| |
Accelerated Aging - HIV+ Appear to be 5-17 Years Older Chronologic Age
|
| |
| |
These are collection of recent studies finding aging in HIV+ compared to HIV- by 5 to 17 years using epigenetic aging methods. Included is a collection of brain studies that did not use epigenetic testing and find accelerated brain aging by 3-15 years. These are in line with the report at CROI 2020 by Julia Marcus & Kaiser reporting 9 years average reduced survival in HIV+ but comorbidities remain a larger issue for these HIV+ vs HIV- in this study and authors emphatically saying health quality of life is bad due to these comorbidities, which is the case. I think clearly showing both HIV & comorbidities contribute to reduced survival, lifespan in HIV. Jules
CROI 2020: IMPACT OF ANTIRETROVIRAL THERAPY INITIATION ON EPIGENETIC AGING AND TELOMERE LENGTH
Age advancement (EA minus chronological age) significantly improved after ART initiation (BL: 8.3 vs W96: 6.5 years, p=0.007).
EA stabilized and EAA slowed in the majority of patients after starting ART. However, an age advancement of 6.5 years persisted after the first two years of successful ART. The reversal of epigenetic aging and the increase in blood TL caused by ART initiation are likely driven by changes in T cell subtypes toward less differentiated phenotypes.
At W96, EA correlated negatively with CD4+/CD8+ ratio by flow cytometry, estimated CD4+, nave CD4+ and nave CD8+, and positively with estimated CD8+CD28-CD45RA- T cells and NKs. Mean TL change at W96 was 0.034 (T/S). At W96 TL correlated positively with CD4+/CD8+ ratio by flow cytometry, estimated abundance of total CD4+, nave CD4+ and nave CD8+ and negatively with estimated abundance of CD8+CD28-CD45RA- and NKs (Table).
these numbers of 10-17 years accelerated aging are in line with recent study at CROI from Kaiser finding estimating & projecting an estimated average 9 years difference in lifespan, survival between HIV+ & HIV-neg:
CROI: Increased overall life expectancy but not comorbidity-free years for people with HIV - (03/27/20)
Brain Aging too in HIV+
The Aging HIV Brain - HIV Accelerates Brain Aging by 3 to 15 Years in Various Studies over the Past 9 years
HIV Accelerates Brain Aging by 3 to 15 Years in Various Studies over the Past 9 years
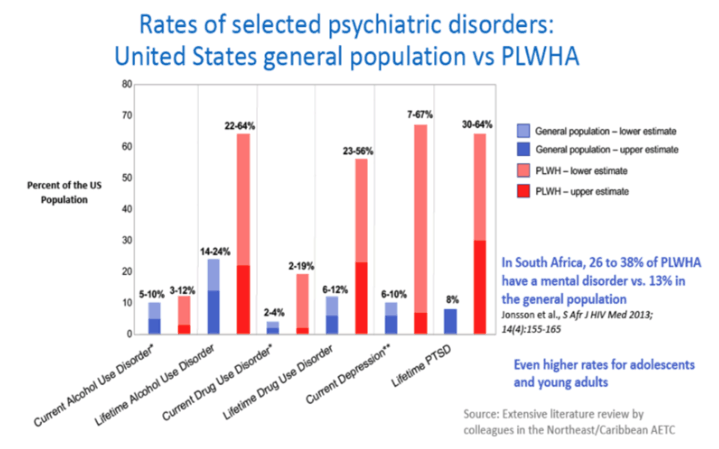
Acceleration of Age-Associated Methylation Patterns in HIV-1-Infected Adults.... adults appeared to be approximately 14 years older than their chronologic age MACS Men
Using this model, we estimate that HIV-1 infection accelerates age-related methylation by approximately 13.7 years in data set 1 and 14.7 years in data set 2.
We selected participants from the Multicenter AIDS Cohort Study (MACS), a study of the natural and treated history of HIV-1 infection in men who have sex with men.
Aging is associated with an increasing incidence of chronic, debilitating, diseases. While cardiovascular, skeletal, and neurodegenerative diseases are widely known and discussed in the general population, there is virtually no organ or tissue system that is not at risk.
Together, this data supports the theory that aging within the immune system plays an important role in aging of the overall organism, and our methylation data suggests that HIV-1 infection may be accelerating this process using similar mechanisms....the researchers suggest that HIV itself accelerates these aging related changes by more than 14 years......These results are an important first step for finding potential therapeutic approaches to mitigate the effects of both HIV and aging......our data show that the effects of HIV-1 infection at a subset of methylation sites appear to be additive with the effects of aging.
we were most surprised that the data suggests HIV-infection can accelerate aging-related epigenetic changes by 13.7 to 14.7 years," said Beth Jamieson, professor of medicine in the division of hematology/oncology at the David Geffen School of Medicine at UCLA and one of the study's senior authors. "This number is in line with both anecdotal and published data suggesting that treated HIV-infected adults can develop the diseases of aging mentioned above, approximately a decade earlier than their uninfected peers.".
