 |
 |
 |
| |
COVID-19 in the Largest US HIV Cohort
|
| |
| |
IAC2020

https://events.ugovirtual.com/event/AIDS2020/en-us#!/Auditorium
abstract
BACKGROUND: Immunocompromised persons are at higher risk of poorer SARS-CoV-2/coronavirus disease 2019 (COVID-19) outcomes. The CDC considers persons with HIV (PWH) a special high-risk population and stated, 'at present time, we have no specific information about the risk of COVID-19 in [PWH]'.1 We examined COVID-19 testing and outcomes in PWH and uninfected persons in the Veterans Aging Cohort Study (VACS), the largest cohort of PWH in the United States.
METHODS: VACS is an open cohort of all Veterans with HIV and 1:2 age-, race/ethnicity-, sex-, and site-matched uninfected Veterans. We extracted COVID-19 laboratory testing results and diagnoses reported through May 17, 2020 and linked demographics, outpatient/inpatient encounters, diagnoses, procedures, health behaviors, and pharmacy records from Veterans Health Administration (VA) electronic health records. Baseline was defined as date of specimen collection, hospital admission, or reported external testing. We estimated associations between baseline characteristics and testing COVID-19-positive (COVID-19+) with logistic regression and associations between HIV and severe COVID-19 (i.e., intensive care, intubation, or death) with Cox regression.
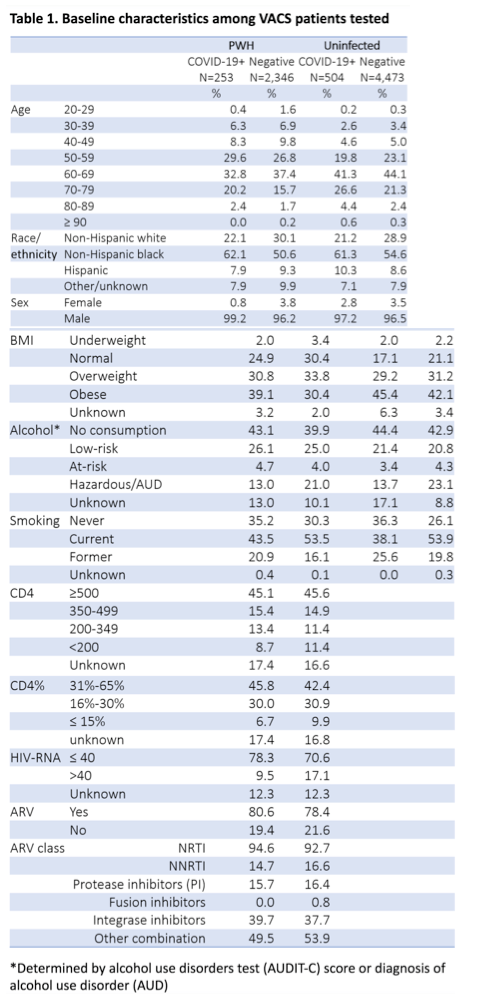
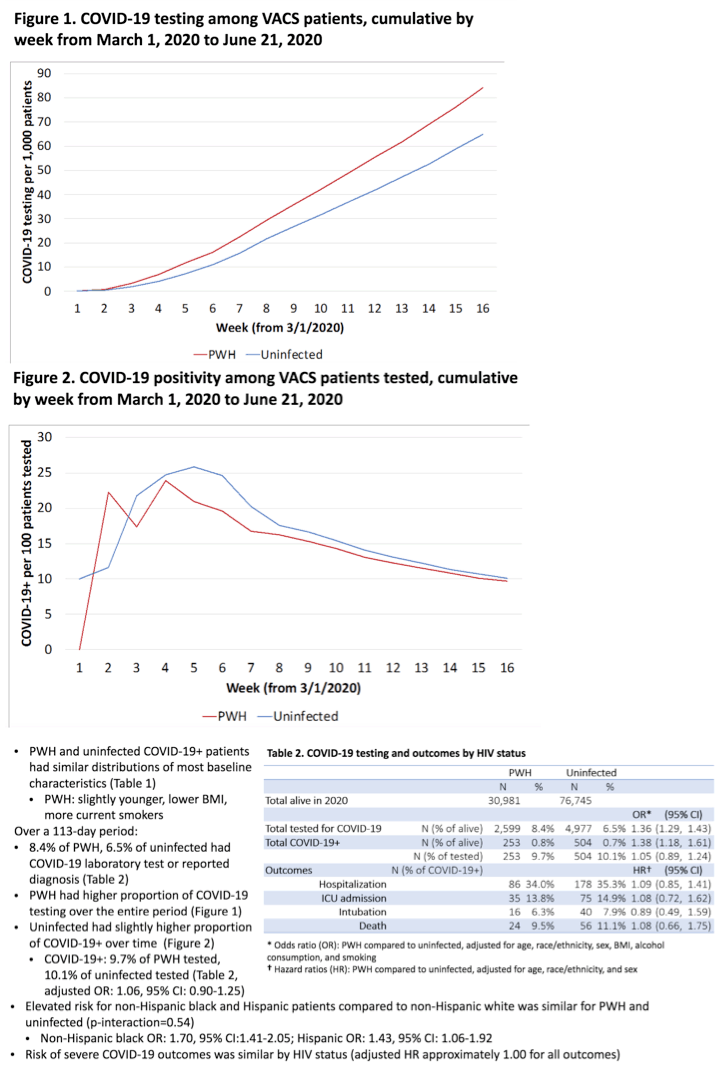
RESULTS: Among VACS participants alive in 2020 (30,948 PWH, 76,618 uninfected), 4.8% of PWH and 3.6% of uninfected engaged in COVID-19-related VA care (Figure 1). Over a 78-day period, 189 PWH (12.7% of tested) and 380 uninfected (13.9%) were diagnosed with COVID-19 (Table 1, adjusted odds ratio [OR]: 1.04, 95% CI: 0.85-1.26). PWH and uninfected COVID-19+ patients had similar distributions of baseline characteristics. Elevated risk for non-Hispanic black (OR: 1.87, 95% CI:1.49-2.36) and Hispanic (OR: 1.57, 95% CI: 1.11-2.22) patients compared to non-Hispanic white was similar for PWH and uninfected (p-interaction=0.47). Risk of severe COVID-19 outcomes was similar by HIV status (adjusted hazard ratios were approximately 1.00 for all outcomes).
CONCLUSIONS: While PWH have higher testing rates, thus far, we have not found evidence of increased burden of positivity among those tested, nor an increased risk of severe COVID-19 outcomes by HIV status. Due to testing shortages and potential for differential adherence to stay-at-home guidance by immunosuppression status, we should continue to monitor testing, positivity, and COVID-related health outcomes. Additionally, potential linkages between antiretroviral treatment and CD4 count with COVID-19 severity and progression needs investigation.


|
| |
|
 |
 |
|
|