 |
 |
 |
| |
IMPACT OF PrEP AND TasP ON INCIDENCE OF HIV DIAGNOSES IN 48 HIGHEST-BURDEN US AREAS
|
| |
| |
CROI 2020 March 10
Reported by Jules Levin
Robertino Mera Giler1, Staci Bush1, Trevor Hawkins1, Moupali Das1, Julius Asubonteng1, Scott McCallister1
1Gilead Sciences, Inc, Foster City, CA, USA
program abstract
Background: Use of Tenofovir Disoproxil/Emtricitabine (TVD) for Pre-Exposure Prophylaxis (PrEP) has significantly reduced the HIV diagnosis rate in many US states, independent of the effect of treatment as prevention (TasP).
Methods: Using publicly available HIV surveillance data on HIV diagnoses from 105 US metropolitan statistical areas (MSAs) (2012-2017), virologic suppression data from 38 US states and DC as a proxy for Treatment as Prevention (TasP), and TVD for PrEP drug utilization obtained from a national pharmacy and medical claims database, we evaluated the independent impact of PrEP and TasP on HIV diagnosis rates in 48 counties and localities in the End the Epidemic Initiative (48-ETE). We calculated the person time at risk of HIV infection excluding time of those taking PrEP as well as those who became HIV positive. Incidence rates, rate ratios and 95% confidence intervals were assessed using a multilevel Poisson regression model for the 48-ETE and overall after adjusting for the effect of PrEP and TasP.
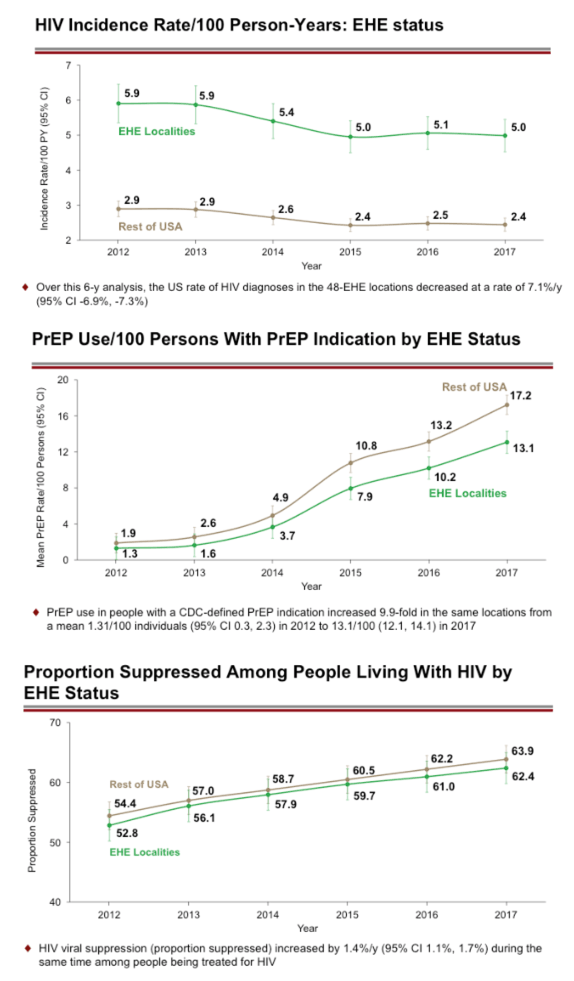
Results: Over this 6-year analysis, the US rate of HIV diagnoses in the 48-ETE locations decreased at a rate of 7.1% (95%CI –6.9 to –7.3%) per year while PrEP use in those with a CDC-defined PrEP indication increased 9.9-fold in the same locations from a mean 1.31/100 individuals (95% CI 0.3-2.3) in 2012 to 13.1/100 (95% CI 12.1-14.1) in 2017. HIV viral suppression (viral load <200 c/mL) increased by 1.4% per year (95% CI 1.1 to 1.7%) during the same time among HIV treated subjects. A multivariate poisson model showed that PrEP use was significantly associated with the decline in the rate of new HIV cases in the 48-ETE localities, independent of a significant TasP effect. 48-ETE localities with an average PrEP use rate of 17.4 per 100 subjects at risk could expect a decline of 15.5% in the rate of new HIV diagnoses. 48-ETE localities had significantly higher new HIV diagnosis rate than the rest of the US MSAs (IRR 2.0, 95% 1.61 – 2.58), but had a significantly lower PrEP use (-2.1 per 100 subjects at risk, 95% CI -0.93 to -3.2), and TasP proportion (-1.30 %, 95% CI -0.41 to -2.2%) than those MSAs not selected for intervention.
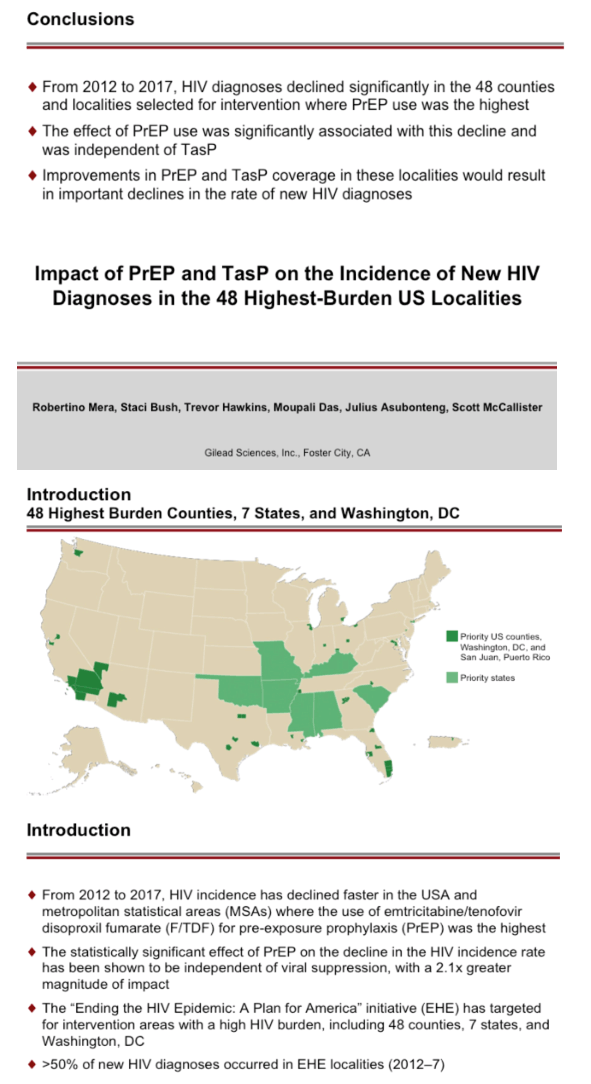
Conclusion: From 2012-2017, HIV diagnoses declined significantly in the 48 counties and localities selected for intervention where PrEP use was the highest. The effect of PrEP use was significantly associated with this decline and was independent of treatment as prevention. Improvements in PrEP and TasP coverage in these localities could yield important declines in the rate of new HIV diagnoses.


|
| |
|
 |
 |
|
|