 |
 |
 |
| |
Trends in Marijuana, Alcohol, and Opioid Use in Pregnant and Postpartum Women with HIV
|
| |
| |
CROI 2020
Reported by Jules Levin
Lynn M. Yee MD MPH1,Deborah Kacanek ScD2, Chase Brightwell MS2, Lisa B. Haddad MD MPH3, Jennifer Jao MD MPH1, Kathleen M. Powis MD2,4, Tzy-Jyun Yao PhD2, George R. Seage III ScD2, and Ellen G. Chadwick MD1, for the Pediatric HIV/AIDS Cohort Study1Northwestern University Feinberg School of Medicine, 2Harvard TH Chan School of Public Health, 3Emory University School of Medicine, 4Massachusetts General Hospital

Abstract
Concurrent with the opioid epidemic in the United States (US), rates of marijuana use have risen among pregnant and non-pregnant women of reproductive age. Amid evolving legal and social changes, little is known about substance use among pregnant and postpartum women living with HIV (WLHIV). Our objective was to evaluate trends over time in marijuana, alcohol, and opioid use during pregnancy and the first year postpartum among US WLHIV.
We analyzed data on marijuana, alcohol, and/or opioid use from the Surveillance Monitoring for ART Toxicities (SMARTT) study of the Pediatric HIV/AIDS Cohort Study. SMARTT has been enrolling pregnant WLHIV at 22 US sites since 2007. SMARTT-enrolled pregnant WLHIV from 2007-2019 with self-reported substance use data available in pregnancy, 1 year postpartum, or both were included (postpartum opioid use not collected). Prevalence of any marijuana, alcohol, opioid, and concomitant alcohol and marijuana use was calculated by calendar year, separately for pregnancy and postpartum periods. We fit log binomial general estimating equation models to evaluate linear trend in use over time, accounting for repeat pregnancies.
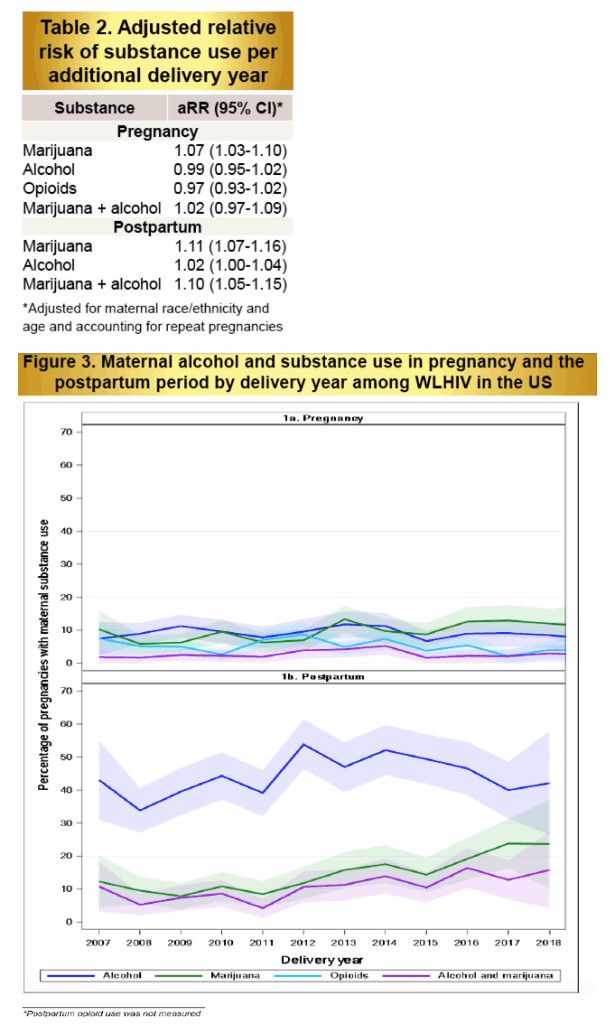
Substance use data were available for 2,926 pregnancies from 2,310 WLHIV. Women were primarily non-Hispanic black (63.5%) or Hispanic (28.1%) and aged 25-39 years (67.6%). Between 2007 and 2019, marijuana use during pregnancy increased from 7.1% to 11.7% (Figure 1a). Alcohol and opioid use in pregnancy were unchanged over this period (mean prevalence 9.4% and 5.2% respectively). Alcohol and marijuana use were more prevalent in the 1st trimester compared to the 2nd or 3rd, while opioid use was similar across trimesters. In the postpartum period, alcohol and marijuana use were common (mean prevalence 44.4% and 13.6% respectively), with marijuana increasing over time (Figure 1b). On average, risk of marijuana use increased each year by 6% and 11% for pregnancy and postpartum, respectively (Relative Risk [RR] 1.06, 95% Confidence Interval [CI] 1.03-1.10; RR 1.11, 95% CI 1.06-1.16). Postpartum combined alcohol and marijuana use increased from 6.7% to 16.4%, a 10% per year increase (RR 1.10, 95% CI 1.05-1.15).
Opioid use among pregnant and postpartum WLHIV in SMARTT remained low and stable despite the US opioid epidemic, whereas the prevalence of marijuana use increased between 2007 and 2019, as did postpartum concomitant alcohol use. Increasing marijuana use in pregnant and postpartum WLHIV warrants further attention.


|
| |
|
 |
 |
|
|