results, may improve efficiency of anal cancer screening.
|
| |
|
 |
 |
|
|