 |
 |
 |
| |
Non-Overweight Patients with Nonalcoholic Fatty Liver Disease, Diabetes
Fare Worse Than Overweight Patients Before and After Liver Transplant
|
| |
| |
November 12, 2021
A new study has found that people with nonalcoholic fatty liver disease (NAFLD) cirrhosis who are not overweight and are on a waiting list for a liver transplant fare worse than overweight patients before and after transplant surgery. The study concludes that these at-risk patients need better nutritional counseling and other interventions to help prevent serious health problems while they are waiting for liver transplant.
Non-Overweight Patients with Nonalcoholic Fatty Liver Disease, Diabetes Fare Worse
Than Overweight Patients Before and After Liver Transplant
ALEXANDRIA, Va. - A new study has found that people with nonalcoholic fatty liver disease
(NAFLD) cirrhosis who are not overweight and are on a waiting list for a liver transplant fare
worse than overweight patients before and after transplant surgery. The study concludes that
these at-risk patients need better nutritional counseling and other interventions to help prevent
serious health problems while they are waiting for liver transplant.
Researchers at the Yale School of Medicine, Beth Israel Deaconess Medical Center and
Harvard Medical School will present the study this week at The Liver Meeting Digital
Experience™ held by the American Association for the Study of Liver Diseases.
Although both obesity and diabetes are known independent risk factors for NAFLD cirrhosis, too
little is known about how underweight and normal-weight patients with NAFLD fare before and
after liver transplant. Information about the role of diabetes in poor patient outcomes, including
early removal from liver transplant waiting lists and even post-transplant death, is also limited.
"NAFLD is one of the leading etiologies of liver disease among adults awaiting liver
transplantation, and non-overweight individuals with NAFLD represent a subset of patients with
a distinct risk factor profile characterized by increased visceral adipose tissue, underlying insulin
resistance and genetic predisposition," said Pedro Ochoa-Allemant, MD, the study's lead
researcher and resident physician at the department of internal medicine at the Yale School of
Medicine. "Despite an apparent healthy status with lower body mass index, these patients have
increased cardiometabolic risk factors, such as diabetes, that are associated with subsequent
worse outcomes throughout the transplant process." The study found that non-overweight patients on a liver transplant waiting list were more likely than overweight or obese patients to:
• Be female, be older, have public insurance and have a low liver function.
• Have ascites, or fluid buildup in the abdomen, from severe liver disease and hepatic
encephalopathy.
• Have a transjugular intrahepatic portosystemic shunt - a passage surgically created to
allow fluid to move from one organ to another.
• Be removed early from liver transplant waitlists.
• Die after a liver transplant.
Compared with overweight patients who did not have diabetes, non-overweight patients with
diabetes on a transplant list:
• Had even higher rates of severe outcomes.
• Had significantly higher rates of waitlist removal.
• Needed better nutritional counseling and healthy lifestyle interventions to help them
lower their risk of severe outcomes as they waited for a new liver and after they had
transplant surgery.
Non-overweight patients died after liver transplants at a higher rate than overweight patients
whether they had diabetes or not.
"Our study suggests that non-overweight individuals with NAFLD cirrhosis have higher rates of
waitlist removal due to clinical deterioration, as well as worse post-transplant survival compared
with their overweight and obese counterparts," said Ochoa-Allemant. "Therefore, it is crucial to
identify these individuals at higher risk for adverse outcomes and effectively intervene by
enhancing nutritional support, promoting physical activity and investigating other potential
metabolic interventions to minimize risk before and after liver transplantation."
The researchers identified 24,127 people with NAFLD who were on liver transplant waiting lists
from Feb.2002, through June 2020, from the United Network for Organ Sharing database. Of
these individuals, 6.8 percent were non-overweight, with a body mass index (BMI) between 18.5
and 24.9 kg/m2), and 93.2 percent were overweight or obese, with a BMI above this range.
Dr. Ochoa-Allemant's poster entitled "Non-Overweight NAFLD and Diabetes Impact Outcomes
in NAFLD Cirrhosis on Transplant Waitlist: A UNOS Analysis" (1505) has been designated a
poster of distinction and can be viewed at The Liver Meeting Digital Experience™. The
corresponding abstract can be found in the journal HEPATOLOGY.
