 |
 |
 |
| |
CIRRHOSIS IS ASSOCIATED WITH SIGNIFICANT ADVERSE PREGNANCY
COMPLICATIONS: A 7-YEAR NATIONWIDE INPATIENT SAMPLE STUDY
|
| |
| |
- patients with cirrhosis were found to have a significantly higher rate of preeclampsia/eclampsia (10.50% vs. 5.27%, p<0.001) and preterm labor (11.42% vs. 6.29%, p<0.001). higher all-cause maternal mortality (0.46% vs. 0.01%, p<0.001) - multidisciplinary approach including liver specialists and high-risk pregnancy specialists is needed
AASLD 2021 Nov 12-16

Bing Chen, Department of Medicine, Mount Sinai Morningside and West Hospitals, Yichen Wang, Mercy Internal Medicine Service, Trinity Health of New England and Tatyana Kushner, Division of Liver Disease, Mount Sinai Hospital
Background: Earlier data evaluating pregnant women with cirrhosis from the National Inpatient Sample (NIS) from 1993 to 2005 suggested that cirrhotic patients have an increased risk of obstetric complications. With the increase in prevalence of cirrhosis seen during pregnancy, we aimed to perform an updated analysis of NIS data to evaluate pregnancy outcomes associated with cirrhosis.
Methods: We performed a retrospective study using the NIS database from 2012 to 2018. Previously validated ICD-9 and ICD-10 codes for pregnancy-related admissions were utilized to identify all pregnant women. Patients with acute liver diseases were excluded. Patients with a diagnosis of cirrhosis were identified. We evaluated pregnancy-related complications including rates of C-section, preeclampsia/eclampsia, preterm labor, and gestational diabetes (GDM), as well as all-cause in-hospital mortality, length of stay, and total charge of the hospital stay in pregnant women with cirrhosis compared to women without cirrhosis. Multivariate logistic regression was used to adjust for age at pregnancy and race.
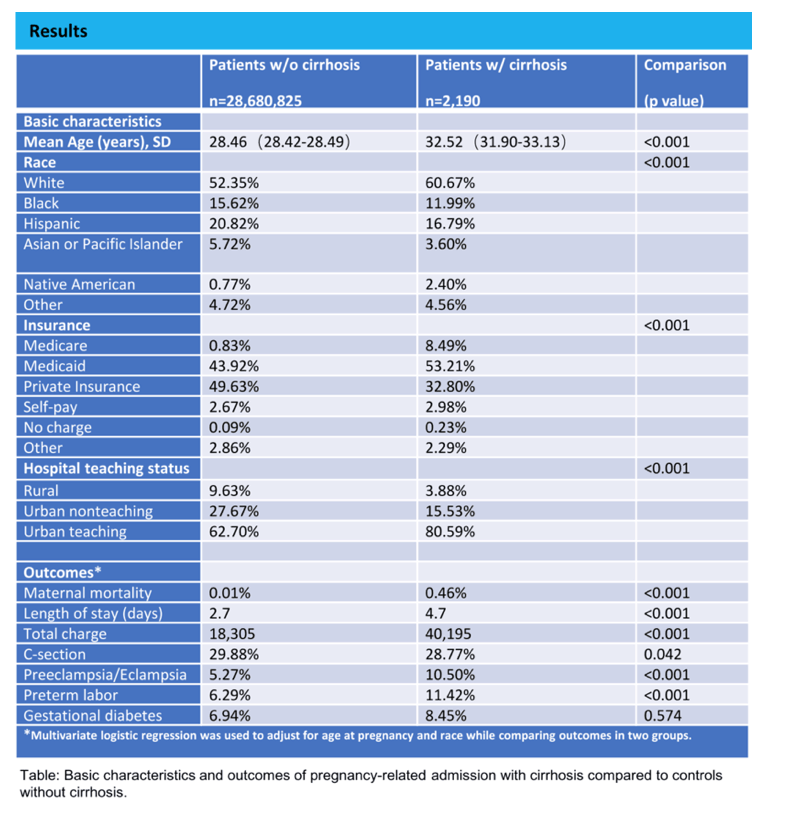
Results: A total of 28.67 million pregnancy-related admissions which met our eligibility criteria were identified. Cirrhosis was found in 2190 (0.01%) patients. Compared to patients without cirrhosis, patients with cirrhosis were older (32.5 years vs. 28.5 years, p<0.001) and more likely to be white (61% vs. 52%) (Table 1). They were more likely to have Medicare (8.49% vs. 0.83%, p<0.001) and Medicaid (53.21% vs. 43.92%, p<0.001) and have pregnancy care in an urban teaching hospital (80.59% vs. 52.70%, p<0.001). In comparison to patients without cirrhosis, patients with cirrhosis were found to have a significantly higher rate of preeclampsia/eclampsia (10.50% vs. 5.27%, p<0.001) and preterm labor (11.42% vs. 6.29%, p<0.001). Patients with cirrhosis had a much higher all-cause maternal mortality (0.46% vs. 0.01%, p<0.001), longer mean length of hospital stay (4.7 days vs. 2.7 days, p<0.001), and a higher cost associated with hospitalization (40,195 dollars vs. 18,305 dollars, p<0.001).
Conclusion:Although cirrhosis remains rare in pregnant women it is associated with a significantly higher rate of preeclampsia/eclampsia, preterm labor, all-cause maternal mortality, length of stay, and cost of hospitalization. A multidisciplinary approach including liver specialists and high-risk pregnancy specialists is needed to ensure early detection, recognition, and diagnosis of cirrhosis during pregnancy, and manage pregnant women with cirrhosis to optimize maternal and fetal outcomes.


|
| |
|
 |
 |
|
|