Antiretroviral Therapy Does Not Dial Back Advanced Epigenetic Age With HIV
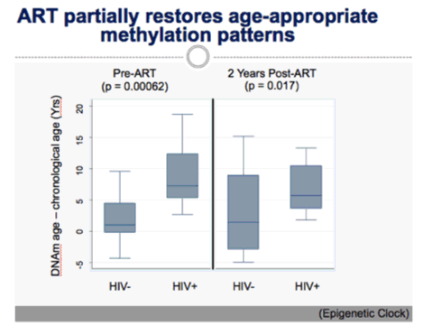
According to the epigenetic clock, men with untreated HIV infection had a DNA methylation age about 8 years older than their chronological age (P = 0.00062). When these men started ART, treatment did not restore an age-appropriate DNA methylation age. After 2 years of ART, about 6 years still separated epigenetic age from chronological age (P = 0.017).
Before they began ART, men with HIV had higher levels of total, senescent, terminally differentiated, and activated CD8 cells than HIV-negative men. These CD8-cell subsets were significantly associated with DNA methylation age. Even after 1 and 2 years of ART, all four CD8-cell subsets remained elevated compared to the HIV-negative group, and all remained significantly associated with DNA methylation age.
Methylome-wide Analysis of Chronic HIV Infection Reveals Five-Year Increase in Biological Age and Epigenetic Targeting of HLA
"our study provides a robust estimate of a 5-year age advancement in HIV/cART individuals....increasing expected mortality risk by 19%”
For uninfected controls, the calculated biological age had a very highconcordance with chronological age (Figure 2D, Pearson’sr= 0.94). In contrast, the HIV+ patients had a biological ageadvancement of 4.9 years on average (p < 10_8by Student’s ttest, 95% confidence interval 3.4-7.1 years,Figures 2E and2F). These results were consistent with our previous unsuper-vised analysis (Figures 1B and 1C) in suggesting that HIV infection leads to advanced aging. Furthermore, we found that theage advancement of HIV+ individuals was negatively correlatedwith the ratio of CD4+/ CD8+T lymphocytes (Spearman’s rho =_0.2, p < 0.02).
we found that the amount ofmethylation at this gene was correlated with a patient’s CD4+/CD8+T cell ratio (Figure S6). Taken together, these results indi-cate that the HLA locus is likely differentially methylated acrossblood cell types and also changes within individual cell types inresponse to HIV.
These findings support a link between HIV infection and aging (Rickabaugh et al., 2015), as quantitatively measured by epigenomic profiling (Figure 1D).......patients more recently infected with HIV (<5 years) had no significant difference in age advancement from those patients with chronic (>12 years) infection----These findings lend support to the theory that age advancement occurs early in the course of disease as a consequence of acute infection or reaction to drug treatment.....we found that the age advancement of HIV+ individuals was negatively correlated with the ratio of CD4+ / CD8+ T lymphocytes......we had observed multiple effects of HIV on the methylome including changes in cellular composition, age advancement, and a general increase in methylome disorder. These differences might be particularly pronounced in HIV-infected patients, some of whom have low CD4+ T cell counts...
Inability of ART to restore age-appropriate epigenetic patterns in HIV-infected adults
these data suggest that HIV-induced age-acceleration, partially mediated through epigenetic changes, may be directly associated with the earlier functional and clinical decline observed in virally suppressed HIV-infected adults on ART.....We previously documented that untreated HIV-infected adults have DNA methylation patterns that predict their epigenetic age to be 14 years older than their chronologic age, suggesting that HIV-infection accelerates at least some of the underlying mechanisms of aging (Rickabaugh et al. PLoSOne 2015). However, as it is HIV-infected adults on ART who are at increased risk for clinical and functional outcomes of aging, we hypothesized that ART initiation does not restore HIV-perturbed epigenetic patterns to age-appropriate levels, and that DNA methylation ages stay advanced in treated HIV-infected adults compared to chronologically age matched-controls.
Epigenetic Clock analysis revealed that untreated HIV-infection was associated with an accelerated DNAm age of ∼8 years (p = 0.00062). Untreated HIV-infection was also associated with an increase in total, senescent, terminally differentiated, and activated CD8+ T-cells and those subsets were significantly associated with DNAm. ART was unable to restore DNAm age to age-appropriate levels (p = 0.017) and all four CD8+ T-cell subsets remained elevated and significantly associated with DNAm age.