About AASLD AASLD is the leading organization of clinicians and researchers committed to preventing and
curing liver disease. The work of our members has laid the foundation for the development of
drugs used to treat patients with viral hepatitis. Access to care and support of liver disease
research are at the center of AASLD's advocacy efforts. News releases and additional information about AASLD are available online at www.aasld.org.
Media Contact: Nola Gruneisen Phone: 571-292-3068 Email: media@aasld.org
--------------------
Abstract
NON-OVERWEIGHT NAFLD AND DIABETES IMPACT OUTCOMES IN NAFLD CIRRHOSIS ON TRANSPLANT WAITLIST: A UNOS ANALYSIS
Pedro Ochoa-Allemant1, Hirsh Trivedi2, Alan Bonder3 and Zachary Fricker3, (1)Internal Medicine, Yale School of Medicine, New Haven, CT, (2)Division of Gastroenterology and Hepatology, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA, (3)Liver Center, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston, MA
Background: Obesity and diabetes (DM) are known independent risk factors in patients with non-alcoholic fatty liver disease (NAFLD), but limited data exists describing pre- and post-liver transplant (LT) outcomes in non-overweight patients and their association with DM. Among patients with NAFLD, we evaluated the associations of non-overweight NAFLD and DM with adverse waitlist removal and post-LT mortality.
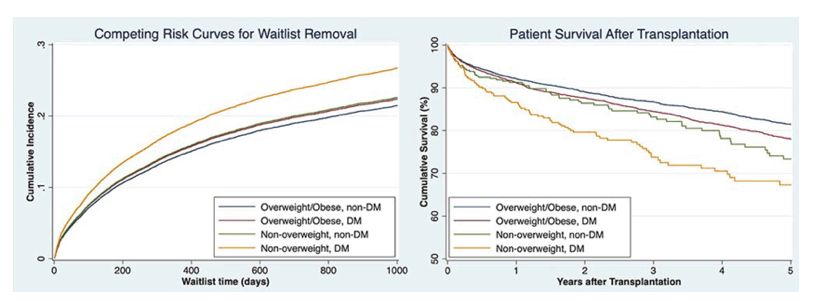
Methods: We used the United Network of Organ Sharing (UNOS) database to identify adult patients with NAFLD listed for LT between February 27, 2002, and June 30, 2020. Patients were classified as "non-overweight" (BMI 18.5-24.9 kg/m2) or "overweight/obese" (BMI ≥25 kg/m2). The primary outcome was waitlist removal due to death before LT or clinical deterioration. The secondary outcome was all-cause mortality after LT. We used competing-risks analysis to estimate waitlist removal and Cox proportional hazards models to estimate post-LT survival.
Results: 24,127 patients with NAFLD (non-overweight 6.8%, overweight/obese 93.2%) were listed for LT. Non-overweight patients with NAFLD were more frequently women, older, more likely to have public insurance, and had worse functional status compared to overweight/obese patients. Moreover, they had a higher prevalence of ascites, hepatic encephalopathy, and TIPS at listing. Non-overweight patients suffered higher waitlist removal (SHR 1.14, 95% CI 1.03-1.27; P=.01) and all-cause mortality after LT (HR 1.50, 95% CI 1.27-1.76; P<.001) compared to overweight/obese patients. Non-overweight patients with DM had higher waitlist removal (SHR 1.29, 95% CI 1.12-1.48; P<.001) and all-cause mortality after LT (HR 1.95, 95% CI 1.57-2.42; P<.001) compared to overweight/obese patients without DM. After multivariable analysis, non-overweight patients with DM had significantly higher waitlist removal (SHR 1.18, 95% CI 1.03-1.36; P=.02). In addition, the non-overweight without DM (HR 1.47, 95% CI 1.25-1.73; P<.001) and non-overweight with DM (HR 1.84, 95% CI 1.48-2.28; P<.001) had higher post-LT mortality.
Conclusion: Non-overweight patients with NAFLD cirrhosis on the transplant waitlist have worse pre- and post-LT outcomes. In particular, the combination of low/normal BMI and DM was most strongly associated with waitlist removal and all-cause mortality after LT. Optimizing metabolic risks in non-overweight NAFLD patients with diabetes through appropriate nutritional counseling and lifestyle intervention may help mitigate poor outcomes on the transplant waitlist.
|
| |
|
 |
 |
|
|