 |
 |
 |
| |
Testosterone Use Tied to Signals of Atherosclerosis Progression in Men With HIV
|
| |
| |
CCROI 2020, March 8-11, 2020, Boston
Mark Mascolini
HIV-positive men who used testosterone therapy--especially new users--ran a higher risk of worsening signals of atherosclerosis than men who formerly used testosterone [1]. The study also tied low total testosterone to one marker of atherosclerosis progression.
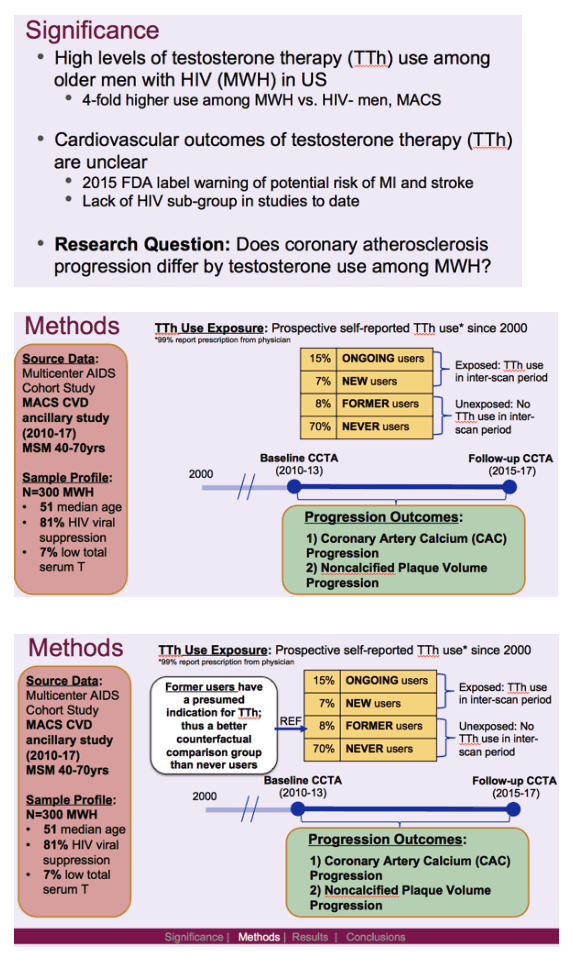
Testosterone use remains high among men with HIV, especially older men, noted Multicenter AIDS Cohort Study (MACS) researchers who conducted this analysis. They observed that the long-term cardiovascular impact of testosterone boosting remains unclear, particularly in men with HIV, who often have other cardiovascular risk factors.
To address these issues, the MACS team compared markers of atherosclerosis over time in HIV-positive men who currently, formerly, or never used testosterone. MACS men 40 to 70 years old had cardiac CT angiograms to evaluate subclinical coronary plaque progression between a baseline visit in 2010-2013 and a follow-up visit in 2015-2017. Median time between scans stood at 4.6 years.
Men classified themselves as ongoing testosterone users, new users, former users, or never users. The researchers recorded atherosclerosis progression by measuring both coronary artery calcium and coronary artery plaque. To assess the impact of testosterone use on coronary artery calcium and plaque progression, they used multivariable models adjusted for demographics, cardiovascular risk factors, and HIV-related factors.
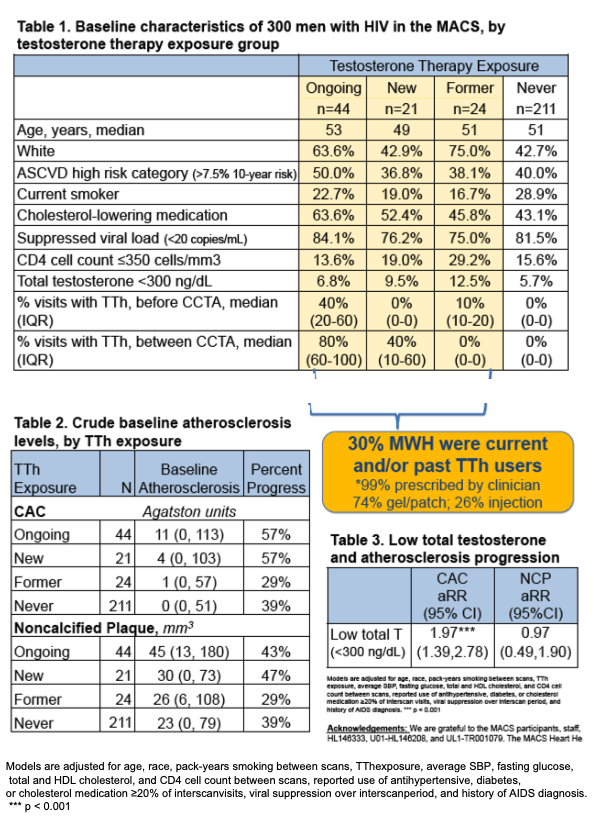
The study group included 44 ongoing testosterone users, 21 new users, 24 former users, and 211 never users. Median age was similar across the four groups: 53, 49, 51, and 51. Three quarters or more in each group had an HIV load below 20 copies (84%, 76%, 75%, and 82%). Proportions of current smokers among ongoing testosterone users, new users, former users, and never users were 23%, 19%, 17%, and 29%, and proportions with more than a 7.5% 10-year atherosclerotic cardiovascular disease risk were 50%, 37%, 38%, and 40%. Respective proportions of men with baseline total testosterone below 300 ng/dL were 6.8%, 9.5%, 12.5%, and 5.7%. These last results suggested that former users had a presumed need and prescription for testosterone therapy, and therefore the researchers used them as the comparison group in statistical analyses.
Rates of coronary artery calcium progression were higher in new and ongoing testosterone users (57% of both groups) than in never users (39%) or former users (29%). Noncalcified plaque progression risk was also higher in new users (47%) and ongoing users (43%) than in never users (39%) or former users (29%).
Multivariate analysis determined that adjusted relative risk of coronary artery calcium progression was significantly higher in new testosterone users (2.37) and ongoing users (1.99) than in former users. New users also had a significantly higher adjusted relative risk of noncalcified plaque progression than formers users (2.16). Ongoing users had a nonsignificantly higher risk of noncalcified plaque progression than formers users (1.52). Low baseline total testosterone (below 300 ng/dL) also predicted coronary artery calcium progression (but not noncalcified plaque progression) independent of testosterone use, demographic factors, and health factors (adjusted relative risk 1.97).
The MACS investigators believe these are the first HIV-specific findings on how testosterone use affects subclinical cardiovascular disease outcomes in a way that can inform clinical decisions. They recommended "attention to cardiovascular disease risk factors and guideline-driven implementation of cardiovascular disease risk reduction strategies" in men taking or contemplating testosterone therapy.
Reference
1. Haberlen SA, Post WS, Budoff M, et al. Testosterone therapy and subclinical atherosclerosis progression among men with HIV. Conference on Retroviruses and Opportunistic Infections (CROI). March 8-11, 2020. Boston. Abstract 642.
-------------------------------





|
| |
|
 |
 |
|
|