Perinatally acquired HIV infection accelerates epigenetic aging in South African adolescents
These findings suggest that an epigenetically older immune system is associated with lower cognitive functioning. Despite a mean age of initiation of ART treatment of 3.4 years and usage for more than 7 years, considerable cognitive impairment is apparent.
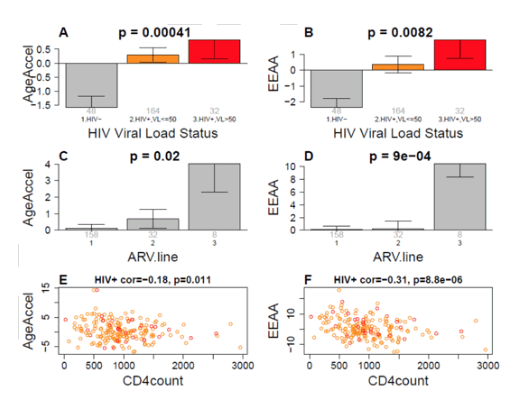
In a recent large scale meta-analysis involving over 13 thousand subjects from 13 cohorts, we have shown that both AgeAccelerationResidual and EEAA are predictive of mortality, independent of chronological age, even after adjusting for additional risk factors, and within the racial/ethnic groups that we examined (Caucasians, Hispanics, African Americans) [32].
we recently found evidence that HIV infection is associated with accelerated epigenetic aging based on the epigenetic clock[15] in both brain and peripheral blood mononuclear cells [10]. That is, brains of adults infected with HIV demonstrated age acceleration of 7.4 years compared to uninfected controls, and 5.2 years in peripheral blood mononuclear cells, findings that have been validated by other groups[12-14]. Furthermore, we have found that accelerated epigenetic aging can be observed in brain tissue samples of adults diagnosed pre-mortem with HIV-associated neurocognitive disorders (HAND) [16].
Our analysis of ART line (first/second/third) (variable ARV.line) reveals that adolescents who are on second or third line ART treatment are more likely to have accelerated ageing (Figure 1C,D).
Both AgeAccelerationResidual and EEAA remain significantly associated with current CD4 T cell counts and ARV.line even after adjusting for viral load, educational status, ethnicity, and other potential confounders (Table 2).
EEAA is significantly associated with overall cognitive impairment status (Figure 2A), and more specifically with the following cognitive domains: attention, working memory, executive functioning, and processing speed (Figure 2B-E).
This is the first study to show that a) perinatally acquired HIV infection is associated with epigenetic age acceleration in blood, and b) extrinsic epigenetic age acceleration is associated with lower cognitive functioning in these adolescents. The study took place in South Africa, one of the countries most affected by HIV/AIDS with the highest rate of new HIV infections in the world. Despite a mean age of initiation of ART treatment of 3.4 years and usage for more than 7 years, considerable cognitive impairment is apparent.
Epigenetic Age Acceleration and Non-AIDS Defining Cancers Among HIV Infected Adults
Cross sectional studies have observed epigenetic age acceleration for those with HIV both on and off ART compared to uninfected individuals; however, we don't know whether epigenetic age acceleration is associated with age related diseases such as cancer among those with HIV or ultimately if these biomarkers could be used to predict disease in this population.
The majority of both cases and controls were on ART with suppressed viral load at the time of sampling and similar high proportion of current smokers.
This table describes our primary study results and main findings of associations between 5-year epigenetic age acceleration measures and these two types of cancer. First, you can see that we did not find any significant associations between these epigenetic age measures and anal cancer. For lung cancer only GrimAge Acceleration was significantly associated with 316% greater odds per 5-year increase in age acceleration.
Reversal of epigenetic aging and immunosenescent trends in humans
we conducted what may be the first human clinical trial designed to reverse aspects of human aging, the TRIIM (Thymus Regeneration, Immunorestoration, and Insulin Mitigation) trial, in 2015-2017. The purpose of the TRIIM trial was to investigate the possibility of using recombinant human growth hormone (rhGH) to prevent or reverse signs of immunose‐nescence in a population of 51‐ to 65‐year‐old putatively healthy men, which represents the age range that just precedes the col‐lapse of the TC.
rhGH was used based on prior evidence that growth hormone (GH) has thymotrophic and immune reconstituting effects in animals (Kelley et al., 1986) and human HIV patients (Napolitano et al., 2008; Plana et al., 2011)
|
|
| |
| |
|
|
|