 |
 |
 |
| |
Empiric Antibiotics Frequent-But Usually Not Needed-for COVID-19
|
| |
| |
IDWeek 2020, October 22-25, 2020
Mark Mascolini
More than half of in-hospital COVID-19 patients in a 1705-person study received empiric antibiotics* [1]. But only 3.5% turned out to have community-onset bacterial infections. The number needed to treat to achieve any benefit with empiric antibiotics was 20 in a study published around the time of IDWeek 2020 [2].
Researchers from the University of Michigan and collaborating centers noted the urge to begin empiric antibiotics when a person gets admitted to the hospital with COVID-19. Up to half of people who die with COVID-19 also have a bacterial infection. Most deaths in the 1918 influenza pandemic resulted from bacterial infection, especially Streptococcus pneumoniae.
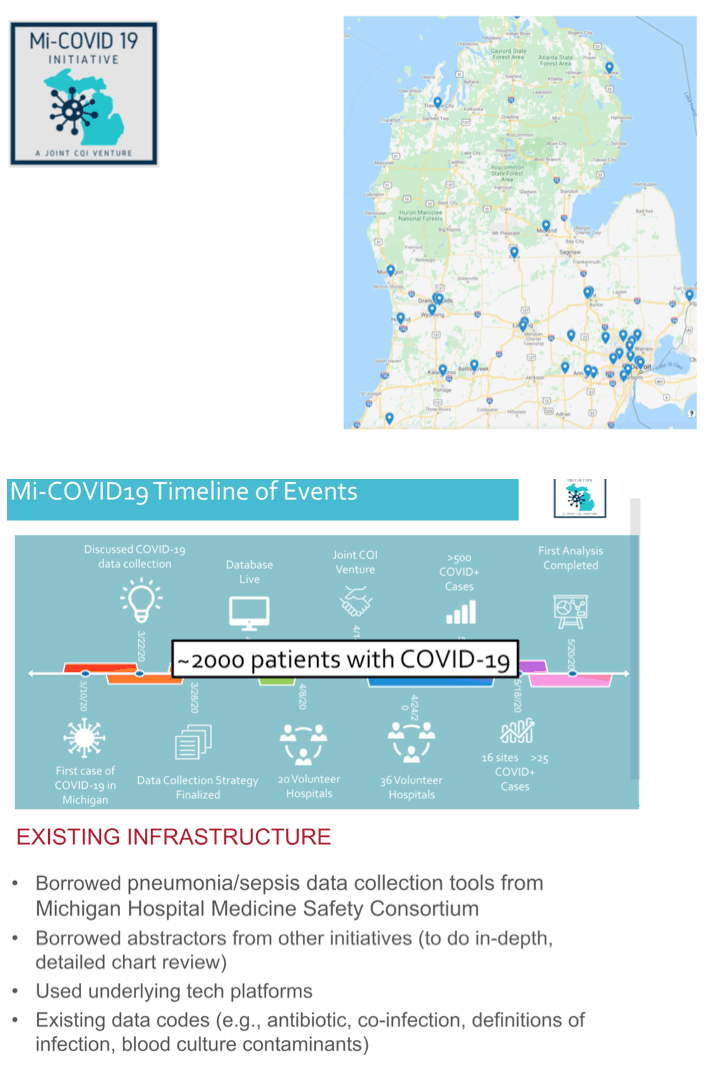
To begin answering the question whether people with COVID-19 need empiric antibiotics when they enter the hospital, the Michigan researchers first determined rates of empiric antibiotic use (defined as antibiotics in the 2 days after admission) and community-onset coinfection (a positive culture or diagnostic test in the first 2 hospital days). They used Poisson generalized estimating equation models to identify predictors of empiric antibiotic use.
