 |
 |
 |
| |
Four in 5 on ART Resume Therapy in Hospital, One Third Change ARVs - Impact of hospitalization on antiretroviral therapy for people living with HIV
|
| |
| |
IDWeek 2020, October 22-25, 2020
Mark Mascolini
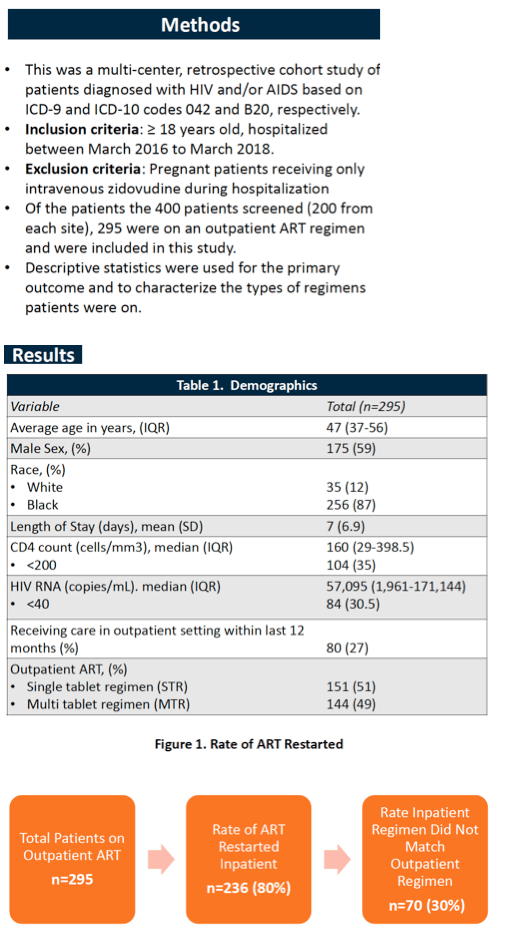
Among 295 people taking antiretroviral therapy (ART) when admitted to the hospital, 80% restarted ART as an inpatient, and 30% of that group restarted a regimen containing different antiretrovirals (ARVs) [1]. Swapping a single-tablet regimen for a multidrug combination, and switching from a nonnucleoside (NNRTI) to an integrase inhibitor explained most in-hospital ARV changes.
Collaborators from Augusta University and the University of Georgia noted that immediately continuing ART may not be a top priority when a person with HIV enters a hospital. Patient status, formulary restrictions, potential drug-drug interactions, and staff knowledge may all contribute to gaps or changes in ART. Inappropriate gaps or changes could persist when a person with HIV leaves the hospital and may adversely affect HIV control and other outcomes.
The Georgia team aimed to measure the rate of ART restarts and changes after hospital admission in nonpregnant adults who entered one of two hospitals between March 2016 and March 2018. This retrospective chart review considered 400 people with HIV, 200 from each hospital. Analysis focused on 295 people taking ART when admitted to the hospital.
The study group averaged 47 years in age, 59% were men, 87% black, and 12% white. Median CD4 count stood at 160 (interquartile range [IQR] 29 to 398.5), and 30.5% of the group had a viral load below 40 copies. Among those with a detectable load, median load stood at 57,095 copies (IQR 1961 to 171,144). Only 80 people (27%) received regular outpatient care in the preceding 12 months.
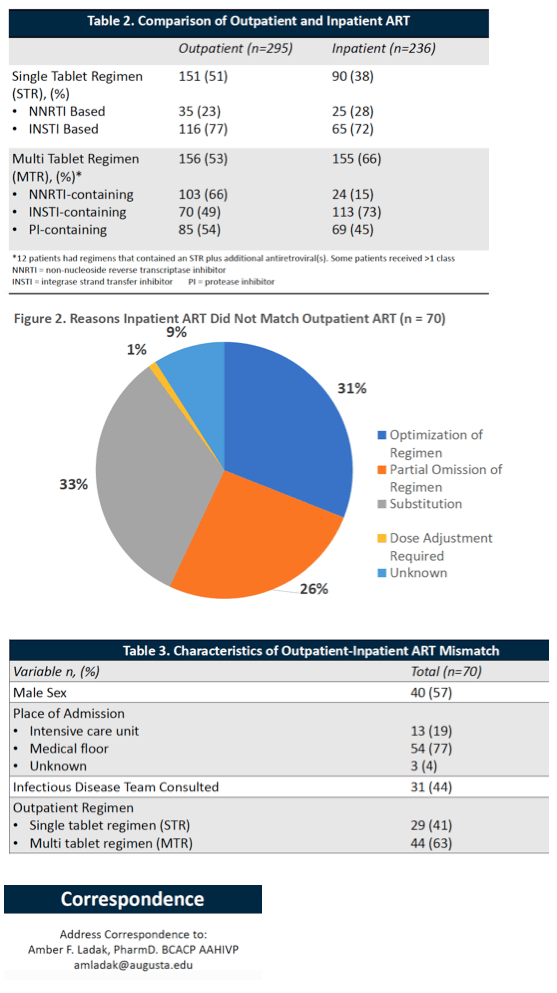
Among these 295 people on ART, 151 (51%) took a single-tablet regimen and 144 (49%) a multitablet combination when entering the hospital. In all, 236 people (80%) restarted ART in the hospital, and 70 of those 236 (30%) restarted a regimen different from their previous outpatient combination. Principal recorded reasons for changing the regimen were substitution in 33%, regimen optimization in 31%, and partial regimen omission in 26%. Only 1% of ART changes were attributed to a needed dose adjustment. The researchers stressed that 69% of regimen modifications did not reportedly involve attempts to improve the regimen.
Principal ART shifts reflected a decline in single-tablet regimens (51% outpatient to 38% inpatient) and a corresponding jump in multitablet regimens (53% outpatient to 66% inpatient). Among multitablet regimens, the proportion including an NNRTI dropped (66% outpatient to 15% inpatient) while the fraction including an integrase inhibitor rose (49% outpatient to 73% inpatient). Thus hospital prescribers evinced a preference for integrase inhibitors over NNRTIs, even at the cost of trading an all-in-one pill for two or more tablets.
The researchers could not pinpoint any factors corresponding to changing the outpatient regimen, including patient sex, place of admission (intensive care or medical floor), or consulting an infectious disease team. They proposed a positive spin of this finding, suggesting "there are many opportunities to improve transitions of care and antiretroviral stewardship."
Reference
1. Ladak AF, Young HN, Tang E, Curtis J, Chastain DB. Impact of hospitalization on antiretroviral therapy for people living with HIV. IDWeek 2020, October 22-25, 2020. Abstract 1022.

|
| |
|
 |
 |
|
|