| |
Cognitive disorders in people living with HIV
|
| |
| |
Download the PDf here
Lancet HIV July 2020
Alan Winston, Serena Spudich
Pathogenesis and contributing factors:
Legacy effects from HIV and its complications, Neuroinflammation, Antiretroviral toxicities, Ageing and comorbidities, Lifestyle factors, Cerebrospinal fluid HIV RNA escape and HIV persistence
Potential causes of cognitive impairment in effectively-treated people with HIV are described, highlighting the contribution of HIV-related factors as well as lifestyle factors.
Abstract
High rates of cognitive disorders in antiretroviral-treated people living with HIV have been described worldwide. The
exact prevalence of such cognitive disorders is determined by the definitions used, and the presence of these cognitive
disorders significantly impacts the overall wellbeing of people with HIV. With the cohort of people with HIV becoming
increasingly older, and having high rates of comorbidities and concomitant medication use, rates of cognitive
disorders are likely to increase. Conversely, interventions are being sought to reduce the size of the latent HIV
reservoir. If successful, such interventions are likely to also reduce the HIV reservoir in the brain compartment,
which could result in improvements in cognitive function and reduced rates of impairment.
Conclusions
Challenges remain in defining, understanding, and treating cognitive dysfunction in people with HIV on ART. Cognitive impairment in the setting of well treated HIV is heterogeneous, and can be due to either or both legacy effects and active processes. In order to optimally develop effective therapies to improve symptoms, it is necessary to differentiate prior versus progressive injury. Clinical trials may need to define so-called biotypes of cognitive impairment on the basis of clinical assessments as well as other biomarkers for correct aetiological diagnosis. Additionally, systemic and central nervous system disease are linked, such that in most cases targeted CNS therapy is probably not necessary and systemic management is sufficient. Exceptions include cases of cerebrospinal fluid HIV RNA escape, where adjustment of ART to address antiretroviral drug resistance or inadequate drug efficacy in the CNS appears to be important. Early initiation of ART may protect the brain, however just how early is necessary remains unknown. The extent to which HIV persistence (latent or active infection) in the CNS relates to clinical symptoms and might present a barrier to HIV cure efforts is uncertain.
Despite these challenges, it is clear that virologically suppressive ART and optimisation of confounding conditions (such as treatment of mood disorders and reduction of lifestyle factors that worsen cognition) are key aspects of clinical management of cognitive impairment in people with HIV. Additionally, investigation and clinical trials of cognitive impairment in under-resourced settings, where the burden of HIV worldwide is highest, and demographics, lifestyle factors, and treatment options might be different from well-resourced settings that have generated most existing data, is an emerging priority.
• neuroinflammation could be causing persistent damage, and could result in an accelerated decline in cognitive performance.
• How the ageing process will affect people with HIV and how such effects will impact on cognitive performance over time is an area of controversy. Another area of debate is whether an accelerated ageing phenotype exists in people with HIV on ART. With regards to cognitive performance and the context of an accelerated ageing phenotype, the question is whether the natural decline in cognitive performance observed with ageing, is more marked, or accelerated, in people with HIV than in the general population. Some longitudinal studies have suggested an accelerated cognitive ageing phenotype to be present in people with HIV,52, 53, 54 with other studies suggesting that age-related cognitive decline is similar in people with HIV and lifestyle-similar controls.55
• Differences in the characteristics of the cohorts and study design might explain these inconsistencies, with further longitudinal studies with closely and carefully matched control groups required to evaluate this important question.
• mood disorders might relate to historical events such as childhood trauma and violence, and a history of post-traumatic stress disorder, rates of which may be higher in people with HIV.....a close association between depressive symptoms and overall cognitive function.
• The clinical penetration effectiveness score is a pharmacokinetic and pharmacodynamic scoring system, which rates antiretroviral agents based on their hypothetical antiviral activity in the central nervous system. 72
• Although in principle, pharmacokinetic and pharmacodynamic scoring systems are of interest, the evidence base to determine ART for an individual on the basis of such scoring systems is lacking, and basic evidence-based principles for determining optimal ART should always prevail.
