 |
 |
 |
| |
Can More People Stops NRTIs for HBV? Hints From a 48-Week Study
|
| |
| |
EASL 2020, Digital International Liver Congress, August 27-29, 2020
Mark Mascolini
Stopping nucleot(s)ide analogs (NRTIs) in noncirrhotic hepatitis B e-antigen (HBeAg)-negative people with chronic HBV infection always led to virologic relapse in an ongoing study, but 5% of participants had HBsAg loss within 48 weeks [1]. This interim analysis linked HBsAg loss to HBsAg below 10 IU/mL before stopping therapy. Nine in 10 participants remain off treatment at 48 weeks. Australian researchers who conducted the NA-STOP study believe their results suggest that treatment withdrawal may be appropriate for certain people on long-term NRTI therapy.
HBV treatment guidelines recommend indefinite NRTI therapy for people with HBeAg-negative chronic HBV infection. (HBeAg indicates active, transmissible HBV infection.) But some people who stop long-term NRTIs have sustained virologic suppression off treatment, and 6% to 55% have HBsAg loss. (HBsAg indicates current HBV infection.) International guidelines differ on when NRTI discontinuation may be tried in HBeAg-negative people with chronic HBV.
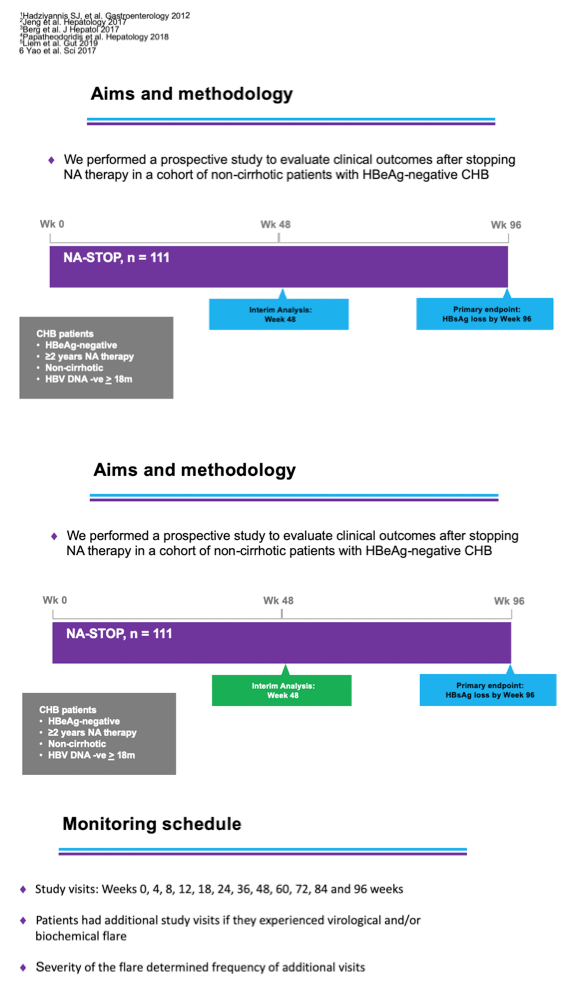
To explore these dynamics, Australian investigators mounted NA-STOP, a prospective multicenter study of stopping NRTIs in HBV patients without cirrhosis who attain long-term virologic suppression on treatment. The study included HBeAg-negative, noncirrhotic patients with virologic suppression for at least 18 months on NRTI therapy taken without interruption for at least 2 years. The protocol called for restarting NRTIs if (1) HBV DNA rose above 2000 IU/mL with (a) either alanine aminotransferase (ALT) more than 5 times the upper limit of normal (ULN) for at least 16 consecutive weeks, or (b) ALT more than 10 times ULN for at least 8 consecutive weeks, or with (2) International Normalized Ratio (INR) at or above 1.5, (3) bilirubin more than 2 times ULN, (4) any clinical feature of portal hypertension (ascites) or hepatic encephalopathy, or (5) investigator discretion.
