 |
 |
 |
| |
Need for optimization of screening methods for
anal intraepithelial neoplasia in people living with HIV
|
| |
| |
CROI 2020
Reported by Jules Levin
Stefan Esser1, Alexander Kreuter2, Anja Potthoff3, Norbert H. Brockmeyer3, Mark Oette4, Aylin Yavuz1, Karl-Heinz Jöckel5,6, Laven Mavarani5, Hildegard Lax5,6, Konstantinos Bilbilis5,6, Ulrike Wieland7
1Clinic of Dermatology, Department of Venereology, University Hospital Essen, Essen, Germany 2Department of Dermatology, Venereology and Allergology, Helios St. Elisabeth Hospital Oberhausen, University Witten-Herdecke, Oberhausen, Germany
3Department of Dermatology, Venereology and Allergology, Interdisciplinary Immunological Outpatient Clinic, Center for Sexual Health and Medicine, Ruhr University Bochum, Bochum, Germany
4Department of General Medicine, Gastroenterology and Infectious Diseases, Augustinerinnen Hospital, Cologne, Germany 5Institute for Medical Informatics, Biometry and Epidemiology (IMIBE), University Hospital Essen, Essen, Germany
6Centre for Clinical Studies Essen (ZKSE), c/o IMIBE, University Hospital Essen, Essen, Germany 7Institute of Virology, National Reference Center for Papilloma and Polyomavirus, University of Cologne, Faculty of Medicine and University Hospital of Cologne, Cologne, Germany

Abstract
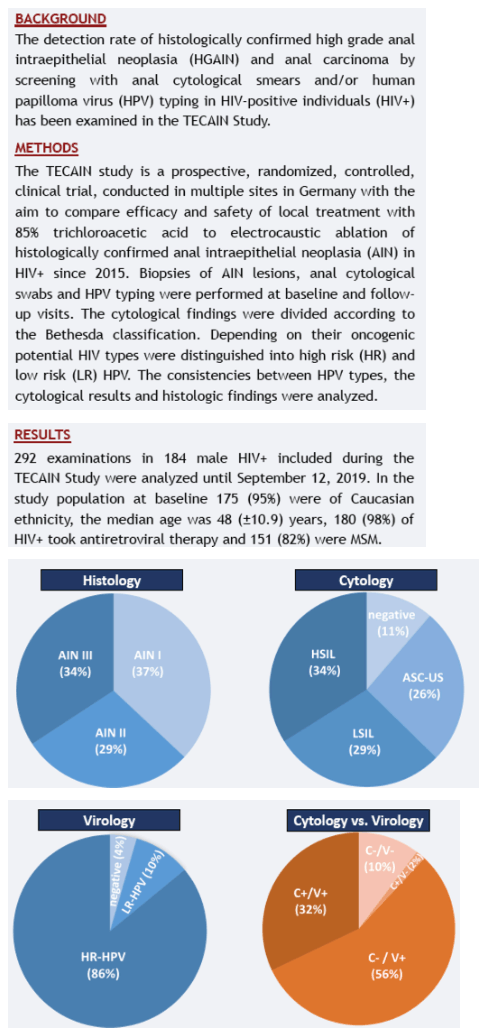
The detection rate of histologically confirmed high grade anal intraepithelial neoplasia (HGAIN) and anal carcinoma by screening with anal cytological (cyto.) smears and/or human papilloma virus (HPV) typing in HIV-positive individuals (HIV+) has been examined in the TECAIN Study.
The prospective, randomized, national, multicenter TECAIN study compared the efficacy of local treatment with 85% trichloroacetic acid to electrocaustic ablation of histologically confirmed AIN in HIV+ since 2015 in Germany. Biopsies of AIN lesions, anal cyto. Swabs and HPV typing were performed at Baseline and follow-up visits. The cyto. findings were divided according to the Bethesda classification. Depending on their oncogenic potential HIV types were distinguished into high risk (HR) and low risk (LR) HPV. The consistencies between HPV types, the cyto. results and histologic findings were analysed.
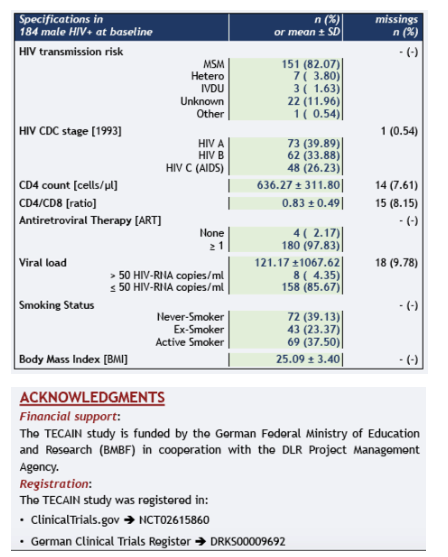
292 examinations (exa.) in 184 HIV+ included during the TECAIN Study were analyzed until September 12, 2019. At Baseline the median age was 48 years, 98% of HIV+ took antiretroviral therapy and 81% were MSM. Histologically, 108 exa. (37%) showed AIN I as the highest grade HPV-associated lesion, 84 (29%) AIN II and 100 (34%) AIN III. Thus in 184 exa. (63%) HGAIN were detected. At the same time, LSIL diagnosed in 84 (29%), ASC-US in 76 (26%), HSIL in 99 (34%) and negative cyto. results in 33 (11%) cases. Virologically, in 251 cases (86%) at least one HR-HPV could be diagnosed and 28 (10%) LR-HPV. No HPV was detected in 13 (4%) exa.. A cyto. screening found no HSIL in 66.3% of all HGAIN cases. No HR-HPV was detected in 12% of all HGAIN cases. If both cytology and virology results were considered together, only 10.3% of all HGAIN cases showed no higher grade abnormalities.
Simultaneous screening with anal cyto. and virological smears detect HGAIN much more reliable than cytology alone (fig. 1). Comparable results in gynecology have led to an extension of routine diagnostics by the addition of HPV typing to cervical cancer screening guidelines in Germany. Fig. 1: Results (n=292) of virological and cytological examinations of all HGAIN cases in the TECAIN RCT and detection rates in simultaneous screening of cytological (C+) and virological (V+) smears.

|
| |
|
 |
 |
|
|