 |
 |
 |
| |
Reducing ART to less than 3-ARV regimen linked to increased systemic inflammation
|
| |
| |
Sergio Serrano-Villar
IAC 2020 Virtual
Reported by Jules Levin
On behalf of all co-authors: María Rosa López-Huertas, Félix Gutiérrez, Manuela Beltrán, Mario Pons, Pompeyo Viciana, Joaquín Portilla, Federico García, Santiago Moreno, and CoRIS (Spanish AIDS Cohort)
ABSTRACT
BACKGROUND: We assessed the long-term consequences of changing triple therapy (3DR) to 2-drug regimens (2DR) or PI-based monotherapy (1DR) on virological failures, clinical events, and systemic inflammation.
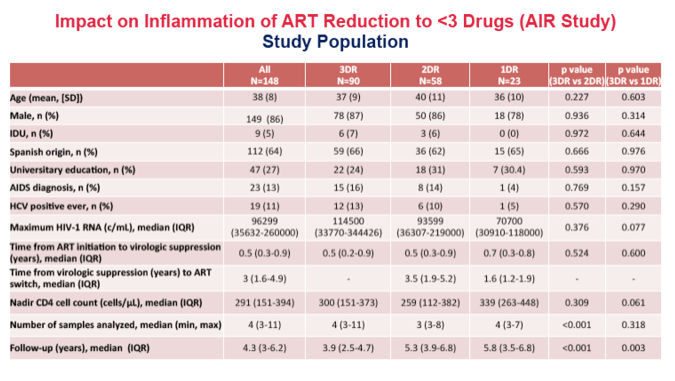
METHODS: We selected ART-naive patients initiating triple ART from 2004 to 2018 in the Spanish AIDS Research Network (CoRIS) who achieved