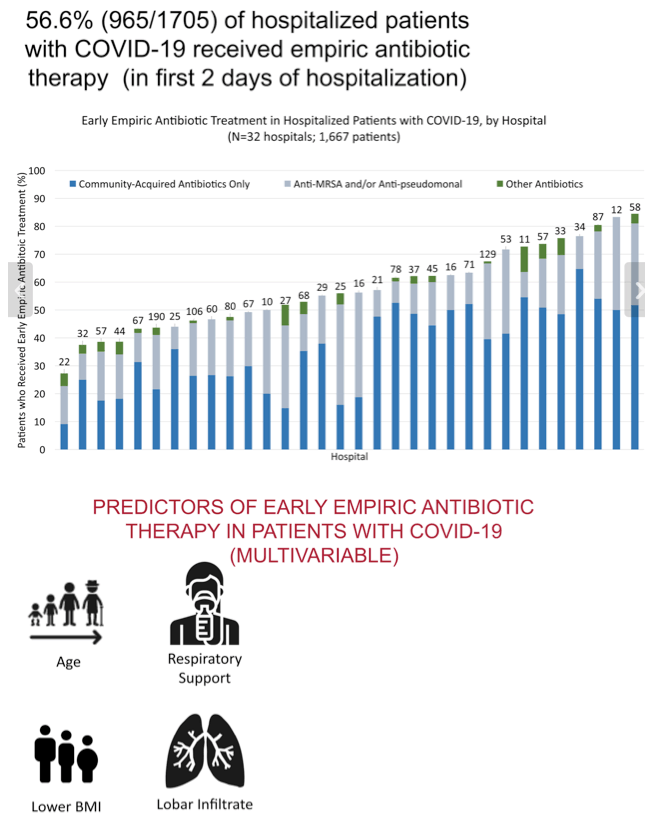
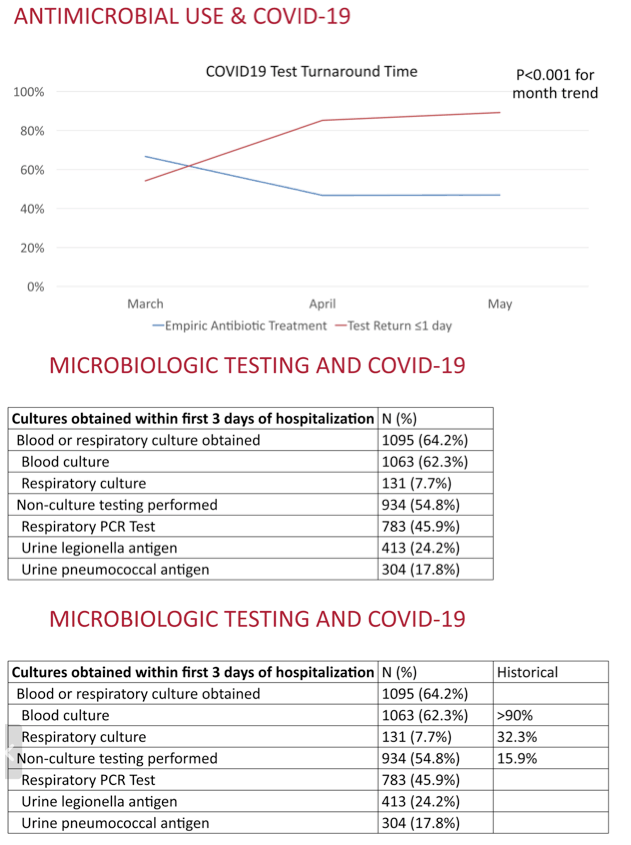
The analysis involved 1705 people admitted to the hospital with COVID-19 at 38 Michigan hospitals between March 13, 2020 and June 18, 2020. The researchers counted 965 COVID-19 inpatients who got empiric antibiotics (56.6%) in the first 2 days of hospitalization. Yet only 59 of those 1705 people (3.5%; 1.8% blood, 1.7% respiratory) had confirmed community-onset bacterial infection. Empiric antibiotic frequency ranged widely across participating hospital, from 27% to 84%.
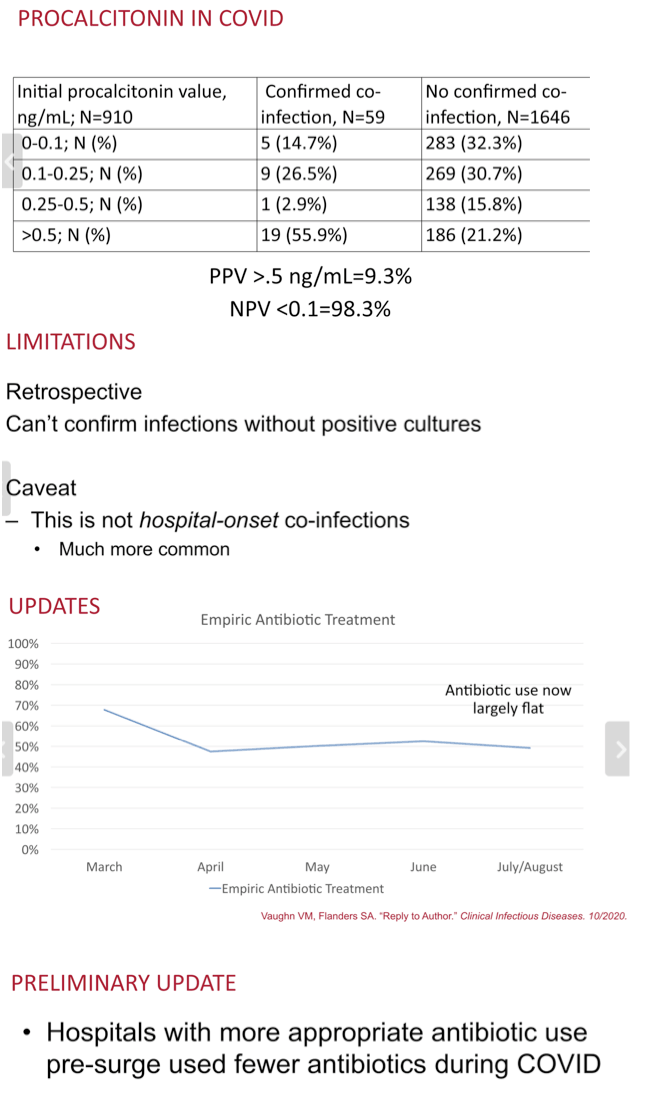
Compared with the 1646 people who did not have confirmed community-onset bacterial coinfection, the 59 who did not were older (median 72.6 vs 64.5 years, rate ratio [RR] 1.30, P = 0.006), had a lower body mass index (26.6 vs 30.0 kg/m2, RR 0.94, P = 0.009), had a higher (worse) Charlson comorbidity score (median 2 vs 1, RR 1.20, P < 0.001), and were more likely to have moderate to severe kidney disease (44.1% vs 25.7%, RR 2.19, P = 0.002), more likely to be admitted to a skilled nursing home (39.0% vs 12.9%, RR 3.96, P < 0.001), more likely to be admitted immediately to the intensive care unit (35.6% vs 10.0%, RR 4.45, P < 0.001), more likely to require mechanical ventilation (27.1% vs 6.1%, RR 6.74, P < 0.001), more likely to have an initial procalcitonin value above 0.5 (55.9% vs 21.2%, RR 4.99, P = 0.001), more likely to have sepsis, severe sepsis, or septic shock on hospital day 1 or 2, and had a higher peak white blood cell count on hospital day 1 or 2 (10 vs 6.8 K/uL, RR 1.03, P < 0.001).
Nine independent predictors of empiric antibiotic use emerged in multivariable analysis, at the following adjusted rate ratios (aRR) and 95% confidence intervals (CI):
Higher likelihood of empiric antibiotics:
-- Each additional 10 years of age: aRR 1.04, 95% CI 1.01 to 1.08, P = 0.02
-- Low-flow oxygen (vs no respiratory support): aRR 1.18, 95% CI 1.06 to 1.31, P = 0.002