• In addition to antiretroviral management, consideration should also be given to the optimal management of other non-infectious comorbidities and depressive conditions when optimising treatment for people with HIV with cognitive disorders.
• Commencing ART early will reduce the duration of time that the brain tissue is exposed to uncontrolled HIV replication, and therefore might reduce CNS damage, neuroinflammation, and potentially rates of cognitive disorders.
• Risk factors for cerebrospinal fluid HIV RNA escape include a prior history of antiretroviral drug resistance, which can lead to ART treatment failure in the CNS compartment, often without evidence of such failure in the plasma compartment, and a low nadir CD4 lymphocyte count.
• it is unclear whether interventions to study HIV cure could be injurious for the brain, given the specific risks of inflammation, neuronal injury, and viral escape in the CNS compartment. ART treatment interruption, undertaken to assess the impact of therapeutic interventions on the potential of ART-free remission, is particularly controversial, since old studies of prolonged interruption showed biomarker evidence of inflammation and injury in the CNS. 80 However, modern interventions typically involve brief and tightly monitored ART interruption, which might not have such deleterious effects in the brain.81
• While varied methods have demonstrated HIV DNA in the cerebrospinal fluid and brains of people with HIV on suppressive ART, it is uncertain whether these virions are capable of replication, and thus able to serve as a source of HIV rebound that would prevent HIV remission if not directly eliminated.
Pathogenesis and contributing factors
Legacy effects from HIV and its complications
Advances in HIV management over the past 20 years have been unprecedented. Prior to these advances, people with HIV experienced many conditions which may have had long-term effects on brain health, such as clinically evident AIDS-defining CNS infections and cancers, and toxicities from the initial generations of antiretroviral drugs. Additionally, processes associated with cognitive disorders in HIV, including neuroinflammation,24, 25 brain atrophy,26, 27 and injury to neurons, as detected via the cerebrospinal fluid and neuroimaging,28 can be initiated and progressively worsen during early untreated HIV infection. While these processes appear to be attenuated once ART is started and viral suppression is achieved, the lengthy duration of HIV infection in many people with HIV prior to initiation of therapy might lead to a subtle but lasting neural dysfunction. Although these legacies are not ongoing or necessarily progressive during modern stable treatment regimens, the resultant detrimental effects on cognitive reserve, which does not recover, may be apparent several decades later. For individuals who have experienced these so-called legacy effects and therefore have a reduced cognitive reserve, current insults to the CNS, including natural changes with ageing, might have a greater impact (figure).
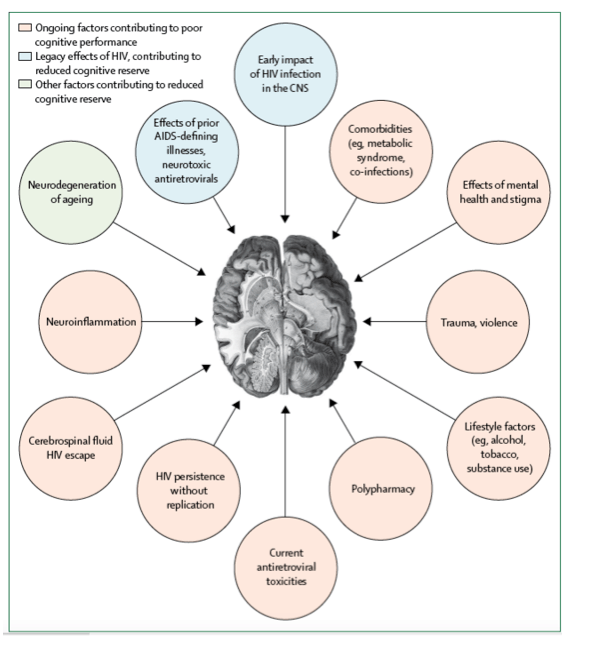
Neuroinflammation
Activation of the innate and adaptive immune systems, immunosenescence, and chronic inflammation are widely reported features of ART-treated HIV disease. 29 This persistent immune activation and inflammation in people with HIV on otherwise suppressive ART is postulated to be a major driver of many age-related non-infectious comorbidities, and a major driver of cognitive disorders.