virologic suppression (VS) in the first 48 weeks of ART and either remained on 3DR or were switched to 2DR (3TC+bPI; 3TC+DTG; DTG+RPV, CAB+RPV) or 1DR (bDRV or bLPV). We calculated cause-specific cumulative incidence curves and used multivariate Cox proportional hazards models adjusted for potential confounders to estimate hazard ratios for the endpoints: 1) severe non-AIDS events (NAE), 2) AIDS or AIDS-related death, 3) all-cause death, 4) virological failure, 5) composite endpoint of virological failure/serious NAE/death. In a nested study, we compared IL-6, CRP, D-dimers and IFABP trajectories during VS using multivariate mixed models and linear splines.
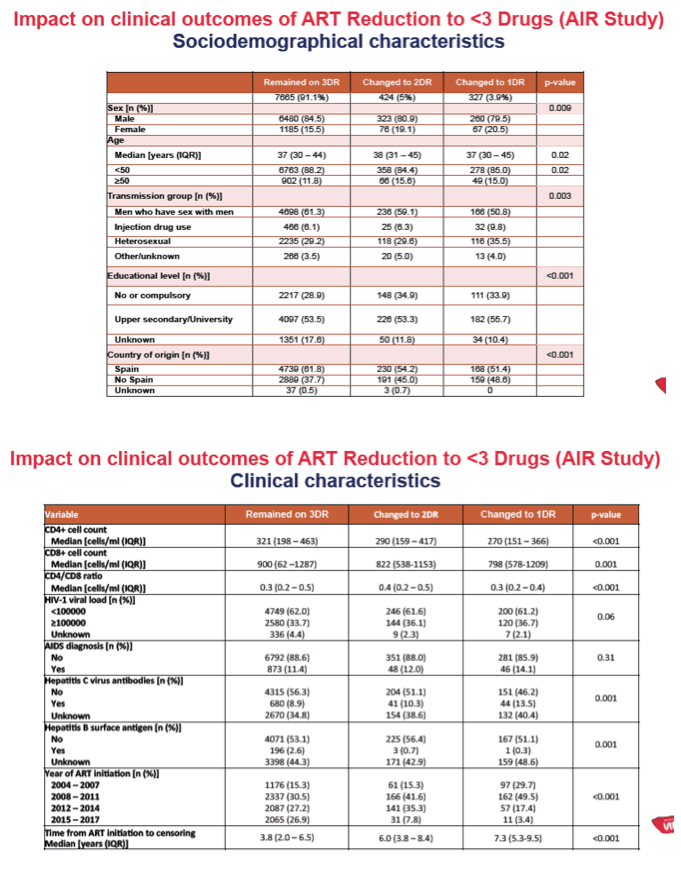
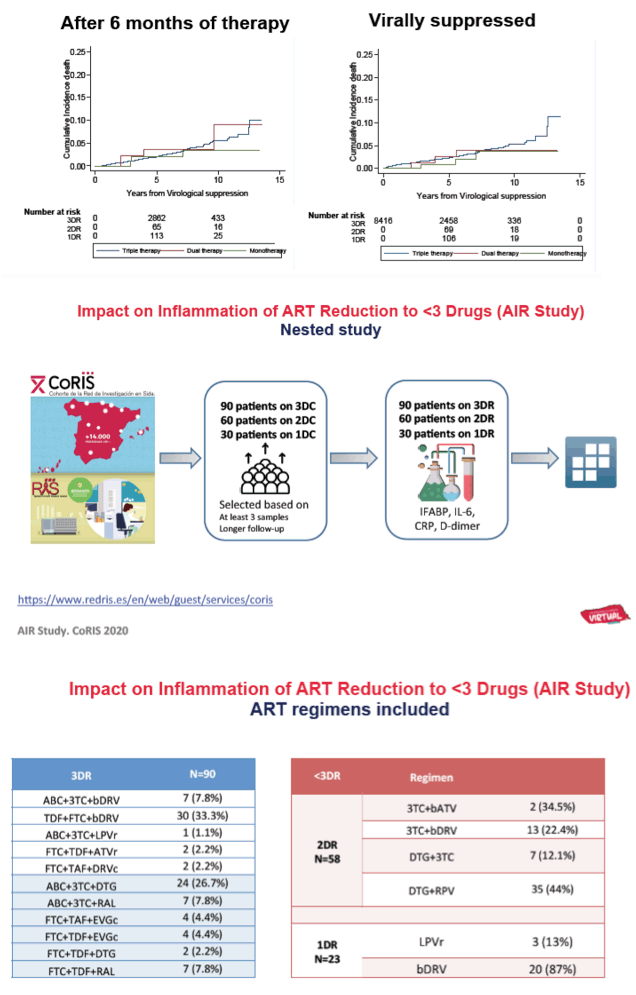