-- Heated high-flow nasal cannula (vs no respiratory support): aRR 1.50, 95% CI 1.28 to 1.76, P < 0.001
-- Invasive mechanical ventilation (vs no respiratory support): aRR 1.29, 95% CI 1.07 to 1.54, P = 0.007
-- Severe sepsis on admission: aRR 1.16, 95% CI 1.07 to 1.27, P < 0.001
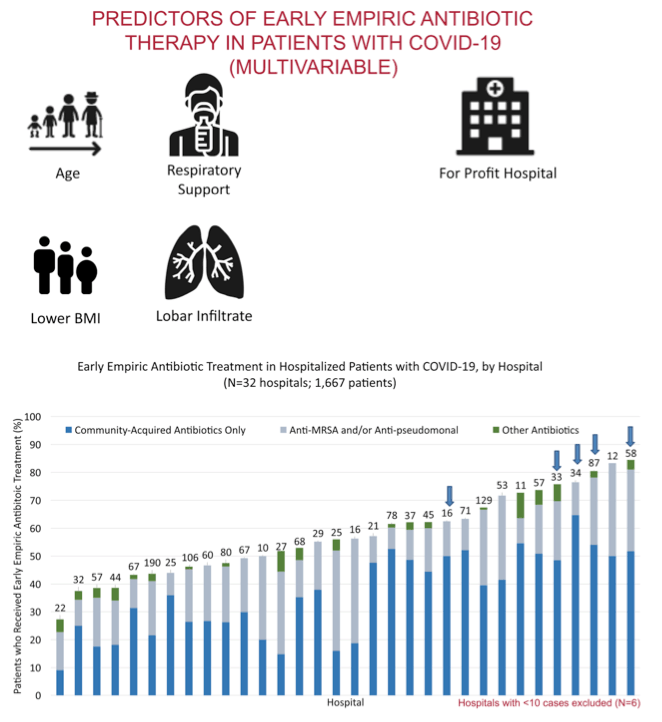
-- For-profit vs nonprofit hospital: aRR 1.30, 95% CI 1.15 to 1.47, P < 0.001
Lower likelihood of empiric antibiotics:
-- Each point higher body mass index: aRR 0.99, 95% CI 0.99 to 1.00, P = 0.03
-- Initial chest x-ray or CT normal: aRR 0.72, 95% CI 0.62 to 0.84, P < 0.001
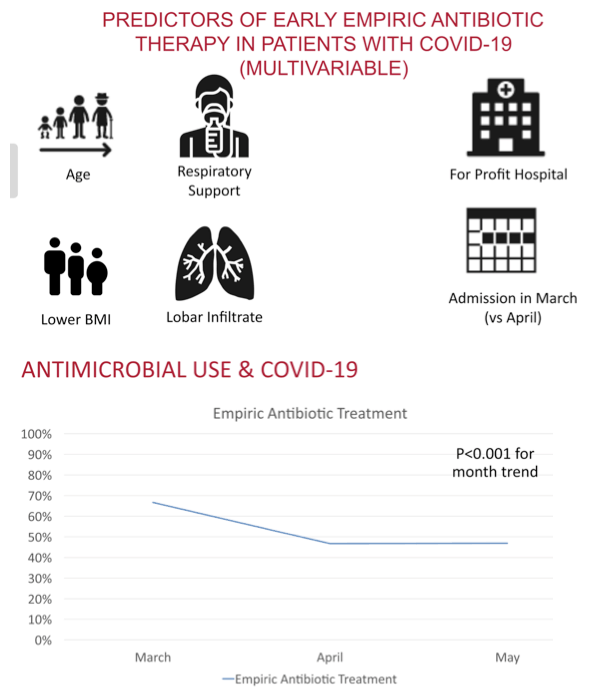
-- Admission in April 2020 (vs March 2020): aRR 0.71, 95% CI 0.63 to 0.81, P < 0.001
Use of empiric antibiotics waned significantly from just below 70% of inpatients in March to just below 50% in May (P < 0.001 for month trend). Over the same period COVID-19 test turnaround time of 1 day or less rose from just below 60% to above 80% (P < 0.001 for month trend).
The Michigan collaborators concluded that much empiric antibiotic use for COVID-19 patients admitted to the hospital is probably unnecessary. Although use of empiric antibiotics fell significantly in these 38 hospitals from March through July/August, the empiric prescribing rate remained largely flat after April, a finding indicating the need for greater antibiotic prescribing stewardship.
*Empiric antibiotics are those given when a clinician suspects a bacterial infection but does not yet have confirming test results.
References
1. Vaughn V, Gandhi TN, Petty LA, et al. Empiric antibiotic therapy and community-onset bacterial co-infection in patients hospitalized with COVID-19: a multi-hospital cohort study. IDWeek 2020, October 22-25, 2020. Abstract 74.
2. Vaughn VM, Gandhi TN, Petty LA, et al. Empiric antibiotic therapy and community-onset bacterial co-infection in patients hospitalized with COVID-19: a multi-hospital cohort study. Clin Infect Dis. ciaa1239,https://doi.org/10.1093/cid/ciaa1239