Activated immune cells, some of which are HIV-infected, invade the CNS and can result in neuroinflammation and propagation of HIV infection to resident cells within the brain and adjacent nervous system tissues. Elevated concentrations of soluble markers of monocyte activation and inflammation in the cerebrospinal fluid in people with HIV on suppressive ART provides evidence of such neuroinflammation. 30 The association between elevated concentrations of inflammatory markers and cognitive impairment in people with HIV on ART suggests that cognitive disorders might be in part a consequence of persistent neuroinflammation despite ART.31 Imaging studies utilising PET have also suggested increased binding of PET ligands, which bind to activated microglial cells, in otherwise effectively treated people with HIV, and suggested an association between increased microglial activation in some brain regions and reduced performance on cognitive tests.32, 33 Unlike the legacy effects of HIV, which are unlikely to be causing progressive damage to the CNS or progressive cognitive decline, neuroinflammation could be causing persistent damage, and could result in an accelerated decline in cognitive performance.
Antiretroviral toxicities
Given the sharp decline in frank HIV-dementia since the availability of virologically effective ART, there can be little doubt that, in general, ART is beneficial with regard to cognitive function and brain health in people with HIV on a population level. Nonetheless, several antiretroviral drugs have known central nervous system toxicities that might have an impact on cognitive health.
The non-nucleoside reverse transcriptase inhibitor efavirenz has a wide array of neuropsychiatric side effects, with effects on sleep, abnormal dreams, and anxiety recognised early in the drug's development as being associated with the drug.34 Awareness of these toxicities allowed clinicians to inform people with HIV commencing efavirenz of these frequently observed adverse events. It was not until several years later that studies reported poorer cognitive performance in cohorts of people with HIV receiving efavirenz-based ART than those on other regimens.35 Improvement in cognitive function has been observed in people with HIV who have ceased taking efavirenz-based ART.36, 37
Neuropsychiatric side effects are reported with the integrase-strand transfer inhibitors. These neuropsychiatric side-effects differ markedly in several aspects from the adverse events reported with efavirenz. First, during the licensing studies no specific neuropsychiatric toxicities were observed with these drugs, with reports instead occurring in postlicensing cohort data.38 Why such effects were not apparent in phase 3 development programmes is unclear, but might be due to differences in the characteristics of participants who enter drug development programmes compared with the characteristics of the wider population of people with HIV, or due to a lack of ascertainment of such toxicities in phase 3 programmes. Second, unlike efavirenz, the integrase-strand transfer inhibitor toxicities are not apparent in most individuals, but rather only in specific at-risk populations, such as those with underlying depression or anxiety, and older individuals. This could also help explain why these adverse events were not observed within the clinical trials, as this phenotype of participant might have been less likely to enter a clinical trial (the predominant phenotype of people with HIV in drug development studies has traditionally been young white men). Third, the reported toxicities from integrase-strand transfer inhibitors are predominantly insomnia and anxiety, with no reports thus far describing a specific effect on cognition. However, vigilance for potential effects of the integrase-strand transfer inhibitors on cognitive performance would be prudent, given it took several years to recognise such an effect from efavirenz use.
In addition to clinical evidence of CNS toxicities caused by antiretroviral drugs outlined previously, laboratory and imaging studies have suggested potential mechanisms whereby antiretroviral drugs could have neuronal toxicities. Neuronal cell culture studies have observed toxicities from several of the antiretroviral drugs in current clinical use.39 Potential proposed toxicities include mitochondrial toxicities and direct neuronal toxicities. MRI spectroscopy and functional imaging studies have also provided insight into potential toxicities, with reductions in neuronal integrity metabolites observed in people with HIV receiving older nucleoside reverse transcriptase inhibitors on spectroscopy, and differing effects on blood oxygen dependent contrast between different antiretroviral combinations on functional MRI.40
Cerebrospinal fluid HIV RNA escape and HIV persistence
With modern antiretroviral regimens, suppression of plasma HIV RNA is achievable in most treated individuals. Systemic ART is also very effective at suppressing HIV RNA in other body compartments, including suppressing cerebrospinal fluid HIV RNA. However, rarely, cerebrospinal fluid HIV RNA can be detectable when plasma HIV RNA is not detectable, or cerebrospinal fluid HIV RNA levels might be greater than plasma HIV RNA ones. This scenario is generally termed cerebrospinal fluid HIV RNA escape. 41, 42
In cases where detectable cerebrospinal fluid HIV RNA is an incidental finding, a conservative approach is generally recommended, with ongoing clinical monitoring of the individual to ensure symptoms do not develop. Such scenarios would include people with HIV, who are otherwise asymptomatic, undergoing lumbar puncture examination for research programmes.
