 |
 |
 |
| |
Cost Analysis Questions Value of F/TAF vs Generic F/TDF for PrEP
|
| |
| |
Download the PDF here
CROI 2020, March 8-11, 2020, Boston
Mark Mascolini
Switching from the initial preexposure prophylaxis (PrEP) pill emtricitabine/tenofovir disoproxil fumarate (F/TDF) to the recently licensed emtricitabine/tenofovir alafenamide (F/TAF) could prevent 25 cases of end-stage renal disease and more than 2000 fractures over 5 years, according to a cost-effectiveness analysis by researchers at Massachusetts General Hospital and the Yale School of Public Health [1,2]. But the higher cost of F/TAF than a probably imminent generic F/TDF may be too steep to justify those safety gains, the researchers argued in their cost analysis.
In a poster presented at CROI [1] and an article simultaneously published in Annals of Internal Medicine [1], Rochelle Walensky and colleagues estimated "the greatest possible clinical benefits and economic savings" with F/TAF, as well as the highest price payers should be willing to tolerate for F/TAF over generic F/TDF.
Sold as Truvada, F/TDF became the only licensed PrEP pill in 2012. F/TAF got licensed for PrEP in 2019 and proved virologically noninferior to F/TDF, while upsetting kidney and bone markers less, in the DISCOVER trial [3,4].
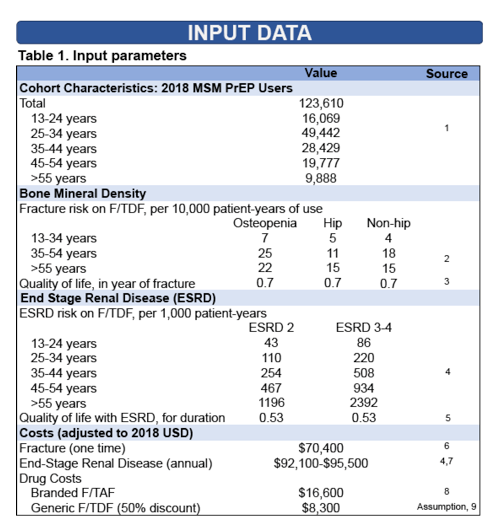
The Mass General-Yale team used published data to estimate fractures, end-stage renal disease cases, quality-adjusted life years (QALYs), costs, and cost-effectiveness of F/TAF. They claimed to "tip the scales" in favor of F/TAF in portraying its potential bone and kidney advantages in the best possible light. For example, they assumed that all fractures resulting from F/TDF use would require surgery and all cases of severe kidney disease would be irreversible and require dialysis.
Setting societal "willingness to pay" thresholds at $50,000, $100,000, and $150,000, the researchers projected maximum justifiable prices for F/TAF. Then they estimated the number of people in the United States who could get F/TDF or F/TAF if the entire US HIV prevention budget--more than $900 million--went only to pay for PrEP.
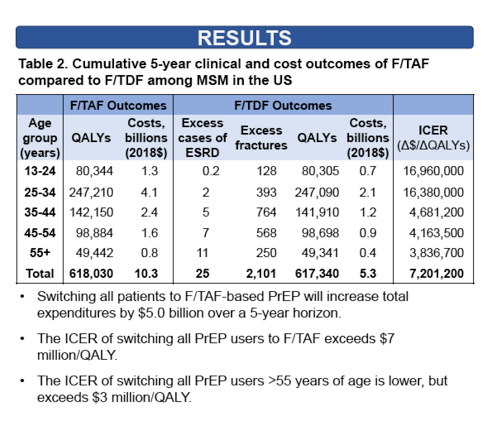
In an analysis limited to US men who have sex with men (MSM), using F/TDF rather than F/TAF for 5 years would lead to 25 excess cases of end-stage renal disease, the researchers calculated, and to 2101 excess fractures. Total 5-year QALYs for MSM would be similar for F/TAF (618,030) and F/TDF (617,340). But 5-year costs would stand almost twice higher with F/TAF ($10.3 billion) than F/TDF ($5.3 billion). The incremental cost-effectiveness ratio (ICER, change in cost/change in QALYs) of switching all PrEP users to F/TAF would be $7.2 million/QALY.
If society were willing to pay no more than $100,000 per QALY, the investigators reckoned that the "maximum justifiable price markup" of F/TAF over F/TDF would be $370 in the total population and $670 in an older-than-55 population.
F/TAF carries an annual price tag of $16,000 if used daily. With the US HIV prevention budget set at $900.8 million, the Mass General-Yale group calculated that F/TAF would allow no more than 54,300 people in the United States to get PrEP. That number amounts to 11% of an estimated 492,000 US MSM. If all PrEP users switched to a generic PrEP that costs 50% of F/TAF, PrEP coverage would double. PrEP coverage would quadruple if generic F/TDF came in at a 75% discount compared with F/TAF.
In their article [2] the researchers concede their analysis rests on daily dosing of F/TAF. Using PrEP only before and after sex has proved as effective as daily PrEP [5] and would cost considerably less.
But focused on the results as they stand, the researchers proposed that "the imminent availability of generic F/TDF represents an extraordinary opportunity to expand PrEP coverage among the most price-sensitive members of the HIV at-risk population."
References
1. Walensky RP, Horn T, McCann NC, Freedberg K, Paltiel AD. F/TAF vs F/TDF for PrEP: How much is "better" worth? Conference on Retroviruses and Opportunistic Infections (CROI). March 8-11, 2020. Boston. Abstract 1089.
2. Walensky RP, Horn T, McCann NC, Freedberg K, Paltiel AD. Comparative pricing of branded tenofovir alafenamide-emtricitabine relative to generic tenofovir disoproxil fumarate-emtricitabine for HIV preexposure prophylaxis. Ann Intern Med. 2020. doi: 10.7326/M19-3478.
3. Hare CB, Coll J, Ruane P, et al. The phase 3 DISCOVER study: daily F/TAF or F/TDF for HIV preexposure prophylaxis. Conference on Retroviruses and Opportunistic Infections. March 4-7, 2019. Seattle. Abstract 104. http://www.natap.org/2019/CROI/croi_21.htm
4. Krakower DS, Daskalakis DC, Feinberg J, Marcus JL. Tenofovir alafenamide for HIV preexposure prophylaxis: what can we DISCOVER about its true value? Ann Intern Med. 2020 Jan 14. doi: 10.7326/M19-3337.
5. Molina JM, Charreau I, Spire B, et al. Efficacy, safety, and effect on sexual behaviour of on-demand pre-exposure prophylaxis for HIV in men who have sex with men: an observational cohort study. Lancet HIV. 2017;4:e402-e410.
|
| |
|
 |
 |
|
|