Abstract
Background
Antibacterials may be initiated out of concern for bacterial co-infection in patients with COVID-19. We determined prevalence and predictors of empiric antibacterial therapy and community-onset bacterial co-infections in hospitalized patients with COVID-19.
Methods
Randomly sampled cohort of 1705 patients hospitalized with COVID-19 in 38 Michigan hospitals between 3/13/2020-6/18/2020. Data were collected on early (prescribed within 2 days of hospitalization) empiric antibacterial therapy and community-onset bacterial co-infections (positive culture or diagnostic test within 3 days). Poisson generalized estimating equation models were used to assess predictors of empiric antibacterial use.
Results
Of 1705 patients with COVID-19, 56.6% were prescribed early empiric antibacterial therapy; 3.5% (59/1705) had a confirmed community-onset bacterial infection. Across hospitals, early empiric antibacterial use varied from 27%-84%. Patients were more likely to receive early empiric antibacterial therapy if they were older (adjusted rate ratio [ARR]: 1.04 [1.00-1.08] per 10 years), had a lower body mass index (ARR: 0.99 [0.99-1.00] per kg/m 2), had more severe illness (e.g., severe sepsis, ARR: 1.16 [1.07-1.27]), had a lobar infiltrate (ARR: 1.21 [1.04-1.42]), or were admitted to a for-profit hospital (ARR: 1.30 [1.15-1.47]). Over time, COVID-19 test turnaround time (returned ≤1 day in March [54.2%, 461/850] vs. in April [85.2%, 628/737], P<.001) and empiric antibacterial use (ARR: 0.71 [0.63-0.81] April vs. March) decreased.
Conclusion
The prevalence of confirmed community-onset bacterial co-infections was low. Despite this, half of patients received early empiric antibacterial therapy. Antibacterial use varied widely by hospital. Reducing COVID-19 test turnaround time and supporting stewardship could improve antibacterial use.





|
| |
|
 |
 |
|
|