 |
 |
 |
| |
High Resolution Anoscopy (HRA) in the Real World:
Predictors of Guideline-Based Follow Up at a Large Academic Medical Center
|
| |
| |
CROI 2020
Reported by Jules Levin
Richard Silvera, MD, MPH1; Michael Gaisa, MD, PhD1; Yuxin Liu, MD, PhD1; Ashish Deshmukh, PhD, MPH2; Keith Sigel, MD, PhD, MPH1
1Icahn School of Medicine at Mount Sinai, New York, NY; 2University of Texas at Houston, Houston, TX

Program Abstract
Persons living with HIV (PLWH) have nearly 20-fold elevated risk of anal cancer compared to the general population. Several guidelines recommend annual anal cancer screening using anal cytology, high-resolution anoscopy (HRA) guided biopsies, and treatment of high grade intraepithelial lesions (HSIL), the precursors to anal cancer. Untreated HSIL can progress to invasive cancer and frequently recurs after treatment (>50%) necessitating longitudinal surveillance. Using data from our large screening cohort, we evaluated rates and predictors of adherence to surveillance HRAs following a diagnosis of anal HSIL.
The Mount Sinai Anal Dysplasia Program is an HRA referral site for a large urban population of PLWH and HIV-uninfected MSM. We collected data on demographics, HIV clinical variables, and HRA attendance and outcomes from 2009-2019. We identified patients who were diagnosed with HSIL on first HRA and measured the following outcomes: (1) adherence to any follow-up, including repeat HRA or ablation, at any time after initial HSIL diagnosis; (2) follow-up examination within 18 months of HSIL diagnosis; (3) return for HSIL ablation within 6 months; (4) surveillance HRA following ablation. We also evaluated the predictors of these outcomes.
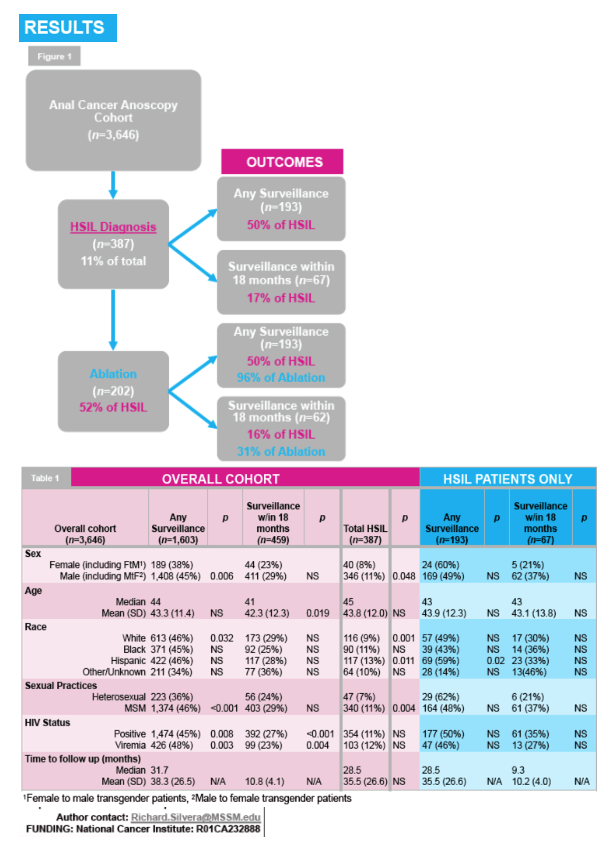
3,646 unique patients underwent at least one HRA during the study. 387 patients (11%) had HSIL or cancer on initial HRA. Of this group, median age was 45, 92% were PLWH, 90% were male, 88% MSM, with diverse race/ethnicity: 30% White, 23% Black, and 30% Hispanic. 202 patients (52% of the HSIL cohort; see Figure) underwent ablation. Median time to ablation from HRA was 49 days (10% were ablated >180 days). Of those who received ablation, 71% followed up at any time. Among those not receiving ablation, 27% followed up at any time. Among HSIL patients the only significant predictor of adherence to surveillance was Hispanic ethnicity (p=.02). 35% of patients diagnosed with HSIL never returned. Compared to Whites (69%), Hispanics were more likely to return (73%, p=.04), while Blacks (54%, p=.02) and PLWH with viremia (57%; p=.05) were less likely to return after HSIL diagnosis.
Adherence to treatment and surveillance following an initial diagnosis of anal HSIL was poor in a large, urban anal cancer screening cohort. Future research to understand barriers and facilitators could inform interventions to improve adherence to anal cancer screening.

|
| |
|
 |
 |
|
|