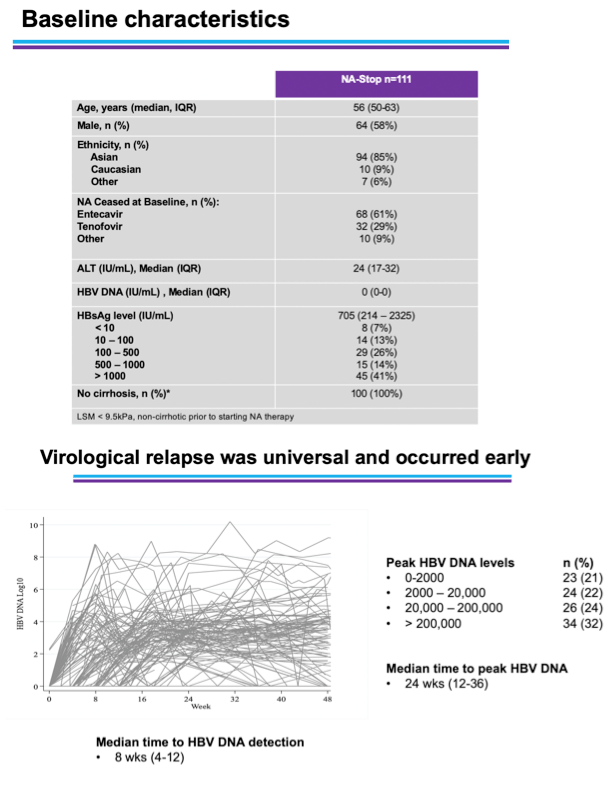
Primary analysis will come 96 weeks after NRTIs stop. This preliminary 48-week analysis involved 107 of 111 participants. When NA-STOP members enrolled, they had a median age of 56 years, 58% were men, 85% were Asian, and 9% were Caucasian. No patients had cirrhosis, and median HBsAg stood at 705 IU/mL (interquartile range [IQR] 214 to 2325).
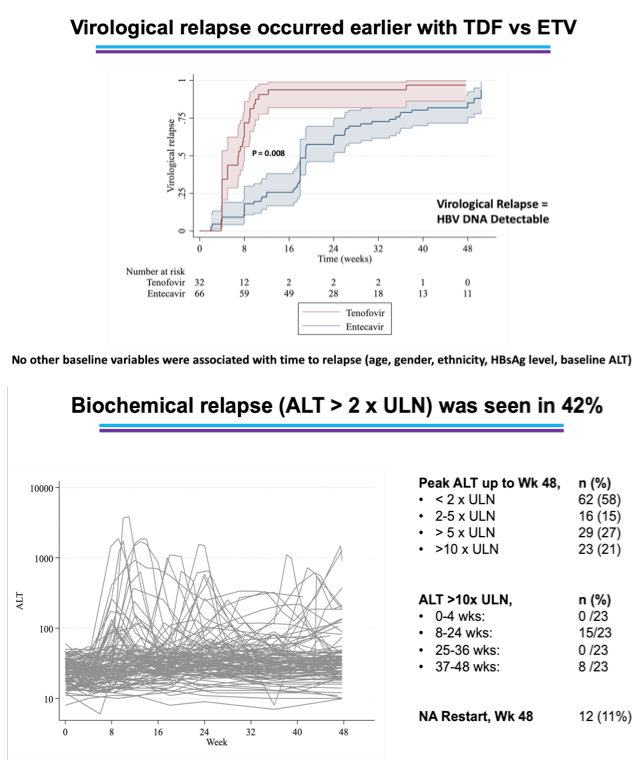
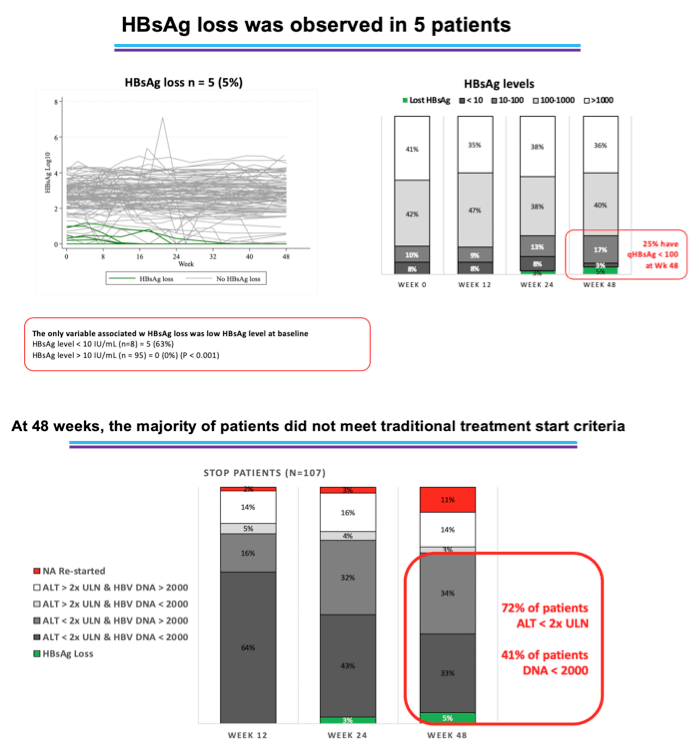
All participants experienced virologic relapse when treatment stopped, with a median time to HBV reactivation of 8 weeks (IQR 4 to 12). Relapse occurred significantly earlier with tenofovir disoproxil fumarate (TDF) than with entecavir (P = 0.008). Twenty-three study participants (21% of 107) had peak HBV DNA below 2000 IU/mL, 24 (22%) had peak HBV DNA between 2000 and 20,000 IU/mL, 26 (24%) peaked at 20,000 to 200,000 IU/mL, and 34 (32%) peaked above 200,000 IU/mL.
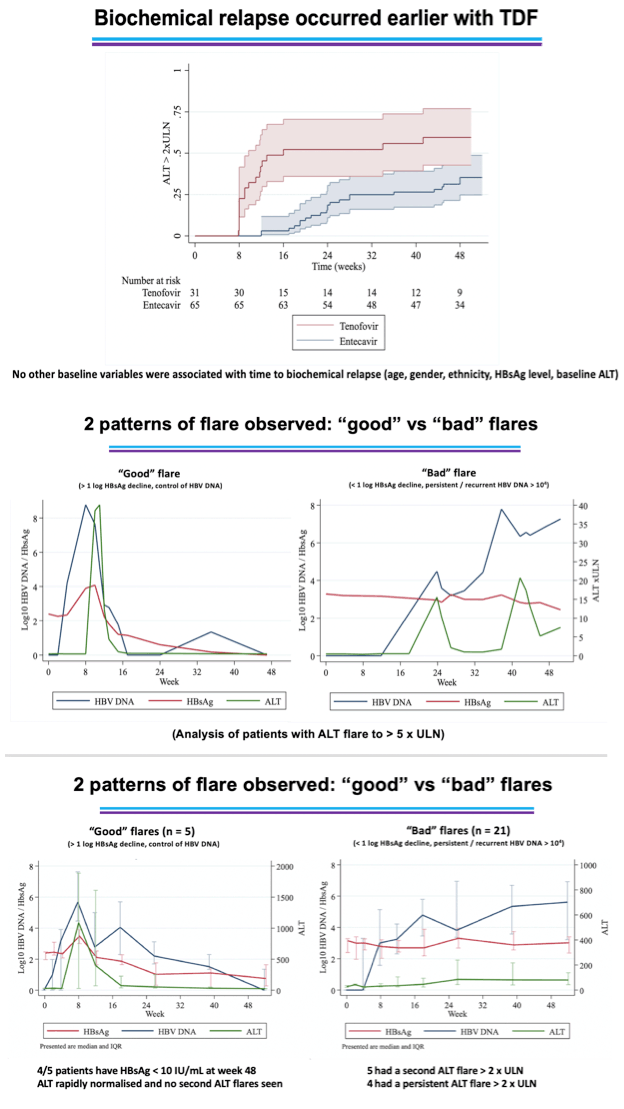
The researchers observed two ALT flare patterns: a "good" flare indicated by more than a 1-log (10-fold) drop in HBsAg and HBV DNA control), and a "bad" flare with less than a 10-fold drop in HBsAg and persistent or recurrent HBV DNA. Five study participants (4.7% of 107) had "good" flares and 21 (19.6%) had "bad" flares. Four of 5 people with "good" flares had an HBsAg below 10 IU/mL 48 weeks after NRTI withdrawal. In those people, ALT rapidly returned to normal and no secondary ALT flares occurred.