In the context of symptomatic individuals, and, of relevance here, in individuals with new or worsening cognitive symptoms, cerebrospinal fluid HIV RNA should generally not be ignored, with detailed management described later on.
Risk factors for cerebrospinal fluid HIV RNA escape include a prior history of antiretroviral drug resistance, which can lead to ART treatment failure in the CNS compartment, often without evidence of such failure in the plasma compartment, and a low nadir CD4 lymphocyte count. It is plausible that advanced immunosuppression and prolonged untreated HIV results in more extensive CNS HIV infection and inflammation, which could lead to compartmentalised replication and emergence of drug resistance during ART. The exposure and effect of antiretroviral drugs within sanctuary sites of the body might also have impact on cerebrospinal fluid escape. Indeed, reports have described the use of ART regimens containing boosted protease inhibitors as a significant risk factor for cerebrospinal fluid HIV RNA escape.43 Boosted protease inhibitors have a relatively low cerebrospinal fluid inhibitory quotient (concentration of free drug compared to the inhibitory concentration required to suppress HIV replication) providing credence to this hypothesis. However, it should be noted that ART regimens based on boosted protease inhibitors are generally reserved for people with HIV with drug-resistant HIV strains, and teasing out whether it is the presence of HIV drug resistance, or pharmacokinetic and pharmacodynamics drivers that cause the cerebrospinal fluid HIV RNA escape is challenging.
More recently, detection of HIV infected cells44 and HIV proteins 45 in cerebrospinal fluid from people with HIV on sustained effective ART has been associated with reduced cognitive performance, although further studies are needed to determine whether HIV persistence in the CNS without viral replication is causally related to ongoing cognitive impairment.
Lifestyle factors
Factors that might predispose to cognitive disorders, particularly cigarette smoking, substance abuse, and alcohol misuse, are highly prevalent in people with HIV. Over the past 10 years, substantial changes in recreational drug use have been seen, especially in men who have sex with men, including so-called chemsex, which refers to drug use to facilitate sexual intercourse and includes the use of mephedrone and crystallised methamphetamine. 46 Not only can substance use directly affect cognitive health via the direct toxicities to the CNS, but also via pharmacological interactions with antiretroviral drugs and concomitant medication.
Ageing and comorbidities
Many cohort studies have reported the prevalence of non-infectious comorbidities to be more highly prevalent in people with HIV than those without HIV, even when compared with lifestyle-similar HIV-negative controls.12 It is well documented in the literature that the presence of non-infectious comorbidities can impact negatively on cognitive function, with this observation replicated in HIV cohorts.47 Infectious comorbidities are also more frequent in people with HIV, including sexually transmitted infections. Cytomegalovirus,48 syphilis,49 and Mycobacterium tuberculosis50 infection have each been associated with poorer cognitive function, although whether this association results from direct effects of pathogens, immune responses, or unrecognised factors that increase risk of coinfections and cognitive impairment is unknown.51
How the ageing process will affect people with HIV and how such effects will impact on cognitive performance over time is an area of controversy. Another area of debate is whether an accelerated ageing phenotype exists in people with HIV on ART. With regards to cognitive performance and the context of an accelerated ageing phenotype, the question is whether the natural decline in cognitive performance observed with ageing, is more marked, or accelerated, in people with HIV than in the general population. Some longitudinal studies have suggested an accelerated cognitive ageing phenotype to be present in people with HIV,52, 53, 54 with other studies suggesting that age-related cognitive decline is similar in people with HIV and lifestyle-similar controls.55
Differences in the characteristics of the cohorts and study design might explain these inconsistencies, with further longitudinal studies with closely and carefully matched control groups required to evaluate this important question.
