 |
 |
 |
| |
Risk of Hepatocellular Carcinoma among Persons Living with HIV and Viral Hepatitis Coinfection in the United States and Canada, 1996-2015
|
| |
| |
Increasing screening & access to care my help reduce risk for HCC
CROI 2020 March 11
Reported by Jules Levin
Jing Sun, Keri Althoff, YuezhouJing, Mari M. Kitahata, Chad J. Achenbach, GypsyamberD’Souza, Marina Klein, Bryan Lau, Joseph Lim, Vincent Lo Re, Julia L. Marcus, Angel M. Mayor, Michael J. Silverberg, Gregory D. Kirk, for the NA-ACCORD of IeDEA

program abstract
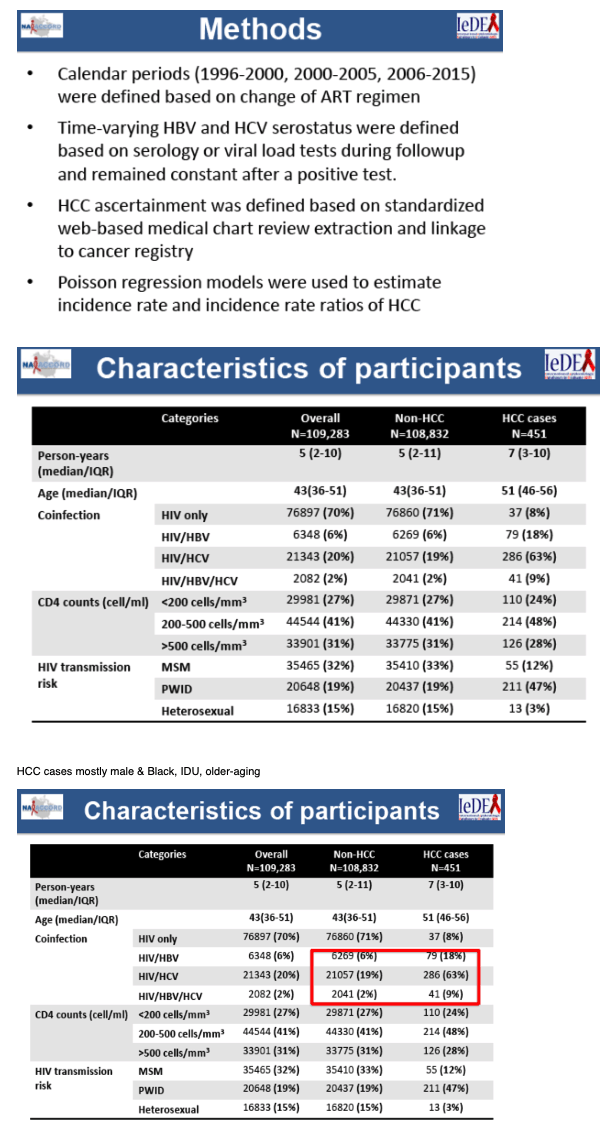
People living with HIV (PWH) are often co-infected with HBV and HCV, leading to increased risk of hepatocellular carcinoma (HCC). HCC risk may have changed in the current era of potent combination antiretroviral therapy (ART). We assessed temporal trends in HCC among PWH, comparing HCC rates by viral hepatitis infection status, risk populations, and HIV disease severity in the North America AIDS Cohort Collaboration on Research and Design (NA-ACCORD).
We examined 3 calendar periods: early- (1996-2000), mid- (2001-2005), and modern- ART (2006-2015). HCC diagnoses were identified and validated through cancer registries or medical records. HBV and HCV infection were confirmed by serologic and/or virologic test and categorized as ever, never infected, or missing. CD4 counts were measured at entry of each calendar period or the beginning of cohort-specific cancer diagnosis ascertainment. HIV RNA viral load (vl) was measured two years before HCC diagnosis or before the end of cancer diagnosis ascertainment. Poisson regression models estimated HCC incidence rates (IR) and rate ratios (aIRR), adjusted for age, sex, race, and viral hepatitis infection. Age-related cumulative incidence of HCC by calendar periods were calculated.