All 5 people with "good" flares attained HBsAg loss. Only one variable predicted HBsAg loss: HBsAg below 10 IU/mL before treatment stopped (P < 0.001 vs participants with an on-treatment HBsAg above 10 IU/mL). At week 48, 5% of participants had HBsAg below 10 IU/mL, 17% were between 10 and 100 IU/mL, 40% were between 100 and 1000 IU/mL, and 36% were above 1000 IU/mL.
At the 48-week point, 11% of participants had restarted NRTI therapy. At 48 weeks, 72% of participants had an ALT below 2 times ULN and 41% had HBV DNA below 2000 IU/mL.
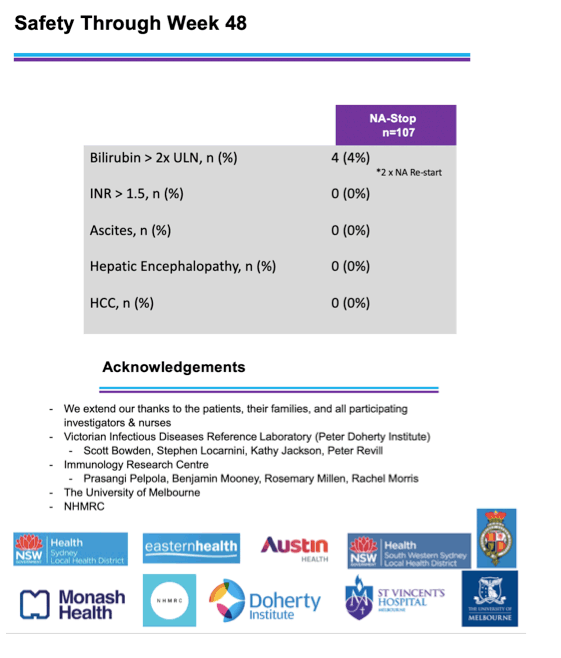
NRTI withdrawal proved largely safe through 48 weeks. At that point only 4 people (4%) had bilirubin more than 2 times ULN. No one had an International Normalized Ratio (ILN) above 1.5, ascites, hepatic encephalopathy, or hepatocellular carcinoma.
Summing up, the NA-STOP team stressed that 89% of people remained off treatment 48 weeks after stopping NRTI therapy, and 41% had HBV DNA below 2000 IU/mL. Follow-up will continue through 96 weeks. Five people had HBsAg loss at 48 weeks, and all had an HBsAg below 10 IU/mL before stopping therapy. The researchers believe their findings "support a place for treatment withdrawal in selected patients on long-term [NRTI] therapy."
Reference
1. Hall S, Burns G, Levy M, et al. A prospective study of nucleot(s)ide analogue discontinuation in non-cirrhotic HBeAg-negative chronic hepatitis B patients: interim analysis at week 48 demonstrates profound reductions of HBsAg associated with ALT flare. EASL 2020, Digital International Liver Congress, August 27-29, 2020. Abstract AS095.



|
| |
|
 |
 |
|
|