| |
|
Effect of Metabolic Traits on the Risk of Cirrhosis and Hepatocellular Cancer in Nonalcoholic Fatty Liver Disease
|
| |
| |
Nov 2019
Download the PDF here
A Comparison Study of Prevalence and Risk Factors for Nonalcoholic Fatty Liver Disease (NAFLD) and Nonalcoholic Steatohepatitis (NASH) by Transient Elastography (TE) in HIV Infected Patients, Newark....http://www.natap.org/2019/IDWeek/IDWeek_35.htm
Each additional metabolic trait increased the risk of cirrhosis and HCC in patients with NAFLD. Diabetes conferred the highest risk of progression to HCC. Patients with diabetes and coexisting hypertension and obesity may be important targets for secondary prevention.
We assembled a retrospective cohort of patients with NAFLD diagnosed at 130 facilities in the Veterans Administration between January 1, 2004, and December 31, 2008, with follow‐up through December 31, 2015
In this large cohort study of patients with NAFLD, we found that all four metabolic traits (diabetes, obesity, hypertension, and hyperlipidemia) were individually and jointly associated with an increased risk of developing incident cirrhosis and HCC. Higher burden of coexisting metabolic traits was linked with higher risk in this cohort with relatively mild liver disease at inception.
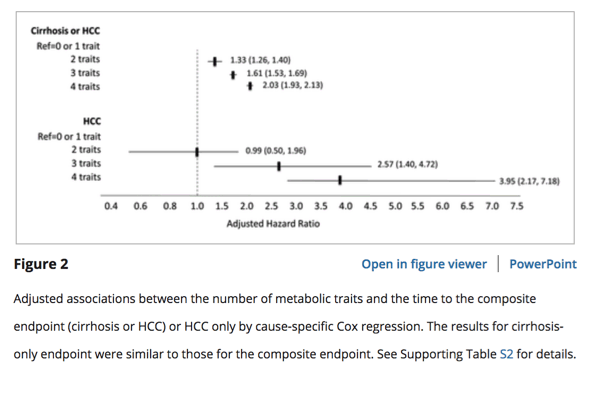
Of the 271,906 patients, 22,794 developed cirrhosis, and 253 developed HCC during a mean of 9 years follow‐up. At baseline, the mean body mass index was 31.6 (SD, 5.6), 28.7% had diabetes, 70.3% had hypertension, and 62.3% had dyslipidemia with substantial overlap among these traits. The risk of progression was the lowest in patients with only one or no metabolic trait. There was a stepwise increase in risk with each additional metabolic trait. Compared with patients with no metabolic trait, patients with both hypertension and dyslipidemia had 1.8‐fold higher risk of progression to cirrhosis/HCC (hazard ratio [HR] = 1.8, 95% confidence interval [CI] = 1.59‐2.06); the risk was 2.6‐fold higher in patients with diabetes, obesity, dyslipidemia, and hypertension (HR = 2.6, 95% CI = 2.3‐2.9). These associations were stronger for HCC. Diabetes had the strongest association with HCC in this cohort.
In summary, metabolic traits increased the risk of cirrhosis and HCC in this large cohort of patients with NAFLD. Diabetes had the strongest association with HCC in the presence or absence of cirrhosis. We were able to explain more of the progression risk when we considered metabolic traits jointly rather than individually. Our findings highlight the need for comprehensive evaluation of diabetes, hypertension, dyslipidemia, and obesity for prevention of future morbidity and mortality in NAFLD. Although several treatments for NAFLD are currently in the pipeline, these therapies may fail to stem the rising tide of cirrhosis and HCC in NAFLD if we do not simultaneously target coexisting metabolic traits.
| |
| |
| |
|
|
|