RESULTS: From 14458 patients, 8416 met the inclusion criteria; 7665 remained on 3DR, 424 switched to 2DR and 327 to 1DR. The median time from enrolment to censoring was 4.9, 6.9 and 8.4 years in the 3DR, 2DR and 1DR groups, respectively (P<0.001).
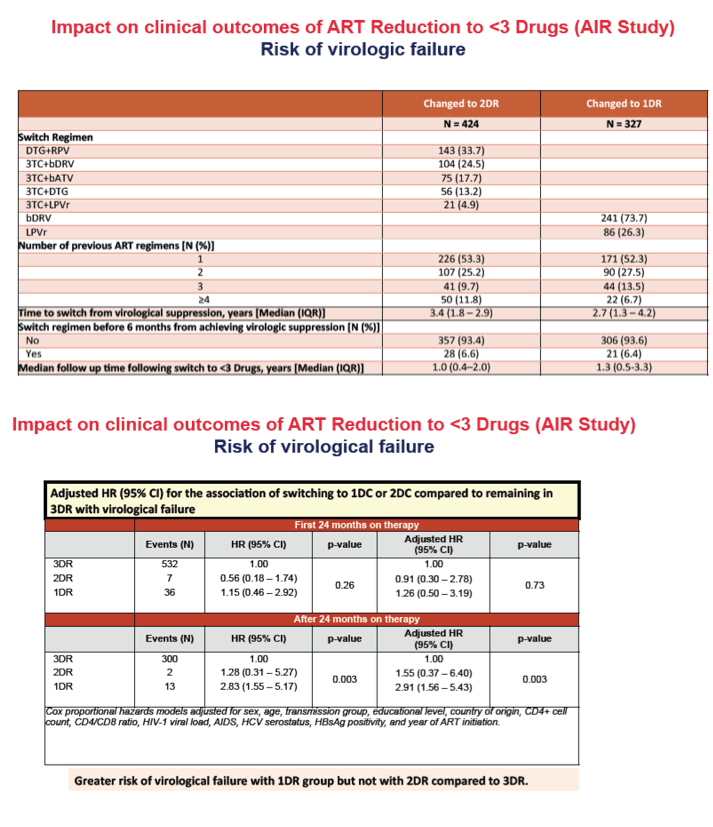
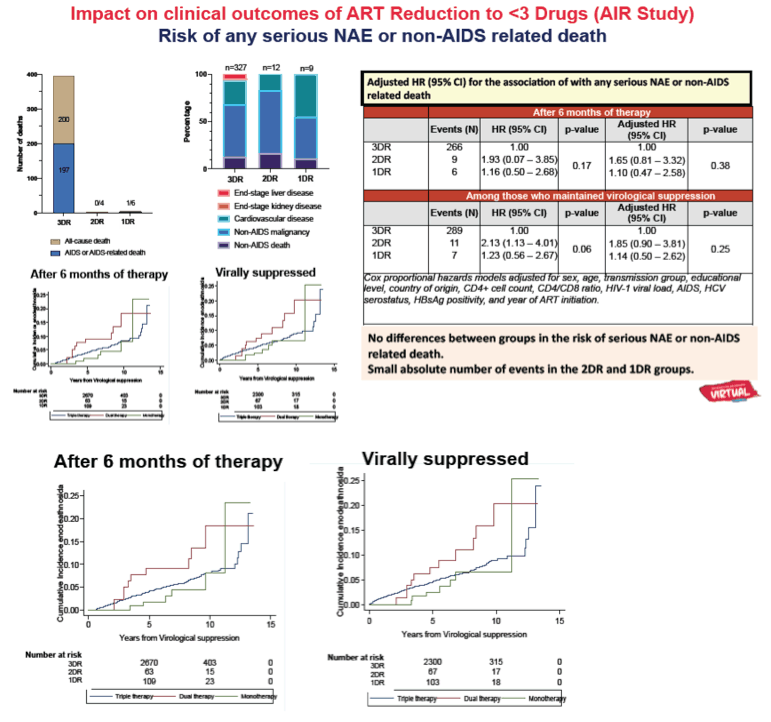
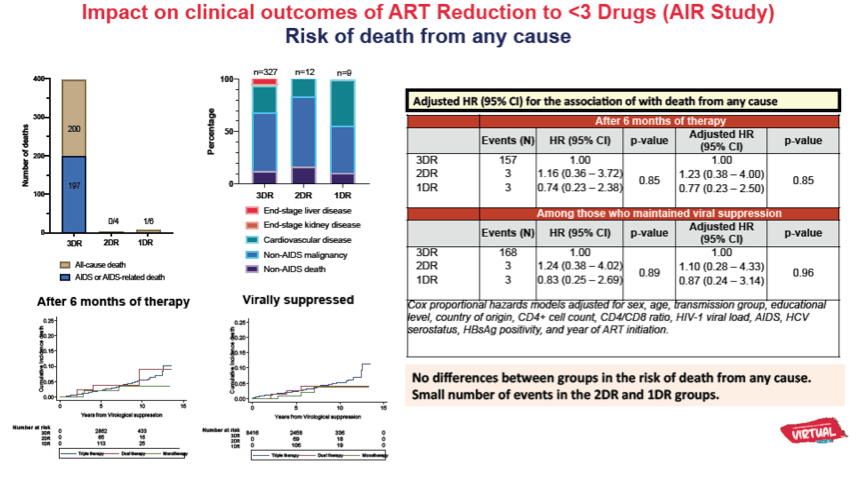
No between-group differences in the risk of endpoints 1-3 were detected. ART reduction after 24 months of therapy was associated with greater risk of virological failure (P=0.003) and greater risk of the composite endpoint (p=0.005), both driven by higher risk with 1DR but not with 2DR.
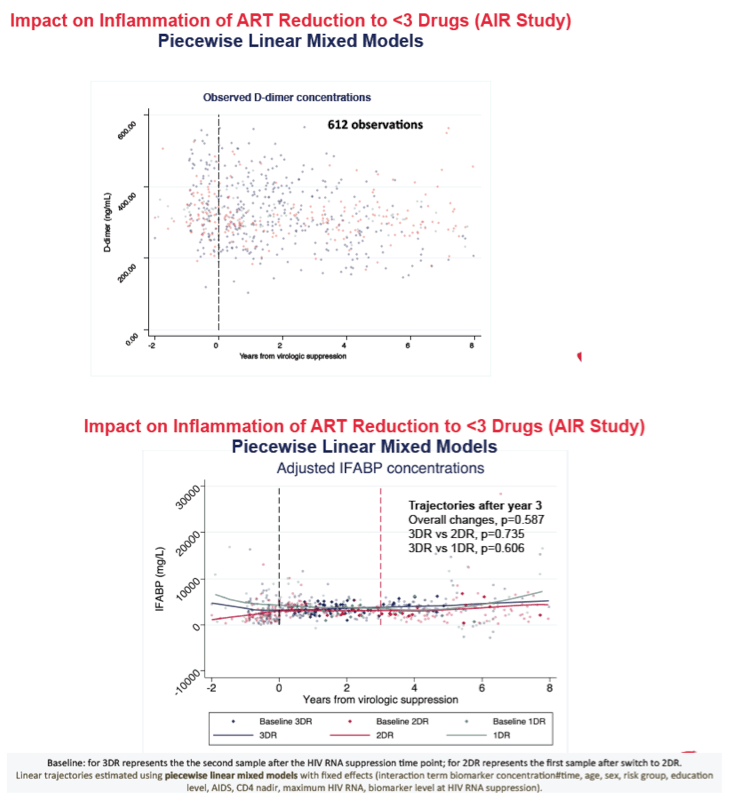
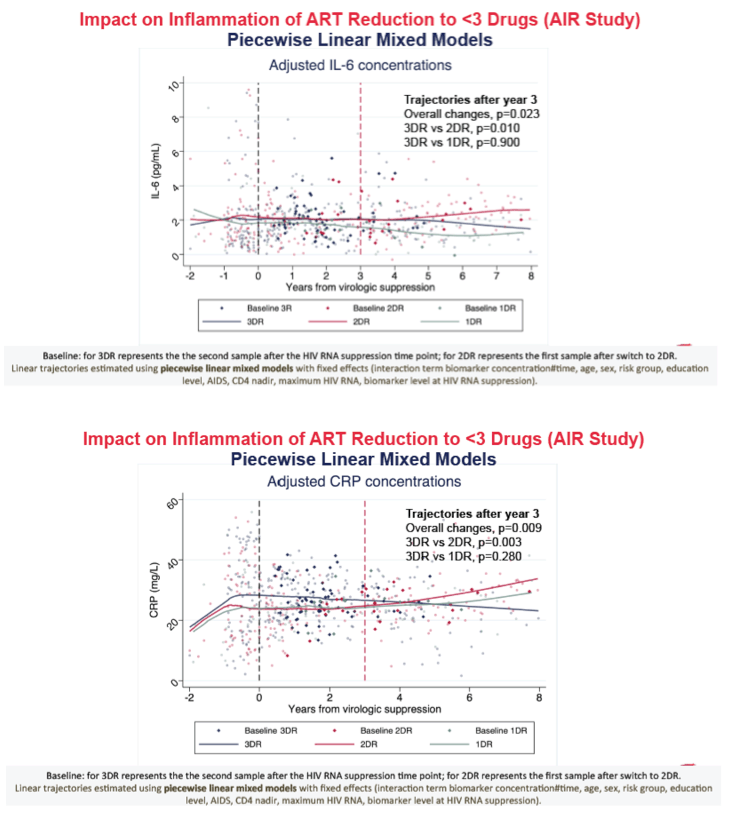
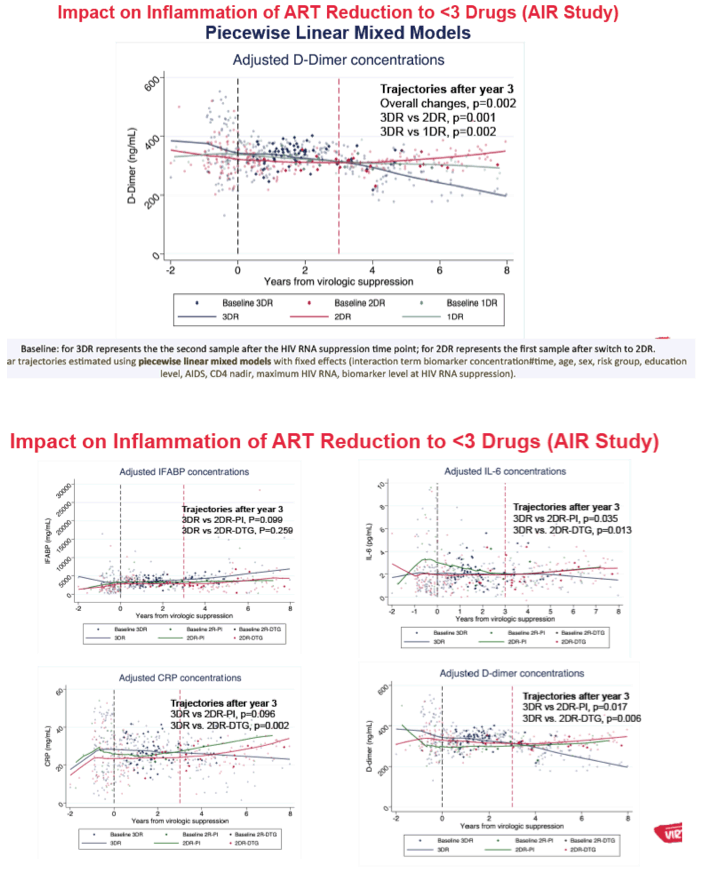
We analyzed 710 samples from 174 subjects (3DR, N=90; 2DR, N=61; 1DR, N=23). Compared to 3DR, 2DR was associated with increases of IL-6 (p=0.01), CRP (p=0.003) and D-dimers (p=0.001) after year 3 from VS. A similar pattern was observed for the comparison between 3DR and 1DR, (only significant for D-dimers trajectories, p=0.002).
CONCLUSIONS: In this large cohort of virally suppressed individuals, 1DR was associated with a greater risk of virological failure, with no significant differences between 2DR and 3DR. However, maintaining 3DR was associated with a more favorable long-term anti-inflammatory profile than switching to 2DR or 1DR. The potential clinical implications of these findings on the development of non-AIDS events deserve further investigation.




|
| |
|
 |
 |
|
|