 |
 |
 |
| |
IMPLEMENTATION OF MOBILE PrEP, STI, AND HIV
PREVENTION SERVICES IN SOUTH FLORIDA
|
| |
| |
CROI 2020
Reported by Jules Levin
Susanne Doblecki-Lewis1, Erin Kobetz1, Stefani A. Butts1, Katherine Klose1, Angela M. McGaugh1, Brian B. Leon1, Gilianne Narcisse1, Jessica Morel1, Yue Pan1
1University of Miami, Miami, FL, USA,2Prevention305, Miami, FL, USA

Abstract Body:
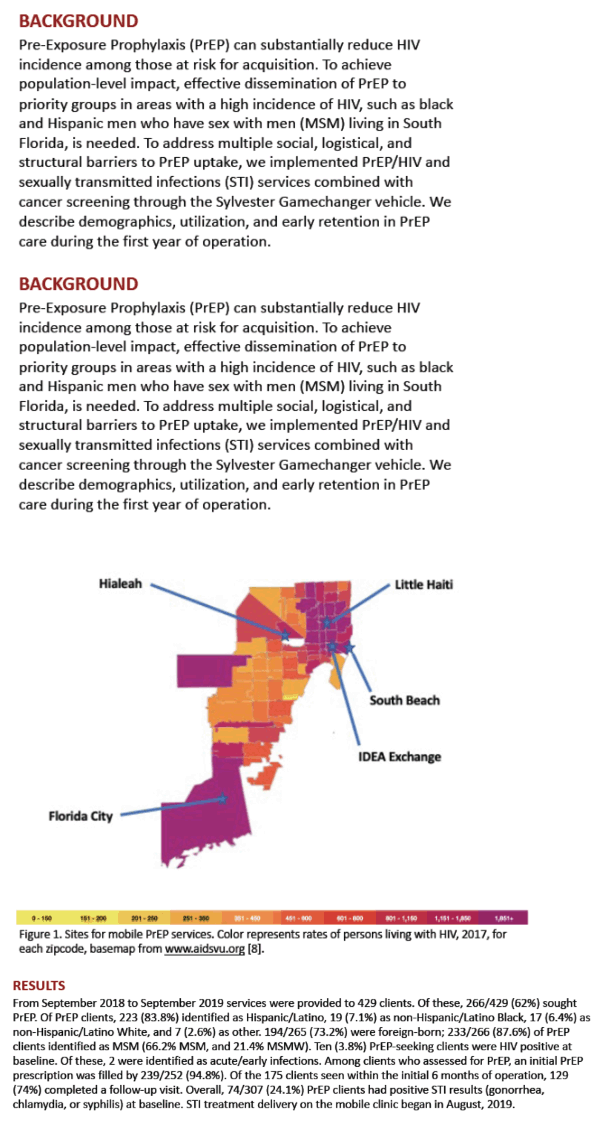
Pre-Exposure Prophylaxis (PrEP) can substantially reduce HIV incidence among those at risk for acquisition. To achieve population-level impact, effective dissemination of PrEP to priority groups in areas with a high incidence of HIV, such as black and Hispanic men who have sex with men (MSM) living in South Florida, is needed. To address multiple social, logistical, and structural barriers to PrEP uptake, we implemented PrEP/HIV and sexually transmitted infections (STI) services combined with cancer screening through the Sylvester Gamechanger vehicle. We describe demographics, utilization, and early retention in PrEP care during the first year of operation.
The mobile clinic was positioned at 4 sites in Miami with high HIV incidence with input from community stakeholders. Key program personnel were a medical provider, HIV/PrEP counselors, and a pharmacist. In addition to self-referrals, Prevention305 and Latino Salud, community-based organizations, developed focused patient recruitment through social media. All services were provided at no cost. Normative demographics, risk behavior, STIs, and early-maintenance-in-care data, were collected. Descriptive statistics were compiled using SPSS.
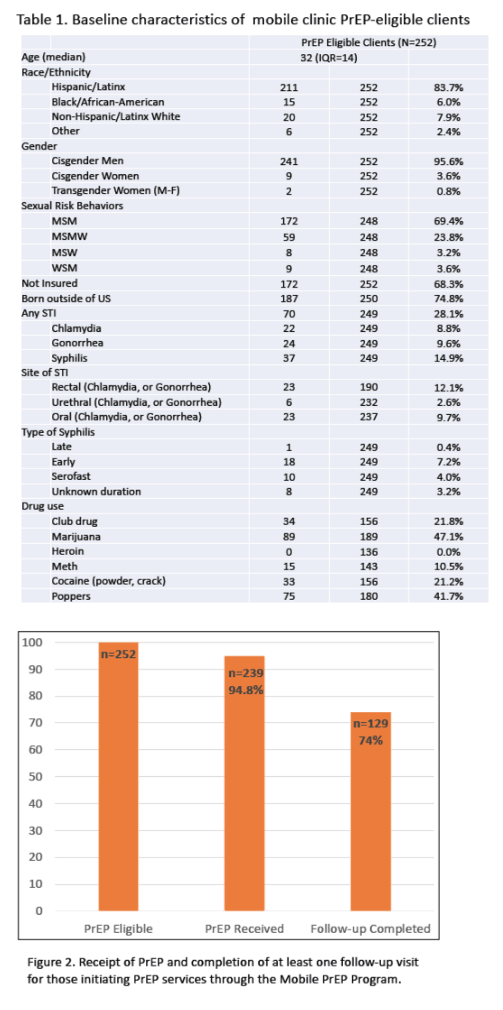
From September 2018 to September 2019 services were provided to 429 clients. Of these, 266/429 (62%) sought PrEP. Of PrEP clients, 223 (83.8%) identified as Hispanic, 19 (7.1%) as non-Hispanic Black, 17 (6.4%) as non-Hispanic White, and 7 (2.6%) as other. 194/265 (73.2%) were foreign-born; 233/266 (87.6%) of PrEP clients identified as MSM (66.2% MSM only, and 21.4% MSMW). Ten (3.8%) PrEP-seeking clients were HIV positive at baseline. Of these, 2 were identified as acute/early infections. Among clients assessed for PrEP, an initial PrEP prescription was filled by 239/251 (95.2%). Of the 175 clients seen within the initial 6 months of operation, 129 (74%) completed a follow-up visit. Overall, 74/307 (24.1%) PrEP clients had positive STI results (gonorrhea, chlamydia, or syphilis) at baseline. STI treatment delivery on the mobile clinic began in August, 2019.
Implementation of HIV-PrEP prevention and STI services using a mobile clinic model is acceptable and effective in engaging Hispanic/Latino immigrant MSM at risk for HIV and STIs. Low-barrier-to-entry services delivered through a mobile clinic inclusive of other prevention services can be an effective method for engagement of priority populations with difficulty accessing traditional clinic settings.

|
| |
|
 |
 |
|
|