The management of older individuals with multiple comorbidities often involves polypharmacy. Cognitive decline associated with concomitant medication use and polypharmacy is well described, and is probably an important factor driving cognitive disorders in older people with HIV.56
Different concomitant medications can have differing impacts on cognitive performance, with data suggesting anticholinergic, anxiolytic, anticonvulsant, and opioid medication has a greater impact than other types of medication.57
Mental health and stigma
High rates of depression and other mental health conditions have been described in people with HIV since the start of the epidemic. Prior to the advent of effective ART, with the very poor prognosis associated with HIV disease, such high rates of depression were not unexpected. However, why such high rates of depression continue to exist in people with HIV with otherwise effectively treated HIV disease remains unclear. Potential explanations include heightened rates of mood disorders in individuals at risk of acquiring HIV; living with a medical condition that remains highly stigmatised, with this stigma manifesting clinically as anxiety and depression; the neuropsychiatric toxicities of ART, manifesting as depressive symptoms; and residual or progressive neuroinflammation leading to depressive symptoms. For some individuals, the heightened rates of mood disorders might relate to historical events such as childhood trauma and violence, and a history of post-traumatic stress disorder, rates of which may be higher in people with HIV. 58
Whatever the underlying pathogenesis of depression and other mental health conditions in people with HIV, these conditions are probably relevant when considering cognitive disorders. Depression can manifest as concentration difficulties and significantly affect overall cognitive performance. Over recent years, the impact of mental health on cognitive health has gained increasing attention, with several studies clearly describing a close association between depressive symptoms and overall cognitive function.
51
Management
ART is the mainstay of treatment for cognitive disorders in HIV. Clinical trials of adjunctive therapeutic interventions, intended to reduce cognitive impairment in people with HIV, have in general shown no effect to date (table 2). As highlighted in table 2, adjunctive therapies that have been trialled have had several mechanisms of action, highlighting the lack of an individual known pathogenic mechanism underlying cognitive disorders in people with HIV.
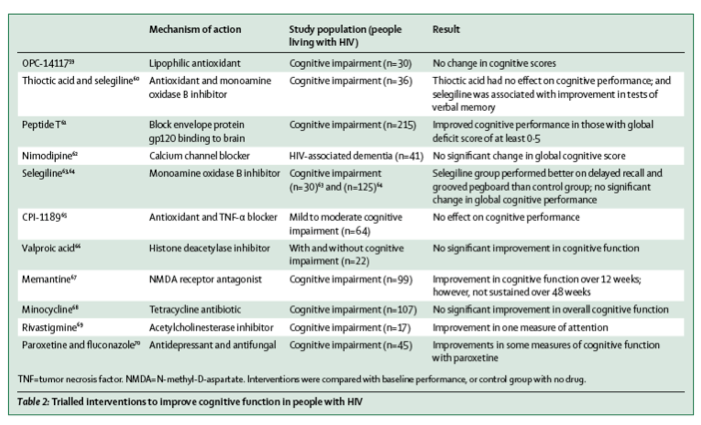
Several randomised clinical trials of interventions to improve cognition in people with HIV on ART are underway, investigating the effects of ART intensification with maraviroc and dolutegravir (NCT02519777), adjunctive therapy with tesamorelin to address metabolic abnormalities (NCT02572323), and adjunctive therapy with intranasal insulin as a neuroprotective agent (NCT03081117 and NCT03277222). To date, however, the evidence base is lacking and no specific proven intervention for the management of cognitive disorders in people with HIV exists. Thus, management is based on best clinical practice, with several important strategies for consideration.
Management of cerebrospinal fluid HIV RNA escape is an example of an important strategy. Although the evidence is from case series and case reports, it suggests active management of cerebrospinal fluid HIV RNA in neurologically symptomatic individuals can result in substantial clinical improvement. 71
Management comprises of modification of ART on the basis of both historical and current HIV resistance test results from the plasma and cerebrospinal fluid. Given this syndrome is manageable, with evidence for clinical improvement ensuing from active management, the important message is to always actively assess for cerebrospinal fluid HIV RNA escape with cerebrospinal fluid sampling.
