 |
 |
 |
| |
Who does not show up for followup in an HIV PrEP clinic?
More Education Favors Steady PrEP-Bisexuals, Heterosexuals Need More Support
|
| |
| |
IDWeek 2020, October 22-25, 2020
Mark Mascolini
People with at least a college education had a 30% lower risk of missing HIV preexposure prophylaxis (PrEP) visits in a 6-year 654-person Rhode Island study [1]. Bisexuals and heterosexuals each had a doubled risk of leaving a PrEP program when compared with same-sex individuals.
Many PrEP programs have a steady fall-off in scheduled PrEP visits, which defeats long-term personal and population-level goals in preventing HIV infection. Because few US studies examine rates and reasons for missing scheduled PrEP visits-or predictors of missing PrEP visits-researchers from Brown University and Miriam Hospital in Providence, Rhode Island set out to study those issues.
The analysis involved all cisgender people who came to Rhode Island's main PrEP clinic from 2013 through 2019. The investigators defined loss to follow-up as failing to keep a PrEP appointment within 98 days of the last visit. They defined reengagement in care as missing at least 2 consecutive follow-up visits then returning for a follow-up appointment.
The 654 study participants had a median age of 31 (interquartile range 25 to 43). Most participants were white (64%), non-Hispanic (81%), and male (96%). Almost two thirds (62%) had a college education, and almost everyone (97%) had health insurance.
Over the 2013-2019 study period, 469 people (72%) were lost to follow-up (stopped returning for PrEP visits) and 185 (28%) remained in care. People who kept regular PrEP visits were significantly older than those who missed visits (34 vs 30 years old, P < 0.001) and were more likely to have only same-sex sex versus sex with both men and women or only with the opposite sex (P = 0.003). Other factors that favored keeping PrEP appointments were having a college education (P < 0.001), having a higher income (P < 0.001), not having an HIV-positive male partner (P = 0.02), and longer observation time (median 16.1 versus 6.4 months, P < 0.001). Among the 469 people who stopping returning for PrEP visits, 127 (27%) later returned for at least one appointment.
Cisgender males tended to keep their PrEP appointments more consistently than cisgender females, but that difference was not statistically significant (P = 0.07). Factors that did not affect appointment keeping were race, ethnicity (Hispanic or not), having more than 5 male sex partners, having anal sex without condoms, and having a sexually transmitted infection.
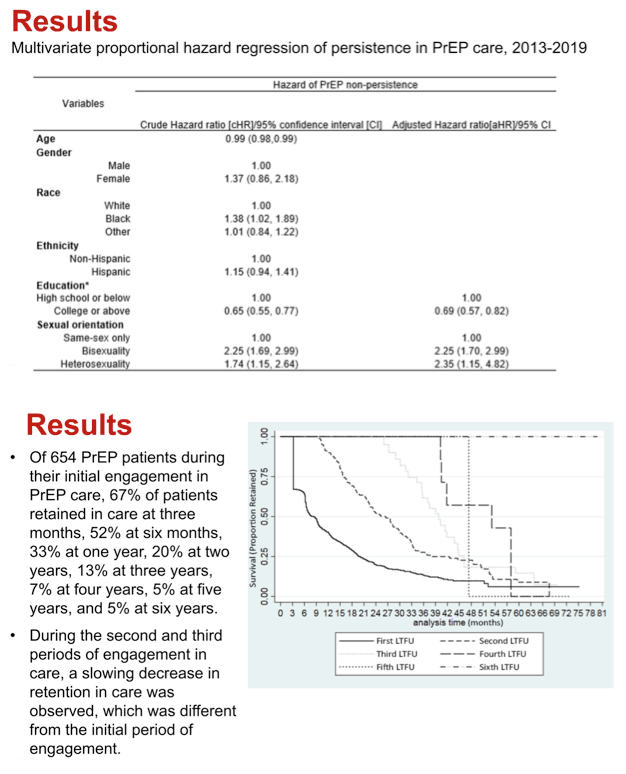
Multivariate proportional hazard regression picked out three factors that independently affected PrEP appointment keeping. Compared with people with less education, those with a college education or more had about a 30% lower risk of missing PrEP visits (adjusted hazard ratio [aHR] 0.69, 95% confidence interval [CI] 0.57 to 0.82). Compared with people who had only same-sex sex, bisexuals had more than a doubled risk of missing PrEP appointments (aHR 2.25, 95% CI 1.70 to 2.99), as did heterosexuals (aHR 2.35, 95% CI 1.15 to 4.82). In this analysis, gender, race, and ethnicity did not independently affect PrEP appointment keeping.
The study did not distinguish between people who stopped PrEP even though they remained at high risk for HIV and people who stopped PrEP because their HIV risk dropped. For example, people who stop having sex with many partners, especially unknown partners, or who start using condoms every time they have sex will correctly perceive a lower risk of HIV infection and may no longer feel the need to take their PrEP pill every day or before and after every sex episode. Also, study results may not apply to all HIV groups because only 4% of participants were women, and only about one third were nonwhite.
The Brown/Miriam researchers underlined the encouraging finding that one quarter of people who stopped keeping PrEP visits later returned. They believe identifying predictors of spotty versus steady PrEP care will help health workers focus on those groups that need the most support in keeping appointments.
Reference
1. Williams R, Flanigan TP, Bazerman L, et al. Who does not show up for followup in an HIV PrEP clinic? IDWeek 2020, October 22-25, 2020. Abstract 101.




|
| |
|
 |
 |
|
|