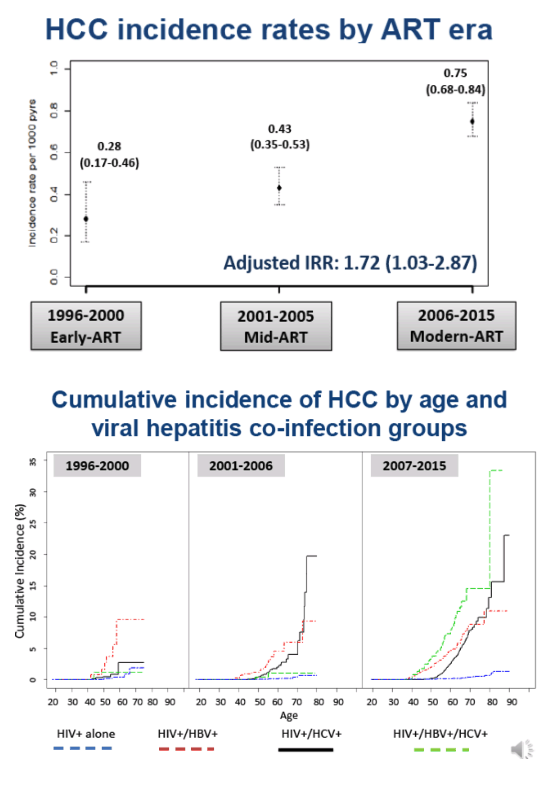
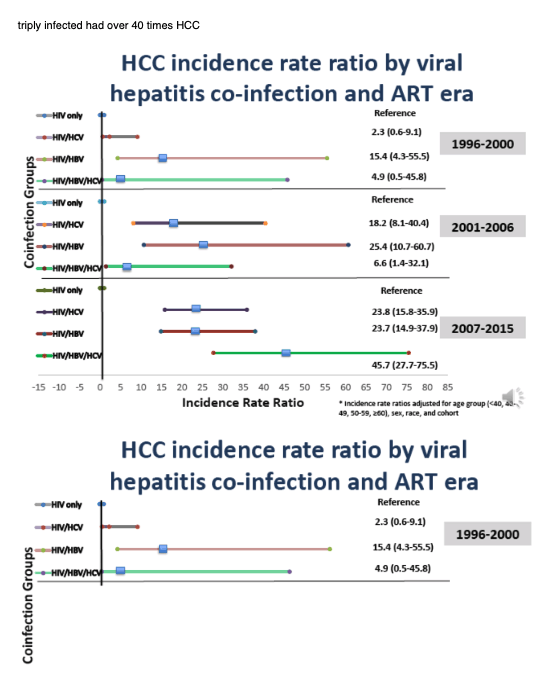
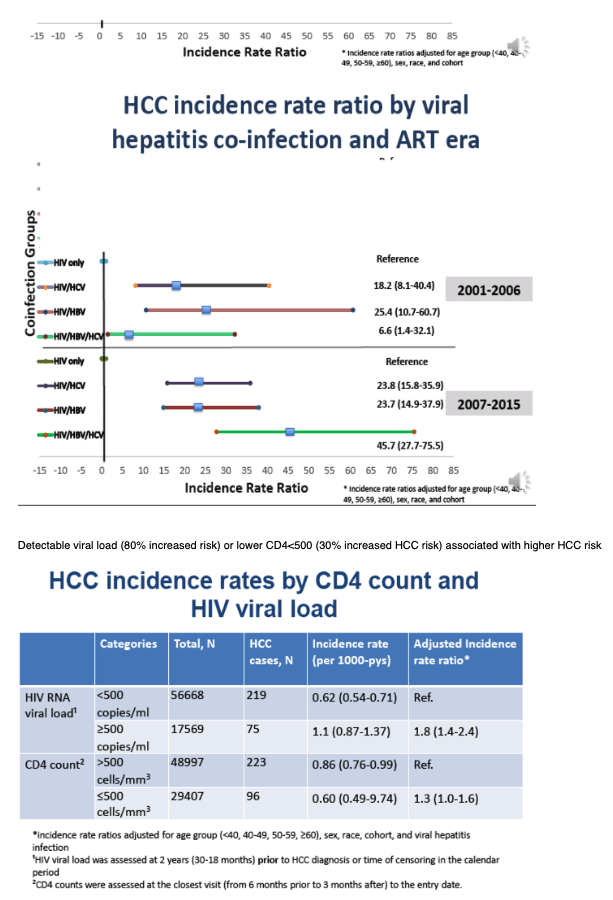
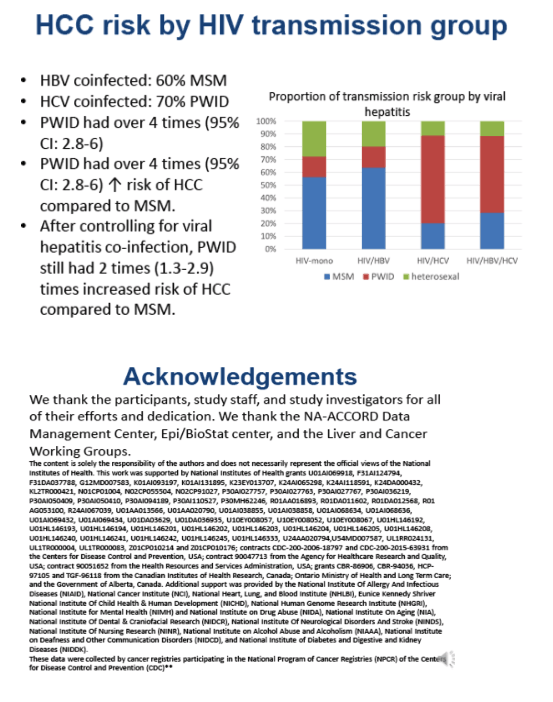
Of 109,283 HIV patients with 723,441 person-years (pys) of follow-up, 20% were HCV co-infected, 6% HBV co-infected, 2% triple-infected, 451 developed HCC. PWH who had HBV and/or HCV co-infection were more likely than HIV-monoinfected PWH to develop HCC and did so at earlier ages. From 1996 to 2015, HCC IR increased from 0.28 to 0.75/1000 pys. As compared to HIV-monoinfected persons, PWH co-infected with HBV and/or HCV had substantially greater age-related cumulative incidence of HCC in all 3 periods (Figure). Higher HIV vl (500 copies/ml) and lower CD4 counts (500 cells/mL) were associated with higher HCC risk (aIRR: 1.8, 95% confidence interval (CI): 1.4-2.4 and aIRR: 1.3, 95% CI: 1.0-1.6, respectively). People who injected drugs had higher HCC risk compared with men who had sex with men (aIRR: 2.0, 95% CI: 1.3-2.9), even after controlling for viral hepatitis co-infection.
HCC rates among PWH increased significantly over time. Patients with viral hepatitis co-infection, lower CD4, higher HIV vl, or HIV transmission through injection drug use had higher HCC risk. These findings suggest the importance of HIV viral suppression and treatment of viral hepatitis among PWH in the ART era in order to reduce HCC risk.

|
| |
|
 |
 |
|
|