Other antiretroviral strategies include assessing and reviewing for toxicities. Individuals on efavirenz-containing ART without other explanations for the cognitive symptoms should be switched to other ART regimens, and vigilance for emerging toxicities from newer antiretroviral agents and classes is required.
In any Review of cognitive disorders in people with HIV, the clinical penetration effectiveness score needs to be mentioned. The clinical penetration effectiveness score is a pharmacokinetic and pharmacodynamic scoring system, which rates antiretroviral agents based on their hypothetical antiviral activity in the central nervous system. 72
Although in principle, pharmacokinetic and pharmacodynamic scoring systems are of interest, the evidence base to determine ART for an individual on the basis of such scoring systems is lacking, and basic evidence-based principles for determining optimal ART should always prevail. Such principles include using guideline-based ART regimens, as these are the regimens with the greatest evidence base, and regimens based on HIV drug resistance testing.
In addition to antiretroviral management, consideration should also be given to the optimal management of other non-infectious comorbidities and depressive conditions when optimising treatment for people with HIV with cognitive disorders.
Prevention of cognitive disorders
Several of the risk factors for cognitive disorders in people with HIV are avoidable or could be reduced. Regarding the legacy effects of HIV disease, such risk factors are likely to decline in future years. ART is now recommended for all people with HIV, irrespective of disease status or CD4 lymphocyte measurements. Commencing ART early will reduce the duration of time that the brain tissue is exposed to uncontrolled HIV replication, and therefore might reduce CNS damage, neuroinflammation, and potentially rates of cognitive disorders. Benefit of ART irrespective of CD4 lymphocyte count was observed within the Strategic Timing of Antiretroviral Therapy study. 73
Although a neurology substudy of this research did not observe cognitive benefits in patients randomly assigned to immediately commence antiretroviral therapy, such potential benefits could have been mitigated by the majority of participants in the primary study receiving efavirenz-based combination ART regimens (whereby efavirenz use could have mitigated cognitive benefits).74
Some recent studies, designed to examine rates of cognitive impairment in people with HIV starting ART early after acquisition of HIV, have suggested rates of cognitive impairment to be similar to the rate in people without HIV.75, 76
Important questions here are how early is early enough, in terms of starting ART, to gain this potential benefit, and whether these findings are durable after many years of ART treatment, which will require additional studies with extended follow-up. Widespread so-called immediate ART treatment schemes, based on likely clinical and public health benefits of starting ART as early as possible after HIV diagnosis,77 might additionally benefit the brain, especially in individuals identified with acute or recent HIV infection. However, adherence in vulnerable populations started on ART through such programmes will be of critical importance as a determinant of long-term cognitive outcomes.
Future considerations
HIV cure, encompassing HIV eradication (complete elimination of all latent HIV within the host) or the more realistic goal of remission (ability to maintain plasma viral load below the limit of detection without ART), is a desirable goal for people with HIV, given current lifelong challenges of medication adherence, non-AIDS related comorbidities, and stigma, even in those with access to antiretroviral treatment who achieve optimal immune recovery. Controversy exists as to whether the CNS is a barrier to HIV cure efforts, perhaps requiring specific approaches that effectively target the CNS, in addition to systemic sites of HIV latency.78, 79
While varied methods have demonstrated HIV DNA in the cerebrospinal fluid and brains of people with HIV on suppressive ART, it is uncertain whether these virions are capable of replication, and thus able to serve as a source of HIV rebound that would prevent HIV remission if not directly eliminated.
Similarly, it is unclear whether interventions to study HIV cure could be injurious for the brain, given the specific risks of inflammation, neuronal injury, and viral escape in the CNS compartment. ART treatment interruption, undertaken to assess the impact of therapeutic interventions on the potential of ART-free remission, is particularly controversial, since old studies of prolonged interruption showed biomarker evidence of inflammation and injury in the CNS.80
However, modern interventions typically involve brief and tightly monitored ART interruption, which might not have such deleterious effects in the brain. 81
|
|
| |
| |
|
|
|